Abstract
Purpose
Intraventricular hemorrhage (IVH) is a common affliction of preterm infants and often results in posthemorrhagic hydrocephalus (PHH). These patients typically eventually require permanent CSF diversion and are presumed to be indefinitely shunt-dependent. To date, however, there has been no study of long-term shunt revision requirements in patients with PHH.
Methods
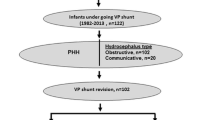
We analyzed retrospectively collected data for 89 preterm patients diagnosed with grades III and IV IVH and PHH at our institution from 1998 to 2011.
Results
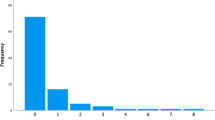
Sixty-nine out of 89 patients (77.5 %) underwent ventriculoperitoneal (VP) shunt placement, and 33 (47.8 %) required at least one shunt revision and 18 (26.1 %) required multiple revisions. The mean ± standard deviation follow-up time for shunted patients was 5.0 ± 3.3 years. The majority of early failures were due to proximal catheter malfunction, while later failures were mostly due to distal catheter problems. There was a significant difference in the number of patients requiring revisions in the first 3 years following initial VP shunt insertion compared after 3 years, with 28 revisions versus 10 (p < 0.004). In 8 out of 10 patients who underwent shunt revisions after 3 years, evidence of obstructive hydrocephalus was found on imaging either in the form of an isolated fourth ventricular cyst or aqueductal stenosis.
Conclusions
Our results suggest that in a distinct subset of patients with PHH, obstructive hydrocephalus may develop, resulting in long-term dependence on CSF diversion. Further study on the factors associated with long-term shunt dependence and revision requirements within the PHH group is warranted.




Similar content being viewed by others
References
Alan N, Manjila S, Minich N, Bass N, Cohen AR, Walsh M, et al. (2012) Reduced ventricular shunt rate in very preterm infants with severe intraventricular hemorrhage: an institutional experience. J Neurosurg Pediatr 10:357–364
Beez T, Sarikaya-Seiwert S, Bellstadt L, Muhmer M, Steiger HJ (2014) Role of ventriculoperitoneal shunt valve design in the treatment of pediatric hydrocephalus—a single center study of valve performance in the clinical setting. Childs Nerv Syst 30:293–297
Berry JG, Hall MA, Sharma V, Goumnerova L, Slonim AD, Shah SS (2008) A multi-institutional, 5-year analysis of initial and multiple ventricular shunt revisions in children. Neurosurgery 62:445–453 discussion 453–444
Brouwer A, Groenendaal F, van Haastert IL, Rademaker K, Hanlo P, de Vries L (2008) Neurodevelopmental outcome of preterm infants with severe intraventricular hemorrhage and therapy for post-hemorrhagic ventricular dilatation. J Pediatr 152:648–654
Brouwer AJ, van Stam C, Uniken Venema M, Koopman C, Groenendaal F, de Vries LS (2012) Cognitive and neurological outcome at the age of 5–8 years of preterm infants with post-hemorrhagic ventricular dilatation requiring neurosurgical intervention. Neonatology 101:210–216
Chittiboina P, Pasieka H, Sonig A, Bollam P, Notarianni C, Willis BK, et al. (2013) Posthemorrhagic hydrocephalus and shunts: what are the predictors of multiple revision surgeries? J Neurosurg Pediatr 11:37–42
Lazareff JA, Peacock W, Holly L, Ver Halen J, Wong A, Olmstead C (1998) Multiple shunt failures: an analysis of relevant factors. Childs Nerv Syst 14:271–275
Lee IC, Lee HS, Su PH, Liao WJ, Hu JM, Chen JY (2009) Posthemorrhagic hydrocephalus in newborns: clinical characteristics and role of ventriculoperitoneal shunts. Pediatr Neonatol 50:26–32
Levy ML, Masri LS, McComb JG (1997) Outcome for preterm infants with germinal matrix hemorrhage and progressive hydrocephalus. Neurosurgery 41:1111–1117 discussion 1117–1118
Limbrick Jr DD, Mathur A, Johnston JM, Munro R, Sagar J, Inder T, et al. (2010) Neurosurgical treatment of progressive posthemorrhagic ventricular dilation in preterm infants: a 10-year single-institution study. J Neurosurg Pediatr 6:224–230
McGirt MJ, Wellons 3rd JC, Nimjee SM, Bulsara KR, Fuchs HE, George TM (2003) Comparison of total versus partial revision of initial ventriculoperitoneal shunt failures. Pediatr Neurosurg 38:34–40
Notarianni C, Vannemreddy P, Caldito G, Bollam P, Wylen E, Willis B, et al. (2009) Congenital hydrocephalus and ventriculoperitoneal shunts: influence of etiology and programmable shunts on revisions. J Neurosurg Pediatr 4:547–552
Parker SL, Attenello FJ, Sciubba DM, Garces-Ambrossi GL, Ahn E, Weingart J, et al. (2009) Comparison of shunt infection incidence in high-risk subgroups receiving antibiotic-impregnated versus standard shunts. Childs Nerv Syst 25:77–83 discussion 85
Patwardhan RV, Nanda A (2005) Implanted ventricular shunts in the United States: the billion-dollar-a-year cost of hydrocephalus treatment. Neurosurg 56:139–144 discussion 144–135
Reddy GK, Bollam P, Caldito G (2014) Long-term outcomes of ventriculoperitoneal shunt surgery in patients with hydrocephalus. World Neurosurg 81:404–410
Reinprecht A, Dietrich W, Berger A, Bavinzski G, Weninger M, Czech T (2001) Posthemorrhagic hydrocephalus in preterm infants: long-term follow-up and shunt-related complications. Childs Nerv Syst 17:663–669
Robinson S (2012) Neonatal posthemorrhagic hydrocephalus from prematurity: pathophysiology and current treatment concepts. J Neurosurg Pediatr 9:242–258
Sciubba DM, Noggle JC, Carson BS, Jallo GI (2008) Antibiotic-impregnated shunt catheters for the treatment of infantile hydrocephalus. Pediatr Neurosurg 44:91–96
Shah SS, Hall M, Slonim AD, Hornig GW, Berry JG, Sharma V (2008) A multicenter study of factors influencing cerebrospinal fluid shunt survival in infants and children. Neurosurgery 62:1095–1102 discussion 1102–1093
Shannon CN, Simon TD, Reed GT, Franklin FA, Kirby RS, Kilgore ML, et al. (2011) The economic impact of ventriculoperitoneal shunt failure. J Neurosurg Pediatr 8:593–599
Simon TD, Riva-Cambrin J, Srivastava R, Bratton SL, Dean JM, Kestle JR (2008) Hospital care for children with hydrocephalus in the United States: utilization, charges, comorbidities, and deaths. J Neurosurg Pediatr 1:131–137
Simon TD, Whitlock KB, Riva-Cambrin J, Kestle JR, Rosenfeld M, Dean JM, et al. (2012) Association of intraventricular hemorrhage secondary to prematurity with cerebrospinal fluid shunt surgery in the first year following initial shunt placement. J Neurosurg Pediatr 9:54–63
Smith ER, Butler WE, Barker 2nd FG (2004) In-hospital mortality rates after ventriculoperitoneal shunt procedures in the United States, 1998 to 2000: relation to hospital and surgeon volume of care. J Neurosurg 100:90–97
Stein SC, Guo W (2008) Have we made progress in preventing shunt failure? A critical analysis. J Neurosurg Pediatr 1:40–47
Stone JJ, Walker CT, Jacobson M, Phillips V, Silberstein HJ (2013) Revision rate of pediatric ventriculoperitoneal shunts after 15 years. J Neurosurg Pediatr 11:15–19
Stone SS, Warf BC (2014) Combined endoscopic third ventriculostomy and choroid plexus cauterization as primary treatment for infant hydrocephalus: a prospective North American series. J Neurosurg Pediatr 14:439–446
Talamonti G, D'Aliberti G, Collice M (2007) Myelomeningocele: long-term neurosurgical treatment and follow-up in 202 patients. J Neurosurg 107:368–386
Tuli S, Drake J, Lawless J, Wigg M, Lamberti-Pasculli M (2000) Risk factors for repeated cerebrospinal shunt failures in pediatric patients with hydrocephalus. J Neurosurg 92:31–38
Wang JY, Amin AG, Jallo GI, Ahn ES (2014) Ventricular reservoir versus ventriculosubgaleal shunt for posthemorrhagic hydrocephalus in preterm infants: infection risks and ventriculoperitoneal shunt rate. J Neurosurg Pediatr 14:447–454
Warf BC, Campbell JW, Riddle E (2011) Initial experience with combined endoscopic third ventriculostomy and choroid plexus cauterization for post-hemorrhagic hydrocephalus of prematurity: the importance of prepontine cistern status and the predictive value of FIESTA MRI imaging. Childs Nerv Syst 27:1063–1071
Wellons JC, Shannon CN, Kulkarni AV, Simon TD, Riva-Cambrin J, Whitehead WE, et al. (2009) A multicenter retrospective comparison of conversion from temporary to permanent cerebrospinal fluid diversion in very low birth weight infants with posthemorrhagic hydrocephalus. J Neurosurg Pediatr 4:50–55
Willis B, Javalkar V, Vannemreddy P, Caldito G, Matsuyama J, Guthikonda B, et al. (2009) Ventricular reservoirs and ventriculoperitoneal shunts for premature infants with posthemorrhagic hydrocephalus: an institutional experience. J Neurosurg Pediatr 3:94–100
Disclosures
The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Financial support
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, J.Y., Jackson, E.M., Jallo, G.I. et al. Shunt revision requirements after posthemorrhagic hydrocephalus of prematurity: insight into the time course of shunt dependency. Childs Nerv Syst 31, 2123–2130 (2015). https://doi.org/10.1007/s00381-015-2865-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-015-2865-5