Abstract
Objective
The purpose of this study was to evaluate the outcomes of computed tomography (CT) guidance using percutaneous catheter with low-dose drainage local chemotherapy (modified PCD) and antituberculous therapy (ATT) for the treatment of spinal tuberculosis in children.
Methods
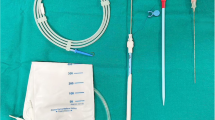
Twenty-seven children suffering from spinal tuberculosis were treated with modified PCD and ATT in our institute from 2002 to 2012. We describe our treatment, which involves CT-guided percutaneous puncture and local chemotherapy (continuous low-dose (20 mL) irrigation). The patients were evaluated based on the Frankel scoring system, the kyphotic Cobb angle, and the erythrocyte sedimentation rate (ESR).
Results
All patients were followed up for an average of 31.00 ± 13.94 months. No sinus formation was detected. All patients responded well to this treatment. The ESR values were decreased to normal at last follow-up. The neurological functions show significant improvement after operation. Preoperatively, the kyphotic angle was 22.89 ± 7.06°, and it was measured as 21.19 ± 8.73° at the last visit.
Conclusions
Our results showed that percutaneous intubation and low-dose irrigation under CT guidance (modified percutaneous catheter drainage (MPCD)) and ATT are easy, safe, efficient, and less invasive methods for the treatment of spinal tuberculosis in children.


Similar content being viewed by others
References
Organization WH (2009) Global tuberculosis control 2009: epidemiology, strategy, financing. World Health Organization
Newton SM, Brent AJ, Anderson S, Whittaker E, Kampmann B (2008) Paediatric tuberculosis. Lancet Infect Dis 8:498–510
Nelson L, Wells C (2004) Global epidemiology of childhood tuberculosis [Childhood TB]. Int J Tuberc Lung Dis 8:636–647
Lu T-H, Huang R, Chang T, Tsao S, Wu T (2005) Tuberculosis mortality trends in Taiwan: a resurgence of non-respiratory tuberculosis. Int J Tuberc Lung Dis 9:105–110
Yeh Y-P, Chang H-J, Yang J, Chang S-H, Suo J, Chen TH-H (2005) Incidence of tuberculosis in mountain areas and surrounding townships: dose–response relationship by geographic analysis. Ann Epidemiol 15:526–532
Marais BJ, Graham SM, Maeurer M, Zumla A (2013) Progress and challenges in childhood tuberculosis. Lancet Infect Dis 13:287–289
Nene A, Bhojraj S (2005) Results of nonsurgical treatment of thoracic spinal tuberculosis in adults. Spine J 5:79–84
Matsumoto T, Yamagami T, Morishita H, Iida S, Asai S, Masui K, Yamazoe S, Sato O, Nishimura T (2012) CT-guided percutaneous drainage within intervertebral space for pyogenic spondylodiscitis with psoas abscess. Acta Radiol 53:76–80
Cantasdemir M, Kara B, Cebi D, Selcuk N, Numan F (2003) Computed tomography-guided percutaneous catheter drainage of primary and secondary iliopsoas abscesses. Clin Radiol 58:811–815
Dave BR, Kurupati RB, Shah D, Degulamadi D, Borgohain N, Krishnan A (2014) Outcome of percutaneous continuous drainage of psoas abscess: a clinically guided technique. Indian J Orthop 48:67
Zhang H-Q, Lin M-Z, Shen K-Y, Ge L, Li J-S, Tang M-X, Wu J-H, Liu J-Y (2012) Surgical management for multilevel noncontiguous thoracic spinal tuberculosis by single-stage posterior transforaminal thoracic debridement, limited decompression, interbody fusion, and posterior instrumentation (modified TTIF). Arch Orthop Trauma Surg 132:751–757
Zaki SA, Shanbag P, Lad V (2011) Abdominal pain as a presenting feature of spinal tuberculosis in a child. Ann Saudi Med 31:550
Teo HE, Peh WC (2004) Skeletal tuberculosis in children. Pediatr Radiol 34:853–860
Mushkin A, Kovalenko K (1999) Neurological complications of spinal tuberculosis in children. Int Orthop 23:210–212
Powell DA, Hunt WG (2006) Tuberculosis in children: an update. Adv Pediatr 53:279–322
Raj PP (2008) Intervertebral disc: anatomy-physiology-pathophysiology-treatment. Pain Pract 8:18–44
Chapman M, Murray RO, Stoker DJ (1979) Tuberculosis of the bones and joints. In: Seminars in roentgenology. Elsevier. pp. 266–282
Rothman S (1996) The diagnosis of infections of the spine by modern imaging techniques. Orthop Clin North Am 27:15–31
Benzagmout M, Boujraf S, Chakour K, Chaoui MEF (2011) Pott’s disease in children. Surgical neurology international 2
Abbas A, Rizvi SRH, Mahesri M, Salahuddin HRA (2013) Conservative management of spinal tuberculosis: initial series from Pakistan. Asian Spine J 7:73–80
Zhang XF, Wang Y, Xiao SH, Liu ZS, Zhang YG, Liu BW, Xia ZM (2010) Treatment of lumbar and lumbosacral spinal tuberculosis with minimally invasive surgery. Orthop Surg 2:64–70
Bailey HL, Gabriel M, Hodgson A, Shin J (1972) Tuberculosis of the spine in children. J Bone Joint Surg 54:1633–1657
Karlen A (1959) Early drainage of paraspinal tuberculous abscesses in children. J Bone Joint Surg
Boachie-Adjei O, Squillante RG (1996) Tuberculosis of the spine. Orthop Clin North Am 27:95–103
Mueller P, Ferrucci J Jr, Wittenberg J, Simeone J, Butch R (1984) Iliopsoas abscess: treatment by CT-guided percutaneous catheter drainage. Am J Roentgenol 142:359–362
Sapico FL (1996) Microbiology and antimicrobial therapy of spinal infections. Orthop Clin North Am 27:9–13
Jain AK, Maheshwari AV, Jena S (2007) Kyphus correction in spinal tuberculosis. Clin Orthop Relat Res 460:117–123
Rajasekaran S (2002) The problem of deformity in spinal tuberculosis. Clin Orthop Relat Res 398:85–92
Tuli SM (2013) Historical aspects of Pott’s disease (spinal tuberculosis) management. Eur Spine J 22:529–538
Tuli S (2004) Tuberculosis of the skeletal system: bones, joints, spine and bursal sheaths. Jaypee Brothers Publishers
Acknowledgments
This work was financially supported by the Project of Furong Scholar of Hunan Province.
Conflicts of interest
The authors declare that they have no conflict of interests concerning this paper.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yin, X.H., Zhang, H.Q., Hu, X.K. et al. Treatment of pediatric spinal tuberculosis abscess with percutaneous drainage and low-dose local antituberculous therapy: a preliminary report. Childs Nerv Syst 31, 1149–1155 (2015). https://doi.org/10.1007/s00381-015-2694-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-015-2694-6