Abstract
Purpose
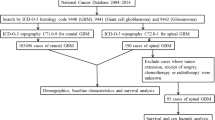
Pediatric spinal glioblastoma multiforme (GBM) is rare. Evidence-directed management relies on studies in which such cases are only a subset of a larger group. We reviewed cases of pediatric spinal GBM to assess outcomes and identify prognostic factors related to treatment.
Methods
Clinical presentations, radiologic findings, surgical variables, radio- and chemotherapeutic management, and outcomes of eight pathologically proven cases of pediatric spinal GBM were reviewed.
Results
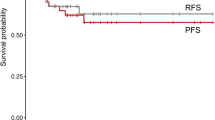
Median age was 10 years. All patients presented with motor deficits. Four had sensory symptoms. Average McCormick score at presentation was II. There were three cervical, one cervicothoracic, and four thoracic tumors. Five had cysts. Patients underwent gross total resection (GTR) (n = 4), subtotal resection (STR) (n = 3), or biopsy (n = 1). Four patients improved neurologically after surgery. One patient was lost to follow-up. Seven received both chemo- and radiotherapy. Average overall survival was 15 months. Average survival after STR and GTR were 12.6 and 19.2 months, respectively. In the GTR subset, the 18-month-old patient survived 30 months, while the other two (>10 years) survived an average of 13.75 months. This difference based on age was not seen in the STR subset. Patients survived an average of 17.5 and 10.5 months, respectively, with and without tumoral cysts. Patients with cervical tumors survived an average of 12.5 months, 18.7 months with thoracic tumors, and 11.5 months with a cervicothoracic tumor.
Conclusions
Tumor location, presence of a cyst, gross total resection, and younger age are possible predictors of prolonged survival. Radiotherapy and chemotherapy remain widely used.





Similar content being viewed by others
References
Lober R, Sharma S, Bell B et al (2010) Pediatric primary intramedullary spinal cord glioblastoma. Rare Tumors 2:e48
McGirt MJ, Chaichana KL, Atiba A et al (2008) Neurological outcome after resection of intramedullary spinal cord tumors in children. Childs Nerv Syst 24:93–97
Perkins SM, Rubin JB, Leonard JR et al (2011) Glioblastoma in children: a single-institution experience. Int J Radiat Oncol Biol Phys 80:1117–1121
Stupp R, Hegi ME, Mason WP et al (2009) Effects of radiotherapy with concomitant and adjuvant temozolomide versus radiotherapy alone on survival in glioblastoma in a randomised phase III study: 5-year analysis of the EORTC-NCIC trial. Lancet Oncol 10:459–466
Sharma S, Free A, Mei Y et al (2010) Distinct molecular signatures in pediatric infratentorial glioblastomas defined by aCGH. Exp Mol Pathol 89:169–174
McCormick PC, Stein BM (1990) Intramedullary tumors in adults. Neurosurg Clin N Am 1:609–630
Raco A, Piccirilli M, Landi A et al (2010) High-grade intramedullary astrocytomas: 30 years' experience at the neurosurgery department of the University of Rome “Sapienza”. J Neurosurg Spine 12:144–153
Garces-Ambrossi GL, McGirt MJ, Mehta VA et al (2009) Factors associated with progression-free survival and long-term neurological outcome after resection of intramedullary spinal cord tumors: analysis of 101 consecutive cases. J Neurosurg Spine 11:591–599
Jallo GI, Freed D, Epstein F (2003) Intramedullary spinal cord tumors in children. Childs Nerv Syst 19:641–649
Gaspar N, Marshall L, Perryman L et al (2010) MGMT-independent temozolomide resistance in pediatric glioblastoma cells associated with a PI3-kinase-mediated HOX/stem cell gene signature. Cancer Res 70:9243–9252
Parekh C, Jubran R, Erdreich-Epstein A et al (2010) Treatment of children with recurrent high grade gliomas with a bevacizumab containing regimen. J Neurooncol 103:673–680
Nakamura M, Shimada K, Ishida E et al (2007) Molecular pathogenesis of pediatric astrocytic tumors. Neuro Oncol 9:113–123
Winters JL, Wilson D, Davis DG (2001) Congenital glioblastoma multiforme: a report of three cases and a review of the literature. J Neurol Sci 188:13–19
Benes V 3rd, Barsa P, Benes V Jr et al (2009) Prognostic factors in intramedullary astrocytomas: a literature review. Eur Spine J 18:1397–1422
Gottardo NG, Gajjar A (2008) Chemotherapy for malignant brain tumors of childhood. J Child Neurol 23:1149–1159
Reddy AT, Wellons JC 3rd (2003) Pediatric high-grade gliomas. Cancer J 9:107–112
Sposto R, Ertel IJ, Jenkin RD et al (1989) The effectiveness of chemotherapy for treatment of high grade astrocytoma in children: results of a randomized trial. A report from the Children's Cancer Study Group. J Neurooncol 7:165–177
Strik HM, Effenberger O, Schafer O et al (2000) A case of spinal glioblastoma multiforme: immunohistochemical study and review of the literature. J Neurooncol 50:239–243
Cohen KJ, Pollack IF, Zhou T et al (2011) Temozolomide in the treatment of high-grade gliomas in children: a report from the Children's Oncology Group. Neuro Oncol 13:317–323
Kerbel RS (2006) Antiangiogenic therapy: a universal chemosensitization strategy for cancer? Science 312:1171–1175
Vredenburgh JJ, Desjardins A, Herndon JE 2nd et al (2007) Phase II trial of bevacizumab and irinotecan in recurrent malignant glioma. Clin Cancer Res 13:1253–1259
Narayana A, Kunnakkat S, Chacko-Mathew J et al (2010) Bevacizumab in recurrent high-grade pediatric gliomas. Neuro Oncol 12:985–990
Wolff JE, Driever PH, Erdlenbruch B et al (2010) Intensive chemotherapy improves survival in pediatric high-grade glioma after gross total resection: results of the HIT-GBM-C protocol. Cancer 116:705–712
Tendulkar RD, Pai Panandiker AS, Wu S et al (2010) Irradiation of pediatric high-grade spinal cord tumors. Int J Radiat Oncol Biol Phys 78:1451–1456
Caroli E, Salvati M, Ferrante L (2005) Spinal glioblastoma with brain relapse in a child: clinical considerations. Spinal Cord 43:565–567
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ononiwu, C., Mehta, V., Bettegowda, C. et al. Pediatric spinal glioblastoma multiforme: current treatment strategies and possible predictors of survival. Childs Nerv Syst 28, 715–720 (2012). https://doi.org/10.1007/s00381-012-1705-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-012-1705-0