Abstract
Aim
This study aims to evaluate the prevalence and clinical characteristics of neurological complications in patients with newly diagnosed neuroblastic tumors (NT).
Patients and method
Hospital file search was performed in patients with NT, and neurological complications, clinical, and treatment features were analyzed.
Results
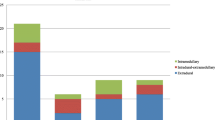
Out of 523 patients with NT, 19 patients had Horner's syndrome, 9 patients had opsoclonus-myoclonus-ataxia syndrome (OMA), 11 patients had central nervous system (CNS) involvement, and 49 patients had spinal cord compression (SCC) at diagnosis. During follow-up, seven more patients had CNS metastases. Survival rates were poor in patients with CNS involvement; all died at a median of 7.9 months after diagnosis. The neurological symptoms and signs of patients with SCC were mild, moderate, and severe in 13, 9, and 22 patients, respectively. Sphincter deficiency and sensory loss were diagnosed in 52.3% and 43.2% of patients. The neurological deficits of 11/17 patients who had symptoms less than 4 weeks were completely resolved or improved. The incidence of sequelae after laminectomy, radiotherapy, and chemotherapy were 46.2%, 66.6%, and 13.6%, respectively.
Conclusion
The prevalence rates of Horner's syndrome, OMA, CNS metastasis, and SCC were found to be 3.6%, 1.8%, 2.2%, and 9.4%, respectively. Metastasis to the CNS indicated a very poor prognosis. No differences in neurological improvement in patients with SCC were found between those treated with radiotherapy, laminectomy, or chemotherapy alone, but laminectomy and radiotherapy caused significant late sequelae. Early diagnosis and proper management is critical to avoid long-term sequelae in patients with SCC.
Similar content being viewed by others
References
Russo C, Cohn SL, Petruzzi MJ, de Alarcon PA (1997) Long-term neurologic outcome in children with opsoclonus-myoclonus associated with neuroblastoma: a report from the Pediatric Oncology Group. Med Pediatr Oncol 28(4):284–288
Pranzatelli MR (1992) The neurobiology of the opsoclonus-myoclonus syndrome. Clin Neuropharmacol 15(3):186–228
Rudnick E, Khakoo Y, Antunes NL, Seeger RC, Brodeur GM, Shimada H, Gerbing RB, Stram DO, Matthay KK (2001) Opsoclonus-myoclonus-ataxia syndrome in neuroblastoma: clinical outcome and antineuronal antibodies—a report from the Children’s Cancer Group Study. Med Pediatr Oncol 36(6):612–622
Matthay KK, Blaes F, Hero B, Plantaz D, De Alarcon P, Mitchell WG, Pike M, Pistoia V (2005) Opsoclonus myoclonus syndrome in neuroblastoma a report from a workshop on the dancing eyes syndrome at the advances in neuroblastoma meeting in Genoa, Italy, 2004. Cancer Lett 228(1–2):275–282
De Bernardi B, Balwierz W, Bejent J, Cohn SL, Garre ML, Iehara T, Plantaz D, Simon T, Angelini P, Cama A, London WB, Kramer K, Katzenstein HM, Tortori-Donati P, Rossi A, D’Angio GJ, Evans AE (2005) Epidural compression in neuroblastoma: diagnostic and therapeutic aspects. Cancer Lett 228(1–2):283–299
Sundaresan N, Sachdev VP, Holland JF, Moore F, Sung M, Paciucci PA, Wu L, Kelligher K, Hough L et al (1995) Surgical treatment of spinal cord compression from epidural metastasis. J Clin Oncol 13(9):2330–2335
Katzenstein HM, Kent PM, London WB, Cohn SL (2001) Treatment and outcome of 83 children with intraspinal neuroblastoma: the Pediatric Oncology Group experience. J Clin Oncol 19(4):1047–1055
Sandberg DI, Bilsky MH, Kushner BH, Souweidane MM, Kramer K, Laquaglia MP, Panageas KS, Cheung NK (2003) Treatment of spinal involvement in neuroblastoma patients. Pediatr Neurosurg 39(6):291–298
Plantaz D, Rubie H, Michon J, Mechinaud F, Coze C, Chastagner P, Frappaz D, Gigaud M, Passagia JG, Hartmann O (1996) The treatment of neuroblastoma with intraspinal extension with chemotherapy followed by surgical removal of residual disease. A prospective study of 42 patients—results of the NBL 90 Study of the French Society of Pediatric Oncology. Cancer 78(2):311–319
Hoover M, Bowman LC, Crawford SE, Stack C, Donaldson JS, Grayhack JJ, Tomita T, Cohn SL (1999) Long-term outcome of patients with intraspinal neuroblastoma. Med Pediatr Oncol 32(5):353–359
Paulino AC, Fowler BZ (2005) Risk factors for scoliosis in children with neuroblastoma. Int J Radiat Oncol Biol Phys 61(3):865–869
Punt J, Pritchard J, Pincott JR, Till K (1980) Neuroblastoma: a review of 21 cases presenting with spinal cord compression. Cancer 45(12):3095–3101
De Bernardi B, Pianca C, Pistamiglio P, Veneselli E, Viscardi E, Pession A, Alvisi P, Carli M, Donfrancesco A, Casale F, Giuliano MG, di Montezemolo LC, Di Cataldo A, Lo Curto M, Bagnulo S, Schumacher RF, Tamburini A, Garaventa A, Clemente L, Bruzzi P (2001) Neuroblastoma with symptomatic spinal cord compression at diagnosis: treatment and results with 76 cases. J Clin Oncol 19(1):183–190
Gunes D, Uysal KM, Cetinkaya H, Gazeteci Tekin H, Yuceer N, Sarialioglu F, Olgun N (2009) Paravertebral malignant tumors of childhood: analysis of 28 pediatric patients. Childs Nerv Syst 25:63–69
Tasdemiroglu E, Ayan I, Kebudi R (1998) Extracranial neuroblastomas and neurological complications. Childs Nerv Syst 14(12):713–718
Matthay KK, Brisse H, Couanet D et al (2003) Central nervous system metastases in neuroblastoma: radiologic, clinical, and biologic features in 23 patients. Cancer 98(1):155–65
Kramer K, Kushner B, Heller G, Cheung NK (2001) Neuroblastoma metastatic to the central nervous system. The memorial sloan-kettering cancer center experience and a literature review. Cancer 91(8):1510–1519
DuBois SG, Kalika Y, Lukens JN, Brodeur GM, Seeger RC, Atkinson JB, Haase GM, Black CT, Perez C, Shimada H, Gerbing R, Stram DO, Matthay KK (1999) Metastatic sites in stage IV and IVS neuroblastoma correlate with age, tumor biology, and survival. J Pediatr Hematol Oncol 21(3):181–189
Shaw PJ, Eden T (1992) Neuroblastoma with intracranial involvement: an ENSG Study. Med Pediatr Oncol 20(2):149–155
Kellie SJ, Hayes FA, Bowman L, Kovnar EH, Langston J, Jenkins JJ 3rd, Pao WJ, Ducos R, Green AA (1991) Primary extracranial neuroblastoma with central nervous system metastases characterization by clinicopathologic findings and neuroimaging. Cancer 68(9):1999–2006
Paulino AC, Nguyen TX, Barker JL Jr (2003) Brain metastasis in children with sarcoma, neuroblastoma, and Wilms' tumor. Int J Radiat Oncol Biol Phys 57(1):177–183
Jaing TH, Yang CP, Hung IJ, Wang HS, Tseng CK, Hsueh C (2003) Brain metastases in children with neuroblastoma—a single-institution experience. Med Pediatr Oncol 41(6):570–571
Evans AE, D’Angio GJ, Randolph J (1971) A proposed staging for children with neuroblastoma. Children’s cancer study group A. Cancer 27(2):374–378
Brodeur GM, Pritchard J, Berthold F, Carlsen NL, Castel V, Castelberry RP, De Bernardi B, Evans AE, Favrot M, Hedborg F et al (1993) Revisions of the international criteria for neuroblastoma diagnosis, staging, and response to treatment. J Clin Oncol 11(8):1466–1477
Peto R, Pike MC, Armitage P, Breslow NE, Cox DR, Howard SV, Mantel N, McPherson K, Peto J, Smith PG (1977) Design and analysis of randomized clinical trials requiring prolonged observation of each patient. II. Analysis and examples. Br J Cancer 35(1):1–39
Aydin GB, Kutluk MT, Büyükpamukçu M, Akyüz C, Kale G, Şenocak ME, Yalçın B, Varan A (2009) Neuroblastoma in Turkish children: experience of a single center. J Pediatr Hematol Oncol 31(7):471–480
Emir S, Akyüz C, Büyükpamukçu M (2003) Correspondence: treatment of the neuroblastoma-associated opsoclonus-myoclonus-ataxia (OMA) syndrome with high-dose methylprednisolone. Med Pediatr Oncol 40(2):139
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Aydin, G.B., Kutluk, M.T., Buyukpamukcu, M. et al. Neurological complications of neuroblastic tumors: experience of a single center. Childs Nerv Syst 26, 359–365 (2010). https://doi.org/10.1007/s00381-009-0979-3
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-009-0979-3