Abstract
Introduction
Although it is widely accepted that lipomas in lipomeningomyelocele (LMMC) are anatomically stable lesions, we present a case of rapidly growing intradural lipoma accompanied by neurological deterioration.
Case summary
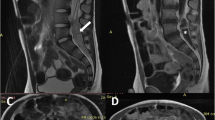
An 8-year-old girl with rapidly regrowing LMMC was admitted to our neurosurgical clinic. She was delivered by cesarean section, and at 47 days old, she underwent detethering surgery because of aggravating weakness. We performed her detethering operation immediately rather than at 3 months as had been previously scheduled because of the rapidly growing lipoma. The second operation was performed at age 8 years because of a regrowing intradural lipoma and aggravating leg deformity. Even if LMMC is expected to be surgically corrected at 2 or 3 months after birth, lipomas could grow rapidly beyond expectation.
Discussion
Close monitoring and follow-up before and after surgery is needed for optimum surgical timing, in order to avoid deteriorating neurological symptoms. The possibility of the rapid growth of intradural lipomas offers additional support for early prophylactic surgery in patients with LMMC.
Conclusion
The potential for rapid growth of spinal lipomas should be considered during first few months of life or even long after surgery. Early diagnosis and optimal surgery are still essential for the treatment of patients with LMMC since there is a high likelihood that residual neurological functions can be preserved.

Similar content being viewed by others
References
Aoki N (1990) Rapid growth of intraspinal lipoma demonstrated by magnetic resonance imaging. Surg Neurol 34:107–110
Byrne RW, Hayes EA, George TM, McLone DG (1995) Operative resection of 100 spinal lipomas in infants less than 1 year of age. Pediatr Neurosurg 23:182–186; discussion 186–187
Giudicelli Y, Pierre-Kahn A, Bourdeaux AM, de Mazancourt P, Lacasa D, Hirsch JF (1986) Are the metabolic characteristics of congenital intraspinal lipoma cells identical to, or different from normal adipocytes? Childs Nerv Syst 2:290–296
Hirsch JF, Pierre-Kahn A (1987) Lumbosacral lipoma associated with spina bifida. Shoni No Noshinkei 12:155–162
Hoffman HJ, Hendrick EB, Humphreys RP (1976) The tethered spinal cord: its protean manifestations, diagnosis and surgical correction. Childs Brain 2:145–155
Kanev PM, Bierbrauer KS (1995) Reflections on the natural history of lipomyelomeningocele. Pediatr Neurosurg 22:137–140
Koyanagi I, Iwasaki Y, Hida K, Abe H, Isu T, Akino M (1997) Surgical treatment supposed natural history of the tethered cord with occult spinal dysraphism. Childs Nerv Syst 13:268–274
Kulkarni AV, Pierre-Kahn A, Zerah M (2004) Spontaneous regression of congenital spinal lipomas of the conus medullaris. Report of two cases. J Neurosurg 101:226–227
La Marca F, Grant JA, Tomita T, McLone DG (1997) Spinal lipomas in children: outcome of 270 procedures. Pediatr Neurosurg 26:8–16
Lee GY, Paradiso G, Tator CH, Gentili F, Massicotte EM, Fehlings MG (2006) Surgical management of tethered cord syndrome in adults: indications, techniques, and long-term outcomes in 60 patients. J Neurosurg Spine 4:123–131
Pierre-Kahn A, Zerah M, Renier D, Cinalli G, Sainte-Rose C, Lellouch-Tubiana A, Brunelle F, Le Merrer M, Giudicelli Y, Pichon J, Kleinknecht B, Nataf F (1997) Congenital lumbosacral lipomas. Childs Nerv Syst 13:298–334; discussion 335
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, K.H., Lee, Y.H., Park, Y.S. et al. Rapidly regrowing lipoma in lipomeningomyelocele: a case report. Childs Nerv Syst 25, 1149–1151 (2009). https://doi.org/10.1007/s00381-009-0935-2
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-009-0935-2