Abstract
Introduction
Intracranial infection is an uncommon but serious complication of head injury.
Case report
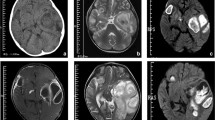
This study describes a boy with a traumatic head injury caused by his mother’s teeth stemming from a traffic accident, without initial alteration of consciousness or focal neurological signs, who subsequently developed an occipital lobe abscess 3 weeks later. Brain abscess culturing yielded human oral flora. To date, our case is the only report documenting skull fracture with subsequent brain abscess formation caused by human oral flora stemming from traumatic injury from his mother’s teeth.
Discussion
A high index of suspicion should be maintained, and early imaging such as computed tomography should be considered for patients with symptoms of intracranial infection or who are at high risk, even after a minor head injury. Early diagnosis, appropriate antibiotic therapy based on knowledge of the causative microbes, and surgery are the major prognostic factors for brain abscess.




Similar content being viewed by others
References
Menon S, Bharadwaj R, Chowdhary A, Kaundinya DV, Palande DA (2008) Current epidemiology of intracranial abscesses: a prospective 5 year study. J Med Microbiol 57:1259–1268
Prasad KN, Mishra AM, Gupta D, Husain N, Husain M, Gupta RK (2006) Analysis of microbial etiology and mortality in patients with brain abscess. J Infect 53:221–227
Takeshita M, Kagawa M, Izawa M, Takakura K (1998) Current treatment strategies and factors influencing outcome in patients with bacterial brain abscess. Acta Neurochir (Wien) 140:1263–1270
Demir MK, Hakan T, Kilicoglu G, Ceran N, Berkman MZ, Erdem I, Goktas P (2007) Bacterial brain abscesses: prognostic value of an imaging severity index. Clin Radiol 62:564–572
Chun CH, Johnson JD, Hofstetter M, Raff MJ (1986) Brain abscess. A study of 45 consecutive cases. Medicine (Baltimore) 65:415–431
Pit S, Jamal F, Cheah FK (1993) Microbiology of cerebral abscess: a four-year study in Malaysia. J Trop Med Hyg 96:191–196
Carpenter J, Stapleton S, Holliman R (2007) Retrospective analysis of 49 cases of brain abscess and review of the literature. Eur J Clin Microbiol Infect Dis 26:1–11
Kilinc H, Yaman M (2006) Brain abscess associated with eyelid contracture. J Craniofac Surg 17:182–184
Rose CE 3rd, Brown JM, Fisher JF (2008) Brain abscess caused by Streptomyces infection following penetration trauma: case report and results of susceptibility analysis of 92 isolates of Streptomyces species submitted to the CDC from 2000 to 2004. J Clin Microbiol 46:821–823
Chaudhry R, Dhawan B, Laxmi BV, Mehta VS (1998) The microbial spectrum of brain abscess with special reference to anaerobic bacteria. Br J Neurosurg 12:127–130
Goldstein EJ, Citron DM, Wield B, Blachman U, Sutter VL, Miller TA, Finegold SM (1978) Bacteriology of human and animal bite wounds. J Clin Microbiol 8:667–672
Brook I (2003) Microbiology and management of human and animal bite wound infections. Prim Care 30:25–39
Stephanov S (1999) Brain abscesses from neglected open head injuries: experience with 17 cases over 20 years. Swiss Surg 5:288–292
Fanning WL, Willett LR, Phillips CF, Wallman LJ (1976) Puncture wound of the eyelid causing brain abscess. J Trauma 16:919–920
Patir R, Sood S, Bhatia R (1995) Post-traumatic brain abscess: experience of 36 patients. Br J Neurosurg 9:29–35
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chang, YC., Lee, JC., Lin, KL. et al. An unusual mechanism for brain abscess formation in a child. Childs Nerv Syst 25, 1035–1038 (2009). https://doi.org/10.1007/s00381-009-0863-1
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-009-0863-1