Abstract
Background
Major skull defects, especially in the anterior region, can present as a most disturbing deformity. Reconstructive cranioplasty can restore cerebral protection and improve craniofacial aesthetics. Complex and large skull defects in children often present reconstructive difficulties.
Materials and methods
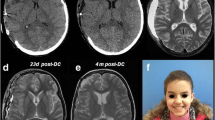
In this paper, an unusual case of a very large post-traumatic defect (318 cm2) in a child managed by a multidisciplinary team is described. The literature is reviewed.
Conclusion
The management of a large complex skull defect in children is still controversial. Each case should be extensively debated in craniofacial units. In our case, bioceramics proved to be an effective and good alternative for final skull reconstruction.



Similar content being viewed by others
Notes
Osteosynt®, produced by Einco Biomaterial, Belo Horizonte, MG, Brazil.
References
Arnaud E (2000) Advances in cranioplasty with osteoinductive biomaterials: summary of experimental studies and clinical prospects. Child’s Nerv Syst 16:659–668
Blum KS, Schneider SJ, Rosenthal AD (1997) Methyl methacrylate cranioplasty in children: long-term results. Pediatr Neurosurg 26:33–35
Durham SR, McComb JG, Levy ML (2003) Correction of large (>25 cm2) cranial defects with “reinforced” hydroxyapatite cement: technique and complications. Neurosurgery 52:842–845
Duskova M, Kozak JI, Mazanek JI, Smahel ZK, Vohradnik M (2000) Bioceramics as an option in correction of facial skeleton deformities. J Craniofac Surg 11:470–479
Edwards MS, Ousterhout DK (1987) Autogeneic skull bone grafts to reconstruct large or complex skull defects in children and adolescents. Neurosurgery 20:273–280
El-Ghannam A (2005) Bone reconstruction: from bioceramics to tissue engineering. Expert Rev Med Devices 2:87–101
Eufinger H, Wehmoller M, Scholz M, Harders A, Machtens E (1999) Reconstruction of an extreme frontal and frontobasal defect by microvascular tissue transfer and a prefabricated titanium implant. Plast Reconstr Surg 104:198–203
Gibstein LA, Abramson DL, Bartlett RA, Orgill DP, Upton J, Mulliken JB (1997) Tissue expansion in children: a retrospective study of complications. Ann Plast Surg 38:358–364
Grant GA, Jolley M, Ellenbogen RG, Roberts TS, Gruss JR, Loeser JD (2004) Failure of autologous bone-assisted cranioplasty following decompressive craniectomy in children and adolescents. J Neurosurg 100:163–168
Gruber R, Peter R, Hora J (1988) The prognosis of cranioplasty following large craniectomy in children. Z Kinderchir 43:375–383
Guyuron B, Shafron M, Columbi B (1988) Management of extensive and difficult cranial defects. J Neurosurg 69:210–212
Hockley AD, Goldin JH, Wake MJC, Iqbal J (1990–91) Skull repair in children. Pediatr Neurosurg 16:271–275
Josan VA, Sgouros S, Walsh AR, Dover MS, Nishikawa H, Hockley AD (2005) Cranioplasty in children. Child’s Nerv Syst 21:200–204
Kline RM Jr, Wolfe SA (1995) Complications associated with the harvesting of cranial bone grafts. Plast Reconstr Surg 95:5–20
LoGiudice J, Gosain AK (2003) Pediatric tissue expansion: indications and complications. J Craniofac Surg 14:866–872
Miyake H, Ohta T, Tanaka H (2000) A new technique for cranioplasty with L-shaped titanium plates and combination ceramic implants composed of hydroxyapatite and tricalcium phosphate (Ceratite). Neurosurgery 46:414–8
Muller A, Krishnan KG, Uhl E, Mast G (2003) The application of rapid prototyping techniques in cranial reconstruction and preoperative planning in neurosurgery. J Craniofac Surg 14:899–914
Ono I, Gunji H, Kaneko F, Numazawa S, Kodama N, Yoza S (1993) Treatment of extensive cranial bone defects using computer-designed hydroxyapatite ceramics and periosteal flaps. Plast Reconstr Surg 92:819–830
Prolo DJ, Oklund SA (1991) The use of bone grafts and alloplastic materials in cranioplasty. Clin Orthop Relat Res 268:270–278
Rish BL, Dillon JD, Meirowsky AM, Caveness WF, Mohr JP, Kistler JP, Weiss GH (1979) Cranioplasty: a review of 1030 cases of penetrating head injury. Neurosurgery 4:381–385
Schwabegger AH, Rainer C, Laimer I, Huemer GM (2005) Hemispheric brain volume replacement with free latissimus dorsi flap as first step in skull reconstruction. Microsurgery 25:325–328
Stula D (1982) The problem of the “sinking skin-flap syndrome” in cranioplasty. J Maxillofac Surg 10:142–145
Suzuki N, Suzuki S, Iwabuchi T (1993) Neurological improvement after cranioplasty. Analysis by dynamic CT scan. Acta Neurochir (Wien) 122:49–53
Taggard DA, Menezes AH (2001) Successful use of rib grafts for cranioplasty in children. Pediatr Neurosurg 34:149–155
Ueda K, Oba S, Omiya Y, Okada M (2001) Cranial-bone defects with depression deformity treated with ceramic implants and free-flap transfers. Br J Plast Surg 54:403–408
Winkler PA, Stummer W, Linke R, Krishnan KG, Tatsch K (2000) Influence of cranioplasty on postural blood flow regulation, cerebrovascular reserve capacity, and cerebral glucose metabolism. J Neurosurg 93:53–61
Xin R, Leng Y, Chen J, Zhang Q (2005) A comparative study of calcium phosphate formation on bioceramics in vitro and in vivo. Biomaterials 26:6477–6486
Acknowledgements
The authors thank Eric Arnaud, M.D., from the Unit of Craniofacial Surgery, Hôpital Necker-Enfants Malades, Paris, France, for kindly revising the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
de Oliveira, R.S., Brigato, R., Gurjão Madureira, J.F. et al. Reconstruction of a large complex skull defect in a child: a case report and literature review. Childs Nerv Syst 23, 1097–1102 (2007). https://doi.org/10.1007/s00381-007-0413-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-007-0413-7