Abstract
Background
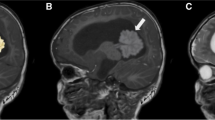
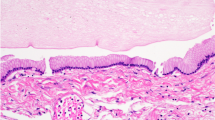
Desmoplastic infantile gangliogliomas are rare intracranial tumors that mostly occur in the first 2 years of life. They are exclusively supratentorial, generally have a voluminous size, and are partially cystic. Histologically they are characterized by a divergent astrocytic and ganglionic differentiation and a prominent desmoplastic stroma; more primitive cells may be observed, which present a higher number of mitoses and these areas can mimic the features of malignant astrocytomas. Surgery is the treatment of choice. Data available from the literature suggest that no complimentary treatment is needed in cases of complete tumor resection. Chemotherapy is an option in infants with infiltration of eloquent CNS structures and progressive disease after surgery. DIGs have generally a good prognosis: recurrence-free intervals of up to 14 years have been reported and spontaneous disappearance of tumor residuals has also been described.
Case reports and discussion
We report two cases of DIGs. The first child underwent a staged partial removal of a huge right fronto-temporo-parietal tumor when she was 2 months old. At that time histological diagnosis was anaplastic astrocytoma and on these grounds she underwent six chemotherapy cycles, with a partial reduction of the tumor residual. When she was 16 months old a new operation and complete removal of the tumor residual was performed; histological diagnosis was DIG. A review of the initial histological samples confirmed this diagnosis. Twenty-two months after surgery no tumor recurrence has been documented. This case is an example of a difficult differential diagnosis, which can lead to incorrect management choices. The second patient was operated on when he was 9 months old for a mostly cystic right temporo-parieto-occipital DIG. At surgery a deep nodule, strictly adherent to the Galen and internal cerebral veins, was not removed. MRI control 9 months after surgery showed the disappearance of the tumor residual. Eleven years after surgery no tumor recurrence has been documented. The history of this patient confirms that tumor residuals do not need complimentary treatment; indeed they do not usually grow and, as in our patient, they can spontaneously disappear.


Similar content being viewed by others
References
Duffner PK, Burger PC, Cohen ME, Sanford RA, Krischer JP, Elterman R, Aronin PA, Pullen J, Horowitz ME, Parent A, Martin P, Kun L (1994) Desmoplastic infantile gangliogliomas: an approach to therapy. Neurosurgery 34:583–589
Ildan F, Tuna M, Gocer IA, Erman T, Cetinalp E (2001) Intracerebral ganglioglioma: clinical and radiological study of eleven surgically treated cases with follow-up. Neurosurg Rev 24:114–118
Kepes JJ, Rubinstein LJ, Eng LF (1979) Pleomorphic xanthoastrocytoma: a distinct meningocerebral glioma of young subjects with relatively favorable prognosis. A study of 12 cases. Cancer 44:1839–1852
Koeller KK, Henry JM (2001) From the archives of the AFIP: superficial gliomas: radiologic-pathologic correlation. Radiographics 21:1533–1556
Mallucci C, Lellouch-Tubiana A, Salazar C, Cinalli G, Renier D, Sainte-Rose C, Pierre-Kahn A, Zerah M (2000) The management of desmoplastic neuroepithelial tumours in childhood. Childs Nerv Syst 16:8–14
Martin DS, Levy B, Awwad EE, Pittman T (1991) Desmoplastic infantile ganglioglioma: CT and MR features. Am J Neuroradiol 12:1195–1197
Moreno A, de Felipe J, Garcia Sola R, Navarro A, Ramon y Cajal S (2001) Neuronal and mixed neuronal glial tumors associated to epilepsy. A heterogeneous and related group of tumours. Histol Histopathol 16:613–622
Paulus W, Schlote W, Perentes E, Jacobis G, Warmuth-Metz M, Roggendorf W (1992) Desmoplastic supratentorial neuroepithelial tumours of infancy. Histopathology 21:43–49
Rothman S, Sharon N, Shiffer J, Toren A, Pollak L, Mandel M, Kenet G, Neumann Y, Nass D (1997) Desmoplastic infantile ganglioglioma. Acta Oncol 36:655–657
Rushing EJ, Rorke LB, Sutton L (1993) Problems in the nosology of desmoplastic tumors of childhood. Pediatr Neurosurg 19:57–62
Setty SN, Miller DC, Camras L, Charbel F, Schmidt ML (1997) Desmoplastic infantile astrocytoma with metastases at presentation. Mod Pathol 10:945–951
Shao L, Tihan T, Burger PC (2002) Desmoplastic infantile ganglioglioma: a clinical and pathological review of eight cases. J Neuropathol Exp Neurol 61:466
Sperner J, Gottschalk J, Neumann K, Schorner W, Lanksch WR, Scheffner D (1994) Clinical, radiological and histological findings in desmoplastic infantile ganglioglioma. Childs Nerv Syst 10:458–463
Taratuto AL, VandenBerg SR, Rorke LB (2002) Desmoplastic infantile astrocytoma and ganglioglioma. In: Kleihues P, Cavanee WK (eds) Pathology and genetics of tumours of the nervous system. IARC, Lyon, pp 6–16
Tenreiro-Picon OR, Kamath SV, Knorr JR, Ragland RL, Smith TW, Lau KY (1995) Desmoplastic infantile ganglioglioma: CT and MRI features. Pediatr Radiol 25:540–543
Tseng JH, Tseng MY, Kuo MF, Tseng CL, Chang YL (2002) Chronological changes on magnetic resonance images in a case of desmoplastic infantile ganglioglioma. Pediatr Neurosurg 36:29–32
Vandenberg SR (1993) Desmoplastic infantile ganglioglioma and desmoplastic cerebral astrocytoma of infancy. Brain Pathol 3:275–281
Vandenberg SR, May EE, Rubinstein LJ, Herman MM, Perentes E, Vinores SA, Collins P, Park TS (1987) Desmoplastic supratentorial neuroepithelial tumors of infancy with divergent differentiation potential ("desmoplastic infantile gangliogliomas"). Report of 11 cases of a distinctive embryonal tumor with favorable prognosis. J Neurosurg 66:58–71
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tamburrini, G., Colosimo, C., Giangaspero, F. et al. Desmoplastic infantile ganglioglioma. Childs Nerv Syst 19, 292–297 (2003). https://doi.org/10.1007/s00381-003-0743-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-003-0743-z