Abstract
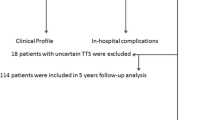
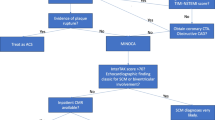
Plasma catecholamines may play an important role in Takotsubo cardiomyopathy (TCM) pathophysiology. Patients with disproportionately high catecholamine responses to stressful events are prone to worse clinical outcomes. Catecholamines stimulate platelet activation and, therefore, may determine the clinical presentation and outcomes of TCM. We conducted a retrospective, descriptive study TCM patients admitted between 2003 and 2013 to Einstein Medical Center, Philadelphia, PA, USA and Danbury Hospital, Danbury, CT, USA. A total of 206 patients met Modified Mayo TCM criteria. Using a multiple logistic model, we tested whether aspirin, dual antiplatelet therapy (DAPT) aspirin + clopidogrel, beta blocker, statin, or ACE inhibitor use were independent predictors of major adverse cardiovascular events (MACE) during the index hospitalization. MACE was defined as in-hospital heart failure, in-hospital death, stroke or respiratory failure requiring mechanical ventilation. Incidence of in-hospital heart failure was 26.7 %, in-hospital death was 7.3 %, stroke was 7.3 % and MACE was 42.3 %. In a multiple logistic regression model (adjusted for gender, race, age, physical stressor, hypertension, diabetes, hyperlipidemia, smoking history, body mass index, initial left ventricular ejection fraction, single antiplatelet therapy, DAPT, beta blocker, statin, and ACE inhibitor) aspirin and DAPT at the time of hospitalization were independent predictors of a lower incidence of MACE during the index hospitalization (aspirin: OR 0.4, 95 % CI (0.16–0.9), P = 0.04; DAPT: OR 0.23; 95 % CI (0.1–0.55); P < 0.01. Physical stressor itself was also found to be an independent predictor of worse MACE: OR 5.1; 95 % CI (2.4–11.5); P < 0.01. In our study, aspirin and DAPT were independent predictors of a lower incidence of MACE during hospitalization for TCM. Prospective clinical trials are needed to confirm the findings of this study.
Similar content being viewed by others
References
Clusters of ‘Broken Hearts’ May be Linked to Massive Natural Disasters Analysis of U.S. Takotsubo Cardiomyopathy cases shows pattern to cue emergency responders. American College of Cardiology available at http://www.cardiosource.org/en/News-Media/Media-Center/News-Releases/2014/03/Pant-ClusteringPR.aspx?w_nav=Search&WT.oss=Clusters%20of%20%22%27broken%22%20%22hearts%27%22%20may%20be%20linked%20to%20massive%20natural%20disasters&WT.oss
Gianni M, Dentali F, Grandi AM, Sumner G, Hiralal R, Lonn E (2006) Apical ballooning syndrome or takotsubo cardiomyopathy: a systematic review. Eur Heart J 27:1523–1529
Kurowski V, Kaiser A, von Hof K, Killermann DP, Mayer B, Hartmann F, Schunkert H, Radke PW (2007) Apical and midventricular transient left ventricular dysfunction syndrome (tako-tsubo cardiomyopathy): frequency, mechanisms, and prognosis. Chest 132:809–816
Nabi H, Hall M, Koskenvuo M, Singh-Manoux A, Oksanen T, Suominen S, Kivimaki M, Vahtera J (2010) Psychological and somatic symptoms of anxiety and risk of coronary heart disease: the health and social support prospective cohort study. Biol Psychiatry 67:378–385
Lam NY, Rainer TH, Ng MH, Leung Y, Cocks RA (2002) Effect of stress hormones on the expression of fibrinogen-binding receptors in platelets. Resuscitation 55:277–283
Pyo MK, Yun-Choi HS, Hong YJ (2003) Apparent heterogeneous responsiveness of human platelet rich plasma to catecholamines. Platelets 14:171–178
von Kanel R, Dimsdale JE (2000) Effects of sympathetic activation by adrenergic infusions on hemostasis in vivo. Eur J Haematol 65:357–369
Yun-Choi HS, Park KM, Pyo MK (2000) Epinephrine induced platelet aggregation in rat platelet-rich plasma. Thromb Res 100:511–518
Tomoda F, Takata M, Kagitani S, Kinuno H, Yasumoto K, Tomita S, Inoue H (1999) Different platelet aggregability during mental stress in two stages of essential hypertension. Am J Hypertens 12:1063–1070
Nunez-Gil IJ, Molina M, Bernardo E, Ibanez B, Ruiz-Mateos B, Garcia-Rubira JC, Vivas D, Feltes G, Luaces M, Alonso J, Zamorano J, Macaya C, Fernandez-Ortiz A (2012) Tako-tsubo syndrome and heart failure: long-term follow-up. Rev Esp Cardiol 65:996–1002
Damås JK, Waehre T, Yndestad A, Otterdal K, Hognestad A, Solum NO, Gullestad L, Frøland SS, Aukrust P (2003) Interleukin-7-mediated inflammation in unstable angina: possible role of chemokines and platelets. Circulation 107:2670–2676
Núñez-Gil IJ, Bernardo E, Feltes G, Escaned J, Mejía-Rentería HD, De Agustín JA, Vivas D, Nombela-Franco L, Jiménez-Quevedo P, Macaya C, Fernández-Ortiz A (2015) Platelet function in Takotsubo cardiomyopathy. J Thromb Thrombolysis 39(4):452–458
Pirzer R, Elmas E, Haghi D, Lippert C, Kralev S, Lang S, Borggrefe M, Kälsch T (2012) Platelet and monocyte activity markers and mediators of inflammation in Takotsubo cardiomyopathy. Heart Vessels 27(2):186–192
Finkel MS, Oddis CV, Jacob TD, Watkins SC, Hattler BG, Simmons RL (1992) Negative inotropic effects of cytokines on the heart mediated by nitric oxide. Science 257:387–389
Mitsuma W, Kodama M, Ito M, Kimura S, Tanaka K, Hoyano M, Hirono S, Aizawa Y (2010) Thromboembolism in Takotsubo cardiomyopathy. Int J Cardiol 139(1):98–100
de Gregorio C, Grimaldi P, Lentini C (2010) Left ventricular thrombus formation and cardioembolic complications in patients with Takotsubo-like syndrome: a systematic review. Int J Cardiol 131(1):18–24
de Gregorio C (2010) Cardioembolic outcomes in stress-related cardiomyopathy complicated by ventricular thrombus: a systematic review of 26 clinical studies. Int J Cardiol 141:11–17
Ouchi K, Nakamura F, Ikutomi M, Oshima T, Ishiwata J, Shinohara H, Kouzaki T, Amaki T (2015) Usefulness of contrast computed tomography to detect left ventricular apical thrombus associated with takotsubo cardiomyopathy. Heart Vessels. doi:10.1007/s00380-015-0637-5
Young ML, Stoehr J, Aguilar MI, Fortuin FD (2014) Takotsubo cardiomyopathy and stroke. Int J Cardiol 176(3):574–576
Nishida J, Kouzu H, Hashimoto A, Fujito T, Kawamukai M, Mochizuki A, Muranaka A, Kokubu N, Shimoshige S, Yuda S, Hase M, Tsuchihashi K, Miura T (2014) “Ballooning” patterns in takotsubo cardiomyopathy reflect different clinical backgrounds and outcomes: a BOREAS-TCM study. Heart Vessels. doi:10.1007/s00380-014-0548-x
Núñez-Gil IJ, Almendro-Delia M, Andrés M, Sionis A, Martin A, Bastante T, Córdoba-Soriano JG, Linares JA, González Sucarrats S, Sánchez-Grande-Flecha A, Fabregat-Andrés O, Pérez B, Escudier-Villa JM, Martin-Reyes R, Pérez-Castellanos A, Rueda Sobella F, Cambeiro C, Piqueras-Flores J, Vidal-Perez R, Bodí V, García de la Villa B, Corbí-Pascua M, Biagioni C, Mejía-Rentería HD, Feltes G, Barrabés J (2015) Secondary forms of Takotsubo cardiomyopathy: a whole different prognosis. Eur Heart J Acute Cardiovasc Care. doi:10.1177/2048872615589512
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standards
In consideration of the Journal’s taking action in reviewing and editing our submission, the author undersigned hereby transfers, assigns, and otherwise conveys all copyright ownership to the Heart and Vessels in the event that such work is published in the Heart and Vessels. We wish to ensure you of our compliance with AMA ethical standards in the treatment of study participants. I warrant that the material contained in the manuscript represents original work, has not been published elsewhere, is not under concurrent consideration for publication elsewhere, and all authors have read and approved the manuscript.
Rights and permissions
About this article
Cite this article
Dias, A., Franco, E., Koshkelashvili, N. et al. Antiplatelet therapy in Takotsubo cardiomyopathy: does it improve cardiovascular outcomes during index event?. Heart Vessels 31, 1285–1290 (2016). https://doi.org/10.1007/s00380-015-0729-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-015-0729-2