Abstract
Purpose
There is a lack of studies in the literature on effects of Virtual Basket™ (VB) and Bubble Blast™ (BB) laser pulse modulations of the Ho:YAG laser on tissue. We aimed to compare the effects of standard modulation (SM), VB, and BB pulse modulations of Ho:YAG laser on kidney tissue.
Methods
An ex vivo experiment was conducted using veal kidneys. The Quanta System Cyber Ho 100W laser generator with a broad setting spectrum at 15–80 W, 10–40 Hz, 1.5–2 J, and medium pulse duration were tested. Incision depth (ID), vaporization area (VA), coagulation area (CA), and total laser area (TLA = VA + CA) were evaluated. Histopathological measurement outcomes were grouped as a low-power group (15, 20, and 30 W) and a high-power group (40, 60, and 80 W) according to the power outputs used.
Results
A total of 108 experiments were performed. In saline and high-power output (40, 60, 80 W), mean VA, TLA, and ID, histopathological measurements were higher in BB pulse modulation than VB and SM pulse modulations (p: 0.03, p: 0.001, and p: 0.003, respectively). In contrast, mean CA and LE measurements were higher in SM than in VB and BB pulse modulations (p < 0.001 and p < 0.001, respectively). There was no statistically significant difference in mean histopathological measurements of VA, CA, TLA, and ID, among SM, VB, and BB pulse modulations in the low-power output group in saline (p > 0.05).
Conclusion
VB can allow controlled dissection, as it does not create a large VA during surgical procedures. BB should be used in a controlled manner in soft tissue surgery due to its strong effect on tissues.
Similar content being viewed by others
Availability of data and materials
The raw data are with the corresponding author and can be provided on request.
Code availability
Not applicable for this section.
References
Alster TS, Li MK (2020) Dermatologic laser side effects and complications: prevention and management. Am J Clin Dermatol 21:711–723. https://doi.org/10.1007/s40257-020-00530-2
Rabley A, O’Shea T, Terry R, Byun S, Louis Moy M (2018) Laser therapy for genitourinary syndrome of menopause. Curr Urol Rep 19:83. https://doi.org/10.1007/s11934-018-0831-y
Yamashita S, Maruyama Y, Tasaka Y, Inoue T, Yasuhara M, Kohjimoto Y, Matsumura T, Hara I (2022) Comparison of stone retropulsion between Moses mode and Virtual Basket mode: an in vitro study using artificial stones. Urolithiasis 50:493–499. https://doi.org/10.1007/s00240-022-01335-0
Aldoukhi AH, Black KM, Ghani KR (2019) Emerging laser techniques for the management of stones. Urol Clin North Am 46:193–205. https://doi.org/10.1016/j.ucl.2018.12.005
Emiliani E, Talso M, Haddad M, Pouliquen C, Derman J, Côté JF, Doizi S, Millán F, Berthe L, Audouin M, Traxer O (2018) The true ablation effect of Holmium YAG laser on soft tissue. J Endourol 32:230–235. https://doi.org/10.1089/end.2017.0835
Kuebker JM, Miller NL (2017) Holmium laser enucleation of the prostate: patient selection and outcomes. Curr Urol Rep 18:96. https://doi.org/10.1007/s11934-017-0746-z
Bach T, Muschter R, Sroka R, Gravas S, Skolarikos A, Herrmann TR, Bayer T, Knoll T, Abbou CC, Janetschek G, Bachmann A, Rassweiler JJ (2012) Laser treatment of benign prostatic obstruction: basics and physical differences. Eur Urol 61:317–325. https://doi.org/10.1016/j.eururo.2011.10.009
Enikeev D, Okhunov Z, Rapoport L, Taratkin M, Enikeev M, Snurnitsyna O, Capretz T, Inoyatov J, Glybochko P (2019) Novel thulium fiber laser for enucleation of prostate: a retrospective comparison with open simple prostatectomy. J Endourol 33:16–21. https://doi.org/10.1089/end.2018.0791
Ballesta Martinez B, Peteinaris A, Tsaturyan A, Natsos A, Koukiou G, Vagionis A, Pagonis K, Obaidat M, Liourdi D, Vrettos T, Liatsikos E, Kallidonis P (2022) Stone ablation rates using innovative pulse modulation technology: vapor tunnel, Virtual Basket, and Bubble Blast. An in vitro experimental study. Lasers Surg Med 54:580–587. https://doi.org/10.1002/lsm.23503
Kallidonis P, Vagionis A (2022) The future of laser technology in kidney stones. Curr Opin Urol 32:411–414. https://doi.org/10.1097/mou.0000000000001006
Ragonese M, Dibitetto F, Bassi P, Pinto F (2022) Laser technology in urologic oncology. Urologia 89:338–346. https://doi.org/10.1177/03915603221088721
Iscaife A, Ribeiro Filho LA, Aparecido Pereira MW, Gallucci FP, Chade D, Murta CB, Cordeiro MD, Cardili L, Sarkis AS, Srougi M, Nahas WC (2022) Holmium laser resection of large bladder tumors: technique description, feasibility, and histopathological quality analysis. Urology 165:373. https://doi.org/10.1016/j.urology.2022.04.021
Das AK, Han TM, Hardacker TJ (2020) Holmium laser enucleation of the prostate (HoLEP): size-independent gold standard for surgical management of benign prostatic hyperplasia. Can J Urol 27:44–50
Basulto-Martínez M, Proietti S, Pavia MP, Yeow Y, Eisner BH, Giusti G (2023) Understanding the ablation rate of Holmium:YAG and thulium fiber lasers. Perspectives from an in vitro study. Urolithiasis 51:32. https://doi.org/10.1007/s00240-022-01402-6
Vizziello D, Acquati P, Clementi M (2018) MP27-17 Virtual Basket technology-Impact on high frequency lithotripsy in a urological simulator. J Endourol 32:A277
Bozzini G, Maltagliati M, Berti L, Besana U, Calori A, Pastore AL, Gozen A, Govorov A, Liatsikos E, Micali S, Rocco B, Tunc L, Buizza C (2022) “VirtualBasket” ureteroscopic holmium laser lithotripsy: intraoperative and early postoperative outcomes. Minerva Urol Nephrol 74:344–350. https://doi.org/10.23736/s2724-6051.21.04025-x
Bozzini G, Maltagliati M, Besana U, Berti L, Calori A, Sighinolfi MC, Micali S, Roche JB, Gozen A, Mueller A, Pushkar D, Liatsikos E, Boldini M, Buizza C, Rocco B (2021) Holmium laser enucleation of the prostate with Virtual Basket mode: faster and better control on bleeding. BMC Urol 21:28. https://doi.org/10.1186/s12894-021-00797-5
Acknowledgements
We would like to thank Atıl Emre COSGUN for his contributions to the design, engineering and production of mini robots.
Funding
The study was internally funded.
Author information
Authors and Affiliations
Contributions
MES and MY conceived the study concept and design. MES and MK carried out the experiment. MES performed the laser procedure. MES and MO analyzed the data. MES, MK, MO and MY interpreted the data and wrote the manuscript. MK and MY provided critical feedback and helped shape the research, analysis and manuscript. MES and MY supervised the project. All authors discussed the results and commented on the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Ethical approval
Not applicable for this section. The manuscript does not contain clinical studies or patient data. This article does not contain any studies with human subjects performed by the any of the authors. The authors did not perform any procedures on living humans or animals. Only fresh ex-vivo veal kidneys were utilized in this study.
Consent to participate
Not applicable for this section.
Consent for publication
Not applicable for this section.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
345_2023_4555_MOESM1_ESM.pdf
Fig.1: A) 100 W Ho:YAG (Cyber Ho, Quanta System, Samarate, Italy) laser device. B) veal kidney from a fresh cadaver. C) a mini laser plotter robot system with laser holder that can automatically move linearly on one axis (X-Y). Supplementary file1 (PDF 3235 KB)
345_2023_4555_MOESM2_ESM.pdf
Fig.2: A) experimental setup. B and C) kidney tissues with 20 mm fissure created by laser. Supplementary file2 (PDF 253 KB)
345_2023_4555_MOESM3_ESM.pdf
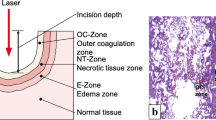
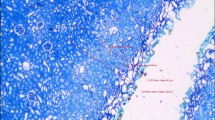
Fig.3: A) lateral effect (LE) (which is defined as the longest horizontal radius from the midpoint of the evaporation gap to normal tissue, including the coagulation zone), incision depth (ID), vaporization area (VA), coagulation area (CA), and total laser area (TLA=VA+CA). B) Surface section (SS) (which is defined as a thin horizontal section of the superficial part of the tissue affected by the laser). Supplementary file3 (PDF 4303 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Şirin, M.E., Karaaslan, M., Ordu, M. et al. Effect of Ho:YAG laser on kidney tissue with Virtual Basket™ and Bubble Blast™ pulse modulation: an experimental ex vivo study. World J Urol 41, 3091–3095 (2023). https://doi.org/10.1007/s00345-023-04555-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-023-04555-0