Abstract
Purpose
Stress urinary incontinence (SUI) is a key factor for post-prostatectomy (RP) quality of life. Current international guidelines struggle to find the adequate place for each kind of surgeries. The aim of this systematic review and meta-analysis considering updated evidence is to assess the efficacy and safety of proACT in treating male patients with post-RP SUI.
Methods
A review of the literature was performed by searching the PubMed database. We narrowed included studies with adult male patients with SUI; outcomes included pads or pad weight per day and quality of life (QOL) questionnaires, as well as safety outcomes.
Results
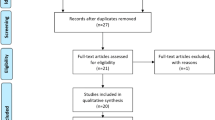
18 studies involving 1570 patients mean age of 68.8 (EC 2.1) were included. The mean follow-up reported was 34.7 months (EC 17.7; median 38.5; range 1–128 months). An average of 60.7% (EC 27) and 40.4% of patients suffered from mild-to-moderate and severe incontinence, respectively. The overall dryness rate was 55.1% (EC 19.3) while respecting the definition of 0–1 pads per day, and the mean dryness rate was 53% (EC 0.2). The mean overall complication rate was 31.2% (EC 18.3%), including an explantation rate of 26.5% (EC 15.3) and a reoperation rate of 22.7% (EC 8.7). The methodological quality of the 18 studies was very heterogeneous.
Conclusion
Implantation of proACT adjustable balloons is a minimally invasive technique that provides medium outcomes (53%) with a strict definition of dryness (0–1 PPD) and important complication rate (31.2%). Past of irradiation is a negative predictive factor for incontinence.

Similar content being viewed by others
Data availability
The data that support the findings privacy or other restrictions of this study are available on request from the corresponding author [TT].
References
Coyne KS, Kvasz M, Ireland AM et al (2012) Urinary incontinence and its relationship to mental health and health-related quality of life in men and women in Sweden, the UK, and the US. Eur Urol 61:88–95. https://doi.org/10.1016/j.eururo.2011.07.049
Köhler N, Friedrich M, Gansera L et al (2014) Psychological distress and adjustment to disease in patients before and after radical prostatectomy. Results of a prospective multi-centre study. Eur J Cancer Care (Engl) 23:795–802. https://doi.org/10.1111/ecc.12186
Crivellaro S, Morlacco A, Bodo G et al (2016) Systematic review of surgical treatment of post radical prostatectomy stress urinary incontinence. Neurourol Urodyn 35:875–881. https://doi.org/10.1002/nau.22873
Haglind E, Carlsson S, Stranne J et al (2015) Urinary incontinence and erectile dysfunction after robotic versus open radical prostatectomy: a prospective, controlled, nonrandomised trial. Eur Urol 68:216–225. https://doi.org/10.1016/j.eururo.2015.02.029
Anderson CA, Omar MI, Campbell SE, et al (2015) Conservative management for postprostatectomy urinary incontinence. Cochrane Database Syst Rev 1:CD001843. https://doi.org/10.1002/14651858.CD001843.pub5
Cornu JN EAU Guidelines on the Management of Non-neurogenic Male LUTS - DISEASE MANAGEMENT - Uroweb. In: Uroweb - European Association of Urology. https://uroweb.org/guidelines/management-of-non-neurogenic-male-luts/chapter/disease-management. Accessed 30 Sep 2022
Jaspreet SS Incontinence after Prostate Treatment: AUA/SUFU Guideline (2019) - American Urological Association. https://www.auanet.org/guidelines-and-quality/guidelines/incontinence-after-prostate-treatment. Accessed 20 Feb 2023
Chen Y-C, Lin P-H, Jou Y-Y, Lin VC-H (2017) Surgical treatment for urinary incontinence after prostatectomy: a meta-analysis and systematic review. PLoS One 12:e0130867. https://doi.org/10.1371/journal.pone.0130867
Martens F, Van der Aa F, Heesakkers J, et al (2022) Prospective multi center registry for patients undergoing surgery for male stress urinary incontinence (saturn): 1 year follow-up in 500 patients. Continence 2:100191. https://doi.org/10.1016/j.cont.2022.100191
Kretschmer A, Hüsch T, Thomsen F et al (2017) Targeting moderate and severe male stress urinary incontinence with adjustable male slings and the perineal artificial urinary sphincter: focus on perioperative complications and device explantations. Int Neurourol J 21:109–115. https://doi.org/10.5213/inj.1632626.313
Larson T, Jhaveri H, Yeung LL (2019) Adjustable continence therapy (ProACT) for the treatment of male stress urinary incontinence: a systematic review and meta-analysis. Neurourol Urodyn 38:2051–2059. https://doi.org/10.1002/nau.24135
Dindo D, Demartines N, Clavien P-A (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213. https://doi.org/10.1097/01.sla.0000133083.54934.ae
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25:603–605. https://doi.org/10.1007/s10654-010-9491-z
Gilling PJ, Bell DF, Wilson LC, et al (2008) An adjustable continence therapy device for treating incontinence after prostatectomy: a minimum 2-year follow-up. BJU Int 102:1426–1430 (discussion 1430–1431). https://doi.org/10.1111/j.1464-410X.2008.07816.x
Hübner WA, Schlarp OM (2005) Treatment of incontinence after prostatectomy using a new minimally invasive device: adjustable continence therapy. BJU Int 96:587–594. https://doi.org/10.1111/j.1464-410X.2005.05689.x
Crivellaro S, Singla A, Aggarwal N et al (2008) Adjustable continence therapy (ProACT) and bone anchored male sling: comparison of two new treatments of post prostatectomy incontinence. Int J Urol 15:910–914. https://doi.org/10.1111/j.1442-2042.2008.02161.x
Finazzi Agrò E, Gregori A, Bianchi D et al (2019) Efficacy and safety of adjustable balloons (Proact™) to treat male stress urinary incontinence after prostate surgery: Medium and long-term follow-up data of a national multicentric retrospective study. Neurourol Urodyn 38:1979–1984. https://doi.org/10.1002/nau.24103
Munier P, Nicolas M, Tricard T, et al (2020) What if artificial urinary sphincter is not possible? Feasibility and effectiveness of ProACT for patients with persistent stress urinary incontinence after radical prostatectomy treated by sling. Neurourol Urodyn. https://doi.org/10.1002/nau.24355
Nash S, Aboseif S, Gilling P et al (2019) Four-year follow-up on 68 patients with a new post-operatively adjustable long-term implant for post-prostatectomy stress incontinence: ProACT™. Neurourol Urodyn 38:248–253. https://doi.org/10.1002/nau.23838
Noordhoff TC, Scheepe JR, Blok BFM (2018) Outcome and complications of adjustable continence therapy (ProACT™) after radical prostatectomy: 10 years’ experience in 143 patients. Neurourol Urodyn 37:1419–1425. https://doi.org/10.1002/nau.23463
Ricard H, Léon G, Branchereau J et al (2022) Adjustable continence balloons in postprostatectomy incontinence: outcomes and complications. Neurourol Urodyn 41:1414–1422. https://doi.org/10.1002/nau.24967
Kjær L, Fode M, Nørgaard N et al (2012) Adjustable continence balloons: clinical results of a new minimally invasive treatment for male urinary incontinence. Scand J Urol Nephrol 46:196–200. https://doi.org/10.3109/00365599.2012.660986
Kocjancic E, Crivellaro S, Ranzoni S et al (2007) Adjustable continence therapy for the treatment of male stress urinary incontinence: a single-centre study. Scand J Urol Nephrol 41:324–328. https://doi.org/10.1080/00365590601153488
Rouprêt M, Misraï V, Gosseine P-N et al (2011) Management of stress urinary incontinence following prostate surgery with minimally invasive adjustable continence balloon implants: functional results from a single center prospective study. J Urol 186:198–203. https://doi.org/10.1016/j.juro.2011.03.016
Crivellaro S, Tosco L, Palazzetti A et al (2012) Geometrical stepper-guided navigation system for ProACT implant under transrectal ultrasound control: preliminary data. Urol Int 89:473–479. https://doi.org/10.1159/000341991
Martens FMJ, Lampe MI, Heesakkers JPFA (2009) ProACT for stress urinary incontinence after radical prostatectomy. Urol Int 82:394–398. https://doi.org/10.1159/000218526
Lebret T, Cour F, Benchetrit J et al (2008) Treatment of postprostatectomy stress urinary incontinence using a minimally invasive adjustable continence balloon device, ProACT: results of a preliminary, multicenter, pilot study. Urology 71:256–260. https://doi.org/10.1016/j.urology.2007.08.062
Trigo-Rocha F, Gomes CM, Pompeo ACL et al (2006) Prospective study evaluating efficacy and safety of Adjustable Continence Therapy (ProACT) for post radical prostatectomy urinary incontinence. Urology 67:965–969. https://doi.org/10.1016/j.urology.2005.11.011
Venturino L, Dalpiaz O, Pummer K, Primus G (2015) Adjustable continence balloons in men: adjustments do not translate into long-term continence. Urology 85:1448–1452. https://doi.org/10.1016/j.urology.2015.01.045
Nestler S, Thomas C, Neisius A et al (2019) Long-term results of ProACT primary and repeat implantation for treatment of stress urinary incontinence in men. World J Urol 37:1173–1179. https://doi.org/10.1007/s00345-018-2483-4
Yiou R, Butow Z, Baron T et al (2015) Adjustable continence therapy (ProACT™) after male sling failure for patients with post-radical prostatectomy urinary incontinence: a prospective study with 1-year follow-up. World J Urol 33:1331–1336. https://doi.org/10.1007/s00345-014-1447-6
Angulo JC, Schönburg S, Giammò A, et al (2019) Systematic review and meta-analysis comparing adjustable transobturator male system (ATOMS) and adjustable continence therapy (ProACT) for male stress incontinence. PLoS One 14:e0225762. https://doi.org/10.1371/journal.pone.0225762
Funding
The authors declare they have no financial interests.
Author information
Authors and Affiliations
Contributions
TT: protocol/project development; literature search; data collection or management; data analysis; manuscript writing/editing. QXS: protocol/project development; data collection or management; data analysis; manuscript writing/editing. PM: Data collection or management; literature search; manuscript editing. JYL: manuscript editing. JL: manuscript editing. CS: manuscript editing. JHP: manuscript editing. WX: protocol/project development; manuscript writing/editing. Authorship principles: All the authors whose names appear on the submission. (1) made substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data; or the creation of new software used in the work; (2) drafted the work or revised it critically for important intellectual content; (3) approved the version to be published; and (4) agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Consent to participate
No human subjects or participants were required for this project or needed consent.
Consent for publication
All the authors and contributors have issued their consent for submission and publication of the following work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tricard, T., Song, QX., Munier, P. et al. Adjustable continence therapy (proACT) for the treatment of male stress urinary incontinence post-prostatectomy: a systematic review and meta-analysis (2023 update). World J Urol 41, 1793–1802 (2023). https://doi.org/10.1007/s00345-023-04452-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-023-04452-6