Abstract
Purpose
The lack of a reliable and reproducible technique to ensure a constantly low temperature of the graft during kidney transplantation (KT) may be a cause of renal nonfunction. The aim of this review was to assess all the methods and devices available to ensure hypothermia during vascular anastomosis in KT.
Methods
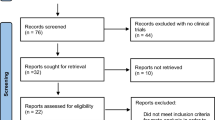
A literature search was conducted through May 2022 using PubMed/Medline, Cochrane Library, Embase and Web of Science databases. Preferred Reporting Items for Systematic Reviews and Meta-analysis (PRISMA) guidelines were followed to identify eligible studies. The review protocol was registered on PROSPERO (CRD42022326550).
Results
A total of 20 studies reporting on four hypothermia techniques met our inclusion criteria. Simple instillation of cold serum is not sufficient, the graft reaching up to 33 ℃ at the end of warm ischemia time (WIT). Plastic bags filled with ice slush have questionable efficiency. The use of a gauze jacket filled with ice-slush was reported in 12/20 studies. It ensures a graft temperature up to 20.3 ℃ at the end of WIT. Some concerns have been linked to potentially inhomogeneous parenchymal cooling and secondary ileus. Novel devices with continuous flow of ice-cold solution around the graft might overcome these limitations, showing a renal temperature below 20 ℃ at all times during KT.
Conclusion
The gauze filled with ice slush is the most common technique, but several aspects can be improved. Novel devices in the form of cold-ischemia jackets can ensure a lower and more stable temperature of the graft during KT, leading to higher efficiency and reproducibility.


Similar content being viewed by others
Availability of data and material
Data are available upon request to the corresponding author.
References
Kamińska D, Kościelska-Kasprzak K, Chudoba P et al (2016) The influence of warm ischemia elimination on kidney injury during transplantation—clinical and molecular study. Sci Rep 3(6):36118. https://doi.org/10.1038/srep36118
Hellegering J, Visser J, Kloke HJ et al (2012) Deleterious influence of prolonged warm ischemia in living donor kidney transplantation. Transplant Proc 44(5):1222–1226. https://doi.org/10.1016/j.transproceed.2012.01.118
Wickham JE (1971) Regional renal hypothermia. Ann R Coll Surg Engl 48(2):99–113
Heylen L, Naesens M, Jochmans I et al (2015) The effect of anastomosis time on outcome in recipients of kidneys donated after brain death: a cohort study. Am J Transplant 15(11):2900–2907. https://doi.org/10.1111/ajt.13397
Tennankore KK, Kim SJ, Alwayn IP, Kiberd BA (2016) Prolonged warm ischemia time is associated with graft failure and mortality after kidney transplantation. Kidney Int 89(3):648–658. https://doi.org/10.1016/j.kint.2015.09.002
Weissenbacher A, Oberhuber R, Cardini B et al (2015) The faster the better: anastomosis time influences patient survival after deceased donor kidney transplantation. Transpl Int 28(5):535–543. https://doi.org/10.1111/tri.12516
Marzouk K, Lawen J, Alwayn I, Kiberd BA (2013) The impact of vascular anastomosis time on early kidney transplant outcomes. Transplant Res 2(1):8. https://doi.org/10.1186/2047-1440-2-8
Ortiz J, Siddeswarappa M, Sea S et al (2011) The elimination of warm ischemic time in kidney transplantation using the ice bag technique: a feasibility study. J Exp Clin Med 3(4):187e190
Feuillu B, Cormier L, Frimat L et al (2003) Kidney warming during transplantation. Transpl Int 16(5):307–312. https://doi.org/10.1007/s00147-003-0549-7
Menon M, Sood A, Bhandari M et al (2014) Robotic kidney transplantation with regional hypothermia: a step-by-step description of the Vattikuti Urology Institute-Medanta technique (IDEAL phase 2a). Eur Urol 65(5):991–1000. https://doi.org/10.1016/j.eururo.2013.12.006
Breda A, Territo A, Gausa L et al (2018) Robot-assisted kidney transplantation: the European experience. Eur Urol 73(2):273–281. https://doi.org/10.1016/j.eururo.2017.08.028
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71
Brown P, Brunnhuber K, Chalkidou K et al (2006) How to formulate research recommendations. BMJ 333:804–806
Kuipers TG, Hellegering J, El Moumni M et al (2017) Kidney temperature course during living organ procurement and transplantation. Transpl Int 30(2):162–169. https://doi.org/10.1111/tri.12892
Karipineni F, Campos S, Parsikia A et al (2014) Elimination of warm ischemia using the Ice Bag Technique does not decrease delayed graft function. Int J Surg 12(6):551–556. https://doi.org/10.1016/j.ijsu.2014.04.002
Fan Y, Zhao J, Zu Q et al (2022) Robot-assisted kidney transplantation: initial experience with a modified hypothermia technique. Urol Int 106(5):504–511. https://doi.org/10.1159/000521959
Abaza R, Ghani KR, Sood A et al (2014) Robotic kidney transplantation with intraoperative regional hypothermia. BJU Int 113(4):679–681. https://doi.org/10.1111/bju.12572
Ahlawat RK, Tugcu V, Arora S et al (2018) Learning curves and timing of surgical trials: robotic kidney transplantation with regional hypothermia. J Endourol 32(12):1160–1165. https://doi.org/10.1089/end.2017.0697
Tuğcu V, Şener NC, Şahin S, Yavuzsan AH, Akbay FG, Apaydın S (2018) Robot-assisted kidney transplantation: comparison of the first 40 cases of open vs robot-assisted transplantations by a single surgeon. BJU Int 121(2):275–280. https://doi.org/10.1111/bju.14014
Siena G, Vignolini G, Mari A et al (2019) Full robot-assisted living donor nephrectomy and kidney transplantation in a twin dedicated operating room: initial experience from a high-volume robotic center. Surg Innov 26(4):449–455. https://doi.org/10.1177/1553350619835429
Vignolini G, Greco I, Sessa F et al (2020) The university of florence technique for robot-assisted kidney transplantation: 3-year experience. Front Surg. 7:583798. https://doi.org/10.3389/fsurg.2020.583798
Modi P, Kumar S, Mishra A et al (2020) Robotic assisted dual kidney transplantation with monolateral iliac vessels. Urology 144:234–240. https://doi.org/10.1016/j.urology.2020.06.030
Maheshwari R, Qadri SY, Rakhul LR et al (2020) Prospective nonrandomized comparison between open and robot-assisted kidney transplantation: analysis of midterm functional outcomes. J Endourol 34(9):939–945. https://doi.org/10.1089/end.2020.0213
Musquera M, Peri L, Ajami T et al (2020) Results and lessons learned on robotic assisted kidney transplantation. Biomed Res Int 2(2020):8687907. https://doi.org/10.1155/2020/8687907
Nataraj SA, Zafar FA, Ghosh P, Ahlawat R (2020) Feasibility and functional outcome of robotic assisted kidney transplantation using grafts with multiple vessels: comparison to propensity matched contemporary open kidney transplants cohort. Front Surg 25(7):51. https://doi.org/10.3389/fsurg.2020.00051
Ganpule A, Patil A, Singh A et al (2020) Robotic-assisted kidney transplant: a single center experience with median follow-up of 2.8 years. World J Urol 38(10):2651–2660. https://doi.org/10.1007/s00345-019-02934-0
Tinney F, Ivanics T, Stracke J et al (2022) Robotic-assisted versus open technique for living donor kidney transplantation: a comparison using propensity score matching for intention to treat. Transplant Direct. 8(5):e1320. https://doi.org/10.1097/TXD.0000000000001320
Li Y, Han X, Dagvadorj BU et al (2020) An effective cooling device for minimal-incision kidney transplantation. Ann Transplant 25:e928773. https://doi.org/10.12659/AOT.928773
Zhu X, Zhao Y, Han X et al (2021) Extraperitoneal laparoscopic kidney transplantation: preliminary clinical experiences from china. Adv Ther 38(3):1677–1689. https://doi.org/10.1007/s12325-021-01639-4
Territo A, Piana A, Fontana M et al (2021) Step-by-step development of a cold ischemia device for open and robotic-assisted renal transplantation. Eur Urol 80(6):738–745. https://doi.org/10.1016/j.eururo.2021.05.026
Acknowledgements
We acknowledge Doc. Nicoletta Colombi, University of Turin, for her valuable contribution to the systematic literature search.
Funding
The study was not funded.
Author information
Authors and Affiliations
Consortia
Contributions
Study concept and design: IA, AT. Acquisition of data: AP, PV, IA. Drafting of the manuscript: IA, AT. Critical revision of the manuscript for important intellectual content: TT, AG, TP, VH, MB, RB, NC, RC, AB, AT. Statistical analysis: None.
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Ethical approval
The study was conducted in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent to participate
Patient consent was not required due to the study design (review).
Consent for publication
All authors approve the submission.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Andras, I., Piana, A., Verri, P. et al. Systematic review of techniques and devices used to avoid warm ischemia time injury during kidney transplantation. World J Urol 41, 993–1003 (2023). https://doi.org/10.1007/s00345-023-04328-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-023-04328-9