Abstract
Purpose
To assess the contemporary in-hospital management of octogenarians and nonagenarians with renal calculi.
Material and Methods
A multicentric retrospective evaluation of patients aged ≥ 80 years hospitalized with kidney stones between 01/2000 and 12/2019. Stone and patient related data were collected, including stone size and location, geriatric status and comorbidities. Surgical treatment patterns and outcome were assessed.
Results
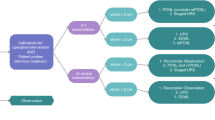
A total of 299 patients (57% female) with kidney stones were analyzed. Mean age was 84.7 years. Patients were largely multimorbid (ASA ≥ 3 in 70%) and about 25% were classified as frail. Active stone treatment was performed in 65% and 35% were treated with urinary diversion (stent or nephrostomy). Prognostic factors for receiving an active stone treatment were age < 90 years, male sex, stone size and quantity, and performance status. Mean overall survival was 23.7 months and when stratified to treatment mean survival were 21 months after urinary diversion, 28 months after URS, 29 months after PCNL and 45 months after SWL.
Conclusion
Age, frailty and performance-status as well as stone size and quantity are predictors for active stone treatment. Octogenarians and nonagenarians, who are considered fit for surgery, tend to live long enough to profit from active stone treatment.

Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Abufaraj M, Xu T, Cao C, Waldhoer T, Seitz C, D’Andrea D et al (2021) Prevalence and trends in kidney stone among adults in the USA: analyses of national health and nutrition examination survey 2007–2018 data. Eur Urol Focus 7(6):1468–1475
Hesse A, Brandle E, Wilbert D, Kohrmann KU, Alken P (2003) Study on the prevalence and incidence of urolithiasis in Germany comparing the years 1979 vs. 2000. Eur Urol 44(6):709–713
Beard JR, Officer A, de Carvalho IA, Sadana R, Pot AM, Michel JP et al (2016) The World report on ageing and health: a policy framework for healthy ageing. Lancet 387(10033):2145–2154
Eredics K, Luef T, Madersbacher S (2021) The future of urology: nonagenarians admitted to a urological ward. World J Urol 39(9):3671–3676
Knoll T, Schubert AB, Fahlenkamp D, Leusmann DB, Wendt-Nordahl G, Schubert G (2011) Urolithiasis through the ages: data on more than 200,000 urinary stone analyses. J Urol 185(4):1304–1311
Daels FP, Gaizauskas A, Rioja J, Varshney AK, Erkan E, Ozgok Y et al (2015) Age-related prevalence of diabetes mellitus, cardiovascular disease and anticoagulation therapy use in a urolithiasis population and their effect on outcomes: the Clinical Research Office of the Endourological Society Ureteroscopy Global Study. World J Urol 33(6):859–864
Jablonski SG, Urman RD (2019) The growing challenge of the older surgical population. Anesthesiol Clin 37(3):401–409
Turk C, Petrik A, Sarica K, Seitz C, Skolarikos A, Straub M et al (2016) EAU guidelines on interventional treatment for urolithiasis. Eur Urol 69(3):475–482
Aykac A, Baran O (2020) Safety and efficacy of retrograde intrarenal surgery in geriatric patients by age groups. Int Urol Nephrol 52(12):2229–2236
Emiliani E, Piccirilli A, Cepeda-Delgado M, Kanashiro AK, Mantilla D, Amaya CA et al (2021) Flexible ureteroscopy in extreme elderly patients (80 years of age and older) is feasible and safe. World J Urol 39(7):2703–2708
Gokcen K, Dundar G, Bagcioglu M, Karagoz MA, Gokce G, Sarica K (2020) Safety and efficacy of RIRS in geriatric patients: a comparative evaluation on an age based manner. Urol J 17(2):129–133
Mager R, Brauers C, Kurosch M, Dotzauer R, Borgmann H, Haferkamp A (2022) Outcomes for geriatric urolithiasis patients aged ≥80 years compared to patients in their seventies. Eur Urol Focus 8(4):1103–1109. https://doi.org/10.1016/j.euf.2021.08.004. (Epub 2021 Aug 26)
Morganstern B, Galli R, Motamedinia P, Leavitt D, Keheila M, Ghiraldi E et al (2015) Percutaneous nephrolithotomy in octogenarians and beyond: How old is too old? Asian J Urol 2(4):208–213
Prattley S, Voss J, Cheung S, Geraghty R, Jones P, Somani BK (2018) Ureteroscopy and stone treatment in the elderly (≥70 years): prospective outcomes over 5- years with a review of literature. Int Braz J Urol 44(4):750–757
Yamashita S, Kohjimoto Y, Hirabayashi Y, Iguchi T, Iba A, Higuchi M et al (2017) Upper urinary tract stone disease in patients with poor performance status: active stone removal or conservative management? BMC Urol 17(1):103
Kino M, Hayashi T, Hino D, Nakada T, Kitoh H, Akakura K (2021) Patients’ poor performance status is an independent risk factor for urosepsis induced by kidney and ureteral stones. Urolithiasis 49(5):477–484
Atalay HA, Canat L, Bayraktarli R, Alkan I, Can O, Altunrende F (2018) Evaluation of stone volume distribution in renal collecting system as a predictor of stone-free rate after percutaneous nephrolithotomy: a retrospective single-center study. Urolithiasis 46(3):303–309
Kokov D, Manka L, Beck A, Winter A, Gerullis H, Karakiewicz PI et al (2019) Only size matters in stone patients: computed tomography controlled stone-free rates after mini-percutaneous nephrolithotomy. Urol Int 103(2):166–171
Maugeri O, Dalmasso E, Peretti D, Venzano F, Chiapello G, Ambruosi C, et al. (2021) Stone free rate and clinical complications in patients submitted to retrograde intrarenal surgery (RIRS): Our experience in 571 consecutive cases. Archivio Italiano Di Urologia Andrologia 93(3):313–7.
Detweiler K, Mayers D, Fletcher SG (2015) Bacteruria and urinary tract infections in the elderly. Urol Clinics N Am 42(4):561–568
Kitano H, Shigemoto N, Koba Y, Hara T, Seiya K, Omori K et al (2021) Indwelling catheterization, renal stones, and hydronephrosis are risk factors for symptomatic Staphylococcus aureus-related urinary tract infection. World J Urol 39(2):511–516
Suskind AM, Walter LC, Zhao S, Finlayson E (2017) Functional outcomes after transurethral resection of the prostate in nursing home residents. J Am Geriatr Soc 65(4):699–703
Joshi HB, Adams S, Obadeyi OO, Rao PN (2001) Nephrostomy tube or “JJ” ureteric stent in ureteric obstruction: assessment of patient perspectives using quality-of-life survey and utility analysis. Eur Urol 39(6):695–701
Koprowski C, Kim C, Modi PK, Elsamra SE (2016) Ureteral stent-associated pain: a review. J Endourol 30(7):744–753
Funding
None.
Author information
Authors and Affiliations
Contributions
KE: data analysis and management, manuscript writing; MD: data collection, data analysis; MÖ: project development, manuscript revision; CW: project development, data collection; ML: data collection; CR: data collection; PS: data collection; JZ: data collection; CEF: data collection; IH: data collection; AW: data collection; SS: project development, data analysis and management, manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants
The paper does not report on primary research. All data analyzed were collected as part of routine diagnosis and treatment. The Ethics Committee of the City of Vienna waived the need for ethics approval and the need to obtain consent for the collection, analysis and publication of the retrospectively obtained and anonymized data for this non-interventional study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Eredics, K., Drerup, M., Özsoy, M. et al. Active stone removal is a safe option for ocotogenarians and nonagenarians with nephrolithiasis. World J Urol 41, 849–856 (2023). https://doi.org/10.1007/s00345-023-04304-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-023-04304-3