Abstract
Purpose
This study aimed to investigate the association between the dietary inflammatory index and lifetime kidney stone prevalence.
Methods
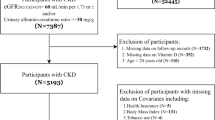
We performed a cross-sectional study utilizing the 2013–2014 National Health and Nutrition Examination Survey data. Data were available on 2192 participants aged > 20 years with a complete kidney stone history and 24 h dietary intake interview. Weighted multivariable linear regression, subgroup analyses, and interaction terms were employed. Covariates including age, race, sex, energy and protein intake, total serum calcium, serum iron, PIR, phosphorus, serum/urine creatinine, HDL, glucose, diastolic and systolic pressure, education level, eGFR, BMI, albuminuria, diabetes, smoking status, and marital status were hierarchically adjusted in three different models.
Results
The average dietary inflammatory index for 2192 participants was − 0.11 ± 1.73, ranging from − 4.52 to 4.28. In the fully adjusted model, participants in the highest dietary inflammatory index tertile (the most proinflammatory) had 72% higher odds of the lifetime prevalence of kidney stones than those in tertile 1 (OR = 1.72, 95% CI: 1.03, 2.88, P = 0.0367). Subgroup analysis showed that the association between the dietary inflammatory index and kidney stone history was only statistically significant in the younger age (age ≥ 60), female, Mexican American groups, married people or people without diabetes, hypertension, low eGFR, and albuminuria.
Conclusions
There is a positive association between the dietary inflammatory index and self-reported kidney stones in US adults, which indicates that dietary patterns could greatly impact kidney stone prevalence.
Similar content being viewed by others
References
Scales CD, Smith AC, Hanley JM, Saigal CS (2012) Prevalence of kidney stones in the United States. Eur Urol 62:160–165. https://doi.org/10.1016/j.eururo.2012.03.052
Rule AD, Lieske JC, Pais VM (2020) Management of kidney stones in 2020. JAMA 323:1961–1962. https://doi.org/10.1001/jama.2020.0662
Shivappa N, Hébert JR, Rietzschel ER, De Buyzere ML, Langlois M, Debruyne E, Marcos A, Huybrechts I (2015) Associations between dietary inflammatory index and inflammatory markers in the asklepios study. Br J Nutr 113:665–671. https://doi.org/10.1017/S000711451400395X
Shivappa N, Wirth MD, Hurley TG, Hébert JR (2017) Association between the dietary inflammatory index (DII) and telomere length and C-reactive protein from the national health and nutrition examination survey-1999–2002. Mol Nutr Food Res. https://doi.org/10.1002/mnfr.201600630
Dominguez-Gutierrez PR, Kusmartsev S, Canales BK, Khan SR (1863) Calcium oxalate differentiates human monocytes Into inflammatory M1 macrophages. Front Immunol 2018:9. https://doi.org/10.3389/fimmu.2018.01863
Shivappa N, Steck SE, Hurley TG, Hussey JR, Hébert JR (2014) Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr 17:1689–1696. https://doi.org/10.1017/S1368980013002115
Shivappa N, Godos J, Hébert JR, Wirth MD, Piuri G, Speciani AF, Grosso G (2017) Dietary inflammatory index and colorectal cancer risk-a meta-analysis. Nutrients. https://doi.org/10.3390/nu9091043
Li J, Lee DH, Hu J, Tabung FK, Li Y, Bhupathiraju SN, Rimm EB, Rexrode KM, Manson JE, Willett WC et al (2020) Dietary inflammatory potential and risk of cardiovascular disease among men and women in the U.S. J Am Coll Cardiol 76:2181–2193. https://doi.org/10.1016/j.jacc.2020.09.535
Shakya PR, Melaku YA, Shivappa N, Hébert JR, Adams RJ, Page AJ, Gill TK (2021) Dietary inflammatory index (DII®) and the risk of depression symptoms in adults. Clin Nutr 40:3631–3642. https://doi.org/10.1016/j.clnu.2020.12.031
National Center for Health Statistics (US) (1994) Plan and operation of the third national health and nutrition examination survey, 1988–94. Series 1: programs and collection procedures. Vital and health statistics series 1. Programs and collection procedures. National Center for Health Statistics, Atlanta, GA
Qin Z, Liu N, Liao R, Jiang L, Su B (2021) The association between dietary inflammatory potential and sex hormones in Male children and adolescents aged 6–19 years. Front Endocrinol (Lausanne) 12:722941. https://doi.org/10.3389/fendo.2021.722941
Zhang C, Bian H, Chen Z, Tian B, Wang H, Tu X, Cai B, Jin K, Zheng X, Yang L et al (2021) The association between dietary inflammatory index and sex hormones among men in the United States. J Urol. https://doi.org/10.1097/JU.0000000000001703
Shoag J, Eisner BH (2014) Relationship between C-reactive protein and kidney stone prevalence. J Urol 191:372–375. https://doi.org/10.1016/j.juro.2013.09.033
Liu N, Ma F, Feng Y, Ma X (2021) The association between the dietary inflammatory index and thyroid function in U. S. adult males. Nutrients. https://doi.org/10.3390/nu13103330
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF, Feldman HI, Kusek JW, Eggers P, Van Lente F, Greene T et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150:604–612
Qin Z, Zhao J, Li J, Yang Q, Geng J, Liao R, Su B (2021) Low lean mass is associated with lower urinary tract symptoms in US men from the 2005–2006 national health and nutrition examination survey dataset. Aging 13:21421–21434. https://doi.org/10.18632/aging.203480
Johnson CL, Paulose-Ram R, Ogden CL, Carroll MD, Kruszon-Moran D, Dohrmann SM, Curtin LR (2013) National health and nutrition examination survey: analytic guidelines, 1999–2010. Vital Health Stat 2:1999–2010
Letavernier E, Daudon M (2018) Vitamin D, hypercalciuria and kidney stones. Nutrients. https://doi.org/10.3390/nu10030366
Ferraro PM, Curhan GC, Gambaro G, Taylor EN (2016) Total, dietary, and supplemental vitamin c intake and risk of incident kidney stones. Am J Kidney Dis 67:400–407. https://doi.org/10.1053/j.ajkd.2015.09.005
Curhan GC, Willett WC, Rimm EB, Stampfer MJ (1993) A prospective study of dietary calcium and other nutrients and the risk of symptomatic kidney stones. N Engl J Med 328:833–838
Muldowney FP, Freaney R, Moloney MF (1982) Importance of dietary sodium in the hypercalciuria syndrome. Kidney Int 22:292–296
Rodriguez A, Curhan GC, Gambaro G, Taylor EN, Ferraro PM (2020) Mediterranean diet adherence and risk of incident kidney stones. Am J Clin Nutr 111:1100–1106. https://doi.org/10.1093/ajcn/nqaa066
Taylor EN, Fung TT, Curhan GC (2009) DASH-style diet associates with reduced risk for kidney stones. J Am Soc Nephrol 20:2253–2259. https://doi.org/10.1681/ASN.2009030276
Mulay SR, Eberhard JN, Desai J, Marschner JA, Kumar SVR, Weidenbusch M, Grigorescu M, Lech M, Eltrich N, Müller L et al (2017) Hyperoxaluria requires TNF receptors to initiate crystal adhesion and kidney stone disease. J Am Soc Nephrol 28:761–768. https://doi.org/10.1681/ASN.2016040486
Huang MY, Chaturvedi LS, Koul S, Koul HK (2005) Oxalate stimulates IL-6 production in HK-2 cells, a line of human renal proximal tubular epithelial cells. Kidney Int 68:497–503
Kusmartsev S, Dominguez-Gutierrez PR, Canales BK, Bird VG, Vieweg J, Khan SR (2016) Calcium oxalate stone fragment and crystal phagocytosis by human macrophages. J Urol 195:1143–1151. https://doi.org/10.1016/j.juro.2015.11.048
Li Y, Shi B, Dong F, Zhu X, Liu B, Liu Y (2019) Effects of inflammatory responses, apoptosis, and STAT3/NF-κB- and Nrf2-mediated oxidative stress on benign prostatic hyperplasia induced by a high-fat diet. Aging 11:5570–5578. https://doi.org/10.18632/aging.102138
Tan BL, Norhaizan ME (2019) Effect of high-fat diets on oxidative stress, cellular inflammatory response and cognitive function. Nutrients. https://doi.org/10.3390/nu11112579
Li Z, Chang L, Ren X, Hu Y, Chen Z (2021) Modulation of rat kidney stone crystallization and the relative oxidative stress pathway by green tea polyphenol. ACS Omega 6:1725–1731. https://doi.org/10.1021/acsomega.0c05903
Acknowledgements
None.
Funding
The National Natural Science Foundation of China (No. 31771662). 1·3·5 project for disciplines of excellence–Clinical Research Incubation Project, West China Hospital, Sichuan University, Grant No. 2019HXFH057.
Author information
Authors and Affiliations
Contributions
NL: protocol/project development, data collection and management, data analysis, and manuscript writing; YF: protocol/project development, data collection and management, and manuscript editing; JL Li: manuscript writing; XM: manuscript editing; FM: protocol/project development and manuscript editing.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
The studies involving human participants were reviewed and approved by the NCHS Ethics Review Board.
Consent for publication
Informed consent was obtained from all individual participants enrolled in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Liu, N., Feng, Y., Li, J. et al. Relationship between the dietary inflammatory index and kidney stone prevalence. World J Urol 40, 1545–1552 (2022). https://doi.org/10.1007/s00345-022-03998-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-022-03998-1