Abstract
Purpose
To examine the ability of the Decipher test to predict early biochemical recurrence after radical prostatectomy and to impact clinical decisions in advance of metastasis and death.
Methods
We identified Decipher tests ordered after radical prostatectomy for adverse pathology in men treated for prostate cancer between 1/1/14 and 8/31/18. Biochemical recurrence was defined as prostate-specific antigen > 0.02 ng/mL. Decipher score is reported as lower risk (< 0.6) and higher risk ≥ 0.60). Kaplan–Meier analysis was used to examine the relationship between Decipher score and time to biochemical recurrence (months). Cox regression was used to analyze the relationship between Decipher score and time to biochemical recurrence while controlling for a number of clinical characteristics. Secondary analyses focused on a subset of men with prostate-specific antigen > 0.02 and < 0.20 ng/mL to determine if high-risk Decipher scores were associated with receipt of salvage treatment.
Results
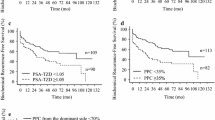
A total of 203 cases were analyzed: 37.9% and 62.1% had lower and higher risk Decipher scores respectively, and 56.2% had a biochemical recurrence. Median (inter-quartile range) follow-up was 20 (13.5, 25.3) months. Decipher score was significantly associated with time to biochemical recurrence (p = 0.027) while in the secondary analyses, high-risk Decipher scores (≥ 0.60) were associated with salvage treatment (p = 0.018). Stage category and Decipher score were significant predictors of time from elevated PSA to salvage treatment in the secondary analyses.
Conclusion
While it might not contribute statistically, Decipher score can be clinically useful in helping patients reach treatment decisions.

Similar content being viewed by others

Availability of data
Sharing of de-identified data with an external entity would require the approval of the Hartford Hospital IRB.
References
Roehl KA, Han M, Ramos CG et al (2004) Cancer progression and survival rates following anatomical radical retropubic prostatectomy in 3,478 consecutive patients: long-term results. J Urol 72:910
Freeland SJ, Humphreys EB, Mangold LA et al (2005) Risk of prostate cancer-specific mortality following biochemical recurrence after radical prostatectomy. JAMA 294:433
Klein EA, Yousefi K, Haddad Z et al (2015) A genomic classifier improves prediction of metastatic disease within 5 years after surgery in node-negative high-risk prostate cancer patients managed by radical prostatectomy without adjuvant therapy. Eur Urol 67:778
Ross AE, Feng FY, Ghadessi M et al (2014) A genomic classifier predicting metastatic disease progression in men with biochemical recurrence after prostatectomy. Prostate Cancer Prostatic Dis 17:64
Ross AE, Johnson MH, Yousefi K et al (2016) Tissue-based genomics augments post-prostatectomy risk stratification in a natural history cohort of intermediate- and high-risk men. Eur Urol 69:157
Klein EA, Santiago-Jimenez M, Yousefi K et al (2017) Molecular analysis of low grade prostate cancer using a genomic classifier of metastatic potential. J Urol 197:122
Spratt DE, Yousefi K, Deheshi S (2017) Individual patient-level meta-analysis of the performance of the decipher genomic classifier in high-risk men after prostatectomy to predict development of metastatic disease. J Clin Oncol 35:1991
Den RB, Yousefi K, Trabulsi EJ et al (2015) Genomic classifier identifies men with adverse pathology after radical prostatectomy who benefit from adjuvant radiation therapy. J Clin Oncol 33:944
Stish BJ, Pisansky TM, Harmsen WS et al (2016) Improved metastasis-free and survival outcomes with early salvage radiotherapy in men with detectable prostate-specific antigen after prostatectomy for prostate cancer. J Clin Oncol 34:3864
Bolla M, van Poppel H, Tombal B et al (2012) Postoperative radiotherapy after radical prostatectomy for high-risk prostate cancer: long-term results of a randomised controlled trial (EORTC trial 22911). Lancet 380:2018
Thompson IM, Tangen CM, Paradelo J et al (2009) Adjuvant radiotherapy for pathological t3n0m0 prostate cancer significantly reduces risk of metastases and improves survival: long-term followup of a randomized clinical trial. J Urol 181:956
Wiegel T, Bartkowiak D, Bottke D et al (2014) Adjuvant radiotherapy versus wait-and-see after radical prostatectomy: 10-year follow-up of the ARO 96–02/AUO AP 09/95 trial. Eur Urol 66:243
Hwang WL, Tendulkar RD, Niemierko A et al (2018) Comparison between adjuvant and early-salvage postprostatectomy radiotherapy for prostate cancer with adverse pathological features. JAMA Oncol 4(5):e175230
Thompson IM, Valicenti R, Albertsen PC, et al. Adjuvant and salvage radiotherapy after prostatectomy: ASTRO/AUA guideline. 2013 Available at https://www.auanet.org/guidelines/prostate-cancer-adjuvant-and-salvage-radiotherapy-after-prostatectomy-(2013). Accessed February 8, 2019.
Sineshaw HM, Gray PJ, Efstathiou JA et al (2015) Declining use of radiotherapy for adverse features after radical prostatectomy: results from the national cancer data base. Eur Urol 68:768
Sokoll LJ, Zhang Z, Chan DW et al (2016) Do ultrasensitive prostate specific antigen measurements have a role in predicting long-term biochemical recurrence-free survival in men after radical prostatectomy? J Urol 195:330
Grivas N, de Bruin D, Barwari K et al (2019) Ultrasensitive prostate-specific antigen level as a predictor of biochemical progression after robot-assisted radical prostatectomy: towards risk adapted follow-up. J Clin Lab Anal. 33(2):e22693. https://doi.org/10.1002/jcla.22693 (Epub 2018 Oct 26)
Stephenson AJ, Kattan MW, Eastham JA et al (2006) Defining biochemical recurrence of prostate cancer after radical prostatectomy: a proposal for a standardized definition. J Clin Oncol 24:3973
Spratt DE, Dai DLY, Den RB (2018) Performance of a prostate cancer genomic classifier in predicting metastasis in men with prostate-specific antigen persistence postprostatectomy. Eur Urol 74(1):107–114. https://doi.org/10.1016/j.eururo.2017.11.024 (Epub 2017 Dec 10)
Vickers AJ, Brewster SF (2012) PSA velocity and doubling time in diagnosis and prognosis of prostate cancer. Br J Med Surg Urol 5:162
Gore JL, du Plessis M, Santiago-Jimenez M et al (2017) Decipher test impacts decision making among patients considering adjuvant and salvage treatment after radical prostatectomy: Interim results from the Multicenter Prospective PRO-IMPACT study. Cancer 123:2850
Parker C, Clarke NW, Cook A, et al (2019) LBA49_PR—timing of radiotherapy (RT) after radical prostatectomy (RP): first results from the RADICALS RT randomised controlled trial (RCT) [NCT00541047]. Ann Oncol 30: v883
Funding
This project did not receive financial support.
Author information
Authors and Affiliations
Contributions
Protocol/project development: CW, JW, IS, TM; data collection and management: JT, KP, AG, AC; data analysis: IS; manuscript writing/editing: CW, IS, TM, JW, JT, KP, AG, AC; supervision: JW.
Corresponding author
Ethics declarations
Conflict of interest
JW serves on the speaker’s bureau for Genomic Health and as a consultant for Covidien.
Ethics approval
This retrospective chart review study involving human participants was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The Hartford Hospital Institutional Review Board (IRB) approved this study.
Consent to participate/consent for publication
The Hartford Hospital Institutional Review Board approved this study with a full waiver of consent.
Code availability
SPSS code could be made available upon request.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
White, C., Staff, I., McLaughlin, T. et al. Does post prostatectomy decipher score predict biochemical recurrence and impact care?. World J Urol 39, 3281–3286 (2021). https://doi.org/10.1007/s00345-021-03661-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-021-03661-1