Abstract
Purpose
To clarify the incidence of and risk factors for febrile urinary tract infection in children with persistent vesicoureteral reflux (VUR) after the discontinuation of continuous antibiotic prophylaxis (CAP), retrospective chart review was performed.
Patients and methods
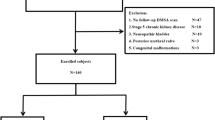
Among children with primary VUR at 10 years of age or younger at presentation, those who had persistent VUR despite conservative management with CAP and who were subsequently followed after discontinuation of CAP were included. Kaplan–Meier curve and Cox’s proportional hazard regression model were used for evaluation of the incidence of and risk factors for febrile urinary tract infection (fUTI) after stopping CAP.
Results
Among 144 children (99 boys and 45 girls), fUTI developed in 34. The 5-year fUTI-free rate after discontinuation of CAP was 69.4%. On multivariate analyses, girls (p = 0.008) and abnormalities on nuclear renal scans (p = 0.0019), especially focal defect (p = 0.0471), were significant factors for fUTI. Although the fUTI-free rate was not different between children who had no or 1 risk factor, it was significantly lower in children with 2 risk factors than in those with no or 1 risk factor.
Conclusions
The present study revealed that girls and abnormal renal scan, especially focal defect, are risk factors for fUTI. Active surveillance without CAP for persistent VUR seems to be a safe option for children with no or 1 risk factor. Prophylactic surgery or careful conservative follow-up may be an option for girls with abnormal renal scan results if VUR persists under CAP.




Similar content being viewed by others
References
Peters CA, Skoog SJ, Arant BS, Copp HL, Elder JS, Hudson RG, Khoury AE, Lorenzo AJ, Pohl HG, Shapiro E, Snodgrass WT, Diaz M (2010) Summary of the AUA guideline on management of primary vesicoureteral reflux in children. J Urol 184(3):1134–1144. https://doi.org/10.1016/j.juro.2010.05.065
Nakamura M, Moriya K, Mitsui T, Tanaka H, Nonomura K (2009) Abnormal dimercapto-succinic acid scan is a predictive factor of breakthrough urinary tract infection in children with primary vesicoureteral reflux. J Urol 182(4 Suppl):1694–1697. https://doi.org/10.1016/j.juro.2009.03.070
Moriya K, Mitsui T, Kitta T, Nakamura M, Kanno Y, Kon M, Nishimura Y, Shinohara N, Nonomura K (2015) Early discontinuation of antibiotic prophylaxis in patients with persistent primary vesicoureteral reflux initially detected during infancy: outcome analysis and risk factors for febrile urinary tract infection. J Urol 193(2):637–642. https://doi.org/10.1016/j.juro.2014.08.007
Lebowitz RL, Olbing H, Parkkulainen KV, Smellie JM, Tamminen-Möbius TE (1985) International system of radiographic grading of vesicoureteric reflux. International reflux study in children. Pediatr Radiol 15(2):105–109
Estrada CR, Passerotti CC, Graham DA, Peters CA, Bauer SB, Diamond DA, Cilento BG, Borer JG, Cendron M, Nelson CP, Lee RS, Zhou J, Retik AB, Nguyen HT (2009) Nomograms for predicting annual resolution rate of primary vesicoureteral reflux: results from 2462 children. J Urol 182(4):1535–1541. https://doi.org/10.1016/j.juro.2009.06.053
Schwab CW, Wu HY, Selman H, Smith GH, Snyder HM, Canning DA (2002) Spontaneous resolution of vesicoureteral reflux: a 15 year perspective. J Urol 168(6):2594–2599. https://doi.org/10.1097/01.ju.0000037530.11361.8b
Knudson MJ, Austin JC, McMillan ZM, Hawtrey CE, Cooper CS (2007) Predictive factors of early spontaneous resolution in children with primary vesicoureteral reflux. J Urol 178(4 Pt 2):1684–1688. https://doi.org/10.1016/j.juro.2007.03.161
Hoberman A, Greenfield SP, Mattoo TK, Keren R, Mathews R, Pohl HG, Kropp BP, Skoog SJ, Nelson CP, Moxey-Mims M, Chesney RW, Carpenter MA (2014) Antimicrobial prophylaxis for children with vesicoureteral reflux. N Engl J Med 370(25):2367–2376. https://doi.org/10.1056/NEJMoa1401811
Brandström P, Jodal U, Sillén U, Hansson S (2011) The Swedish reflux trial: review of a randomized, controlled trial in children with dilating vesicoureteral reflux. J Pediatr Urol 7(6):594–600. https://doi.org/10.1016/j.jpurol.2011.05.006
de Bessa J, de Carvalho Mrad FC, Mendes EF, Bessa MC, Paschoalin VP, Tiraboschi RB, Sammour ZM, Gomes CM, Braga LH, Bastos Netto JM (2015) Antibiotic prophylaxis for prevention of febrile urinary tract infections in children with vesicoureteral reflux: a meta-analysis of randomized, controlled trials comparing dilated to nondilated vesicoureteral reflux. J Urol 193(5 Suppl):1772–1777. https://doi.org/10.1016/j.juro.2014.10.092
Lee T, Park JM (2017) Vesicoureteral reflux and continuous prophylactic antibiotics. Investig Clin Urol 58(Suppl 1):S32–S37. https://doi.org/10.4111/icu.2017.58.S1.S32
Prospective trial of operative versus non-operative treatment of severe vesicoureteric reflux in children: five year’s observation. Birmingham Reflux Study Group (1987). Br Med J (Clin Res Ed) 295 (6592):237–241
Cooper CS, Chung BI, Kirsch AJ, Canning DA, Snyder HM (2000) The outcome of stopping prophylactic antibiotics in older children with vesicoureteral reflux. J Urol 163(1):269–272 (discussion 272–263)
Leslie B, Moore K, Salle JL, Khoury AE, Cook A, Braga LH, Bägli DJ, Lorenzo AJ (2010) Outcome of antibiotic prophylaxis discontinuation in patients with persistent vesicoureteral reflux initially presenting with febrile urinary tract infection: time to event analysis. J Urol 184(3):1093–1098. https://doi.org/10.1016/j.juro.2010.05.013
Kitchens DM, Herndon A, Joseph DB (2010) Outcome after discontinuing prophylactic antibiotics in children with persistent vesicoureteral reflux. J Urol 184(4 Suppl):1594–1597. https://doi.org/10.1016/j.juro.2010.04.020
Al-Sayyad AJ, Pike JG, Leonard MP (2005) Can prophylactic antibiotics safely be discontinued in children with vesicoureteral reflux? J Urol 174(4 Pt 2):1587–1589 (discussion 1589)
Stein R, Dogan HS, Hoebeke P, Kočvara R, Nijman RJ, Radmayr C, Tekgül S, Urology EAo Urology ESfP (2015) Urinary tract infections in children: EAU/ESPU guidelines. Eur Urol 67(3):546–558. https://doi.org/10.1016/j.eururo.2014.11.007
Shaikh N, Morone NE, Bost JE, Farrell MH (2008) Prevalence of urinary tract infection in childhood: a meta-analysis. Pediatr Infect Dis J 27(4):302–308. https://doi.org/10.1097/INF.0b013e31815e4122
Koff SA, Wagner TT, Jayanthi VR (1998) The relationship among dysfunctional elimination syndromes, primary vesicoureteral reflux and urinary tract infections in children. J Urol 160(3 Pt 2):1019–1022
Chen JJ, Mao W, Homayoon K, Steinhardt GF (2004) A multivariate analysis of dysfunctional elimination syndrome, and its relationships with gender, urinary tract infection and vesicoureteral reflux in children. J Urol 171(5):1907–1910. https://doi.org/10.1097/01.ju.0000120288.82950.a2
Nakai H, Kakizaki H, Konda R, Hayashi Y, Hosokawa S, Kawaguchi S, Matsuoka H, Nonomura K, Shimada K, Kawamura T, Prospective Study Committee of Reflux Nephropathy Forum Jp (2003) Clinical characteristics of primary vesicoureteral reflux in infants: multicenter retrospective study in Japan. J Urol 169(1):309–312. https://doi.org/10.1097/01.ju.0000042766.09295.72
Yamazaki Y, Shiroyanagi Y, Matsuno D, Nishi M (2009) Predicting early recurrent urinary tract infection in pretoilet trained children with vesicoureteral reflux. J Urol 182(4 Suppl):1699–1702. https://doi.org/10.1016/j.juro.2009.03.020
Mingin GC, Nguyen HT, Baskin LS, Harlan S (2004) Abnormal dimercapto-succinic acid scans predict an increased risk of breakthrough infection in children with vesicoureteral reflux. J Urol 172(3):1075–1077 (discussion 1077)
Loukogeorgakis SP, Burnand K, MacDonald A, Wessely K, De Caluwe’ D, Rahman N, Farrugia MK (2020) Renal scarring is the most significant predictor of breakthrough febrile urinary tract infection in patients with simplex and duplex primary vesico-ureteral reflux. J Pediatr Urol 16(2):189.e181-189.e187. https://doi.org/10.1016/j.jpurol.2019.11.018
Shaikh N, Haralam MA, Kurs-Lasky M, Hoberman A (2019) Association of renal scarring with number of febrile urinary tract infections in children. JAMA Pediatr. https://doi.org/10.1001/jamapediatrics.2019.2504
Funding
None.
Author information
Authors and Affiliations
Contributions
MN contributed to conception and design, data analysis, and manuscript writing/editing. KM was involved in conception and design, data collection, data analysis, and critical revision of the manuscript for scientific and factual content. MK and YN collected and analyzed the data. HC and TK critically revised the manuscript for scientific and factual content. NS supervised the study.
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declare that they have no competing interests.
Ethical approval
This study has been approved by the institutional review board. The institutional review board approved protocol number is 017-0197. The need for written informed consent was waived because this study was conducted by retrospective chart review.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nakamura, M., Moriya, K., Kon, M. et al. Girls and renal scarring as risk factors for febrile urinary tract infection after stopping antibiotic prophylaxis in children with vesicoureteral reflux. World J Urol 39, 2587–2595 (2021). https://doi.org/10.1007/s00345-020-03524-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-020-03524-1