Abstract
Introduction
Focal therapy (FT) for localized prostate cancer (PCa) is a promising treatment strategy. Although, according to guidelines, it should be regarded as an experimental option, its introduction into clinical practice has occurred at an accelerated speed. It is, thus, crucial for Urologists to understand FT limitations and potential drawbacks that may derive from its use.
Methods
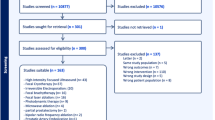
We performed a literature search of peer-reviewed English language articles using Pubmed and the words “focal therapy” AND “prostate cancer” to identify relevant articles. Web search was complemented by manual search.
Results
From a biological perspective, in contrast with the index lesion theory, which still needs to be better supported, PCa is a multifocal and multiclonal entity. Also, the effects of FT on PCa microenvironment are unclear. From a clinical perspective, patient selection is still not precisely defined. Even when all variables potentially decreasing mpMRI and biopsy accuracy are optimized, up to one out of two men may be incorrectly selected for FT, leaving a significant proportion of clinically significant PCa (csPCa) untreated. Underestimation of PCa volume and variant histologies are other additional mpMRI potential limitations. No RCTs have been performed against the standard of care to support FT. There is absence of long-term results and FT series reaching medium-term follow-up have non-optimal oncological control with significant re-treatment needs. When PCa recurs/persists after FT, little is known about the appropriate management strategies and their outcomes. Finally, the optimal follow-up scheme post-FT remains unclear.
Conclusions
Several arguments are present against the use of FT for localized PCa. Studies are needed to overcome current limitations and support FT before it can be included as part of the standard management of prostate cancer.
Similar content being viewed by others
References
Marra G, Gontero P, Valerio M (2016) Changing the prostate cancer management pathway: why focal therapy is a step forward. Arch Esp Urol 69:271–280
van der Poel HG, van den Bergh RCN, Briers E, Cornford P, Govorov A, Henry AM et al (2018) Focal therapy in primary localised prostate cancer: the european association of urology position in 2018. Eur Urol 74:84–91
Valerio M, Ahmed HU, Emberton M, Lawrentschuk N, Lazzeri M, Montironi R et al (2014) The role of focal therapy in the management of localised prostate cancer: a systematic review. Eur Urol 66:732–751
Valerio M, Cerantola Y, Eggener SE, Lepor H, Polascik TJ, Villers A et al (2017) New and established technology in focal ablation of the prostate: a systematic review. Eur Urol 71:17–34
Marra G, Ploussard G, Ost P, De Visschere PJL, Briganti A, Gandaglia G et al (2018) Focal therapy in localised prostate cancer: real-world urological perspective explored in a cross-sectional European survey. Urol Oncol Semin Orig Investig 36:529.e11–529.e22
Jain AL, Sidana A, Maruf M, Sugano D, Calio B, Wood BJ et al (2019) Analyzing the current practice patterns and views among urologists regarding focal therapy for prostate cancer. Urol Oncol 37:182.e1–182.e8
Mouraviev V, Mayes JM, Sun L, Madden JF, Moul JW, Polascik TJ (2007) Prostate cancer laterality as a rationale of focal ablative therapy for the treatment of clinically localized prostate cancer. Cancer 110:906–910
Polascik TJ, Mouraviev V (2008) Focal therapy for prostate cancer. Curr Opin Urol 18:269–274
Liu W, Laitinen S, Khan S, Vihinen M, Kowalski J, Yu G et al (2009) Copy number analysis indicates monoclonal origin of lethal metastatic prostate cancer. Nat Med 15:559–565
Ahmed HU (2009) The index lesion and the origin of prostate cancer. N Engl J Med 361:1704
Mehra R, Tomlins SA, Yu J, Cao X, Wang L, Menon A et al (2008) Characterization of TMPRSS2-ETS gene aberrations in androgen-independent metastatic prostate cancer. Cancer Res 68:3584–3590
Haffner J, Potiron E, Bouyé S, Puech P, Leroy X, Lemaitre L et al (2009) Peripheral zone prostate cancers: location and intraprostatic patterns of spread at histopathology. Prostate 69:276–282
Armenia J, Wankowicz SAM, Liu D, Gao J, Kundra R, Reznik E et al (2018) The long tail of oncogenic drivers in prostate cancer. Nat Genet 50:645–651
Fraser M, Sabelnykova VY, Yamaguchi TN, Heisler LE, Livingstone J, Huang V et al (2017) Genomic hallmarks of localized, non-indolent prostate cancer. Nature 541:359–364
Lindberg J, Mills IG, Klevebring D, Liu W, Neiman M, Xu J et al (2013) The mitochondrial and autosomal mutation landscapes of prostate cancer. Eur Urol 63:702–708
Abeshouse A, Ahn J, Akbani R, Ally A, Amin S, Andry CD et al (2015) The molecular taxonomy of primary prostate cancer. Cell 163:1011–1025
Giraldo NA, Sanchez-Salas R, Peske JD, Vano Y, Becht E, Petitprez F et al (2019) The clinical role of the TME in solid cancer. Br J Cancer 120:45–53
Tourinho-Barbosa RR, De La Rosette J, Sanchez-Salas R (2018) Prostate cancer multifocality, the index lesion, and the microenvironment. Curr Opin Urol 28:499–505
Marra G, Dell’oglio P, Baghdadi M, Cathelineau X, Sanchez-Salas R (2019) EvaluatioN of HIFU Hemiablation and short term androgen deprivation therapy combination to enhance prostate cancer control (ENHANCE) study investigators: multimodal treatment in focal therapy for localized prostate cancer using concomitant short-term androgen deprivation therapy: the ENHANCE prospective pilot study. Minerva Urol Nefrol. 71:544–548
Moldovan PC, Van den Broeck T, Sylvester R, Marconi L, Bellmunt J, van den Bergh RCN et al (2017) What is the negative predictive value of multiparametric magnetic resonance imaging in excluding prostate cancer at biopsy? A systematic review and meta-analysis from the European Association of Urology Prostate Cancer Guidelines Panel. Eur Urol 72:250–266
Mirak SA, Shakeri S, Bajgiran AM, Felker ER, Sung KH, Asvadi NH et al (2019) Three tesla multiparametric magnetic resonance imaging: comparison of performance with and without endorectal coil for prostate cancer detection, PI-RADSTM version 2 category and staging with whole mount histopathology correlation. J Urol 201:496–502
Stabile A, Giganti F, Kasivisvanathan V, Giannarini G, Moore CM, Padhani AR et al (2020) Factors influencing variability in the performance of multiparametric magnetic resonance imaging in detecting clinically significant prostate cancer: a systematic literature review. Eur Urol Oncol 3(2):145–167
Gatti M, Faletti R, Calleris G, Giglio J, Berzovini C, Gentile F et al (2019) Prostate cancer detection with biparametric magnetic resonance imaging (bpMRI) by readers with different experience: performance and comparison with multiparametric (mpMRI). Abdom Radiol 44:1883–1893
Johnson DC, Raman SS, Mirak SA, Kwan L, Bajgiran AM, Hsu W et al (2019) Detection of individual prostate cancer foci via multiparametric. Magn Reson Imaging 75:712–720
Borofsky S, George AK, Gaur S, Bernardo M, Greer MD, Mertan FV et al (2018) What are we missing? False-negative cancers at multiparametric MR imaging of the prostate. Radiology 286:186–195
Padhani AR, Haider MA, Villers A, Barentsz JO (2019) Multiparametric Magnetic mResonance imaging for prostate cancer detection: what we see and what we miss. Eur Urol 75(5):721–722
Truong M, Feng C, Hollenberg G, Weinberg E, Messing EM, Miyamoto H et al (2018) A comprehensive analysis of cribriform morphology on magnetic resonance imaging/ultrasound fusion biopsy correlated with radical prostatectomy specimens. J urol 199:106–113
Truong M, Hollenberg G, Weinberg E, Messing EM, Miyamoto H, Frye TP (2017) Impact of gleason subtype on prostate cancer detection using multiparametric magnetic resonance imaging: correlation with final histopathology. Am Urol Assoc Educ Res 198:316–321
Baco E, Ukimura O, Rud E, Vlatkovic L, Svindland A, Aron M et al (2015) Magnetic resonance imaging-transectal ultrasound image-fusion biopsies accurately characterize the index tumor: correlation with step-sectioned radical prostatectomy specimens in 135 patients. Eur Urol 67:787–794
Radtke JP, Schwab C, Wolf MB, Freitag MT, Alt CD, Kesch C et al (2016) Multiparametric magnetic resonance imaging (mri) and mri-transrectal ultrasound fusion biopsy for index tumor detection: correlation with radical prostatectomy specimen. Eur Urol 70:846–853
Aoun F, Albisinni S, Van Velthoven R (2019) Cartography-based quality control of prostate cancer care: a necessary ground to targeted focal therapy. Curr Opin Urol 29:65–69
Marra G, Ploussard G, Futterer J, Valerio M, Ploussard G, De Visschere PJL et al (2019) Controversies in MR targeted biopsy: alone or combined, cognitive versus software-based fusion, transrectal versus transperineal approach? World J Urol 37:277–287
Schouten MG, van der Leest M, Pokorny M, Hoogenboom M, Barentsz JO, Thompson LC et al (2017) Why and where do we miss significant prostate cancer with multi-parametric magnetic resonance imaging followed by magnetic resonance-guided and transrectal ultrasound-guided biopsy in biopsy-naïve men? Eur Urol 71:896–903
Giannarini G, Crestani A, Rossanese M, Ficarra V (2017) Multiparametric magnetic resonance imaging targeted biopsy for early detection of prostate cancer: all that glitters is not gold! Eur Urol 71:904–906
Meng X, Rosenkrantz AB, Huang R, Deng FM, Wysock JS, Bjurlin MA et al (2018) The institutional learning curve of magnetic resonance imaging-ultrasound fusion targeted prostate biopsy: temporal improvements in cancer detection in 4 years. J Urol 200:1022–1029
Stabile A, Dell’Oglio P, Gandaglia G, Fossati N, Brembilla G, Cristel G et al (2018) Not all multiparametric magnetic resonance imaging–targeted biopsies are equal: the impact of the type of approach and operator expertise on the detection of clinically significant prostate cancer. Eur Urol Oncol 1:120–128
Johnson DC, Yang JJ, Kwan L, Barsa DE, Mirak SA, Pooli A et al (2019) Do contemporary imaging and biopsy techniques reliably identify unilateral prostate cancer? Implications for hemiablation patient selection. Cancer 125:2955–2964
Hyo Choi Y, Woong YuJ, Yong Kang M, Hwan Sung H, Chang Jeong B, Il Seo S et al (2019) Combination of multiparametric magnetic resonance imaging and transrectal ultrasound-guided prostate biopsies is not enough for identifying patients eligible for hemiablative focal therapy for prostate cancer. World J Urol 37:2129–2135
Tran M, Thompson J, Böhm M, Pulbrook M, Moses D, Shnier R et al (2016) Combination of multiparametric MRI and transperineal template-guided mapping biopsy of the prostate to identify candidates for hemi-ablative focal therapy. BJU Int 117:48–54
Marra G, Eldred-Evans D, Challacombe B, Van Hemelrijck M, Polson A, Pomplun S et al (2017) Pathological concordance between prostate biopsies and radical prostatectomy using transperineal sector mapping biopsies: validation and comparison with transrectal biopsies. Urol Int 99:168–176
Azzouzi A-R, Vincendeau S, Barret E, Cicco A, Kleinclauss F, Van Der Poel HG et al (2017) Padeliporfi n vascular-targeted photodynamic therapy versus active surveillance in men with low-risk prostate cancer (CLIN1001 PCM301): an open-label, phase 3, randomised controlled trial. Artic Lancet Oncol 18:181–191
Klotz L, Emberton M (2014) Management of low risk prostate cancer-active surveillance and focal therapy. Nat Rev Clin Oncol 11:324–334
Ahmed HU, Berge V, Bottomley D, Cross W, Heer R, Kaplan R et al (2014) Can we deliver randomized trials of focal therapy in prostate cancer? Nat Rev Clin Oncol 11:482–491
Leslie T, Davies L, Elliott D, Brewster S, Sooriakumaran P, Rosario D, et al. (2017) PD56–08 the part trial—a phase iii study comparing partial prostate ablation versus radical prostatectomy (part) in intermediate risk prostate cancer—early data from the feasibility study. J Urol
Hamdy FC, Elliott D, Le Conte S, Davies LC, Burns RM, Thomson C et al (2018) Partial ablation versus radical prostatectomy in intermediate-risk prostate cancer: The PART feasibility RCT. Health Technol Assess (Rockv) 22:1–95
https://part.octru.ox.ac.uk/. Accessed 1 May 2020
Reddy D, Shah TT, Dudderidge T, McCracken S, Arya M, Dobbs C et al (2020) Comparative healthcare research outcomes of novel surgery in prostate cancer (IP4-CHRONOS): a prospective, multi-centre therapeutic phase II parallel randomised control trial. Contemp Clin Trials 93:105999
Neal DE, Metcalfe C, Donovan JL, Lane JA, Davis M, Young GJ et al (2020) Ten-year mortality, disease progression, and treatment-related side effects in men with localised prostate cancer from the protect randomised controlled trial according to treatment received. Eur Urol 77:320–330
Stabile A, Orczyk C, Hosking-Jervis F, Giganti F, Arya M, Hindley RG et al (2019) Medium-term oncological outcomes in a large cohort of men treated with either focal or hemi-ablation using high-intensity focused ultrasonography for primary localized prostate cancer. BJU Int 124:431–440
Shah TT, Peters M, Eldred-evans D, Miah S, Yap T, Faure-walker NA et al (2019) Early-medium-term outcomes of primary focal cryotherapy to treat nonmetastatic clinically significant prostate cancer from a prospective multicentre registry. Eur Urol 76:6–13
Oishi M, Gill IS, Tafuri A, Shakir A, Cacciamani GE, Iwata T et al (2019) Hemigland cryoablation of localized low, intermediate and high risk prostate cancer: oncologic and functional outcomes at 5 years. J Urol 202:1188–1198
Marra G, Moschini M, Cathelineau X, Sanchez-Salas R (2020) Re: Hemigland Cryoablation of Localized Low, Intermediate and High Risk Prostate Cancer: Oncologic and Functional Outcomes at 5 Years. J Urol.
Sivaraman A, Barret E (2016) Focal therapy for prostate cancer: an “à la carte” approach. Eur Urol 69:973–975
Linares-Espinós E, Carneiro A, Martínez-Salamanca JI, Bianco F, Castro-Alfaro A, Cathelineau X et al (2018) New technologies and techniques for prostate cancer focal therapy: a review of the current literature. Minerva Urol Nefrol 70(3):252–263
Ganzer R, Arthanareeswaran VKA, Ahmed HU, Cestari A, Rischmann P, Salomon G et al (2018) Which technology to select for primary focal treatment of prostate cancer?-European Section of Urotechnology (ESUT) position statement. Prostate Cancer Prostatic Dis 21:175–186
Tourinho-Barbosa RR, Sanchez-Salas R, Claros OR, Collura-Merlier S, Bakavicius A, Carneiro A et al (2019) Focal therapy for localized prostate cancer with either HIFU or cryoablation: a single institution experience. J Urol. https://doi.org/10.1097/JU.0000000000000506
Noweski A, Roosen A, Lebdai S, Barret E, Emberton M, Benzaghou F et al (2019) Medium-term follow-up of vascular-targeted photodynamic therapy of localized prostate cancer using TOOKAD soluble WST-11 (Phase II Trials). Eur Urol Focus 5:1022–1028
Marra G, Valerio M, Emberton M, Heidenreich A, Crook JM, Bossi A et al (2019) Salvage local treatments after focal therapy for prostate cancer. Eur Urol Oncol 2(5):526–538
Marra G, Gontero P, Walz JC, Sivaraman A, Tourinho-Barbosa R, Cathelineau X et al (2019) Complications, oncological and functional outcomes of salvage treatment options following focal therapy for localized prostate cancer: a systematic review and a comprehensive narrative review. World J Urol. 37:1517–1534
Barret E, Harvey-Bryan KA, Sanchez-Salas R, Rozet F, Galiano M, Cathelineau X (2014) How to diagnose and treat focal therapy failure and recurrence? Curr Opin Urol 24:241–246
Lovegrove CE, Peters M, Guillaumier S, Arya M, Afzal N, Dudderidge T et al (2020) Evaluation of functional outcomes after a second focal high-intensity focused ultrasonography (HIFU) procedure in men with primary localized, non-metastatic prostate cancer: results from the HIFU Evaluation and Assessment of Treatment (HEAT) registry. BJU Int 125(6):853–860
Marconi L, Stonier T, Tourinho-Barbosa R, Moore C, Ahmed HU, Cathelineau X et al (2019) Robot-assisted radical prostatectomy after focal therapy: oncological, functional outcomes and predictors of recurrence(Figure presented.). Eur Urol 76:27–30
Marra G, Van Velthoven R, Valerio M (2019) Re: Lorenzo Marconi, Thomas Stonier, Rafael Tourinho-Barbosa, et al. robot-assisted radical prostatectomy after focal therapy: oncological, functional outcomes and predictors of recurrence. Eur Urol 76:27–30
Gontero P, Marra G, Alessio P, Filippini C, Oderda M, Munoz F et al (2019) Salvage radical prostatectomy for recurrent prostate cancer: morbidity and functional outcomes from a large multicenter series of open versus robotic approaches. J Urol 202:725–731
Onol FF, Bhat S, Moschovas M, Rogers T, Ganapathi H, Roof S et al (2020) Comparison of outcomes of salvage robot-assisted laparoscopic prostatectomy for post-primary radiation vs focal therapy. BJU Int 125:103–111
Thompson JE, Sridhar AN, Tan WS, Freeman A, Haider A, Allen C et al (2019) Pathological findings and magnetic resonance imaging concordance at salvage radical prostatectomy for local recurrence following partial ablation using high intensity focused ultrasound. J Urol 201:1134–1143
Lawrentschuk N, Finelli A, Van Der Kwast TH, Ryan P, Bolton DM, Fleshner NE et al (2011) Salvage radical prostatectomy following primary high intensity focused ultrasound for treatment of prostate cancer. J Urol 185:862–868
Tay KJ, Amin MB, Ghai S, Jimenez RE, Kench JG, Klotz L et al (2019) Surveillance after prostate focal therapy. World J Urol 37:397–407
Huber PM, Afzal N, Arya M, Boxler S, Dudderidge T, Emberton M et al (2020) Prostate specific antigen criteria to diagnose failure of cancer control following focal therapy of nonmetastatic prostate cancer using high intensity focused ultrasound. J Urol 203:734–742
Ahmed HU, El-Shater Bosaily A, Brown LC, Gabe R, Kaplan R, Parmar MK et al (2017) Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet 389:815–822
Hötker AM, Meier A, Mazaheri Y, Zheng J, Capanu M, Chaim J et al (2019) Temporal changes in MRI appearance of the prostate after focal ablation HHS Public Access. Abdom Radiol (NY) 44:272–278
Soria F, Marra G, Allasia M, Gontero P (2018) Retreatment after focal therapy for failure: a bridge too far? Curr Opin Urol 28:544–549
Kinsella N, Stattin P, Cahill D, Brown C, Bill-Axelson A, Bratt O et al (2018) Factors influencing men’s choice of and adherence to active surveillance for low-risk prostate cancer: a mixed-methods systematic review HHS Public Access. Eur Urol 74:261–280
Lang MF, Tyson MD, Alvarez JAR, Koyama T, Hoffman KE, Resnick MJ et al (2017) The influence of psychosocial constructs on the adherence to active surveillance for localized prostate cancer in a prospective. Population-based Cohort Urol 103:173–178
Dall’Era MA (2015) Patient and disease factors affecting the choice and adherence to active surveillance. Curr Opin Urol 25:272–276
Author information
Authors and Affiliations
Contributions
Protocol/project development: PG and GM; Data collection or management: PG and GM; Data analysis: PG and GM; Manuscript writing: GM and PG; Manuscript editing: all authors; Revision for important intellectual contents: all authors.
Corresponding author
Ethics declarations
Conflict of interest
Authors have no conflicts to declare.
Research involving Human Participants and/or Animals
This paper did not involve human participants.
Informed consent
This paper does not require informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gontero, P., Marra, G., Teber, D. et al. Making a case “against” focal therapy for intermediate-risk prostate cancer. World J Urol 39, 719–728 (2021). https://doi.org/10.1007/s00345-020-03303-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-020-03303-y