Abstract
Objective
To evaluate predictive factors of urinary incontinence (UI) after holmium laser enucleation of the prostate (HoLEP).
Methods
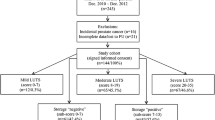
Patients (n = 2346) were included in a retrospective multicentric study from April 2012 to November 2017. Patients’ characteristics (age, BMI, percentage with diabetes), preoperative data (IPSS score, whole gland volume, urinary drainage), operative data (enucleation time, enucleation efficiency, tissue enucleated weight, total delivered energy) and postoperative data were recorded. Absence of UI was defined as no pads at 3 and 6 months. Surgeon experience was stratified in three categories: beginners (< 21 cases), intermediate (21–40 cases) and experienced (> 40 cases). Multivariate logistic regression analysis was performed.
Results
UI was observed in 14.5% of patients (340/2346) at 3 months (95%CI 13–16%) and in 4.2% (98/2346) at 6 months (95%CI 3–5%). On multivariate analysis at 3 months, increasing age (OR per SD = 1.3 [1.14–1.48]), elevated BMI (OR per SD = 1.23 [1.09–1.38]), preoperative urinary drainage (OR = 0.62 [0.45–0.85]), increasing enucleated tissue weight (OR per SD = 1.29 [1.16–1.45]) and experienced surgeon with at least 40 cases (OR = 0.56 [0.42–0.75]) were significantly associated with UI. At 6 months, increasing age (OR per SD = 1.25 [1.01–1.53]), elevated BMI (OR per SD = 1.25 [1.03–1.5]), increasing whole gland volume (OR per one SD log = 1.24 [1.01–1.53]) and diabetes disorder (OR = 1.7 [1.03–2.78]) were significantly associated with UI.
Conclusion
UI after HoLEP was observed in 14.5% of patients at 3 months and 4.2% at 6 months, with stress UI in half of the cases. Surgeon experience with at least 40 cases was the main predictive factor of 3 months UI after HoLEP and diabetes disorder of persistent UI at 6 months.
Similar content being viewed by others
Abbreviations
- BPH:
-
Benign prostatic hyperplasia
- BPO:
-
Benign prostatic obstruction
- CI:
-
Confidence interval
- EEP:
-
Endoscopic enucleation of the prostate
- HoLEP:
-
Holmium laser enucleation of prostate
- IPSS:
-
International Prostate Symptom Score
- MUI:
-
Mixed urinary incontinence
- OR:
-
Odds ratio
- PSA:
-
Prostate-specific antigen
- SD:
-
Standard deviation
- SUI:
-
Stress urinary incontinence
- TURP:
-
Transurethral resection of the prostate
- UUI:
-
Urge urinary incontinence
- UI:
-
Urinary incontinence
References
Gratzke C, Bachmann A, Descazeaud A, Drake MJ, Madersbacher S, Mamoulakis C et al (2015) EAU guidelines on the assessment of non-neurogenic male lower urinary tract symptoms including benign prostatic obstruction. Eur Urol 67(6):1099–1109
Cornu J-N, Ahyai S, Bachmann A, de la Rosette J, Gilling P, Gratzke C et al (2015) A systematic review and meta-analysis of functional outcomes and complications following transurethral procedures for lower urinary tract symptoms resulting from benign prostatic obstruction: an update. Eur Urol 67(6):1066–1096
Robert G, Cornu J-N, Fourmarier M, Saussine C, Descazeaud A, Azzouzi A-R et al (2016) Multicentre prospective evaluation of the learning curve of holmium laser enucleation of the prostate (HoLEP). BJU Int 117(3):495–499
Montorsi F, Naspro R, Salonia A, Suardi N, Briganti A, Zanoni M et al (2004) Holmium laser enucleation versus transurethral resection of the prostate: results from a 2-center, prospective randomized trial in patients with obstructive benign prostatic hyperplasia. J Urol 172(5):1926–1929
Fujisaki A, Goto A, Endo F, Muraishi O, Hattori K, Yasumura S (2016) Practical index of urinary incontinence following holmium laser enucleation of the prostate: a case-series study of the 24-hour pad test immediately after catheter removal. Urol Int 97(3):310–319
Elmansy HM, Kotb A, Elhilali MM (2011) Is there a way to predict stress urinary incontinence after holmium laser enucleation of the prostate? J Urol 186(5):1977–1981
Nam JK, Kim HW, Lee DH, Han J-Y, Lee JZ, Park S-W (2015) Risk factors for transient urinary incontinence after holmium laser enucleation of the prostate. World J Mens Health 33(2):88
Shigemura K, Tanaka K, Yamamichi F, Chiba K, Fujisawa M (2006) Comparison of predictive factors for postoperative incontinence of holmium laser enucleation of the prostate by the surgeons’ experience during learning curve. Int Neurourol J 20(1):59–68
Shigemura K, Yamamichi F, Kitagawa K, Yamashita M, Oka Y, Tanaka H et al (2017) Does surgeon experience affect operative time, adverse events and continence outcomes in holmium laser enucleation of the prostate? A review of more than 1,000 cases. J Urol 198(3):663–670
Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmsten U et al (2002) The standardisation of terminology of lower urinary tract function: report from the standardisation sub-committee of the International Continence Society. Neurourol Urodyn 21(2):167–178
Rubin TH, D.B. (1990) Multiple imputation for nonresponse in surveys. Stat Pap 31(1):180–180
Lerner LB, Tyson MD, Mendoza PJ (2010) Stress incontinence during the learning curve of holmium laser enucleation of the prostate. J Endourol 24(10):1655–1658
Members of the Florey Adelaide Male Ageing Study, Martin SA, Haren MT, Marshall VR, Lange K, Wittert GA (2011) Prevalence and factors associated with uncomplicated storage and voiding lower urinary tract symptoms in community-dwelling Australian men. World J Urol 29(2):179–184
Yalcin S, Gazel E, Somani BK, Yilmaz S, Tunc L (2019) Prostate shape significantly affects the HoLEP procedure time and energy usage: a retrospective pilot study. Minim Invasive Ther Allied Technol 28(4):220–226
Naspro R, Suardi N, Salonia A, Scattoni V, Guazzoni G, Colombo R et al (2006) Holmium laser enucleation of the prostate versus open prostatectomy for prostates > 70g: 24-month follow-up. Eur Urol 50(3):563–568
Minagawa S, Okada S, Sakamoto H, Toyofuku K, Morikawa H (2015) En-Bloc technique with anteroposterior dissection holmium laser enucleation of the prostate allows a short operative time and acceptable outcomes. Urology 86(3):628–633
Walz J, Epstein JI, Ganzer R, Graefen M, Guazzoni G, Kaouk J et al (2016) A critical analysis of the current knowledge of surgical anatomy of the prostate related to optimisation of cancer control and preservation of continence and erection in candidates for radical prostatectomy: an update. Eur Urol 70(2):301–311
Endo F, Shiga Y, Minagawa S, Iwabuchi T, Fujisaki A, Yashi M et al (2010) Anteroposterior dissection HoLEP: a modification to prevent transient stress urinary incontinence. Urology 76(6):1451–1455
Saitta G, Becerra JEA, del Álamo JF, González LL, Elbers JR, Suardi N et al (2019) ‘En Bloc’ HoLEP with early apical release in men with benign prostatic hyperplasia. World J Urol 37(11):2451–2458
Jeong J, Lee HS, Cho WJ, Jung W, You HW, Kim TH et al (2015) Effect of detrusor overactivity on functional outcomes after holmium laser enucleation of the prostate in patients with benign prostatic obstruction. Urology 86(1):133–138
Placer J, Gelabert-Mas A, Vallmanya F, Manresa JM, Menéndez V, Cortadellas R et al (2009) Holmium laser enucleation of prostate: outcome and complications of self-taught learning curve. Urology 73(5):1042–1048
Chang PL, Tsai LH, Huang ST, Wang TM, Hsieh ML, Tsui KH (1998) The early effect of pelvic floor muscle exercise after transurethral prostatectomy. J Urol 160(2):402–405
Author information
Authors and Affiliations
Contributions
VH: project development and manuscript writing; JO, ML: manuscript writing; MB: data collection; AP: data analysis; MM, PET, HB, RM and TM: data collection or management; AV, GR and JR: project development and manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
V. Houssin, J. Olivier, M. Brenier, A. Pierache, M. Laniado, M. Mouton, T. Marquette, A.Villers declare that they have no conflict of interest. PE. Theveniaud, H. Baumert, R. Mallet, G. Robert, J. Rizk: HOLEP proctor for EDAP/TMS.
Informed consent
All participants have given informed consent before inclusion in the present study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Houssin, V., Olivier, J., Brenier, M. et al. Predictive factors of urinary incontinence after holmium laser enucleation of the prostate: a multicentric evaluation. World J Urol 39, 143–148 (2021). https://doi.org/10.1007/s00345-020-03169-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-020-03169-0