Abstract
Introduction
Holmium:yttrium–aluminium–garnet (Ho:YAG) is currently the gold standard for lithotripsy for the treatment of all known urinary stone types. Stone composition and volume are major determinants of the lithotripsy. This in vitro study evaluated the required energy to ablate 1 mm3 of various stone types with different laser settings using Ho:YAG.
Methods
272 µm core-diameter laser fibers (Boston Scientific©) were connected to a 30 Watt MH1 Ho:YAG generator (Rocamed®). An experimental setup consisting of immerged human stones of calcium oxalate monohydrate (COM), uric acid (UA) or cystine (Cys) was used with a single pulse lasing emission (0.6/0.8/1 J), in contact mode. Stones were dried out before three-dimensional scanning to measure ablation volume per pulse (AVP) and required energy to treat 1 mm3 (RE).
Results
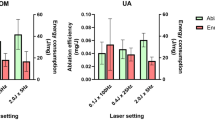
All settings considered, ablation volumes per pulse (AVP) for COM were significantly lower than those for UA and Cys (p = 0.002 and p = 0.03, respectively), whereas AVP for Cys was significantly lower than those for UA (p = 0.03). The mean REs at 0.6 J pulse energy (PE) for COM, Cys and UA were 34, 8.5 and 3.2 J, respectively The mean REs at 1 J PE for COM, Cys and UA were 14.7, 6.4 and 2 J, respectively. At 0.6 J PE, RE for COM was more than tenfold and fivefold higher than those for UA and Cys, respectively.
Conclusion
This in vitro study shows for the first time a volumetric evaluation of Ho:YAG efficiency by the ablation volume per pulse on human stone samples, according to various pulse energies. The REs for COM, UA and Cys should be considered in clinical practice.




Similar content being viewed by others
References
Gupta PK (2007) Is the holmium:YAG laser the best intracorporeal lithotripter for the ureter? A 3-year retrospective study. J Endourol 21(3):305–309
Kronenberg P, Somani B (2018) Advances in lasers for the treatment of stones—a systematic review. Curr Urol Rep. 19(6):45
Kadihasanoglu M, Yucetas U, Culha MG, Erkan E, Toktas MG (2017) Effect of stone composition on the outcomes of semi-rigid ureteroscopy using holmium: yttrium–aluminum–garnet laser or pneumatic lithotripsy. J Coll Physicians Surg-Pak JCPSP 27(4):227–231
Türk C, Petřík A, Sarica K, Seitz C, Skolarikos A, Straub M et al (2016) EAU guidelines on interventional treatment for urolithiasis. Eur Urol 69(3):475–482
EAU guidelines on interventional treatment for urolithiasis.—PubMed—NCBI [Internet]. [cité 26 juin 2019]. Disponible sur: https://www.ncbi.nlm.nih.gov/pubmed/26344917
Pradère B, Doizi S, Proietti S, Brachlow J, Traxer O (2018) Evaluation of guidelines for surgical management of urolithiasis. J Urol 199(5):1267–1271
Assimos D, Krambeck A, Miller NL, Monga M, Murad MH, Nelson CP et al (2016) Surgical management of stones: American Urological Association/Endourological Society guideline. Part I. J Urol. 196(4):1153–1160
Assimos D, Krambeck A, Miller NL, Monga M, Murad MH, Nelson CP et al (2016) Surgical Management of stones: American Urological Association/Endourological Society guideline, part II. J Urol. 196(4):1161–1169
Wilhelm K, Miernik A, Hein S, Schlager D, Adams F, Benndorf M et al (2018) Validating automated kidney stone volumetry in CT and mathematical correlation with estimated stone volume based on diameter. J Endourol 32(7):659–664
Daudon M (2004) Analysis and classification of calculi: contribution to the etiology of calculous disease. Rev Med Suisse Romande 124(8):445–453
D Slicer [Internet]. https://www.slicer.org/. Cited 10 May 2019
De Coninck V, Traxer O (2018) The time has come to report stone burden in terms of volume instead of largest diameter. J Endourol. 32(3):265–266
Merigot de Treigny O, Bou Nasr E, Almont T, Tack I, Rischmann P, Soulié M et al (2015) The cumulated stone diameter: a limited tool for stone burden estimation. Urology. 86(3):477–481
Patel SR, Nakada SY (2011) Quantification of preoperative stone burden for ureteroscopy and shock wave lithotripsy: current state and future recommendations. Urology 78(2):282–285
Lidén M, Andersson T, Broxvall M, Thunberg P, Geijer H (2012) Urinary stone size estimation: a new segmentation algorithm-based CT method. Eur Radiol 22(4):731–737
Sridhar S, Kumaravel N (2001) Automatic segmentation of medical images for renal calculi and analysis. Biomed Sci Instrum. 37:405–409
Marsousi M, Plataniotis KN, Stergiopoulos S (2014) Shape-based kidney detection and segmentation in three-dimensional abdominal ultrasound images. Conf Proc Annu Int Conf IEEE Eng Med Biol Soc IEEE Eng Med Biol Soc Annu Conf. 2014:2890–2894
Hassani H, Raynal G, Spie R, Daudon M, Vallée J-N (2012) Imaging-based assessment of the mineral composition of urinary stones: an in vitro study of the combination of Hounsfield unit measurement in noncontrast helical computerized tomography and the twinkling artifact in color Doppler ultrasound. Ultrasound Med Biol 38(5):803–810
Peyronnet B, Robert G, Comat V, Rouprêt M, Gomez-Sancha F, Cornu J-N et al (2017) Learning curves and perioperative outcomes after endoscopic enucleation of the prostate: a comparison between GreenLight 532-nm and holmium lasers. World J Urol 35(6):973–983
Panthier F, Pasquier J, Bruel S, Azancot V, De La Taille A, Gasman D (2019) En bloc greenlight laser enucleation of prostate (GreenLEP): about the first hundred cases. World J Urol. https://doi.org/10.1007/s00345-019-02941-1
Mekayten M, Lorber A, Katafigiotis I, Sfoungaristos S, Leotsakos I, Heifetz EM et al (2019) Will stone density stop being a key factor in endourology? The impact of stone density on laser time using Lumenis Laser p120w and standard 20 W laser: a comparative study. J Endourol 33(7):585–589
Esch E, Simmons WN, Sankin G, Cocks HF, Preminger GM, Zhong P (2010) A simple method for fabricating artificial kidney stones of different physical properties. Urol Res 38(4):315–319
Molina WR, Marchini GS, Pompeo A, Sehrt D, Kim FJ, Monga M (2014) Determinants of holmium:yttrium–aluminum–garnet laser time and energy during ureteroscopic laser lithotripsy. Urology 83(4):738–744
Teichman JM, Vassar GJ, Bishoff JT, Bellman GC (1998) Holmium:YAG lithotripsy yields smaller fragments than lithoclast, pulsed dye laser or electrohydraulic lithotripsy. J Urol 159(1):17–23
Kronenberg P, Traxer O (2015) Update on lasers in urology 2014: current assessment on holmium:yttrium–aluminum–garnet (Ho:YAG) laser lithotripter settings and laser fibers. World J Urol 33(4):463–469
Doizi S, Keller EX, De Coninck V, Traxer O (2018) Dusting technique for lithotripsy: what does it mean? Nat Rev Urol. 15(11):653–654
Talso M, Emiliani E, Haddad M, Berthe L, Baghdadi M, Montanari E et al (2016) Laser fiber and flexible ureterorenoscopy: the safety distance concept. J Endourol. 30(12):1269–1274
Peplinski B, Faaborg D, Miao E, Alsyouf M, Myklak K, Kelln W et al (2016) The effect of laser fiber cleave technique and lithotripsy time on power output. J Endourol. 30(6):678–684
Haddad M, Emiliani E, Rouchausse Y, Coste F, Berthe L, Doizi S et al (2017) Impact of laser fiber tip cleavage on power output for ureteroscopy and stone treatment. World J Urol. 35(11):1765–1770
Ventimiglia E, Traxer O (2019) Is very high power/frequency really necessary during laser lithotripsy? RE: understanding the popcorn effect during holmium laser lithotripsy for dusting (Aldoukhi et al, Urology. 2018 Dec;122:52–57). Urology 127:135. https://doi.org/10.1016/j.urology.2019.01.032
Aldoukhi AH, Roberts WW, Hall TL, Teichman JMH, Ghani KR (2018) Understanding the popcorn effect during holmium laser lithotripsy for dusting. Urology Déc 122:52–57
Aldoukhi AH, Ghani KR (2019) Reply to: letter-to-the-editor: understanding the popcorn effect during holmium laser lithotripsy for dusting. Urology. 127:135–136
Ventimiglia E, Traxer O (2019) What Is Moses effect: a historical perspective. J Endourol. mai 33(5):353–357
Keller EX, de Coninck V, Audouin M, Doizi S, Bazin D, Daudon M et al (2019) Fragments and dust after holmium laser lithotripsy with or without « Moses technology »: How are they different? J Biophotonics 12(4):e201800227
Winship B, Wollin D, Carlos E, Li J, Peters C, Simmons WN et al (2018) Dusting efficiency of the Moses holmium laser: an automated in vitro assessment. J Endourol 32(12):1131–1135
Aldoukhi AH, Roberts WW, Hall TL, Ghani KR (2019) Watch your distance: the role of laser fiber working distance on fragmentation when altering pulse width or modulation. J Endourol 33(2):120–126
Sroka R, Pongratz T, Scheib G, Khoder W, Stief CG, Herrmann T et al (2015) Impact of pulse duration on Ho:YAG laser lithotripsy: treatment aspects on the single-pulse level. World J Urol 33(4):479–485
Emiliani E, Talso M, Cho S-Y, Baghdadi M, Mahmoud S, Pinheiro H et al (2017) Optimal Settings for the Noncontact Holmium:YAG Stone Fragmentation Popcorn Technique. J Urol. 198(3):702–706
Wollin DA, Ackerman A, Yang C, Chen T, Simmons WN, Preminger GM et al (2017) Variable pulse duration from a new holmium:YAG laser: the effect on stone comminution, fiber tip degradation, and retropulsion in a dusting model. Urology 103:47–51
Acknowledgements
In vivo imaging was performed at Life Imaging Facility of Paris Descartes University (Plateforme Imageries du Vivant), supported by France Life Imaging (grant ANR-11-INBS-0006) and Infrastructures Biologies-Santé.
Funding
Frédéric Panthier received a French Association of Urology Research Grant (2018).
Author information
Authors and Affiliations
Contributions
FP and EV: equal contribution: protocol development, data collection and management, data analysis, manuscript writing and editing. LB: protocol development, data collection and management, manuscript editing. CC: protocol development, data collection. MD: protocol development, data collection. SD: protocol development, manuscript writing and editing. OT: protocol development, data analysis, manuscript writing and editing.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest. However, Olivier Traxer has declared as being a consultant for Boston Scientific Corporation, Coloplast, Wolf, B-Braun, IPG photonics, Lumenis, Olympus and Rocamed. Steeve Doizi has declared as being a consultant for Boston Scientific Corporation and Coloplast.
Research involving human participants or animals
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
This article does not contain any studies with human participants or animals performed by any of the authors. Human stone samples were used in this study, with the informed consent of each patient.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Panthier, F., Ventimiglia, E., Berthe, L. et al. How much energy do we need to ablate 1 mm3 of stone during Ho:YAG laser lithotripsy? An in vitro study. World J Urol 38, 2945–2953 (2020). https://doi.org/10.1007/s00345-020-03091-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-020-03091-5