Abstract
Purpose
This study would like to develop a novel model similar to human prostate in terms of its texture profile, sensation upon resection, and anatomical hallmarks for resident transurethral resection of the prostate (TUR-P) training.
Methods
Ten phantom designs were proposed, using broadly available ingredients and a homemade protocol. Three steps of evaluation and development were done: objective measurement measuring texture profile (e.g. hardness, elasticity, cohesiveness/consistency, and adhesiveness/stickiness) using TA-XT2i Texture Analyzer (Llyod Instruments, Ametek Inc) to compare the designs with human prostate, finding the most similar design to prostate; expert consensus by a panel of urologist/senior residents comparing the simulation of TUR-P on the selected design with pre-existing control phantom; and anatomical design development using 3D printing for molding.
Results
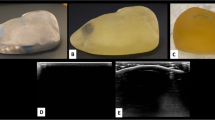
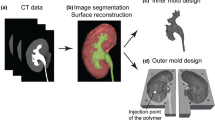
Texture profile analysis for mean hardness, elasticity, cohesiveness/consistency, and adhesiveness/stickiness of human prostate was 3753.4 ± 673.4, 85 ± 1.9, 0.7 ± 0.03, and 0, respectively, and design IX was the most similar to human prostate (3660.7 ± 465.6, 87.0 ± 2.5, 0.6 ± 0.05, 0). Furthermore, expert consensus showed superiority of design IX compared with pre-existing control phantom (16.95 ± 1.36 vs 8.86 ± 3.10; P < 0.001). Most of the respondents agreed that the texture, consistency, and phantom ability to mimic human prostate upon resection were similar with human prostate, though hallmarks of the prostate e.g. veromontanum, and lobes were lacking. We used these feedbacks to develop a mold, designed to produce these important anatomical hallmarks.
Conclusion
This study developed a cost-effective prostate model from a food-based design that is similar to human prostate in terms of its texture and sensation upon TUR-P resection provided with important anatomical hallmarks.





Similar content being viewed by others
References
Tjahdojati, Soebadi DM, Umbas R, Purnomo BB, Widjanarko S, Mochtar CA et al (2017) Panduan penatalaksanaan klinis: pembesaran prostat jinak (benign prostatic hyperplasia/BPH). Ikatan Ahli Urologi Indonesia
Brewin J, Ahmed K, Khan MS, Jaye P, Dasgupta P (2014) Face, content, and construct validation of the Bristol TURP trainer. J Surg Educ 71(4):500–505
Kapadia MR, Da-Rosa DA, Mac-Rae HM, Dunnington GL (2007) Current assessment and future directions of surgical skills laboratories. J Surg Educ 64(5):260–265
Matsumoto ED, Hamstra SJ, Radomski SB, Cusimano MD (2001) A novel approach to endourological training: training at the surgical skills center. J Urol 166:1261–1266
Niessen WJ, Viergever MA (2001) Medical image computing and computer-assisted intervention—MICCAI 2001. In: The forth international conference Proceedings. Springer, Utrecht, pp 360–367
Burdea G, Patounakis G, Popescu V, Weiss RE (1999) Virtual reality-based training for the diagnosis of prostate cancer. IEEE Trans Biomed Eng 46(10):1253–1260
Tjiam IM, Berkers CH, Schout BM, Brinkman WM, Witjes JA, Scherpbier AJ et al (2014) Evaluation of the educational value of a virtual reality TURP simulator according to a curriculum-based approach. Simul Healthc 9(5):288–294
Källström R, Hjertberg H, Kjölhede H, Svanvik J (2005) Use of a virtual reality, real-time, simulation model for the training of urologists in transurethral resection of the prostate. Scand J Urol Nephrol 39(4):313–320
Bach T, Geavlete B, Herrmann TRW, Gross AJ (2009) Homemade” TUR-simulator for less than $40 U.S.? The “TupperTM” experience. J Endourol 23(3):509–513
Khan R, Aydin A, Khan MS, Dasgupta P, Ahmed K (2015) Simulation-based training for prostate surgery. BJU Int 116(4):665–674
Ahmad S, Byrne D, Ghulam N (2013) Training model for transurethral resection of prostate using human cadavers embalmed by Thiel's method. Videourology. https://doi.org/10.1089/vid.2013.0026
Hou S, Ross G, Tait I, Halliday P, Tang B (2017) Development and validation of a novel and cost-effective animal tissue model for training transurethral resection of the prostate. J Surg Educ 74(5):898–905
Sweet R, Porter J, Oppenheimer P et al (2002) Simulation of bleeding in endoscopic procedures using virtual reality. J Endourol 16:451–455
Ben-Zvi T, Hueber PA, Valdivieso R, Azzizi M, Tholomier C, Bienz M et al (2015) Urological resident exposure to transurethral surgical options for BPH management in 2012–2013: a pan-Canadian survey. Can Urol Assoc J 9(3–4):E236
Funding
There is no external funding done for this study. All expenses were covered by the institution and authors.
Author information
Authors and Affiliations
Contributions
NR: project design, project development, data collection, and manuscript writing. HWKP: data collection and manuscript writing. PB: manuscript writing and supervision. IW: data collection and supervision. CAM: data analysis and supervision. ARAHH: project design, supervision, and manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Statement of human rights
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (The Ethics Committee of the Faculty of Medicine, University of Indonesia; Ethical Approval number 0224/UN2.F1/ETIK/2018) and with the 1964 Helsinski declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rasyid, N., Putra, H.W.K., Birowo, P. et al. TUR-P phantom for resident surgical training: food-based design as a human mimicking model of the prostate. World J Urol 38, 2907–2914 (2020). https://doi.org/10.1007/s00345-020-03085-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-020-03085-3