Abstract
Purpose
To perform a systematic review and meta-analysis of the literature inherent robotic nephroureterectomy (RNU) and to compare its outcomes with those of other nephroureterectomy (NU) techniques.
Methods
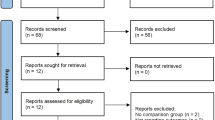
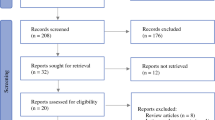
A systematic literature search was performed up to April 2019 using PubMed, Embase®, and Web of Science. The Preferred Reporting Items for Systematic Review and Meta-analysis Statement was followed for study selection. The following data were extracted for each study: baseline features, surgical outcomes, oncological outcomes, and survival outcomes. Stata® 15.0 was used for statistical analysis.
Results
Literature search identified 80 studies eligible for the meta-analysis and overall 87,291 patients were included in the analysis: open NU (ONU; n = 45,601), hand-assisted laparoscopic NU (HALNU; n = 442), laparoscopic NU (LNU n = 31,093), and RNU (n = 10,155). RNU was more likely to be performed in those patients with multifocal tumor location (proportion: 0.19; 95% CI 0.14, 0.24) and high-grade disease (proportion: 0.70; 95% CI 0.53, 0.68). The lowest EBL was recorded in the RNU group (weighted mean (WM) 163.31 mL; 95% CI 88.94, 237.68), whereas the highest was in the ONU group (414.99 mL; 95% CI 378.52, 451.46). Operative time was shorter for ONU (224.98 mL; 95% CI 212.26, 237.69). RNU had lower rate of intraoperative complications (0.02; 95% CI 0.01, 0.05). ONU showed higher odds of transfusions (0.20; 95% CI 0.15, 0.25). LOS was statistically significantly shorter for the RNU group (5.35 days; 95% CI 4.97, 5.82). HALNU seemed to present lower risk of PSM (0.02; 95% CI − 0.01, 0.05), and lower risk of recurrence (0.22; 95% CI 0.15, 0.30), metastasis (0.07; 95% CI 0.05, 0.10), and cancer-related death (0.03; 95% CI 0.01, 0.06). ONU showed the lowest 5 years cancer specific survival (proportion: 0.77; 95% CI 0.74, 0.80). No correlation was found between the surgical technique and recurrence-free and cancer-specific survival.
Conclusions
Evidence regarding RNU for the treatment of UTUC is increasing but it remains quite sparse and of low quality. Despite this, RNU seems to be safe, and to offer the advantages of a minimally invasive approach without impairing the oncological outcomes. Nevertheless, ONU, HALNU, and LNU still represent a valid, and commonly used surgical treatment option. As RNU becomes more popular, and concerns related to its use remain, the best surgical technique for NU remains to be determined.



Similar content being viewed by others
References
Rouprêt M, Babjuk M, Compérat E, Zigeuner R, Sylvester RJ, Burger M, Cowan NC, Böhle A, Van Rhijn BW, Kaasinen E, Palou J, Shariat SF (2015) European Association of Urology Guidelines on upper urinary tract urothelial cell carcinoma: 2015 update. Eur Urol 68:868–879
Mullen E, Ahmed K, Challacombe B (2017) Systematic review of open versus laparoscopic versus robot-assisted nephroureterectomy. Rev Urol 19:32–43
Gakis G, Schubert T, Alemozaffar M, Bellmunt J, Bochner BH, Boorjian SA, Daneshmand S, Huang WC, Kondo T, Konety BR, Laguna MP, Matin SF, Siefker-Radtke AO, Shariat SF, Stenzl A (2017) Update of the ICUD-SIU consultation on upper tract urothelial carcinoma 2016: treatment of localized high-risk disease. World J Urol 35:327–335
Lee SM, McKay A, Grimes N, Umez-Eronini N, Aboumarzouk OM (2019) Distal ureter management during nephroureterectomy: evidence from a systematic review and cumulative analysis. J Endourol 33:263–273. https://doi.org/10.1089/end.2018.0819
Hemal A, Stansel I, Babber P, Patel M (2011) Robotic-assisted nephroureterectomy and bladder cuff excision without intraoperative repositioning. Urology 78:357–364
Autorino R, Zargar H, Kaouk JH (2014) Robotic-assisted laparoscopic surgery: recent advances in urology. Fertil Steril 102:939–949
Rodriguez JF, Packiam VT, Boysen WR, Johnson SC, Smith ZL, Smith ND, Shalhav AL, Steinberg GD (2017) Utilization and outcomes of nephroureterectomy for upper tract urothelial carcinoma by surgical approach. J Endourol 31:661–665
Moher D, Liberati A, Tetzlaff J, Altman DG; PRISMA Group (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8:336–341
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA, PRISMA-P Group (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev 4:1. https://doi.org/10.1186/2046-4053-4-1
Howick J, Chalmers I, Glasziou P, Heneghan C, Liberati A, Moschetti I, Phillips B, Thornton H (2011) Explanation of the 2011 Oxford Centre for Evidence-Based Medicine (OCEBM) Levels of Evidence (background document). Oxford Centre for Evidence- Based Medicine. https://www.cebm.net/index.aspx?o=5653.
Wells GA, Shea B, O’Connell D, Robertson J, Peterson J, Welch V, Losos M, Tugwell P (2013) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomized studies in meta-analyses. Ottawa Hospital Research Institute. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 6 June 2019
Jadad AR, Moore RA, Carroll D et al (1996) Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials 17:1–12
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13. https://doi.org/10.1186/1471-2288-5-13
Ades AE, Lu G, Higgins JP (2005) The interpretation of random-effects meta-analysis in decision models. Med Decis Making 25:646–654
Soria F, Shariat SF, Lerner SP, Fritsche HM, Rink M, Kassouf W, Spiess PE, Lotan Y, Ye D, Fernández MI, Kikuchi E, Chade DC, Babjuk M, Grollman AP, Thalmann GN (2017) Epidemiology, diagnosis, preoperative evaluation and prognostic assessment of upper-tract urothelial carcinoma (UTUC). World J Urol 35:379–387
Lee H, Kim HJ, Lee SE, Hong SK, Byun SS (2019) Comparison of oncological and perioperative outcomes of open, laparoscopic, and robotic nephroureterectomy approaches in patients with non-metastatic upper-tract urothelial carcinoma. PLoS ONE 14:e0210401. https://doi.org/10.1371/journal.pone.0210401
Lim SK, Shin TY, Kim KH, Han WK, Chung BH, Hong SJ, Choi YD, Rha KH (2014) Laparoendoscopic single-site (LESS) robot-assisted nephroureterectomy: comparison with conventional multiport technique in the management of upper urinary tract urothelial carcinoma. BJU Int 114:90–97
Melquist JJ, Redrow G, Delacroix S, Park A, Faria EE, Karam JA, Matin SF (2016) Comparison of single-docking robotic-assisted and traditional laparoscopy for retroperitoneal lymph node dissection during nephroureterectomy with bladder cuff excision for upper-tract urothelial carcinoma. Urology 87:216–223
Patel MN, Hemal AK (2018) Does advancing technology improve outcomes? comparison of the Da Vinci Standard/S/Si to the Xi robotic platforms during robotic nephroureterectomy. J Endourol 32:133–138. https://doi.org/10.1089/end.2017.0477
Argun OB, Mourmouris P, Tufek I, Tuna MB, Keskin S, Obek C, Kural AR (2016) Radical nephroureterectomy without patient or port repositioning using the Da Vinci Xi Robotic System: initial experience. Urology 92:136–139
Tinay I, Gelpi-Hammerschmidt F, Leow JJ, Allard CB, Rodriguez D, Wang Y, Chung BI, Chang SL (2016) Trends in utilisation, perioperative outcomes, and costs of nephroureterectomies in the management of upper tract urothelial carcinoma: a 10-year population-based analysis. BJU Int 117:954–960
Trudeau V, Gandaglia G, Shiffmann J, Popa I, Shariat SF, Montorsi F, Perrotte P, Trinh QD, Karakiewicz PI, Sun M (2014) Robot-assisted versus laparoscopic nephroureterectomy for upper-tract urothelial cancer: A population-based assessment of costs and perioperative outcomes. Can Urol Assoc J 8:E695–701
Nazzani S, Bazinet A, Preisser F, Mazzone E, Tian Z, Mistretta FA, Shariat SF, Saad F, Zorn KC, Montanari E, Briganti A, Carmignani L, Karakiewicz PI (2019) Comparison of perioperative outcomes between open and minimally invasive nephroureterectomy: A population-based analysis. Int J Urol 26:487–492
Zargar H, Krishnan J, Autorino R, Akca O, Brandao LF, Laydner H, Samarasekera D, Ko O, Haber GP, Kaouk JH, Stein RJ (2014) Robotic nephroureterectomy: a simplified approach requiring no patient repositioning or robot redocking. Eur Urol 66:769–777
Moschini M, Foerster B, Abufaraj M, Soria F, Seisen T, Roupret M, Colin P, De la Taille A, Peyronnet B, Bensalah K, Herout R, Wirth MP, Novotny V, Chlosta P, Bandini M, Montorsi F, Simone G, Gallucci M, Romeo G, Matsumoto K, Karakiewicz P, Briganti A, Shariat SF (2017) Trends of lymphadenectomy in upper tract urothelial carcinoma (UTUC) patients treated with radical nephroureterectomy. World J Urol 35:1541–1547
Nouralizadeh A, Tabatabaei S, Basiri A, Simforoosh N, Soleimani M, Javanmard B, Ansari A, Shemshaki H (2018) Comparison of open versus laparoscopic versus hand-assisted laparoscopic nephroureterectomy: a systematic review and meta-analysis. J Laparoendosc Adv Surg Tech A 28:656–681. https://doi.org/10.1089/lap.2017.0662
Ha YS, Chung JW, Choi SH, Lee JN, Kim BS, Kim TH, Yoo ES, Kwon TG, Byun SS, Choi YD, Kang HW, Yun SJ, Kim WJ, Kim HT (2017) Impact of a bladder cuff excision during radical nephroureterectomy on cancer specific survival in patients with upper tract urothelial cancer in Korea a retrospective, multiinstitutional study. Minerva Urol Nefrol 69:466–474
Mistretta FA, Carrion DM, Nazzani S, Vásquez JL, Fiori C, De Cobelli, Porpiglia F, Esperto F (2019) Bladder recurrence of primary upper tract urinary carcinoma following nephroureterectomy, and risk of upper urinary tract recurrence after ureteral stent positioning in patients with primary bladder cancer. Minerva Urol Nefrol 71:191–200. 10.23736/S0393-2249.19.03311-3.
Peyronnet B, Seisen T, Dominguez-Escrig JL, Bruins HM, Yuan CY, Lam T, Maclennan S, Ndow J, Babjuk M, Comperat E, ZigeunerR SRJ, Burger M, Mostafid H, van Rhijn BWG, Gontero P, Palou J, Shariat SF, Roupret M (2019) Oncological outcomes of laparoscopic nephroureterectomy versus open radical nephroureterectomy for upper tract urothelial carcinoma: an European Association of Urology Guidelines systematic review. Eur Urol Focus 5:205–223. https://doi.org/10.1016/j.euf.2017.10.003
Simone G, Papalia R, Guaglianone S, Ferriero M, Leonardo C, Forastiere E, Gallucci M (2009) Laparoscopic versus open nephroureterectomy: perioperative and oncologic outcomes from a randomised prospective study. Eur Urol 56:520–526. https://doi.org/10.1016/j.eururo.2009.06.013
Foerster B, D'Andrea D, Abufaraj M, Broenimann S, Karakiewicz PI, Rouprêt M, Gontero P, Lerner SP, Shariat SF, Soria F (2019) Endocavitary treatment for upper tract urothelial carcinoma: a meta-analysis of the current literature. Urol Oncol. https://doi.org/10.1016/j.urolonc.2019.02.004
Territo A, Foerster B, Shariat SF, Rouprêt M, Gaya JM, Palou J, Breda A (2018) Diagnosis and kidney-sparing treatments for upper tract urothelial carcinoma: state of the art. Minerva Urol Nefrol 70:242–251. https://doi.org/10.23736/S0393-2249.18.03058-8
Acknowledgements
Dr. Alessandro Veccia is an Italian Society of Urology-American Urological Association (SIU-AUA) research fellow. Funding for his fellowship is also provided by the VCU Urology Research Fund.
Funding
None.
Author information
Authors and Affiliations
Contributions
Protocol/project development: AV, RA. Data collection or management: AV, SF. Data analysis: AV, RA. Manuscript writing / editing: AV, RA, AA, and HZ. Other (Supervision): CS, GG, SP, MF, GC, LJH, FP.
Corresponding author
Ethics declarations
Conflict of interest:
The authors declare that they have no conflict of interest.
Research involving Human Participants and/or Animals
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Veccia, A., Antonelli, A., Francavilla, S. et al. Robotic versus other nephroureterectomy techniques: a systematic review and meta-analysis of over 87,000 cases. World J Urol 38, 845–852 (2020). https://doi.org/10.1007/s00345-019-03020-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-019-03020-1