Abstract
Purpose
Penile cancer is a rare but aggressive disease, often requiring a rapid and extensive surgical treatment of the primary tumor and staging or treatment of the inguinal lymph node basins. Current management and guidelines of the disease are mainly based on retrospective data, as there is a lack of controlled trials or large series. The purpose of this work is to review contemporary data on the impact of centralization and formation of rare disease networks on penile cancer care and outcomes.
Methods
This narrative, non-systematic review is based on publications retrieved by a PubMed and EMBASE search and on the current guidelines of the European Association of Urology, the National Institute for Health and Care Excellence, and the National Comprehensive Cancer network.
Results
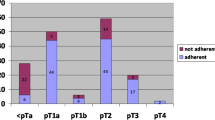
The low case load, particularly in non-specialized centres, combined with limited evidence regularly results in a disparity between the treatment strategy and the guidelines. The suboptimal guideline adherence is specifically the case for organ-sparing surgery and surgical staging of the groin areas in selected cases. Treatment of the disease in high-volume referral centres has been shown to improve the use of organ-sparing surgery, the utilization of invasive lymph node staging in high-risk patients, and finally has resulted in increased survival rates.
Conclusions
The management of penile cancer in disease networks and in countries where centralized healthcare is offered positively influences functional and oncological outcomes. We propose that governments and health care providers should be encouraged to centralize healthcare for rare tumors such as penile cancer.
Similar content being viewed by others
References
Hakenberg OW, Compérat EM, Minhas S, Necchi A, Protzel C, Watkin N (2015) EAU guidelines on penile cancer: 2014 update. Eur Urol 67(1):142–150
Douglawi A, Masterson TA (2017) Updates on the epidemiology and risk factors for penile cancer. Transl Androl Urol 6(5):785–790
Cindolo L, Bada M, Varga J, Nyirady P, Battaglia M, Boccasile S et al (2017) The adherence to the eau guidelines on penile cancer treatment could influence the survival: multicenter, retrospective, European study. J Urol 197(4):976
https://kankerregister.org/. Accessed 1 Mar 2019
Sri D, Sujenthiran A, Lam W, Minter J, Tinwell BE, Corbishley CM et al (2018) A study into the association between local recurrence rates and surgical resection margins in organ-sparing surgery for penile squamous cell cancer. BJU Int 122(4):576–582
Leijte JAP, Kirrander P, Antonini N, Windahl T, Horenblas S (2008) Recurrence patterns of squamous cell carcinoma of the penis: recommendations for follow-up based on a two-centre analysis of 700 patients. Eur Urol 54(1):161–169
Philippou P, Shabbir M, Malone P, Nigam R, Muneer A, Ralph DJ et al (2012) Conservative surgery for squamous cell carcinoma of the penis: resection margins and long-term oncological control. J Urol 188(3):803–808
Albersen M, Parnham A, Joniau S, Sahdev V, Christodoulidou M, Castiglione F et al (2018) Predictive factors for local recurrence after glansectomy and neoglans reconstruction for penile squamous cell carcinoma. Urol Oncol 36(4):141–146
Djajadiningrat RS, van Werkhoven E, Meinhardt W, van Rhijn BWG, Bex A, van der Poel HG et al (2014) Penile sparing surgery for penile cancer—does it affect survival? J Urol 192(1):120–126
Sosnowski R, Kuligowski M, Kuczkiewicz O, Moskal K, Wolski JK, Bjurlin MA et al (2016) Primary penile cancer organ sparing treatment. Cent Eur J Urol 69(4):377–383
Bayles AC, Sethia KK (2010) The impact of Improving Outcomes Guidance on the management and outcomes of patients with carcinoma of the penis. Ann R Coll Surg Engl 92(1):44–45
Raskin Y, Vanthoor J, Milenkovic U, Muneer A, Albersen M (2019) Organ-sparing surgical and nonsurgical modalities in primary penile cancer treatment. Curr Opin Urol 29(2):156–164
Baumgarten A, Chipollini J, Yan S, Ottenhof SR, Tang DH, Draeger D et al (2018) Penile sparing surgery for penile cancer: a multicenter international retrospective cohort. J Urol 199(5):1233–1237
Hughes BE, Leijte JAP, Kroon BK, Shabbir MA, Swallow TW, Heenan SD et al (2010) Lymph node metastasis in intermediate-risk penile squamous cell cancer: a two-centre experience. Eur Urol 57(4):688–692
Kirrander P, Andrén O, Windahl T (2013) Dynamic sentinel node biopsy in penile cancer: initial experiences at a Swedish referral centre. BJU Int 111(3b):E48–E53
Graafland NM, Lam W, Leijte JAP, Yap T, Gallee MPW, Corbishley C et al (2010) Prognostic factors for occult inguinal lymph node involvement in penile carcinoma and assessment of the high-risk EAU subgroup: a two-institution analysis of 342 clinically node-negative patients. Eur Urol 58(5):742–747
Kroon BK, Horenblas S, Lont AP, Tanis PJ, Gallee MPW, Nieweg OE (2005) Patients with penile carcinoma benefit from immediate resection of clinically occult lymph node metastases. J Urol 173(3):816–819
Cabañas R (1977) An approach for the treatment of penile. Cancer 39:456–466
Leijte JAP, Hughes B, Graafland NM, Kroon BK, Olmos RAV, Nieweg OE et al (2009) Two-center evaluation of dynamic sentinel node biopsy for squamous cell carcinoma of the penis. J Clin Oncol 27(20):3325–3329
Woldu SL, Ci B, Hutchinson RC, Krabbe L-M, Singla N, Passoni NM et al (2018) Usage and survival implications of surgical staging of inguinal lymph nodes in intermediate- to high-risk, clinical localized penile cancer: a propensity-score matched analysis. Urol Oncol 36(4):159.e7–159.e17
Vanthoor J, Milenkovic U, Everaerts W, Van Poppel H, De Meerleer G, Dumez H et al (2018) Single centre audit of implementation of a care pathway in penile cancer. Eur Urol Suppl 17(14):e3027
Zhu Y, Gu W-J, Xiao W-J, Wang B-H, Azizi M, Spiess PE et al (2019) Important therapeutic considerations in T1b penile cancer: prognostic significance and adherence to treatment guidelines. Ann Surg Oncol 26(2):685–691
Joshi SS, Handorf E, Strauss D, Correa AF, Kutikov A, Chen DYT et al (2018) Treatment trends and outcomes for patients with lymph node-positive cancer of the penis. JAMA Oncol 4(5):643–649
Cindolo L, Spiess PE, Bada M, Chipollini JJ, Nyirády P, Chiodini P et al (2018) Adherence to EAU guidelines on penile cancer translates into better outcomes: a multicenter international study. World J Urol. https://doi.org/10.1007/s00345-018-2549-3
Breen KJ, O’Connor KM, Power DG, Mayer NJ, Rogers E, Sweeney P (2015) Penile cancer—guideline adherence produces optimum results. Surgeon 13(4):200–206
Campbell RA, Slopnick EA, Ferry EK, Zhu H, Kim SP, Abouassaly R (2017) Disparity between pre-existing management of penile cancer and NCCN guidelines. Urol Oncol 35(8):531.e9–531.e14
Bada M, Berardinelli F, Nyiràdy P, Varga J, Ditonno P, Battaglia M et al (2019) Adherence to the EAU guidelines on penile cancer treatment: European, multicentre, retrospective study. J Cancer Res Clin Oncol 145(4):921–926
Kamel MH, Bissada N, Warford R, Farias J, Davis R (2017) Organ sparing surgery for penile cancer: a systematic review. J Urol 198(4):770–779
Williams SB, Ray-Zack MD, Hudgins HK, Oldenburg J, Trinh Q-D, Nguyen PL et al (2019) Impact of centralizing care for genitourinary malignancies to high-volume providers: a systematic review. Eur Urol Oncol 2:265–273
Guidance on cancer services: improving outcomes in urological cancers—The manual. https://www.nice.org.uk. Accessed 1 Mar 2019
Ayres BE, Hounsome L, Alnajjar H, Sharma D, Verne J, Watkin NA (2014) 50 Has centralisation of penile cancer services in the United Kingdom improved survival? Eur Urol Suppl 13(1):e50
Tang V, Clarke L, Gall Z, Shanks JH, Nonaka D, Parr NJ et al (2014) Should centralized histopathological review in penile cancer be the global standard? BJU Int 114(3):340–343
Matulewicz RS, Flum AS, Helenowski I, Jovanovic B, Palis B, Bilimoria KY et al (2016) Centralization of penile cancer management in the United States: a combined analysis of the American Board of Urology and National Cancer Data Base. Urology 90:82–88
Kamel MH (2019) Should the care of penile cancer be confined to centralized centers of excellence? Eur Urol Focus. https://doi.org/10.1016/j.euf.2019.01.013
Author information
Authors and Affiliations
Consortia
Contributions
JV: data collection and manuscript writing. AT: data collection and manuscript writing. IT: manuscript writing and supervision. MA: manuscript writing and supervision.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Vanthoor, J., Thomas, A., Tsaur, I. et al. Making surgery safer by centralization of care: impact of case load in penile cancer. World J Urol 38, 1385–1390 (2020). https://doi.org/10.1007/s00345-019-02866-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-019-02866-9