Abstract
Objective
Growing literature supports good survival expectancies in bladder cancer (BCa) patients affected by clinical node metastases (cN+) treated with multimodal therapy. We evaluated the role of adjuvant chemotherapy in cN+BCa patients treated with radical cystectomy (RC) and pelvic lymph node dissection (PLND) without neoadjuvant chemotherapy (NAC).
Methods
We evaluated a total of 192 patients with BCa and cN+. All patients were treated with RC and PLND without NAC between 2001 and 2013. Kaplan–Meier analyses and Cox regression analyses were used to assess the impact of adjuvant chemotherapy (ACT) on recurrence, cancer-specific mortality (CSM) and overall mortality (OM) after surgery.
Results
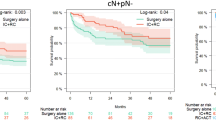
Overall, 99 patients (51.6%) were found without node metastases at RC, while 18 (9.4%), 58 (30.2%) and 17 (8.9%) patients were found pN1, pN2 and pN3, respectively. With a median follow-up of 48 months, in cN+ patients we recorded 5-year recurrence, CSM and OM of 55, 53 and 51%, respectively. Overall, 36 (18.8%) patients were treated with adjuvant chemotherapy. At univariable analyses, ACT was associated with improved overall survival [Hazard ratio (HR): 0.42, confidence interval (CI) 0.20–0.86, p = 0.02) in pN+ subgroup only. These results were confirmed at multivariable analyses, where ACT was associated with improved CSS (HR: 0.45, CI 0.21–0.89, p = 0.03) and OS (HR: 0.37, CI 0.17–0.81, p = 0.01).
Conclusions
We report good survival outcomes in cN+ patients treated with RC. The use of ACT after surgery increases survival expectancies, especially in those patients with pathological node disease. Our data need to be further evaluated in prospective setting.


Similar content being viewed by others
References
Alfred Witjes J, Lebret T, Compérat EM, Cowan NC, De Santis M, Bruins HM et al (2016) Updated 2016 EAU guidelines on muscle-invasive and metastatic bladder cancer. Eur Urol. https://doi.org/10.1016/j.eururo.2016.06.020
Shariat SF, Karakiewicz PI, Palapattu GS, Lotan Y, Rogers CG, Amiel GE et al (2006) Outcomes of radical cystectomy for transitional cell carcinoma of the bladder: a contemporary series from the Bladder Cancer Research Consortium. J Urol 176:2414–2422. https://doi.org/10.1016/j.juro.2006.08.004 (discussion 2422)
Sun M, Abdollah F, Bianchi M, Trinh Q-D, Shariat SF, Jeldres C et al (2012) Conditional survival of patients with urothelial carcinoma of the urinary bladder treated with radical cystectomy. Eur J Cancer 48:1503–1511. https://doi.org/10.1016/j.ejca.2011.11.024
Moschini M, Karnes RJ, Sharma V, Gandaglia G, Fossati N, Dell’Oglio P et al (2016) Patterns and prognostic significance of clinical recurrences after radical cystectomy for bladder cancer: A 20-year single center experience. Eur J Surg Oncol 42(5):735–743. https://doi.org/10.1016/j.ejso.2016.02.011
Stein JP, Lieskovsky G, Cote R, Groshen S, Feng AC, Boyd S et al (2001) Radical cystectomy in the treatment of invasive bladder cancer: long-term results in 1,054 patients. J Clin Oncol 19:666–675
Shariat SF, Palapattu GS, Karakiewicz PI, Rogers CG, Vazina A, Bastian PJ et al (2007) Discrepancy between clinical and pathologic stage: impact on prognosis after radical cystectomy. Eur Urol 51(1):137–149. https://doi.org/10.1016/j.eururo.2006.05.021
Moschini M, Morlacco A, Briganti A, Hu B, Colombo R, Montorsi F et al (2016) Clinical lymphadenopathy in urothelial cancer: a transatlantic collaboration on performance of cross-sectional imaging and oncologic outcomes in patients treated with radical cystectomy without neoadjuvant chemotherapy. Eur Urol Focus. https://doi.org/10.1016/j.euf.2016.11.005
Galsky MD, Stensland K, Sfakianos JP, Mehrazin R, Diefenbach M, Mohamed N et al (2016) Comparative effectiveness of treatment strategies for bladder cancer with clinical evidence of regional lymph node involvement. J Clin Oncol 34:2627–2635. https://doi.org/10.1200/JCO.2016.67.5033
Ho PL, Willis DL, Patil J, Xiao L, Williams SB, Melquist JJ et al (2016) Outcome of patients with clinically node-positive bladder cancer undergoing consolidative surgery after preoperative chemotherapy: the M.D. Anderson Cancer Center Experience. Urol Oncol 34(59):1–8. https://doi.org/10.1016/j.urolonc.2015.08.012
Zargar-Shoshtari K, Zargar H, Lotan Y, Shah JB, van Rhijn BW, Daneshmand S et al (2015) A multi-institutional analysis of outcomes in patients with clinically node positive urothelial bladder cancer treated with induction chemotherapy and radical cystectomy. J Urol. https://doi.org/10.1016/j.juro.2015.07.085
Grossman HB, Natale RB, Tangen CM, Speights VO, Vogelzang NJ, Trump DL et al (2003) Neoadjuvant chemotherapy plus cystectomy compared with cystectomy alone for locally advanced bladder cancer. N Engl J Med 349(9):859–866. https://doi.org/10.1056/nejmoa022148
International Collaboration of Trialists, Medical Research Council Advanced Bladder Cancer Working Party (now the National Cancer Research Institute Bladder Cancer Clinical Studies Group), European Organisation for Research and Treatment of Cancer Genito-Urinary Tract Cancer Group, Australian Bladder Cancer Study Group, National Cancer Institute of Canada Clinical Trials Group, Finnbladder et al (2011) International phase III trial assessing neoadjuvant cisplatin, methotrexate, and vinblastine chemotherapy for muscle-invasive bladder cancer: long-term results of the BA06 30894 trial. J Clin Oncol 29:2171–2177. https://doi.org/10.1200/JCO.2010.32.3139
Dorfman RE, Alpern MB, Gross BH, Sandler MA (1991) Upper abdominal lymph nodes: criteria for normal size determined with CT. Radiology 180:319–322. https://doi.org/10.1148/radiology.180.2.2068292
Greene FL, Page DL, Fleming IDE (2002) Urinary bladder. In: AJCC Cancer Staging Manual. 6 (Edn) Springer, New York
Shariat SF, Svatek RS, Tilki D, Skinner E, Karakiewicz PI, Capitanio U et al (2010) International validation of the prognostic value of lymphovascular invasion in patients treated with radical cystectomy. BJU Int 105:1402–1412. https://doi.org/10.1111/j.1464-410X.2010.09217.x
Novara G, Svatek RS, Karakiewicz PI, Skinner E, Ficarra V, Fradet Y et al (2010) Soft tissue surgical margin status is a powerful predictor of outcomes after radical cystectomy: a multicenter study of more than 4,400 patients. J Urol 183:2165–2170. https://doi.org/10.1016/j.juro.2010.02.021
Daneshmand S, Ahmadi H, Huynh LN, Dobos N (2012) Preoperative staging of invasive bladder cancer with dynamic gadolinium-enhanced magnetic resonance imaging: results from a prospective study. Urology 80:1313–1318. https://doi.org/10.1016/j.urology.2012.07.056
Moschini M, Jeffrey Karnes R, Gandaglia G, Luzzago S, Dell’Oglio P, Rossi MS et al (2016) Preoperative favorable characteristics in bladder cancer patients cannot substitute the necessity of extended lymphadenectomy during radical cystectomy: a sensitivity curve analysis. Urology 88:97–103. https://doi.org/10.1016/j.urology.2015.12.005
Author information
Authors and Affiliations
Contributions
MM Project development, Manuscript writing, Data analysis. AM Project development. JC Project development, Data Collection. SFS Manuscript writing, Data analysis. PDO Project development, Data Collection. EZ Project development, Data Collection. AS Manuscript writing, Data analysis. FM Manuscript writing, Data analysis. AB Project development. RC Project development. AG Project development, Manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standards
All person gave their informed consent to use their data for this retrospective study.
Rights and permissions
About this article
Cite this article
Moschini, M., Mattei, A., Cornelius, J. et al. Surgical treatment for clinical node-positive bladder cancer patients treated with radical cystectomy without neoadjuvant chemotherapy. World J Urol 36, 639–644 (2018). https://doi.org/10.1007/s00345-018-2190-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-018-2190-1