Abstract
Purpose
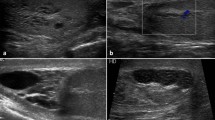
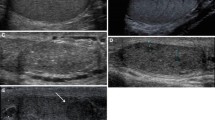
The objective of this study was to assess whether CCDS might improve the outcome of testicular sperm retrieval in patients with azoospermia. Furthermore, we evaluated potential sonographic alterations of the testis before and after trifocal and Micro-TESE.
Methods
78 patients were enrolled prospectively: 24 with obstructive azoospermia (OA) and 54 with non-obstructive azoospermia (NOA). 31 of 54 patients in the NOA group had negative surgical sperm retrieval. Testicular volume, hormonal parameters and sonographical findings were compared before and after TESE. The spermatogenetic score was determined for all retrieval sites. CCDS was performed at the upper, middle and lower segment of the testis. Ultrasound parameters and peak systolic velocity (PSV) were measured pre- and post-operatively.
Results
Testicular volume and epididymal head size were significantly increased in OA patients compared to NOA patients. Ultrasound parameters were comparable between NOA patients with and without successful sperm retrieval. A higher intratesticular PSV was significantly correlated with a better spermatogenic score in the corresponding sonographic position. However, after adjustment for other clinical confounders, PSV does not show a significant influence on the spermatogenic score. Testicular volume decreased significantly in all patients post-operatively after 6 weeks (p < 0.001). Finally, the PSV significantly increased in all patients 24 h after surgery and nearly returned to baseline levels after 6 weeks (p < 0.001).
Conclusions
A higher intratesticular PSV may be helpful as a pre-operative diagnostic parameter in mapping for better sperm retrieval, but CCDS does not help to predict successful testicular sperm retrieval after adjustment for other clinical confounders.


Similar content being viewed by others
References
Jarow JP, Espeland MA, Lipshultz LI (1989) Evaluation of the azoospermic patient. J Urol 142:62–65
Wosnitzer M, Goldstein M, Hardy MP (2014) Review of Azoospermia. Spermatogenesis 4:e28218
Pantke P, Diemer T, Marconi M, Bergmann M, Steger K et al (2008) Testicular sperm retrieval in azoospermic men. Eur Urol Suppl 7:703–714
Marconi M, Keudel A, Diemer Th, Bergmann M, Steger K et al (2012) Combined trifocal and microsurgical testicular sperm extraction is the best technique for testicular sperm retrieval in “low-chance” non-obstructive azoospermia. Eur Urol 62:713–719
Bromage SJ, Falconer DA, Liebermann BA, Sangar V, Payne SR (2007) Sperm retrieval rates in subgroups of primary azoospermic males. Eur Urol 51:534–540
Turunc T, Gul U, Haydardedeoglu B, Bal N, Kuzgunbay B et al (2010) Conventional testicular sperm extraction combined with the microdissection technique in non-obstructive azoospermia patients in a prospective comperative study. Fertil Steril 94:2157–2160
Tüttelmann F, Werny F, Cooper TG, Kliesch S, Simoni M et al (2011) Clinical experience with azoospermia: aetiology and chances for spermatozoa detection upon biopsy. Int J Androl 34:291–298
Schwarzer JU, Steinfatt H, Schleyer M, Köhn FM, Fiedler K et al (2013) No relationship between biopsy sites near the main testicular vessels or rete testis and successful sperm retrieval using conventional or microdissection biopsies in 220 non-obstructive azoospermic men. Asian J Androl 15:795–798
Weidner WHG, Schuppe H-C, Pilatz A, Altinkilic B, Diemer T (2014) Sperm cells for artificial reproduction and germ cell transplantation. Eur Urol Suppl 13:83–88
Abdel Raheem A, Garaffa G, Rushwan N, De Luca F, Zacharakis E et al (2013) Testicular histopathology as a predictor of a positive sperm retrieval in men with non-obstructive azoospermia. BJU Int 111:492–499
Schlegel PN, Su LM (1997) Physiological consequences of testicular sperm extraction. Hum Reprod 12:1688–1692
Ramasamy R, Lin K, Gosden LV, Rosenwaks Z, Palermo GD et al (2009) High serum FSH levels in men with nonobstructive azoospermia do not affect success of microdissection testicular sperm extraction. Fertil Steril 92:590–593
Mitchell V, Robin G, Boitrelle F, Massart P, Marchetti C et al (2011) Correlation between testicular sperm extraction outcomes and clinical, endocrine and testicular histology parameters in 120 azoospermic men with normal serum FSH levels. Int J Androl 34:299–305
Mitchell V, Boitrelle F, Pigny P, Robin G, Marchetti C et al (2010) Seminal plasma levels of anti-Müllerian hormone and inhibin B are not predictive of testicular sperm retrieval in non-obstructive azoospermia: a study of 139 men. Fertil Steril 94:2147–2150
Deruyver Y, Vanderschueren D, van der Aa F (2014) Outcome of microdissection TESE compared with conventional TESE in non-obstructive azoospermia: a systematic review. Andrology 2:20–24
Bryson CF, Ramasamy R, Sheehan M, Palermo GD, Rosenwaks Z et al (2014) Severe testicular atrophy does not affect the success of microdissection testicular sperm extraction. J Urol 191:175–178
Ramasamy R, Ricci JA, Palermo GD, Gosden LV, Rosenwaks Z et al (2009) Successful fertility treatment for Klinefelter’s syndrome. J Urol 182:1108–1113
Aksglaede I, Juul A (2013) Testicular function and fertility in men with Klinefelter syndrome: a review. Eur J Endocrinol 168:R67–R76
Ferhi K, Avakian R, Griveau JF, Guille F (2009) Age as only predictive factor for successful sperm recovery in patients with Klinefelter’s syndrome. Andrologia 41:84–87
Mehta A, Bolyakov A, Roosma J, Schlegel PN, Paduch DA (2013) Successful testicular sperm retrieval in adolescents with Klinefelter syndrome treated with at least 1 year of topical testosterone and aromatase inhibitor. Fertil Steril 100:970–974
Lotti F, Maggi M (2014) Ultrasound of the male genital tract in relation to male reproductive health. Hum Reprod Update 21(1):56–83
Pezzella A, Barbonetti A, D´Andrea S, Necozione S, Micillo A et al (2014) Ultrasonographic caput epididymis diameter is reduced in non-obstructive azoospermia compared with normozoospermia but is not predictive for successful sperm retrieval after TESE. Hum Reprod 29:1368–1374
van Brakel J, de Muinck Keizer-Schrama SM, van Casteren NJ, Hazebroek FW, Dohle GR (2015) Scrotal ultrasound findings in previously congenital and acquired unilateral undescended testes and their contralateral normally descended testis. Andrology 3(5):888–894
Biagiotti G, Cavallini G, Modenini F, Vitali G, Gianaroli L (2002) Spermatogenesis and spectral echo-colour Doppler traces from the main testicular artery. BJU Int 90:903–908
Battaglia C, Giulini S, Regnani G, Di Girolamo R, Paganelli S et al (2000) Seminal plasma nitrite/nitrate and intratesticular Doppler flow in fertile and infertile subjects. Hum Reprod 15:2554–2558
Pinggera GM, Mitterberger M, Bartsch G, Strasser H, Gradl J et al (2008) Assessment of the intratesticular resistive index by colour Doppler ultrasonography measurements as a predictor of spermatogenesis. BJU Int 101:722–726
Herwig R, Tosun K, Pinggera GM, Soelder E, Moeller KT et al (2004) Tissue perfusion essential for spermatogenesis and outcome of testicular sperm extraction (TESE) for assisted reproduction. J Assist Reprod Genet 21:175–180
Nowroozi MR, Ayati M, Amini E, Radkhah K, Jamshidian H et al (2015) Assessment of testicular perfusion prior to sperm extraction predicts success rate and decreases the number of required biopsies in patients with non-obstructive azoospermia. Int Urol Nephrol 47:53–58
Foresta C, Garolla A, Bettella A, Ferlin A, Rossato M et al (1998) Doppler ultrasound of the testis in azoospermic subjects as a parameter of testicular function. Hum Reprod 13:3090–3093
Ramasamy R, Yagan N, Schlegel PN (2005) Structural and functional changes to the testis after conventional versus microdissection testicular sperm extraction. Urology 65:1190–1194
McLachlan RI, Rajpert-De Meyts EK, Hoei-Hansen CE, de Kretser DE, Skakkebaek NE (2007) Histological evaluation of the human testis—approaches to optimizing the clinical value of the assessment: mini review. Hum Reprod 22:2–16
World Health Organization. (2010) WHO laboratory manual for the examination of human semen and sperm-cervical mucus interaction, 5th edn. Cambridge University Press, Cambridge
Pilatz A, Rusz A, Wagenlehner F, Weidner W, Altinkilic B (2013) Reference values for testicular volume, epididymal head size and peak systolic velocity of the testicular artery in adult males measured by ultrasonography. Ultraschall Med 34:349–354
Altinkilic B, Pilatz A, Weidner W (2013) Detection of normal intratesticular perfusion using colour-coded duplex sonography obviates the need for scrotal exploration in patients with clinical suspicion of testicular torsion. J Urol 189:1853–1858
Kliesch S, Bergmann M (2011) Hodenbiopsie. In: Krause W, Weidner W, Sperling H, Diemer T (eds) Andrologie. Thieme, Stuttgart. New York, pp 150–161
R Core Team (2016). R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. ISBN 3-900051-07-0. http://www.R-project.org. Accessed 06 Nov 2016
Christensen RHB (2015) Ordinal—regression models for ordinal data. R package version 2015.6-28. http://www.cran.r-project.org/package=ordinal/. Accessed 06 Nov 2016
Bates D, Maechler M, Bolker B, Walker S (2015) Fitting linear mixed-effects models using lme4. J Stat Softw 67:1–48
Freour T, Com E, Barriere P, Bouchot O, Jean M et al (2013) Comparative proteomic analysis coupled with conventional protein assay as a strategy to identify predictors of successful testicular sperm extraction in patients with non-obstructive azoospermia. Andrology 1(3):414–420
Wang C, Yang C, Chen X, Yao B, Yang C et al (2011) Altered profile of seminal plasma microRNAs in the molecular diagnosis of male infertility. Clin Chem 57(12):1722–1731
Battaglia C, Giulini S, Regnani G, Madgar I, Facchinetti F et al (2001) Intratesticular Doppler flow, seminal plasma nitrites/nitrates, and nonobstructive sperm extraction from patients with obstructive and nonobstructive azoospermia. Fertil Steril 75:1088–1094
Tunc L, Alkibay T, Küpeli B, Tokgöz H, Bozkirli I (2005) Power Doppler ultrasound mapping in nonobstructive azoospermic patients prior to testicular sperm extraction. Arch Androl 51:277–283
Souza CAB, Filho JSL, Fagundes P, Freitas FM, Passos EP (2005) Sperm recovery prediction in azoospermic patients using Doppler ultrasonography. Int Urol Nephrol 37:535–540
Silber SJ (2000) Microsurgical TESE and the distribution of spermatogenesis in non-obstructive azoospermia. Hum Reprod 15:2278–2284
Takada S, Tsujimura A, Ueda T, Matsuoka Y, Takao T et al (2008) Androgen decline in patients with nonobstructive azoospemia after microdissection testicular sperm extraction. Urology 72:114–118
Westlander G, Ekerhovd E, Granberg S, Hanson L, Hanson C et al (2001) Testicular ultrasonography and extended chromosome analysis in men with nonmosaic Klinefelter syndrome: a prospective study of possible predictive factors for successful sperm recovery. Fertil Steril 75:1102–1105
Martinoli C, Pretolesi F, Crespi G, Bianchi S, Gandolfo N et al (1998) Power Doppler sonography: clinical applications. Eur J Radiol 27(Suppl 2):133–140
Eytan O, Har-Toov J, Fait G, Yavetz H, Hauser R et al (2001) Vascularity index distribution within the testis: a technique for guiding testicular sperm extraction. Ultrasound Med Biol 27:1171–1176
Li M, Du J, Wang ZQ, Li FH (2012) The value of sonoelastography scores and the strain ratio in differential diagnosis of azoospermia. J Urol 188:1861–1866
Manning M, Junemann KP, Alken P (1998) Decrease in testosterone blood concentrations after testicular sperm extraction for intracytoplasmic sperm injection in azoospermic men. Lancet 352:37
Schill T, Bals-Pratsch M, Küpker W, Sandmann J, Johannisson R et al (2003) Clinical and endocrine follow-up of patients after testicular sperm extraction. Fertil Steril 79:281–286
Acknowledgements
This study was supported by the DFG (German Research Foundation), KFO 181-2, Proj. 8: Atherosclerosis-related disturbances of spermatogenesis: lessons from the ApoE-/-/LDL receptor-/- knockout mouse model and prospective investigations in men.
Author information
Authors and Affiliations
Contributions
BA: Project development, Data collection, Manuscript writing. AP: Project development, Data collection, Data analysis. TD: Project development, Data collection, Manuscript editing. JW: Data collection, Data analysis. MB: Data collection. SS: Data analysis. UL: Data analysis. HCS: Project development, Data collection. WW: Project development, Manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was approved by the local institutional review board (Ref. No. 26/11).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Altinkilic, B., Pilatz, A., Diemer, T. et al. Prospective evaluation of scrotal ultrasound and intratesticular perfusion by color-coded duplex sonography (CCDS) in TESE patients with azoospermia. World J Urol 36, 125–133 (2018). https://doi.org/10.1007/s00345-017-2039-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-017-2039-z