Abstract
Purpose
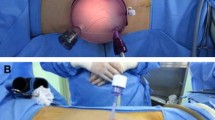
To analyze our preliminary outcomes on the use of 3 mm instruments for laparoscopic live donor nephrectomy (LLDN).
Methods
Our series includes thirteen patients, who underwent LLDN using 3-mm instruments and laparoscope and 5-mm transumbilical trocar. The patients were followed at 7 and 14 days from discharge and were specifically asked about their cosmetic satisfaction. At follow-up, the recipient graft function was controlled, as well as the donor’s cosmetic results. Eight months after surgery, all thirteen patients were asked to fill out the Patient Scar Assessment Questionnaire and Scoring System (PSAQ).
Results
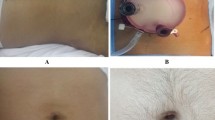
All patients presented good recovery after surgery. Regarding cosmetic outcomes, the donors expressed their satisfaction toward the minimal incision size and optimal esthetic results at 7 and 14 days from discharge home. The low scores on each section of the PSAQ confirmed the favorable outcomes. Early graft function was satisfactory at 1 and 3 months after the kidney transplantation. Furthermore, there were no major complications in the recipients.
Conclusions
Our persistent positive results with the use of 3-mm instruments during LLDN support this technique as a good alternative to the standard laparoscopic approach for minimizing the incision site, while maintaining safety and excellent clinical outcomes. The fact that the general laparoscopic standards are maintained could make this approach a very attractive alternative to the other minimally invasive approaches for live donor nephrectomy. The hope is in that the higher degree of satisfaction in the donor population demonstrated in this study may likely enhance living kidney donation.








Similar content being viewed by others
References
Velidedeoglu E, Williams N, Brayman KL et al (2002) Comparison of open, laparoscopic, and hand-assisted approaches to live-donor nephrectomy. Transplantation 74:169–172
Cadeddu JA, Ratner L, Kavoussi LR (2000) Laparoscopic donor nephrectomy. Semin Laparosc Surg 7:195–199
Ratner LE, Kavoussi LR, Sroka M et al (1997) Laparoscopic assisted live donor nephrectomy—a comparison with the open approach. Transplantation 63:229–233
Chan DY, Ratner LE, Kavoussi LR (1999) Laparoscopic donor nephrectomy: standard of care or unnecessary risk of organ loss? Curr Opin Urol 9:219–222
Park YH, Min SK, Lee JN et al (2004) Comparison of survival probabilities for living-unrelated versus cadaveric renal transplant recipients. Transplant Proc 36:2020–2022. doi:10.1016/j.transproceed.2004.08.122
Harper JD, Breda A, Leppert JT et al (2010) Experience with 750 consecutive laparoscopic donor nephrectomies—is it time to use a standardized classification of complications? J Urol 183:1941–1946. doi:10.1016/j.juro.2010.01.021
Wright AD, Will TA, Holt DR et al (2008) Laparoscopic living donor nephrectomy: a look at current trends and practice patterns at major transplant centers across the United States. J Urol 179:1488–1492. doi:10.1016/j.juro.2007.11.066
Hiller J, Sroka M, Holochek MJ et al (1997) Functional advantages of laparoscopic live-donor nephrectomy compared with conventional open-donor nephrectomy. J Transpl Coord Off Publ North Am Transpl Coord Organ NATCO 7:134–140
Fornara P, Doehn C, Seyfarth M, Jocham D (2000) Why is urological laparoscopy minimally invasive? Eur Urol 37:241–250
Lam JS, Breda A, Schulam PG (2007) Is laparoscopic donor nephrectomy the new standard? Nat Clin Pract Urol 4:186–187. doi:10.1038/ncpuro0755
Alcaraz A, Musquera M, Peri L et al (2011) Feasibility of transvaginal natural orifice transluminal endoscopic surgery-assisted living donor nephrectomy: is kidney vaginal delivery the approach of the future? Eur Urol 59:1019–1025. doi:10.1016/j.eururo.2011.03.021
Canes D, Berger A, Aron M et al (2010) Laparo-endoscopic single site (LESS) versus standard laparoscopic left donor nephrectomy: matched-pair comparison. Eur Urol 57:95–101. doi:10.1016/j.eururo.2009.07.023
Musquera M, Peri L, Izquierdo L et al (2011) Pioneer experience in Spain with LSSS nephrectomy in living donor. Actas Urol Esp 35:559–562. doi:10.1016/j.acuro.2011.04.007
Gill IS, Canes D, Aron M et al (2008) Single port transumbilical (E-NOTES) donor nephrectomy. J Urol 180:637–641. doi:10.1016/j.juro.2008.04.028 (discussion 641)
Gagner M, Garcia-Ruiz A (1998) Technical aspects of minimally invasive abdominal surgery performed with needlescopic instruments. Surg Laparosc Endosc 8:171–179
Soble JJ, Gill IS (1998) Needlescopic urology: incorporating 2-mm instruments in laparoscopic surgery. Urology 52:187–194
Gill IS, Ross JH, Sung GT, Kay R (2000) Needlescopic surgery for cryptorchidism: the initial series. J Pediatr Surg 35:1426–1430. doi:10.1053/jpsu.2000.16405
Durani P, McGrouther DA, Ferguson MW (2009) The patient scar assessment questionnaire: a reliable and valid patient-reported outcomes measure for linear scars. Plast Reconstr Surg 123:1481–1489. doi:10.1097/PRS.0b013e3181a205de
Breda A, Villamizar JM, Faba OR et al (2012) Laparoscopic live donor nephrectomy with the use of 3-mm instruments and laparoscope: initial experience at a tertiary center. Eur Urol 61:840–844. doi:10.1016/j.eururo.2011.11.038
Breda A, Veale J, Liao J, Schulam PG (2007) Complications of laparoscopic living donor nephrectomy and their management: the UCLA experience. Urology 69:49–52. doi:10.1016/j.urology.2006.09.030
Breda A, Bui MH, Liao JC, Schulam PG (2007) Association of bowel rest and ketorolac analgesia with short hospital stay after laparoscopic donor nephrectomy. Urology 69:828–831. doi:10.1016/j.urology.2007.01.083
Breda A, Bui MH, Liao JC et al (2006) Incidence of ureteral strictures after laparoscopic donor nephrectomy. J Urol 176:1065–1068. doi:10.1016/j.juro.2006.04.079
Greco F, Hoda MR, Alcaraz A et al (2010) Laparoscopic living-donor nephrectomy: analysis of the existing literature. Eur Urol 58:498–509. doi:10.1016/j.eururo.2010.04.003
Carvalho GL, Cavazzola LT, Rao P (2013) Minilaparoscopic surgery—not just a pretty face! What can be found beyond the esthetics reasons? J Laparoendosc Adv Surg Tech A 23:710–713. doi:10.1089/lap.2013.0147
Fiori C, Morra I, Bertolo R et al (2013) Standard vs mini-laparoscopic pyeloplasty: perioperative outcomes and cosmetic results. BJU Int 111:E121–E126. doi:10.1111/j.1464-410X.2012.11376.x
Pini G, Goezen AS, Schulze M et al (2012) Small-incision access retroperitoneoscopic technique (SMART) pyeloplasty in adult patients: comparison of cosmetic and post-operative pain outcomes in a matched-pair analysis with standard retroperitoneoscopy: preliminary report. World J Urol 30:605–611. doi:10.1007/s00345-011-0740-x
Tisdale BE, Kapoor A, Hussain A et al (2007) Intact specimen extraction in laparoscopic nephrectomy procedures: Pfannenstiel versus expanded port site incisions. Urology 69:241–244. doi:10.1016/j.urology.2006.09.061
Porpiglia F, Autorino R, Cicione A et al (2014) Contemporary urologic minilaparoscopy: indications, techniques, and surgical outcomes in a multi-institutional european cohort. J Endourol Endourol Soc. doi:10.1089/end.2014.0134
Simforoosh N, Soltani MH, Hosseini Sharifi SH et al (2013) Mini-laparoscopic live donor nephrectomy: initial series. Urol J 10:1054–1058
Jacobs SC, Cho E, Foster C et al (2004) Laparoscopic donor nephrectomy: the University of Maryland 6-year experience. J Urol 171:47–51. doi:10.1097/01.ju.0000100221.20410.4a
Acknowledgments
We wish to thank all the patients participating in the study.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Breda, A., Schwartzmann, I., Emiliani, E. et al. Mini-laparoscopic live donor nephrectomy with the use of 3-mm instruments and laparoscope. World J Urol 33, 707–712 (2015). https://doi.org/10.1007/s00345-014-1360-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-014-1360-z