Abstract
Objective
To compare the outcomes of robotic-assisted laparoscopic prostatectomy (RALP) using a dual versus single-console system in a resident training program using intraoperative, perioperative and postoperative measures.
Methods
Patients with PCa who underwent RALP prior to and after implementing a dual-console system at an academic institution were reviewed from 2006–2012. All surgeries were performed by a single-faculty surgeon well after the learning curve was established. In all cases, chief residents participated in the surgery and performed progressively more portions. Demographic, intraoperative and pathologic parameters were obtained. Continence and erectile function were assessed at 6 and 12 months. Postoperative complications were graded using the Clavien–Dindo classification. Predictors of outcomes on univariate analysis were included in multivariate logistic or linear models.
Results
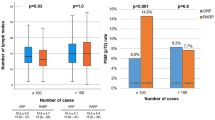
Of 381 patients, 185 and 196 underwent single- or dual-console RALP, respectively. There was a significant decrease in mean operative time using the dual-console system (222 vs. 171 min, p < 0.0001) as well as in the incidence of intraoperative complications (8.65 vs. 1.53 %, p < 0.0001) and postoperative complications (14.1 vs. 6.63 %, p = 0.03.) Complications of Clavien grade ≥3a occurred more frequently with a single-console system (7 vs. 1 %, p = 0.003.) Differences persisted when controlling for potential confounders by multivariate regression. Postoperative measures of continence, erectile function and the rate of biochemical recurrence were similar between cohorts.
Conclusions
When training resident surgeons to perform RALP, a dual-console system may improve intraoperative and perioperative outcomes. The dual-console may represent a safer, more efficient modality for robotic surgical education as compared to a single-console system.

Similar content being viewed by others
References
Stitzenberg KB, Wong YN, Nielsen ME, Egleston BL, Uzzo RG (2012) Trends in radical prostatectomy: centralization, robotics, and access to urologic cancer care. Cancer 118:54–62
Melloul E, Raptis DA, Boss A et al (2014) Small animal magnetic resonance imaging: an efficient tool to assess liver volume and intrahepatic vascular anatomy. J Surg Res 187(2):458–465
Buchs NC, Pugin F, Volonte F, Morel P (2013) Learning tools and simulation in robotic surgery: state of the art. World J Surg 37:2812–2819
Fernandes E, Elli E, Giulianotti P (2014) The role of the dual-console in robotic surgical training. Surgery 155(1):1–4
Hanly EJ, Miller BE, Kumar R et al (2006) Mentoring console improves collaboration and teaching in surgical robotics. J Laparoendosc Adv Surg Tech A 16:445–451
Smith AL, Krivak TC, Scott EM et al (2012) Dual-console robotic surgery compared to laparoscopic surgery with respect to surgical outcomes in a gynecologic oncology fellowship program. Gynecol Oncol 126:432–436
Thiel DD, Hutchinson R, Diehl N, Tavlarides A, Williams A, Parker AS (2012) Impact of fellowship training on one-year outcomes of robotic-assisted prostatectomy. JSLS: J Soc Laparoendoscopic Surg/Soc Laparoendoscopic Surg 16:195–201
Herrell SD, Smith JA Jr (2005) Robotic-assisted laparoscopic prostatectomy: what is the learning curve? Urology 66:105–107
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Schreuder HW, Wolswijk R, Zweemer RP, Schijven MP, Verheijen RH (2012) Training and learning robotic surgery, time for a more structured approach: a systematic review. BJOG Int J Obstet Gynaecol 119:137–149
Author information
Authors and Affiliations
Corresponding author
Additional information
Monica S.C. Morgan and Nabeel A. Shakir contributed equally to the development of this manuscript.
Rights and permissions
About this article
Cite this article
Morgan, M.S.C., Shakir, N.A., Garcia-Gil, M. et al. Single- versus dual-console robot-assisted radical prostatectomy: impact on intraoperative and postoperative outcomes in a teaching institution. World J Urol 33, 781–786 (2015). https://doi.org/10.1007/s00345-014-1349-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-014-1349-7