Abstract
Objectives
The objectives of the study were to describe a novel score (safe-R), combining information on surgical margin status (SM) and extend of nerve-sparing (NS) applicable for all patients undergoing radical prostatectomy (RP), and to test the impact of our frozen-section navigated nerve-sparing approach (NeuroSAFE) on safe-R score.
Methods
We retrospectively analyzed 9,635 RPs performed at our center between 2002 and 2011. Of these, 47 % were conducted with NeuroSAFE. Proportions of NS and SM status were assessed. Subsequently, a score for oncological safe NS (safe-R) was developed; Safe-R was categorized as 3 (for negative SM and bilateral NS), 2 (for negative SM and unilateral NS), 1 (for negative SM without NS), and 0 (for patients with positive SM), respectively. The impact of NeuroSAFE on safe-R was analyzed by chi-square test and confirmed by multinomial logistic regression, adjusting for preoperative risk factors.
Results
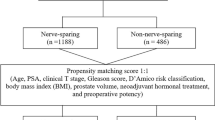
Applying NeuroSAFE resulted in enhanced safe-R score, indicating lower rates of positive SM and higher rates of NS, across all risk categories (all p < 0.001). For example in high-risk patients, NeuroSAFE resulted in lower proportions of safe-R 0 (27.6 vs. 33.6 %) and higher proportions of safe-R 3 (32.4 vs. 17.1 %, p < 0.001). Linkage between the NeuroSAFE approach and safe-R was confirmed after multinomial logistic adjustment for preoperative risk factors. All results were confirmed in a propensity-matched cohort (matched for preoperative risk factors and year of surgery, data not shown).
Conclusion
Safe-R represents a novel tool to assess and report on oncological safe nerve-sparing in RP. NeuroSAFE is associated with enhanced safe-R scores.

Similar content being viewed by others
References
Bill-Axelson A, Holmberg L, Ruutu M et al (2011) Radical prostatectomy versus watchful waiting in early prostate cancer. N Engl J Med 364(18):1708–1717
Budaus L, Isbarn H, Schlomm T et al (2009) Current technique of open intrafascial nerve-sparing retropubic prostatectomy. Eur Urol 56(2):317–324
Schlomm T, Heinzer H, Steuber T et al (2011) Full functional-length urethral sphincter preservation during radical prostatectomy. Eur Urol 60(2):320–329
Rocco F, Carmignani L, Acquati P et al (2006) Restoration of posterior aspect of rhabdosphincter shortens continence time after radical retropubic prostatectomy. J Urol 175(6):2201–2206
Rabbani F, Stapleton AM, Kattan MW, Wheeler TM, Scardino PT (2000) Factors predicting recovery of erections after radical prostatectomy. J Urol 164(6):1929–1934
Pierorazio PM, Spencer BA, McCann TR, McKiernan JM, Benson MC (2007) Preoperative risk stratification predicts likelihood of concurrent PSA-free survival, continence, and potency (the trifecta analysis) after radical retropubic prostatectomy. Urology 70(4):717–722
Loeb S, Smith ND, Roehl KA, Catalona WJ (2007) Intermediate-term potency, continence, and survival outcomes of radical prostatectomy for clinically high-risk or locally advanced prostate cancer. Urology 69(6):1170–1175
Graefen M, Haese A, Pichlmeier U et al (2001) A validated strategy for side specific prediction of organ confined prostate cancer: a tool to select for nerve sparing radical prostatectomy. J Urol 165(3):857–863
Steuber T, Graefen M, Haese A et al (2006) Validation of a nomogram for prediction of side specific extracapsular extension at radical prostatectomy. J Urol 175(3 Pt 1):939–944 discussion 944
Bianco FJ Jr, Scardino PT, Eastham JA (2005) Radical prostatectomy: long-term cancer control and recovery of sexual and urinary function (“trifecta”). Urology 66(5):83–94
Patel VR, Sivaraman A, Coelho RF et al (2011) Pentafecta: a new concept for reporting outcomes of robot-assisted laparoscopic radical prostatectomy. Eur Urol 59(5):702–707
Schlomm T, Tennstedt P, Huxhold C et al (2012) Neurovascular structure-adjacent frozen-section examination (NeuroSAFE) increases nerve-sparing frequency and reduces positive surgical margins in open and robot-assisted laparoscopic radical prostatectomy: experience after 11 069 consecutive patients. Eur Urol 62(2):333–340
D’Amico AV, Whittington R, Malkowicz SB et al (2001) Predicting prostate specific antigen outcome preoperatively in the prostate specific antigen era. J Urol 166(6):2185–2188
McNeal JE, Redwine EA, Freiha FS, Stamey TA (1988) Zonal distribution of prostatic adenocarcinoma. Correlation with histologic pattern and direction of spread. Am J Surg Pathol 12(12):897–906
Gleason DF, Mellinger GT (1974) Prediction of prognosis for prostatic adenocarcinoma by combined histological grading and clinical staging. J Urol 111(1):58–64
Stampf S. Nonrandom: stratification and matching by the propensity score. R package v.11. http://cran.r-project.org. Accessed 21 Sep 2012
Johansson E, Steineck G, Holmberg L et al (2011) Long-term quality-of-life outcomes after radical prostatectomy or watchful waiting: the Scandinavian Prostate Cancer Group-4 randomised trial. Lancet Oncol 12(9):891–899
von Bodman C, Brock M, Roghmann F et al (2013) Intraoperative frozen section of the prostate decreases positive margin rate while ensuring nerve sparing procedure during radical prostatectomy. J Urol 190(2):515–520
Roder MA, Thomsen FB, Christensen IJ et al. (2012) Risk factors associated with positive surgical margins following radical prostatectomy for clinically localized prostate cancer: Can nerve-sparing surgery increase the risk? Scand J Urol (Epub ahead of print)
Budaus L, Isbarn H, Eichelberg C et al (2010) Biochemical recurrence after radical prostatectomy: multiplicative interaction between surgical margin status and pathological stage. J Urol 184(4):1341–1346
Epstein JI (1990) Evaluation of radical prostatectomy capsular margins of resection. The significance of margins designated as negative, closely approaching, and positive. Am J Surg Pathol 14(7):626–632
Ackerman DA, Barry JM, Wicklund RA, Olson N, Lowe BA (1993) Analysis of risk factors associated with prostate cancer extension to the surgical margin and pelvic node metastasis at radical prostatectomy. J Urol 150(6):1845–1850
Singer PA, Tasch ES, Stocking C, Rubin S, Siegler M, Weichselbaum R (1991) Sex or survival: trade-offs between quality and quantity of life. J Clin Oncol 9(2):328–334
Begg CB, Riedel ER, Bach PB et al (2002) Variations in morbidity after radical prostatectomy. N Engl J Med 346(15):1138–1144
Moinpour CM, Hayden KA, Unger JM et al (2008) Health-related quality of life results in pathologic stage C prostate cancer from a Southwest oncology group trial comparing radical prostatectomy alone with radical prostatectomy plus radiation therapy. J Clin Oncol 26(1):112–120
Walz J, Joniau S, Chun FK et al (2011) Pathological results and rates of treatment failure in high-risk prostate cancer patients after radical prostatectomy. BJU Int 107(5):765–770
Chun FK, Haese A, Ahyai SA et al (2008) Critical assessment of tools to predict clinically insignificant prostate cancer at radical prostatectomy in contemporary men. Cancer 113(4):701–709
Boorjian SA, Eastham JA, Graefen M et al (2012) A critical analysis of the long-term impact of radical prostatectomy on cancer control and function outcomes. Eur Urol 61(4):664–675
Sonn GA, Chang E, Natarajan S et al. (2013) Value of targeted prostate biopsy using magnetic resonance-ultrasound fusion in men with prior negative biopsy and elevated prostate-specific antigen. Eur Urol
Cangiano TG, Litwin MS, Naitoh J, Dorey F, deKernion JB (1999) Intraoperative frozen section monitoring of nerve sparing radical retropubic prostatectomy. J Urol 162(3 Pt 1):655–658
Goharderakhshan RZ, Sudilovsky D, Carroll LA, Grossfeld GD, Marn R, Carroll PR (2002) Utility of intraoperative frozen section analysis of surgical margins in region of neurovascular bundles at radical prostatectomy. Urology 59(5):709–714
Conflict of interests
The authors declare that they have no conflict of interest.
Ethical standard
The authors confirm that the study has been performed in accordance with the ethical standards laid down in the Declaration of Helsinki 1964 and its later amendments. All patients gave their informed consent prior to their inclusion in the study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Andreas Becker and Carolina Coelius have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Becker, A., Coelius, C., Adam, M. et al. Safe-R: a novel score, accounting for oncological safe nerve-sparing at radical prostatectomy for localized prostate cancer. World J Urol 33, 77–83 (2015). https://doi.org/10.1007/s00345-014-1273-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-014-1273-x