Abstract
Purpose
The purpose of the study was to evaluate the utility of a 3 T pelvic magnetic resonance imaging (MRI) in detecting a local recurrence in post-prostatectomy prostate cancer patients prior to receiving adjuvant or salvage intensity-modulated radiation therapy (IMRT).
Methods
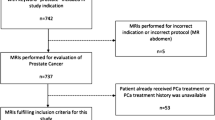
Ninety prostate cancer patients status post-prostatectomy with rising prostate-specific antigen (PSA) had a 3 T pelvic MRI prior to IMRT. The following variables were analyzed for predicting positive findings on MRI: initial presenting and initial post-op PSA, PSA at the time of imaging, PSA velocity, surgical margins, Gleason score, pathological stage, pre-RT digital rectal examination, and type of surgical prostatectomy.
Results
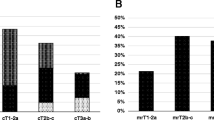
The only significant variable predictive of a positive MRI was positive margins. Specifically, 15 of 46 (33 %) patients with positive margins had a positive MRI, while 5 of 44 (11 %) patients with negative margins had a positive MRI. In the MRI positive group, the location of the positive findings on MRI corresponded with the pathology report in 9 of 12 (75 %) cases.
Conclusion
Post-prostatectomy patients with pathologic positive margins are three times more likely to have positive findings on a 3 T MRI.
Similar content being viewed by others
References
Akin O, Gultekin DH, Vargas HA et al (2011) Incremental value of diffusion weighted and dynamic contrast enhanced MRI in the detection of locally recurrent prostate cancer after radiation treatment: preliminary results. Eur Radiol 21:1970–1978
Bolla M, Van Poppel H, Collette L et al (2005) Postoperative radiotherapy after radical prostatectomy: a randomised controlled trial (EORTC trial 22911). Lancet 366:572–578
Casciani E, Polettini E, Carmenini E et al (2008) Endorectal and dynamic contrast-enhanced MRI for detection of local recurrence after radical prostatectomy. AJR Am J Roentgenol 190:1187–1192
Cirillo S, Petracchini M, Scotti L et al (2009) Endorectal magnetic resonance imaging at 1.5 Tesla to assess local recurrence following radical prostatectomy using T2-weighted and contrast-enhanced imaging. Eur Radiol 19:761–769
Eastham JA, Kuroiwa K, Ohori M et al (2007) Prognostic significance of location of positive margins in radical prostatectomy specimens. Urology 70:965–969
Fuchsjager MH, Pucar D, Zelefsky MJ et al (2010) Predicting post-external beam radiation therapy PSA relapse of prostate cancer using pretreatment MRI. Int J Radiat Oncol Biol Phys 78:743–750
Fuchsjager MH, Shukla-Dave A, Hricak H et al (2009) Magnetic resonance imaging in the prediction of biochemical recurrence of prostate cancer after radical prostatectomy. BJU Int 104:315–320
Giannarini G, Nguyen DP, Thalmann GN et al (2012) Diffusion-weighted magnetic resonance imaging detects local recurrence after radical prostatectomy: initial experience. Eur Urol 61:616–620
Hricak H, Schoder H, Pucar D et al (2003) Advances in imaging in the postoperative patient with a rising prostate-specific antigen level. Semin Oncol 30:616–634
Leventis AK, Shariat SF, Kattan MW et al (2001) Prediction of response to salvage radiation therapy in patients with prostate cancer recurrence after radical prostatectomy. J Clin Oncol 19:1030–1039
Martino P, Scattoni V, Galosi AB et al (2011) Role of imaging and biopsy to assess local recurrence after definitive treatment for prostate carcinoma (surgery, radiotherapy, cryotherapy, HIFU). World J Urol 29:595–605
Mckenna DA, Coakley FV, Westphalen AC et al (2008) Prostate cancer: role of pretreatment MR in predicting outcome after external-beam radiation therapy—initial experience. Radiology 247:141–146
Michalski JM, Lawton C, El Naqa I et al (2010) Development of RTOG consensus guidelines for the definition of the clinical target volume for postoperative conformal radiation therapy for prostate cancer. Int J Radiat Oncol Biol Phys 76:361–368
Moman MR, Van Den Berg CA, Boeken Kruger AE et al (2010) Focal salvage guided by T2-weighted and dynamic contrast-enhanced magnetic resonance imaging for prostate cancer recurrences. Int J Radiat Oncol Biol Phys 76:741–746
National Comprehensive Cancer Network. Prostate Cancer (Version 1.2014). http://www.nccn.org/professionals/physician_gls/pdf/prostate.pdf. Accessed 11 March 2014
Olsen J, Parikh P (2011) Calypso real-time localization and tracking for treatment of prostate cancer with external beam radiotherapy. Image Guided Radiation Therapy. McGraw-Hill, New York, pp 407–410
Pucar D, Sella T, Schoder H (2008) The role of imaging in the detection of prostate cancer local recurrence after radiation therapy and surgery. Curr Opin Urol 18:87–97
Rouviere O (2012) Imaging techniques for local recurrence of prostate cancer: for whom, why and how? Diagn Interv Imaging 93:279–290
Thompson IM Jr, Tangen CM, Paradelo J et al (2006) Adjuvant radiotherapy for pathologically advanced prostate cancer: a randomized clinical trial. JAMA 296:2329–2335
Wiegel T, Bottke D, Steiner U et al (2009) Phase III postoperative adjuvant radiotherapy after radical prostatectomy compared with radical prostatectomy alone in pT3 prostate cancer with postoperative undetectable prostate-specific antigen: ARO 96-02/AUO AP 09/95. J Clin Oncol 27:2924–2930
Willoughby TR, Kupelian PA, Pouliot J et al (2006) Target localization and real-time tracking using the Calypso 4D localization system in patients with localized prostate cancer. Int J Radiat Oncol Biol Phys 65:528–534
Yakar D, Hambrock T, Huisman H et al (2010) Feasibility of 3T dynamic contrast-enhanced magnetic resonance-guided biopsy in localizing local recurrence of prostate cancer after external beam radiation therapy. Invest Radiol 45:121–125
Conflict of interest
There are no conflicts of interest associated with this manuscript by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Verma, V., Chen, L., Michalski, J.M. et al. Evaluation of 3 T pelvic MRI imaging in prostate cancer patients receiving post-prostatectomy IMRT. World J Urol 33, 69–75 (2015). https://doi.org/10.1007/s00345-014-1269-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-014-1269-6