Abstract
Purpose
Bladder dysfunction, secondary to diabetes, is mainly characterized by poor bladder emptying and overflow incontinence. However, there is evidence in literature that storage symptoms, as those suggestive for overactive bladder (OAB), may also affect people with diabetes. The aim of this study was to evaluate the prevalence of overactive bladder, the complaint of urinary urgency with/without urge incontinence, usually with frequency and nocturia, in people with diabetes compared to healthy subjects (control group).
Methods
Symptoms were assessed through the overactive bladder questionnaire (OAB-q), an investigative tool, specifically developed for OAB diagnosis.
Results
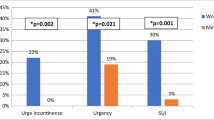
OAB-q scores resulted higher in diabetic people than those of the control group. Age and disease duration resulted in measurements that showed a statistical correlation with the OAB-q scores.
Conclusions
OAB symptoms are more prevalent in diabetic people than in non-diabetic people. This prompts further research to determine whether the onset of OAB symptoms can be considered as an indicator of diabetic neuropathy.
Similar content being viewed by others
Abbreviations
- BOO:
-
Bladder outlet obstruction
- DM:
-
Diabetes mellitus
- DO:
-
Detrusor overactivity
- LUTS:
-
Lower urinary tract symptoms
- MMSE:
-
Mini-mental state examination
- OAB:
-
Overactive bladder
- OAB-q:
-
Overactive bladder questionnaire
- UTI:
-
Urinary tract infection
References
Abrams P, Cardozo L, Fall M, Griffiths D, Rosier P, Ulmstein U, Van Kerrebroek P, Victor A, Wein A (2003) The standardization of terminology of lower urinary tract function: report from the standardisation sub-committee of the International Continence Society. Urology 61(1):37–49
Genuth S, Alberti KG, Bennett P, Buse J, Defronzo R, Kahn R, Kitzmiller J, Knowler WC, Lebovitz H, Lernmark A, Nathan D, Palmer J, Rizza R, Saudek C, Shaw J, Steffes M, Stern M, Tuomilehto J, Zimmet P (2003) Report of the expert committee on the diagnosis and classification of diabetes mellitus. Diabetes Care 26(1):S5–S20
Coyne K, Revicki D, Hunt T, Correy R, Stuart W, Bentkover J, Kurth H, Abrams P (2002) Psychometric validation of an overactive bladder symptom and health-related quality of life questionnaire: the OAB-q. Qual Life Res 11(6):563–574
Coyne KS, Tubaro A, Brubacker L, Bavendam T (2006) Development and validation of patient reported outcome measures for overactive bladder: a review of concepts. Urology 2006
Wiedemann A, Fugsen I (2010) The patient with diabetes in urologic practice: a special risk for lower urinary tract symptoms? Results of the Witten diabetes survey of 4071 type 2 diabetics. Urol A 49(2):238–244
Pannek J (2010) Diagnosis and therapy of functional disorders of the bladder in persons with diabetes mellitus. What do we actually know? Urol A 49(3):381–386
Daneshgari F, Liu G, Birder L, Hanna-Mitchell AT, Chacko S (2009) Diabetic bladder dysfunction: current translational knowledge. J Urol 182(6 Suppl):S18–S26
Lee WC, Wu HP, Tai TY, Yu HJ, Chiang PH (2009) Investigation of urodynamic characteristics and bladder sensory function in the early stages of diabetic bladder dysfunction in women with type 2 diabetes. J Urol 181(1):198–203
Ding J, Qi L, Zu X, Shen P (2010) Urodynamic studies on benign prostatic hyperplasia combined with diabetes mellitus. Zhong Nan Da Xue Xue Bao Yi Xue Ban 35(7):705–710
Ho CH, Tai HC, Yu HJ (2010) Urodynamic findings in female diabetic patients with and without overactive bladder symptoms. Neurourol Urodyn 29(3):424–427
Tong YC, Cheng JT (2007) Aldose reductase inhibitor ONO-2235 restores the alterations of bladder nerve growth factor and neurotrophin receptor p75 genetic expression in streptozotocin induced diabetic rats. J Urol 178(5):2203–2207
Atalik KE, Okudan N, Gokbel H, Kalkan S, Cuce G (2010) Diabetes mellitus- and cooling-induced bladder contraction: an in vitro study. J Smooth Muscle Res 46(4):175–183
Fayyad AM, Hill SR, Jones G (2009) Prevalence and risk factors for bothersome lower urinary tract symptoms in women with diabetes mellitus from hospital-based diabetes clinic. Int Urogynecol J 20:1339–1344
Yamaguchi C, Sakakibara R, Uchiyama T, Yamamoto T, Ito T, Liu Z, Awa Y, Yamamoto K, Nomura F, Yamanishi T, Hattori T (2007) Overactive bladder in diabetes: a peripheral or central mechanism? Neurourol Urodyn 26(6):807–813
Iacovelli E, Gilio F, Meco G, Fattapposta F, Vanacore N, Brusa L, Giacomelli E, Gabriele M, Rubino A, Locuratolo N, Iani C, Pichiorri F, Colosimo C, Carbone A, Palleschi G, Inghilleri M (2010) Bladder symptoms assessed with overactive bladder questionnaire in Parkinson’s disease. Mov Dis 25(9):1203–1209
Tubaro A (2004) Defining overactive bladder: epidemiology and burden of disease. Urology 64(6 Suppl 1):2–6
Fayyad AM, Hill SR, Jones G (2010) Urine production and bladder diary measurements in women with type 2 diabetes mellitus and their relation to lower urinary tract symptoms and voiding dysfunction. Neurourol Urodyn 29(3):354–358
Lin TL, Chen GD, Chen YC, Huang CN, Ng SC (2012) Aging and recurrent urinary tract infections are associated with bladder dysfunction in type 2 diabetes. Source Dep Living Sci Nat Open Univ Taiwan 51(3):381–386
Devore EE, Townsend MK, Resnick NM, Grodstein F (2012) The epidemiology of urinary incontinence in women with type 2 diabetes. J Urol 188(5):1816–1821
Wang Z, Cheng Z, Cristofaro V, Li J, Xiao X, Gomez P, Ge R, Gong E, Strle K, Sullivan MP, Adam RM, White MF (2012) Olumi AF Inhibition of TNF-α improves the bladder dysfunction that is associated with type 2 diabetes. Diabetes 61(8):2134–2145
Liu RT, Chung MS, Chuang YC, Lee JJ, Lee WC, Chang HW, Yang KD, Chancellor MB (2012) The presence of overactive bladder wet increased the risk and severity of erectile dysfunction in men with type 2 diabetes. J Sex Med 9(7):1913–1922
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Palleschi, G., Pastore, A.L., Maggioni, C. et al. Overactive bladder in diabetes mellitus patients: a questionnaire-based observational investigation. World J Urol 32, 1021–1025 (2014). https://doi.org/10.1007/s00345-013-1175-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-013-1175-3