Abstract
Purpose
The aim of this study was to examine urinary tract infection (UTI) associated with conditions causing urinary tract obstruction and stasis, excluding urolithiasis and neuropathic bladder dysfunction.
Methods
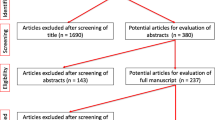
An electronic literature search was performed using the key words urinary tract infection (UTI), benign prostatic hyperplasia (BPH), hydronephrosis, obstruction, reflux, diverticulum, urethra, and stricture. In total, 520 abstracts were reviewed, 210 articles were studied in detail, and 36 were included as references.
Results
It is one of the axioms of Urological practice that urinary tract obstruction and stasis predispose to UTI. Experimental studies indicate that, whereas transurethral inoculates of bacteria are rapidly eliminated from the normal bladder, urethral obstruction leads to cystitis, pyelonephritis, and bacteremia. BPH is, next to urolithiasis, the most common cause of urinary tract obstruction predisposing to UTI. Urethral stricture remains a common cause of UTI in many parts of the world. Urinary stasis in diverticula of the urethra or bladder predisposes to UTI. Experimental studies have shown that, whereas the normal kidney is relatively resistant to infection by organisms injected intravenously, ureteric obstruction predisposes to pyelonephritis. It also causes renal dysfunction which impairs the excretion of antibiotics in the urine, making eradication of bacteria difficult.
Conclusions
In patients with UTI and urinary tract obstruction, targeted antibiotic treatment according to urine culture should be complemented with urgent drainage (bladder catheterization, percutaneous nephrostomy or ureteric stenting) followed by definitive surgery to remove the cause of obstruction or stasis once infection is under control.


Similar content being viewed by others
References
Lipsky BA (1989) Urinary tract infections in men. Epidemiology, pathophysiology, diagnosis, and treatment. Ann Intern Med 110(2):138–150
Johnson DE, Russell RG, Lockatell CV, Zulty JC, Warren JW (1993) Urethral obstruction of 6 hours or less causes bacteriuria, bacteremia, and pyelonephritis in mice challenged with “nonuropathogenic” Escherichia coli. Infect Immun 61(8):3422–3428
Riehmann M, Goetzman B, Langer E, Drinka PJ, Rhodes PR, Bruskewitz RC (1994) Risk factors for bacteriuria in men. Urology 43(5):617–620
Payne SR, Timoney AG, McKenning ST, den Hollander D, Pead LJ, Maskell RM (1988) Microbiological look at urodynamic studies. Lancet 2:1123–1126
Holtgrewe HL, Mebust WK, Dowd JB, Cockett AT, Peters PC, Proctor C (1989) Transurethral prostatectomy: practice aspects of the dominant operation in American urology. J Urol 141:248–253
McConnell JD, Roehrborn CG, Bautista OM, Andriole GL Jr, Dixon CM, Kusek JW, Lepor H, McVary KT, Nyberg LM Jr, Clarke HS, Crawford ED, Diokno A, Foley JP, Foster HE, Jacobs SC, Kaplan SA, Kreder KJ, Lieber MM, Lucia MS, Miller GJ, Menon M, Milam DF, Ramsdell JW, Schenkman NS, Slawin KM, Smith JA, Medical Therapy of Prostatic Symptoms (MTOPS) Research Group (2003) The long-term effect of doxazosin, finasteride and the combination on the clinical progression of benign prostatic hyperplasia. N Engl J Med 349(25):2387–2398
Miller J, Ludwig M, Schroeder-Printzen I, Schiefer HG, Weidner W (1996) Transurethral laser therapy and urinary tract infections. Ann Urol (Paris) 30(3):131–138
Nickel JC, Downey J, Young I, Boag S (1999) Asymptomatic inflammation and/or infection in benign prostatic hyperplasia. BJU Int 84(9):976–981. Comment in: BJU Int 2000;85(9):1155–1156
Ohkawa M, Shimamura M, Tokunaga S, Nakashima T, Orito M (1993) Bacteremia resulting from prostatic surgery in patients with or without preoperative bacteriuria under perioperative antibiotic use. Chemotherapy 39(2):140–146
Hochreiter WW (2008) The issue of prostate cancer evaluation in men with elevated prostate-specific antigen and chronic prostatitis. Andrologia 40(2):130–133
König JE, Senge T, Allhoff EP, König W (2005) Analysis of the inflammatory network in benign prostate hyperplasia and prostate cancer. Prostate 2004;58(2):121–129. Comment in: J Urol 173(1):161
Santucci RA, Joyce GF, Wise M (2007) Male urethral stricture disease. J Urol 177(5):1667–1674
Blacklock AR, Geddes JR, Shaw RE (1983) The treatment of large bladder diverticula. Br J Urol 55:17–20
Pieretti RV, Pieretti-Vanmarcke RV (1999) Congenital bladder diverticula in children. J Pediatr Surg 34:468–473
Adot Zurbano JM, Salinas Casado J, Dambros M, Virseda Chamorro M, Ramírez Fernández JC, Silmi Moyano A, Marcos Díaz J (2005) Urodynamics of the bladder diverticulum in the adult male [Article in Spanish] Arch Esp Urol 58(7):641–649
Daneshgari F, Zimmern PE, Jacomides L (1999) Magnetic resonance imaging detection of symptomatic noncommunicating intraurethral wall diverticula in women. J Urol 161:1259–1261
Romanzi LJ, Groutz A, Blaivas JG (2000) Urethral diverticulum in women: diverse presentations resulting in diagnostic delay and mismanagement. J Urol 164:428–433
Schaeffer AJ, Schaeffer EM (2007) Infections of the urinary tract. In: Wein AJ, Kavoussi LR, Novick AC, Partin AW, Peters CA (eds) Campbell-Walsh Urology, Vol 1, 9th edn. Elsevier, Philadelphia, Chapter 8, pp 221–303
Cox CE, Hinman F Jr (1961) Experiments with induced bacteriuria, vesical emptying and bacterial growth on the mechanism of bladder defense to infection. J Urol 86:739–748
Smellie J, Edwards D, Hunter N, Normand IC, Prescod N (1975) Vesico-ureteric reflux and renal scarring. Kidney Int Suppl 4:S65–S72
Beeson PB, Guze LB (1956) Experimental pyelonephritis: I. Effect of ureteral ligation on the course of bacterial infection in the kidney of the rat. J Exp Med 104:803–815
Bitz H, Darmon D, Goldfarb M, Shina A, Block C, Rosen S, Brezis M, Heyman SN (2001) Transient urethral obstruction predisposes to ascending pyelonephritis and tubulo-interstitial disease: studies in rats. Urol Res 29(1):67–73
Song SH, Lee SB, Park YS, Kim KS (2007) Is antibiotic prophylaxis necessary in infants with obstructive hydronephrosis? J Urol 177(3):1098–1101; discussion 1101
Coelho GM, Bouzada MC, Lemos GS, Pereira AK, Lima BP, Oliveira EA (2008) Risk factors for urinary tract infection in children with prenatal renal pelvic dilatation. J Urol 179(1):284–289
Lee JH, Choi HS, Kim JK, Won HS, Kim KS, Moon DH, Cho KS, Park YS (2008) Nonrefluxing neonatal hydronephrosis and the risk of urinary tract infection. J Urol 179(4):1524–1528
Roth CC, Hubanks JM, Bright BC, Heinlen JE, Donovan BO, Kropp BP, Frimberger D (2009) Occurrence of urinary tract infection in children with significant upper urinary tract obstruction. Urology 73(1):74–78
Eknoyan G, Qunibi WY, Grissom RT, Tuma SN, Ayus JC (1982) Renal papillary necrosis: An update. Medicine (Baltimore) 61:55–73
Gross AJ, Herrmann TR (2007) Management of stones in calyceal diverticulum. Curr Opin Urol 17(2):136–140
Roberts JA (1999) Management of pyelonephritis and upper urinary tract infections. Urol Clin North Am 26(4):753–763
Lane MC, Mobley HL (2007) Role of P-fimbrial-mediated adherence in pyelonephritis and persistence of uropathogenic Escherichia coli (UPEC) in the mammalian kidney. Kidney Int 72(1):19–25
Tseng CC, Huang JJ, Ko WC, Yan JJ, Wu JJ (2001) Decreased predominance of papG class II allele in Escherichia coli strains isolated from adults with acute pyelonephritis and urinary tract abnormalities. J Urol 166(5):1643–1646
Johansen TE (2004) The role of imaging in urinary tract infections. World J Urol 22(5):392–398
Mitterberger M, Pinggera GM, Colleselli D, Bartsch G, Strasser H, Steppan I, Pallwein L, Friedrich A, Gradl J, Frauscher F (2008) Acute pyelonephritis: comparison of diagnosis with computed tomography and contrast-enhanced ultrasonography. BJU Int 101(3):341–344
Abarbanel J, Engelstein D, Lask D, Livne PM (2003) Urinary tract infection in men younger than 45 years of age: is there a need for urologic investigation? Urology 62(1):27–29
Hsu CY, Fang HC, Chou KJ, Chen CL, Lee PT, Chung HM (2006) The clinical impact of bacteremia in complicated acute pyelonephritis. Am J Med Sci 332(4):175–180
Wagenlehner FM, Naber KG (2006) Current challenges in the treatment of complicated urinary tract infections and prostatitis. Clin Microbiol Infect 12(Suppl 3):67–80
Naber KG, Schaeffer AJ, Heyns CF, Matsumoto T, Shoskes DA, Bjerklund Johansen TE (eds) (2010) Urogenital infections. European Association of Urology–International Consultation on Urological Diseases, 1st edn. Arnhem, The Netherlands, ISBN:978-90-79754-41-0
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Heyns, C.F. Urinary tract infection associated with conditions causing urinary tract obstruction and stasis, excluding urolithiasis and neuropathic bladder. World J Urol 30, 77–83 (2012). https://doi.org/10.1007/s00345-011-0725-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-011-0725-9