Abstract
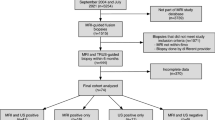
Transrectal ultrasound (TRUS) guided multiple systematic random biopsies are presently the method of choice for determining the presence or absence of prostate cancer. TRUS image information is only used to guide the biopsy needle into the prostate, but not to localize and target cancerous lesions. Our aim in this study was to evaluated the possible predictive value of tumor suspicious endosonographic lesions of the prostate for prostate biopsies. We prospectively compared six systematic biopsies with lesion guided biopsies in a consecutive series of 217 patients. All patients had a prostate specific antigen (PSA) level of >4 ng/ml without a history of prostate disease. In a subgroup of 145 men with sonomorphologic lesions suggestive for prostate cancer (hypoechoic areas or asymmetries predominantly in the peripheral zone), lesion-guided biopsies were taken in addition to the systematic biopsies. We evaluated the number of tumors which were diagnosed or missed by both of the biopsy strategies. Of the 217 evaluated patients, 64 (29%) had histology confirmed cancer. Four patients with negative sextant biopsies had a positive TRUS guided biopsy. Out of 145 patients with a normal TRUS, three were cancer positive by sextant biopsy. A total of 1,387 individual biopsy cores were evaluated. Of the 1,304 systematic biopsy cores, 182 (14%) were positive and 1,122 (86%) negative. Of the 329 TRUS lesion guided biopsy cores 139 (42%) were positive and 190 (58%) negative. Patients with tumor suggestive TRUS lesions have a considerably higher risk of being diagnosed with prostate cancer compared to patients without such lesions. Both systematic sextant and TRUS lesion guided biopsies missed detectable prostate cancer in a minority of patients. Taking the endosonographic morphology of the prostate gland into consideration for biopsy strategies may improve the quality of the biopsy and avoid unnecessary invasive procedures in selected cases.




Similar content being viewed by others
References
Potosky AL, Miller BA, Albertson PC, Kramer BS (1995) The role of increasing detection in the rising incidence of prostate cancer. JAMA 273:548–552
Shinohara K, Scardino PT, Carter SC, Wheeler TM (1989) Pathologic basis of the sonographic appearance of the normal and malignant prostate. Urol Clin Am 16:675–678
Lee F, Gray JM, McLeary RD, Meadows TK, Kumasaka GH, Borlaza GS, Straub WH, Lee FJr, Solomon MH, McHugh TA et al. (1985) Transrectal ultrasound in the diagnosis of prostate cancer: location, echogenicity, histopathology, and staging. Prostate 7:117–129
Ellis WJ, Brawer MK (1994) The significance of isoechoic prostatic carcinoma. J Urol 152:2304–2307
Mettlin C, Murphy GP, Babaian RJ, Chesley A, Kane RA, Littrup PJ, Mostofi FK, Ray PS, Shanberg AM, Toi A (1996) The results of a five-year early prostate cancer detection intervention. Investigators of the American Cancer Society National Prostate Cancer Detection Project. Cancer 77:150–159
Nava L, Montorsi F, Consonni P, Scattoni V, Guazzoni G, Rigatti PJ (1997) Results of a prospective randomized study comparing 6, 12 and 18 transrectal ultrasound guided sextant biopsies in patients with elevated PSA, normal DRE, and normal prostatic ultrasound. Urology 157:59
Vashi AR, Wojno KJ, Gillespie B, Oesterling JE (1997) Patient age and prostate gland size determine the appropriate number of cores per prostate biopsy. J Urol 157:365
Jones JS, Oder M, Zippe CD (2002) Saturation biopsy with periprostatic block can be performed in office. J Urol 168:2108–2110
Fleshner N, Klotz L (2002) Role of “saturation biopsy” in the detection of prostate cancer among difficult diagnostic cases. Urology 60:93–97
Chrouser KL, Lieber MM (2004) Extended and saturation needle biopsy for the diagnosis of prostate cancer. Curr Urol Rep 5:226–230
Loch T, Gettys T, Cochran JS, Fulgham PF, Bertermann H (1990) Computer-aided image-analysis in transrectal ultrasound of the prostate. World J Urol 8:150–153
Holm HH, Gammelgaard J (1981) Ultrasonocally guided precise needle placement in the prostate and the seminal vesicles. J Urol 142:66–70
Lee F, McLeary RD, Meadows TR (1985) Transrectal ultrasound in the diagnosis of prostatic cancer: location, echogenicity, histopathology and staging. Prostate 7:117–129
Loch T, McNeal JE, Stamey TA (1995) Interpretation of bilateral positive biopsies in prostate cancer. J Urol 154:1078–1083
Terris MK, Freiha FS, McNeal JE, Stamey TA (1991) Efficiacy of transrectal ultrasound for identification of clinically undetected prostate cancer. J Urol 146:78
Norberg M, Egevad L,Holmberg L, Sparen P, Norlen B J, Busch C (1997) The sextant protocol for ultrasound-guided core biopsies of the prostate underestimates the presence of cancer. Urology 50:562–566
Hodge KK, McNeal JE, Terris MK, Stamey TA (1989) Random systematic versus directed ultrasound guided transrectal core biopsies of the prostate. J Urol 142:71–75
Bertermann H, Wirth B, Penkert A, Hansmann ML (1989) Ultraschallgezielte transrektale Prostatabiopsie: Bei 1 cm-Läsionen sicher im Ziel. Z Urol Poster 2:110–113
Loch T, Bertermann H, Stöckle M (2000) Technische und anatomische Grundlagen des transrektalen Ultraschalls (TRUS) der Prostata. Urologe B 40:475–483
Ravery V, Billebaud T, Toublanc M, Boccon-Gibod L, Hermieu JF, Moulinier F, Blanc E, Delmas V (1999) Diagnostic value of ten systematic TRUS-guided prostate biopsies. Eur Urol 35: 298–303
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Loch, T., Eppelmann, U., Lehmann, J. et al. Transrectal ultrasound guided biopsy of the prostate: random sextant versus biopsies of sono-morphologically suspicious lesions. World J Urol 22, 357–360 (2004). https://doi.org/10.1007/s00345-004-0462-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-004-0462-4