Abstract
Objectives
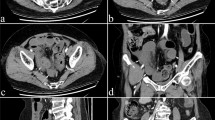
Differences in clinical adverse outcomes (CAO) based on different intestinal stricturing definitions in Crohn’s disease (CD) are poorly documented. This study aims to compare CAO between radiological strictures (RS) and endoscopic strictures (ES) in ileal CD and explore the significance of upstream dilatation in RS.
Methods
This retrospective double-center study included 199 patients (derivation cohort, n = 157; validation cohort, n = 42) with bowel strictures who simultaneously underwent endoscopic and radiologic examinations. RS was defined as a luminal narrowing with wall thickening relative to the normal gut on cross-sectional imaging (group 1 (G1)), which further divided into G1a (without upstream dilatation) and G1b (with upstream dilatation). ES was defined as an endoscopic non-passable stricture (group 2 (G2)). Strictures met the definitions of RS (with or without upstream dilatation) and ES were categorized as group 3 (G3). CAO referred to stricture-related surgery or penetrating disease.
Results
In the derivation cohort, G1b (93.3%) had the highest CAO occurrence rate, followed by G3 (32.6%), G1a (3.2%), and G2 (0%) (p < 0.0001); the same order was found in the validation cohort. The CAO-free survival time was significantly different among the four groups (p < 0.0001). Upstream dilatation (hazard ratio, 1.126) was a risk factor for predicting CAO in RS. Furthermore, when upstream dilatation was added to diagnose RS, 17.6% of high-risk strictures were neglected.
Conclusions
CAO differs significantly between RS and ES, and clinicians should pay more attention to strictures in G1b and G3. Upstream dilatation has an important impact on the clinical outcome of RS but may not be an essential factor for RS diagnosis.
Clinical relevance statement
This study explored the definition of intestinal stricture with the greatest significance for the clinical diagnosis and prognosis of patients with CD, and consequently provided effective auxiliary information for clinicians to formulate strategies for the treatment of CD intestinal strictures.
Key Points
• The retrospective double-center study showed that clinical adverse outcome is different between radiological strictures and endoscopic strictures in CD.
• Upstream dilatation has an important impact on the clinical outcome of radiological strictures but may not be an essential factor for diagnosis of radiological strictures.
• Radiological stricture with upstream dilatation and simultaneous radiological and endoscopic stricture were at increased risk for clinical adverse outcomes; thus, closer monitoring should be considered.





Similar content being viewed by others
Abbreviations
- AUC:
-
Area under the receiver operating characteristic curve
- CAO:
-
Clinical adverse outcome
- CD:
-
Crohn’s disease
- CI:
-
Confidence interval
- CTE:
-
Computed tomography enterography
- ES:
-
Endoscopic stricture
- HR:
-
Hazard ratios
- IDI:
-
Integrated discrimination improvement
- MRE:
-
Magnetic resonance enterography
- RS:
-
Radiological strictures
References
Ng SC, Shi HY, Hamidi N et al (2017) Worldwide incidence and prevalence of inflammatory bowel disease in the 21st century: a systematic review of population-based studies. Lancet 390:2769–2778
Hordonneau C, Buisson A, Scanzi J et al (2014) Diffusion-weighted magnetic resonance imaging in ileocolonic Crohn’s disease: validation of quantitative index of activity. Am J Gastroenterol 109:89–98
Rieder F, Bettenworth D, Ma C et al (2018) An expert consensus to standardise definitions, diagnosis and treatment targets for anti-fibrotic stricture therapies in Crohn’s disease. Aliment Pharmacol Ther 48:347–357
Rieder F, Zimmermann EM, Remzi FH, Sandborn WJ (2013) Crohn’s disease complicated by strictures: a systematic review. Gut 62:1072–1084
Stocker D, King MJ, El Homsi M et al (2021) Luminal narrowing alone allows an accurate diagnosis of Crohn’s disease small bowel strictures at cross-sectional imaging. J Crohns Colitis 15:1009–1018
Pariente B, Mary JY, Danese S et al (2015) Development of the Lemann index to assess digestive tract damage in patients with Crohn’s disease. Gastroenterology 148(52–63):e3
Bruining DH, Zimmermann EM, Loftus EV Jr et al (2018) Consensus recommendations for evaluation, interpretation, and utilization of computed tomography and magnetic resonance enterography in patients with small bowel Crohn’s disease. Radiology 286:776–799
Hill NS, DiSantis DJ (2015) The comb sign. Abdom Imaging 40:1010
Hayashi K, Eguchi S (2019) The power-integrated discriminant improvement: an accurate measure of the incremental predictive value of additional biomarkers. Stat Med 38:2589–2604
Vickers AJ, Elkin EB (2006) Decision curve analysis: a novel method for evaluating prediction models. Med Decis Making 26:565–574
Camp RLD-FM, Rimm DL (2004) X-tile a new bio-informatics tool for biomarker assessment and outcome-based cut-point optimization. Clin Cancer Res 10:7252–7259
Blanche P, Dartigues JF, Jacqmin-Gadda H (2013) Estimating and comparing time-dependent areas under receiver operating characteristic curves for censored event times with competing risks. Stat Med 32:5381–5397
Kamarudin AN, Cox T, Kolamunnage-Dona R (2017) Time-dependent ROC curve analysis in medical research: current methods and applications. BMC Med Res Methodol 17:53
Heagerty PJ, Zheng Y (2005) Survival model predictive accuracy and ROC curves. Biometrics 61:92–105
Krischer JP, Liu X, Vehik K et al (2019) Predicting islet cell autoimmunity and type 1 diabetes: an 8-Year TEDDY study progress report. Diabetes Care 42:1051–1060
Narula N, Wong ECL, Dulai PS, Marshall JK, Colombel JF, Reinisch W (2021) Outcomes of passable and non-passable strictures in clinical trials of Crohn’s disease: a post-hoc analysis. J Crohns Colitis 15:1649–1657
Li XH, Feng ST, Cao QH et al (2021) Degree of creeping fat assessed by CT enterography is associated with intestinal fibrotic stricture in patients with Crohn’s disease: a potentially novel mesenteric creeping fat index. J Crohns Colitis 15:1161–1173
Maaser C, Sturm A, Vavricka SR, et al (2019) European Crohn’s and Colitis Organisation [ECCO] and the European Society of Gastrointestinal and Abdominal Radiology [ESGAR]. ECCO-ESGAR Guideline for diagnostic assessment in IBD Part 1: Initial diagnosis, monitoring of known IBD, detection of complications. J Crohns Colitis.13:144–164
Acknowledgements
The authors would like to thank Zhan-sheng Lv for his assistance with analyzing and processing the data.
Funding
This study has received funding by National Natural Science Foundation of China (82070680, 82072002, 81970483, 82170537, 82270693).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Xue-hua Li.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained (the protocol number was IIT-2021–857).
Methodology
• retrospective
• diagnostic or prognostic study
• multicenter study
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Li Shi, Yang-di Wang, and Xiao-di Shen shared the co-first authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shi, L., Wang, Yd., Shen, Xd. et al. Clinical outcome is distinct between radiological stricture and endoscopic stricture in ileal Crohn’s disease. Eur Radiol 33, 7595–7608 (2023). https://doi.org/10.1007/s00330-023-09743-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-09743-5