Abstract
Objectives
To construct a nomogram with high-frequency shear wave elastography (SWE) as a noninvasive method to accurately assess chronic changes in renal allografts.
Methods
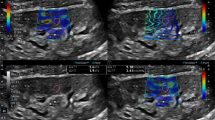
A total of 191 renal transplantation patients (127 cases in the training group and 64 cases in the verification group) were included in this study. All patients received conventional ultrasound and high-frequency SWE examination, followed directly by biopsy the next day. The chronic changes were divided into mild, moderate, and severe. Multivariate logistic analyses were used to select significant variables, which were used to develop the nomogram. Nomogram models were assessed by receiver operating characteristic (ROC) curves, calibration plots, and decision curve analysis (DCA).
Results
The cutoff value of SWE in mild, moderate, and severe chronic changes was 18.9, 22.5, and 27.6 kPa, respectively. The areas under the curve (AUCs) of SWE in the differential diagnosis of mild and moderate to severe chronic changes and mild to moderate and severe chronic changes were 0.817 and 0.870, respectively. Multivariate analysis showed that time since transplantation, proteinuria, glomerular filtration rate, echogenicity, and SWE were independent diagnostic factors for moderate to severe chronic changes (all p < 0.05); thus, a nomogram was successfully developed. The AUCs of the nomogram in the training and validation groups were 0.905 and 0.938, respectively. The high agreement between the model predictions and the actual observations was confirmed by calibration plot and DCA.
Conclusions
Based on SWE, the nomogram provided an insightful and applicable tool to evaluate chronic changes in renal allografts.
Key Points
• In kidney transplantation, compared with acute changes, chronic changes are significantly correlated with cortical stiffness.
• SWE shows good performance in identifying mild to moderate and severe chronic changes, with an AUC of 0.870.
• Time since transplantation, proteinuria, glomerular filtration rate, echogenicity, and SWE are independent diagnostic factors for moderate to severe chronic changes in renal allografts.






Similar content being viewed by others
Abbreviations
- AUC:
-
Area under the curve
- DCA:
-
Decision curve analysis
- GFR:
-
Glomerular filtration rate
- ICC:
-
Intraclass correlation coefficient
- IF:
-
Interstitial fibrosis
- PSV:
-
Peak systolic velocity
- RI:
-
Resistance index
- ROC:
-
Receiver operating characteristic curves
- SWE:
-
Shear wave elastography
- TA:
-
Tubular atrophy
References
Nankivell BJ, Chapman JR (2006) Chronic allograft nephropathy: current concepts and future directions. Transplantation 81:643–654. https://doi.org/10.1097/01.tp.0000190423.82154.01
Sethi S, D'Agati VD, Nast CC et al (2017) A proposal for standardized grading of chronic changes in native kidney biopsy specimens. Kidney Int 91:787–789. https://doi.org/10.1016/j.kint.2017.01.002
Solez K, Axelsen RA, Benediktsson H et al (1993) International standardization of criteria for the histologic diagnosis of renal allograft rejection: the Banff working classification of kidney transplant pathology. Kidney Int 44:411–422. https://doi.org/10.1038/ki.1993.259
Schwarz A, Gwinner W, Hiss M, Radermacher J, Mengel M, Haller H (2005) Safety and adequacy of renal transplant protocol biopsies. Am J Transplant 5:1992–1996. https://doi.org/10.1111/j.1600-6143.2005.00988.x
Randers E, Erlandsen EJ (1999) Serum cystatin C as an endogenous marker of the renal function--a review. Clin Chem Lab Med 37:389–395. https://doi.org/10.1515/CCLM.1999.064
Nankivell BJ, Borrows RJ, Fung CL, O'Connell PJ, Allen RD, Chapman JR (2003) The natural history of chronic allograft nephropathy. New Engl J Med 349:2326–2333. https://doi.org/10.1056/NEJMoa020009
Chapman JR, O'Connell PJ, Nankivell BJ (2005) Chronic renal allograft dysfunction. J Am Soc Nephrol 16:3015–3026. https://doi.org/10.1681/ASN.2005050463
Bamber J, Cosgrove D, Dietrich CF et al (2013) EFSUMB guidelines and recommendations on the clinical use of ultrasound elastography. Part 1: Basic Principles and Technology. Ultraschall Med 34:169–184. https://doi.org/10.1055/s-0033-1335205
Early HM, Cheang EC, Aguilera JM et al (2018) Utility of shear wave elastography for assessing allograft fibrosis in renal transplant recipients: a pilot study. J Ultrasound Med 37:1455–1465. https://doi.org/10.1002/jum.14487
Ma MKM, Law HKW, Tse KS et al (2018) Non-invasive assessment of kidney allograft fibrosis with shear wave elastography: a radiological-pathological correlation analysis. Int J Urol 25:450–455. https://doi.org/10.1111/iju.13536
Bolboaca SD, Elec FI, Elec AD et al (2020) Shear-wave elastography variability analysis and relation with kidney allograft dysfunction: a single-center study. Diagnostics (Basel) 10:41. https://doi.org/10.3390/diagnostics10010041
Roufosse C, Simmonds N, Clahsen-van Groningen M et al (2018) A 2018 reference guide to the Banff classification of renal allograft pathology. Transplantation 102:1795–1814. https://doi.org/10.1097/TP.0000000000002366
Shrout PE, Fleiss JL (1979) Intraclass correlations: uses in assessing rater reliability. Psychol Bull 86:420–428. https://doi.org/10.1037//0033-2909.86.2.420
Arena U, Vizzutti F, Abraldes JG et al (2008) Reliability of transient elastography for the diagnosis of advanced fibrosis in chronic hepatitis C. Gut 57:1288–1293. https://doi.org/10.1136/gut.2008.149708
Castera L, Vergniol J, Foucher J et al (2005) Prospective comparison of transient elastography, Fibrotest, APRI, and liver biopsy for the assessment of fibrosis in chronic hepatitis C. Gastroenterology 128:343–350. https://doi.org/10.1053/j.gastro.2004.11.018
Lukenda V, Mikolasevic I, Racki S, Jelic I, Stimac D, Orlic L (2014) Transient elastography: a new noninvasive diagnostic tool for assessment of chronic allograft nephropathy. Int Urol Nephrol 46:1435–1440. https://doi.org/10.1007/s11255-014-0697-y
Nakao T, Ushigome H, Nakamura T et al (2015) Evaluation of renal allograft fibrosis by transient elastography (Fibro Scan). Transpl P 47:640–643. https://doi.org/10.1016/j.transproceed.2014.12.034
Sommerer C, Scharf M, Seitz C et al (2013) Assessment of renal allograft fibrosis by transient elastography. Transpl Int 26:545–551. https://doi.org/10.1111/tri.12073
Syversveen T, Midtvedt K, Berstad AE, Brabrand K, Strom EH, Abildgaard A (2012) Tissue elasticity estimated by acoustic radiation force impulse quantification depends on the applied transducer force: an experimental study in kidney transplant patients. Eur Radiol 22:2130–2137. https://doi.org/10.1007/s00330-012-2476-4
Grenier N, Poulain S, Lepreux S et al (2012) Quantitative elastography of renal transplants using supersonic shear imaging: a pilot study. Eur Radiol 22:2138–2146. https://doi.org/10.1007/s00330-012-2471-9
Asano K, Ogata A, Tanaka K et al (2014) Acoustic radiation force impulse elastography of the kidneys is shear wave velocity affected by tissue fibrosis or renal blood flow? J Ultrasound Med 33:793–801. https://doi.org/10.7863/ultra.33.5.793
Platt JF, Rubin JM, Bowerman RA et al (1988) The inability to detect kidney disease on the basis of echogenicity. AJR Am J Roentgenol 151:317–319. https://doi.org/10.2214/ajr.151.2.317
Yoo MG, Jung DC, Oh YT, Park SY, Han K (2017) Usefulness of multiparametric ultrasound for evaluating structural abnormality of transplanted kidney: can we predict histologic abnormality on renal biopsy in advance? AJR Am J Roentgenol 209:W139–W144. https://doi.org/10.2214/AJR.16.17397
El-Zoghby ZM, Stegall MD, Lager DJ et al (2009) Identifying specific causes of kidney allograft loss. Am J Transplant 9:527–535. https://doi.org/10.1111/j.1600-6143.2008.02519.x
Halimi JM, Buchler M, Al-Najjar A et al (2007) Urinary albumin excretion and the risk of graft loss and death in proteinuric and non-proteinuric renal transplant recipients. Am J Transplant 7:618–625. https://doi.org/10.1111/j.1600-6143.2007.01665.x
Ma YC, Zuo L, Chen JH et al (2006) Modified glomerular filtration rate estimating equation for Chinese patients with chronic kidney disease. J Am Soc Nephrol 17:2937–2944. https://doi.org/10.1681/ASN.2006040368
Funding
This work was supported by Guangdong Basic and Applied Basic Research Foundation (2020A1515010653), National Natural Science Foundation of China (No. 82102047), and the Major Research Plan of the National Natural Science Foundation of China (92059201).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Xiao-hua Xie.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors (Ming Xu) has significant statistical expertise.
Informed consent
Written informed consent was approved by the Institutional Review Board.
Ethical approval
The study was approved by the ethics committees of The First Affiliated Hospital of Sun Yat-Sen University.
Methodology
• Prospective
• Diagnostic or prognostic study
• Performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(PDF 532 kb)
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, D., Wang, Y., Zhuang, B. et al. Nomogram based on high-frequency shear wave elastography (SWE) to evaluate chronic changes after kidney transplantation. Eur Radiol 33, 763–773 (2023). https://doi.org/10.1007/s00330-022-09054-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-09054-1