Abstract
Purpose
To determine the utility of cervical spine MRI in blunt trauma evaluation for instability after a negative non-contrast cervical spine CT.
Methods
A review of medical records identified all adult patients with blunt trauma who underwent CT cervical spine followed by MRI within 48 h over a 33-month period. Utility of subsequent MRI was assessed in terms of findings and impact on outcome.
Results
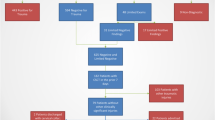
A total of 1,271 patients with blunt cervical spine trauma underwent both cervical spine CT and MRI within 48 h; 1,080 patients were included in the study analysis. Sixty-six percent of patients with a CT cervical spine study had a negative study. Of these, the subsequent cervical spine MRI had positive findings in 20.9%; 92.6% had stable ligamentous or osseous injuries, 6.0% had unstable injuries and 1.3% had potentially unstable injuries. For unstable injury, the NPV for CT was 98.5%. In all 712 patients undergoing both CT and MRI, only 1.5% had unstable injuries, and only 0.42% had significant change in management.
Conclusions
MRI for blunt trauma evaluation remains not infrequent at our institution. MRI may have utility only in certain patients with persistent abnormal neurological examination.
Key Points
• MRI has limited utility after negative cervical CT in blunt trauma.
• MRI is frequently positive for non-specific soft-tissue injury.
• Unstable injury missed on CT is infrequent.

Similar content being viewed by others
Abbreviations
- ALL:
-
Anterior Longitudinal Ligament
- CSI:
-
Cervical spine injury
- CT:
-
Computed tomography
- ED:
-
Emergency department
- GCS:
-
Glasgow Coma Scale
- IRB:
-
Institutional Review Board
- MRI:
-
Magnetic resonance imaging
- MVA:
-
Motor vehicle accident
- NEXUS:
-
National Emergency XRadiography Utilization Study
- NPV:
-
Negative predictive value
- PLC:
-
Posterior ligamentous complex
- PLL:
-
Posterior longitudnal ligament
References
Young AJ, Wolfe L, Tinkoff G, Duane TM (2015) Assessing incidence and risk factors of cervical spine injury in blunt trauma patients using the National Trauma Data Bank. Am Surg 81:879–883
Badhiwala JH, Lai CK, Alhazzani W et al (2015) Cervical spine clearance in obtunded patients after blunt traumatic injury: a systematic review. Ann Intern Med 162:429–437
Harris MB, Kronlage SC, Carboni PA et al (2000) Evaluation of the cervical spine in the polytrauma patient. Spine (Phila Pa 1976) 25:2884–2891 discussion 2892
Levi AD, Hurlbert RJ, Anderson P et al (2006) Neurologic deterioration secondary to unrecognized spinal instability following trauma--a multicenter study. Spine (Phila Pa 1976) 31:451–458
Reid DC, Henderson R, Saboe L, Miller JD (1987) Etiology and clinical course of missed spine fractures. J Trauma 27:980–986
Poonnoose PM, Ravichandran G, McClelland MR (2002) Missed and mismanaged injuries of the spinal cord. J Trauma 53:314–320
Hoffman JR, Mower WR, Wolfson AB, Todd KH, Zucker MI (2000) Validity of a set of clinical criteria to rule out injury to the cervical spine in patients with blunt trauma. National Emergency X-Radiography Utilization Study Group. N Engl J Med 343:94–99
Stiell IG, Wells GA, Vandemheen KL et al (2001) The Canadian C-spine rule for radiography in alert and stable trauma patients. Jama 286:1841–1848
Holmes JF, Akkinepalli R (2005) Computed tomography versus plain radiography to screen for cervical spine injury: a meta-analysis. J Trauma 58:902–905
Hennessy D, Widder S, Zygun D, Hurlbert RJ, Burrowes P, Kortbeek JB (2010) Cervical spine clearance in obtunded blunt trauma patients: a prospective study. J Trauma 68:576–582
Malhotra A, Wu X, Kalra VB et al (2017) Utility of MRI for cervical spine clearance after blunt traumatic injury: a meta-analysis. Eur Radiol 27:1148–1160
Muchow RD, Resnick DK, Abdel MP, Munoz A, Anderson PA (2008) Magnetic resonance imaging (MRI) in the clearance of the cervical spine in blunt trauma: a meta-analysis. J Trauma 64:179–189
Stelfox HT, Velmahos GC, Gettings E, Bigatello LM, Schmidt U (2007) Computed tomography for early and safe discontinuation of cervical spine immobilization in obtunded multiply injured patients. J Trauma 63:630–636
Tomycz ND, Chew BG, Chang YF et al (2008) MRI is unnecessary to clear the cervical spine in obtunded/comatose trauma patients: the four-year experience of a level I trauma center. J Trauma 64:1258–1263
Sanchez B, Waxman K, Jones T, Conner S, Chung R, Becerra S (2005) Cervical spine clearance in blunt trauma: evaluation of a computed tomography-based protocol. J Trauma 59:179–183
Harris TJ, Blackmore CC, Mirza SK, Jurkovich GJ (2008) Clearing the cervical spine in obtunded patients. Spine (Phila Pa 1976) 33:1547–1553
Gargas J, Yaszay B, Kruk P, Bastrom T, Shellington D, Khanna S (2013) An analysis of cervical spine magnetic resonance imaging findings after normal computed tomographic imaging findings in pediatric trauma patients: ten-year experience of a level I pediatric trauma center. J Trauma Acute Care Surg 74:1102–1107
Vanguri P, Young AJ, Weber WF et al (2014) Computed tomographic scan: it's not just about the fracture. J Trauma Acute Care Surg 77:604–607
Diaz JJ Jr, Aulino JM, Collier B et al (2005) The early work-up for isolated ligamentous injury of the cervical spine: does computed tomography scan have a role? J Trauma 59:897–903 discussion 903-894
Kaiser ML, Whealon MD, Barrios C, Kong AP, Lekawa ME, Dolich MO (2012) The current role of magnetic resonance imaging for diagnosing cervical spine injury in blunt trauma patients with negative computed tomography scan. Am Surg 78:1156–1160
Benzel EC, Hart BL, Ball PA, Baldwin NG, Orrison WW, Espinosa MC (1996) Magnetic resonance imaging for the evaluation of patients with occult cervical spine injury. J Neurosurg 85:824–829
Patel MB, Humble SS, Cullinane DC et al (2015) Cervical spine collar clearance in the obtunded adult blunt trauma patient: a systematic review and practice management guideline from the Eastern Association for the Surgery of Trauma. J Trauma Acute Care Surg 78:430–441
Denis F (1983) The three column spine and its significance in the classification of acute thoracolumbar spinal injuries. Spine (Phila Pa 1976) 8:817–831
Cybulski GR, Douglas RA, Meyer PR Jr, Rovin RA (1992) Complications in three-column cervical spine injuries requiring anterior-posterior stabilization. Spine (Phila Pa 1976) 17:253–256
Morrison J, Jeanmonod R (2014) Imaging in the NEXUS-negative patient: when we break the rule. Am J Emerg Med 32:67–70
Ackland HM, Cameron PA, Varma DK et al (2011) Cervical spine magnetic resonance imaging in alert, neurologically intact trauma patients with persistent midline tenderness and negative computed tomography results. Ann Emerg Med 58:521–530
Inaba K, Byerly S, Bush LD et al (2016) Cervical spinal clearance: a prospective Western Trauma Association Multi-institutional Trial. J Trauma Acute Care Surg 81:1122–1130
James IAO, Moukalled A, Yu E et al (2014) A systematic review of the need for MRI for the clearance of cervical spine injury in obtunded blunt trauma patients after normal cervical spine CT. J Emerg Trauma Shock 7:251–255
Russin JJ, Attenello FJ, Amar AP, Liu CY, Apuzzo ML, Hsieh PC (2013) Computed tomography for clearance of cervical spine injury in the unevaluable patient. World Neurosurg 80:405–413
Schoenfeld AJ, Bono CM, McGuire KJ, Warholic N, Harris MB (2010) Computed tomography alone versus computed tomography and magnetic resonance imaging in the identification of occult injuries to the cervical spine: a meta-analysis. J Trauma 68:109–113 discussion 113-104
Panczykowski DM, Tomycz ND, Okonkwo DO (2011) Comparative effectiveness of using computed tomography alone to exclude cervical spine injuries in obtunded or intubated patients: meta-analysis of 14,327 patients with blunt trauma. J Neurosurg 115:541–549
Raza M, Elkhodair S, Zaheer A, Yousaf S (2013) Safe cervical spine clearance in adult obtunded blunt trauma patients on the basis of a normal multidetector CT scan--a meta-analysis and cohort study. Injury 44:1589–1595
Malhotra A, Wu X, Kalra VB, Schindler J, Matouk CC, Forman HP (2016) Evaluation for blunt cerebrovascular injury: review of the literature and a cost-effectiveness analysis. AJNR Am J Neuroradiol 37:330–335
Hogan GJ, Mirvis SE, Shanmuganathan K, Scalea TM (2005) Exclusion of unstable cervical spine injury in obtunded patients with blunt trauma: is MR imaging needed when multi-detector row CT findings are normal? Radiology 237:106–113
Wu X, Malhotra A, Geng B et al (2017) Cost-effectiveness of magnetic resonance imaging in cervical spine clearance of neurologically intact patients with blunt trauma. Ann Emerg Med. https://doi.org/10.1016/j.annemergmed.2017.07.006
Fisher BM, Cowles S, Matulich JR, Evanson BG, Vega D, Dissanaike S (2013) Is magnetic resonance imaging in addition to a computed tomographic scan necessary to identify clinically significant cervical spine injuries in obtunded blunt trauma patients? Am J Surg 206:987–993 discussion 993-984
Sarani B, Waring S, Sonnad S, Schwab CW (2007) Magnetic resonance imaging is a useful adjunct in the evaluation of the cervical spine of injured patients. J Trauma 63:637–640
Schoenfeld AJ, Tobert DG, Le HV et al (2017) The utility of adding magnetic resonance imaging to computed tomography alone in the evaluation of cervical spine injury: a propensity matched analysis. Spine (Phila Pa 1976). https://doi.org/10.1097/brs.0000000000002285
Resnick S, Inaba K, Karamanos E et al (2014) Clinical relevance of magnetic resonance imaging in cervical spine clearance: a prospective study. JAMA Surg 149:934–939
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Ajay Malhotra.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Ethical approval
Institutional Review Board of Yale University approval was obtained for this study.
Informed consent
Written informed consent was waived by Institutional Review Board.
Methodology
• retrospective
• case-control study
• performed at one institution
Electronic supplementary material
ESM 1
(DOCX 40 kb)
Rights and permissions
About this article
Cite this article
Malhotra, A., Durand, D., Wu, X. et al. Utility of MRI for cervical spine clearance in blunt trauma patients after a negative CT . Eur Radiol 28, 2823–2829 (2018). https://doi.org/10.1007/s00330-017-5285-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-017-5285-y