Abstract
Purpose
To test the hypothesis that “acute-period” lumbar MRI in non-elderly patients with low back pain is less frequently performed at clinics/hospitals with greater involvement of full-time radiologists in the imaging workflow.
Methods
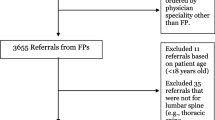
In a national-level claims database, we identified 14,819 non-elderly patients (mean age: 38.7±8.0 years) who visited clinics/hospitals for low back pain in 2013–2015. We classified the clinics/hospitals into four groups based on the level of full-time radiologist involvement and MRI ownership, and compared the frequency of acute-period lumbar MRI using hierarchical logistic regression analysis.
Results
Patients visiting facilities without a full-time radiologist (n=2105) were significantly (p<0.001) more likely to undergo acute-period MRI than those visiting facilities with ≥1 radiologist partially managing imaging workflow (level-1, n=491) or ≥1 radiologist intensively involved in imaging workflow (level-2, n=1190) (15.7% vs. 6.9% and 7.3%; adjusted odds ratio of no-radiologist versus level-2: 2.93, p=0.018). No difference was observed between level-1 and level-2 involvement.
Conclusions
Facilities with no full-time radiologist were more likely to perform acute-period MRI to assess for low back pain, while no difference was seen between facilities with varying levels of radiologist involvement in the imaging workflow. Radiologist involvement may contribute to optimal utilisation of medical imaging.
Key Points
• Lumbar MRI was more frequently performed at facilities without full-time radiologists.
• Full-time radiologists may play an important role in appropriate utilisation of imaging.
• Frequency of MRI was similar between moderate and intensive radiologist involvement.


Similar content being viewed by others
Abbreviations
- MRI:
-
Magnetic resonance imaging
- CT:
-
Computed tomography
- ICD:
-
International Classification of Diseases
References
Ikegami N, Yoo BK, Hashimoto H et al (2011) Japanese universal health coverage: Evolution, achievements, and challenges. Lancet 378:1106–1115
Reich MR, Ikegami N, Shibuya K, Takemi K (2011) 50 years of pursuing a healthy society in Japan. Lancet 378:1051–1053
Yamashita Y, Murayama S, Okada M et al (2016) The essence of the Japan Radiological Society/Japanese College of Radiology Imaging Guideline. Jpn J Radiol 34:43–79
Rao VM, Levin DC (2012) The overuse of diagnostic imaging and the choosing wisely initiative. Ann Intern Med 157:574–576
Kumamaru KK, Kumamaru H, Bateman BT et al (2016) Limited Hospital Variation in the Use and Yield of CT for Pulmonary Embolism in Patients Undergoing Total Hip or Total Knee Replacement Surgery. Radiology 281:152765. https://doi.org/10.1148/radiol.2016152765
Japanese National Database Open data. http://www.mhlw.go.jp/stf/seisakunitsuite/bunya/0000139390.html. Accessed 4 Apr 2017
Shmagel A, Foley R, Ibrahim H (2016) Epidemiology of chronic low back pain in US adults: National Health and Nutrition Examination Survey 2009-2010. Arthritis Care Res (Hoboken) 11:n/a–n/a. doi: https://doi.org/10.1002/acr.22890
Manchikanti L, Singh V, Falco FJE et al (2014) Epidemiology of low back pain in Adults. Neuromodulation 17:3–10
Frank A (1993) Low back pain. BMJ 306:901–909
Andersson GB (1999) Epidemiological features of chronic low-back pain. Lancet 354:581–585
Martin BI, Deyo RA, Mirza SK et al (2008) Expenditures and Health Status Among Adults With Back and Neck Problems. JAMA 299:656
Patel ND, Broderick DF, Burns J, et al (2016) ACR Appropriateness criteria low back pain. J Am Coll Radiol 13(9):1069-78
Chou R, Qaseem A, Owens DK et al (2011) Clinical Guideline Diagnostic Imaging for Low Back Pain : Advice for High-Value Health Care From the American College of Physicians. Ann Intern Med 154:181–190
MinaCare Co. Ltd. http://www.minacare.co.jp/. Accessed 7 Apr 2017
Shima D, Ii Y, Yamamoto Y et al (2014) A retrospective, cross-sectional study of real-world values of cardiovascular risk factors using a healthcare database in Japan. BMC Cardiovasc Disord 14:120
Kumamaru K, SanoY, Ri K, Suzuki M, Hori M, Kamagata K, Irie R, Nakanishi A, Aoki S (2016) Association between Repeat MR Imaging for Benign Lumbar/Cervical Conditions and Imaging Management Fee: An Analysis of Japanese Health Insurance Claims Database. Radiol. Soc. North Am. 2016 Sci. Assem. Annu. Meet. http://archive.rsna.org/2016/16003854.html
Ministry of Health L and W Iryo-shisetsu Chosa 2011. http://www.mhlw.go.jp/toukei/saikin/hw/iryosd/11/dl/gaikyo.pdf
Imaging for Low Back Pain -- Clinical Recommendation. http://www.aafp.org/patient-care/clinical-recommendations/all/cw-back-pain.html. Accessed 21 Mar 2017
Chou R, Qaseem A, Owens DK, Shekelle P (2011) Diagnostic imaging for low back pain: Advice for high-value health care from the American college of physicians. Ann Intern Med 154:181–189
Chou R, Fu R, Carrino JA, Deyo RA (2009) Imaging strategies for low-back pain: systematic review and meta-analysis. Lancet 373:463–472
Pengel LHM, Herbert RD, Maher CG, Refshauge KM (2003) Acute low back pain: systematic review of its prognosis. BMJ 327:323. https://doi.org/10.1136/bmj.327.7410.323
Jensen MC, Brant-Zawadzki MN, Obuchowski N et al (1994) Magnetic resonance imaging of the lumbar spine in people without back pain. N Engl J Med 331:69–73
Modic MT, Obuchowski NA, Ross JS et al (2005) Acute low back pain and radiculopathy: MR imaging findings and their prognostic role and effect on outcome. Radiology 237:597–604
Jarvik JG, Hollingworth W, Martin B et al (2003) Rapid magnetic resonance imaging vs radiographs for patients with low back pain: a randomized controlled trial. JAMA 289:2810–2818
Webster BS, Cifuentes M (2010) Relationship of early magnetic resonance imaging for work-related acute low back pain with disability and medical utilization outcomes. J Occup Environ Med 52:900–907
McCullough BJ, Johnson GR, Martin BI, Jarvik JG (2012) Lumbar MR imaging and reporting epidemiology: Do epidemiologic data in reports affect clinical management? Radiology 262:941–946
Wool HS, Barrett D (2015) AVOIDING SELF-REFERRAL: UNDERSTANDING THE STARK LAWS. Med Econ 92:40–41
Kouri BE, Gregory Parsons R, Alpert HR (2002) Physician self-referral for diagnostic imaging: Review of the empiric literature. Am J Roentgenol 179:843–850
Paxton BE, Lungren MP, Srinivasan RC et al (2012) Physician self-referral of lumbar spine MRI with comparative analysis of negative study rates as a marker of utilization appropriateness. Am J Roentgenol 198:1375–1379
Hendee WR, Becker GJ, Borgstede JP et al (2010) Addressing Overutilization in Medical Imaging. Radiology 257:240–245
Porter ME (2009) A Strategy for Health Care Reform — Toward a Value-Based System. N Engl J Med 361:109–112
Kumamaru KK, Kogure Y, Suzuki M et al (2016) A strategy to optimize radiation exposure for non-contrast head CT: comparison with the Japanese diagnostic reference levels. Jpn J Radiol 34:451–457
Kumamaru KK, Hunsaker AR, Kumamaru H et al (2013) Correlation between early direct communication of positive CT pulmonary angiography findings and improved clinical outcomes. Chest 144:1546–1554
Ip IK, Gershanik EF, Schneider LI et al (2014) Impact of IT-enabled intervention on MRI use for back pain. Am J Med 127:512–518
Allen B, Prabhakar Reddy K, Miller W et al (2017) Summary of the proceedings of the international forum 2016: “Imaging referral guidelines and clinical decision support - how can radiologists implement imaging referral guidelines in clinical routine?”. Insights Imaging. https://doi.org/10.1007/s13244-016-0523-4
US Department of Health and Human Services, Centers for Medicare & Medicaid Services (2017) Medicare Program; Revisions to Payment Policies Under the Physician Fee Schedule and Other Revisions to Part B for CY 2018; Medicare Shared Savings Program Requirements; and Medicare Diabetes Prevention Program. https://www.federalregister.gov/documents/2017/03/22/2017-05675/medicare-program-revisions-to-payment-policies-under-the-physician-fee-schedule-and-other-revisions
Acknowledgements
We, Japan Safe Radiology, presented our recent activity in the ESR EuroSafe
Imaging Poster Exhibition at ECR 2017.
Funding
This study has received funding by JSPS KAKENHI Grant-in-Aid for Young Scientists (B) Grant Number JP16K19176.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Kanako K. Kumamaru, MD, PhD.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors (Hiraku Kumamaru, MD, ScD) has significant statistical expertise.
Informed consent
Written informed consent was not required for this study because the analyses used an unlinkable, anonymous administrative database.
Ethical approval
This study was exempt from institutional review board approval at the institution where the analyses were performed because the analyses used an unlinkable, anonymous administrative database.
Study subject or cohort overlap
Study subjects and cohorts have not been reported previously.
Methodology
• Retrospective. observational cohort study using nationwide administrative database
• Analyses were performed at one institution
Electronic supplementary material
ESM 1
(DOCX 93 kb)
Rights and permissions
About this article
Cite this article
Kumamaru, K.K., Sano, Y., Kumamaru, H. et al. Radiologist involvement is associated with reduced use of MRI in the acute period of low back pain in a non-elderly population. Eur Radiol 28, 1600–1608 (2018). https://doi.org/10.1007/s00330-017-5086-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-017-5086-3