Abstract
Objective
To determine the diagnostic performance of volumetric quantitative dynamic contrast-enhanced MRI (qDCE-MRI) in differentiation between malignant and benign breast lesions.
Methods
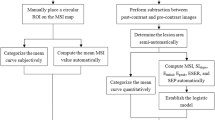
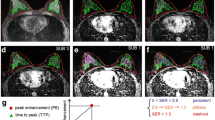
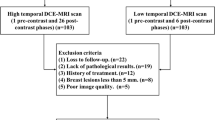
DCE-MRI was performed in 124 patients with 136 breast lesions. Quantitative pharmacokinetic parameters Ktrans, Kep, Ve, Vp and semi-quantitative parameters TTP, MaxCon, MaxSlope, AUC were obtained by using a two-compartment extended Tofts model and three-dimensional volume of interest. Morphologic features (lesion size, margin, internal enhancement pattern) and time-signal intensity curve (TIC) type were also assessed. Logistic regression analysis was used to determine predictors of malignancy, followed by receiver operating characteristics (ROC) analysis to evaluate the diagnostic performance.
Results
qDCE parameters (Ktrans, Kep, Vp, TTP, MaxCon, MaxSlope and AUC), morphological parameters and TIC type were significantly different between malignant and benign lesions (P≤0.001). Multivariate logistic regression analyses showed that Ktrans, Kep, MaxSlope, size, margin and TIC type were independent predictors of malignancy. The diagnostic accuracy of logistic models based on qDCE parameters alone, morphological features plus TIC type, and all parameters combined was 94.9%, 89.0%, and 95.6% respectively.
Conclusion
qDCE-MRI can be used to improve diagnostic differentiation between benign and malignant breast lesions in relation to morphology and kinetic analysis.
Key Points
• qDCE-MRI parameters are useful for discriminating between malignant and benign breast lesions.
• K trans , K ep and MaxSlope were independent predictors of breast malignancy.
• qDCE-MRI has a better diagnostic ability than morphology and kinetic analysis.
• qDCE-MRI can be used to improve the diagnostic accuracy of breast malignancy.



Similar content being viewed by others
Abbreviations
- qDCE-MRI:
-
quantitative dynamic contrast-enhanced magnetic resonance imaging
- Ktrans :
-
volume transfer constant
- Kep :
-
reverse reflux rate constant
- EES:
-
extravascular extracellular space
- Ve :
-
volume fraction of EES
- Vp :
-
volume fraction of plasma
- TTP:
-
time to peak
- MaxCon:
-
maximum concentration
- MaxSlope:
-
maximum slope
- AUC:
-
area under curve
- ROC:
-
receiver operating characteristic
- AUROC:
-
area under receiver operating characteristic curve
- PPV:
-
positive predictive value
- NPV:
-
negative predictive value
- TIC:
-
time-signal intensity curve
- 3D-VOI:
-
three-dimensional volume of interest
- T1W-VIBE:
-
T1-weighted volume interpolated body examination
- ROI:
-
region of interest
- ICC:
-
intra-class correlation coefficient
- OR:
-
odds ratio
- CI:
-
confidence interval
References
Lin Y, Wang C, Zhong Y et al (2013) Striking life events associated with primary breast cancer susceptibility in women: a meta-analysis study. J Exp Clin Cancer Res 32:53
Morrow M, Waters J, Morris E (2011) MRI for breast cancer screening, diagnosis, and treatment. Lancet 378:1804–1811
Kul S, Cansu A, Alhan E, Dinc H, Gunes G, Reis A (2011) Contribution of diffusion-weighted imaging to dynamic contrast-enhanced MRI in the characterization of breast tumors. AJR Am J Roentgenol 196:210–217
Pereira FP, Martins G, Figueiredo E et al (2009) Assessment of breast lesions with diffusion-weighted MRI: comparing the use of different b values. AJR Am J Roentgenol 193:1030–1035
Bedrosian I, Mick R, Orel SG et al (2003) Changes in the surgical management of patients with breast carcinoma based on preoperative magnetic resonance imaging. Cancer 98:468–473
Yin J, Yang J, Han L, Guo Q, Zhang W (2015) Quantitative discrimination between invasive ductal carcinomas and benign lesions based on semi-automatic analysis of time intensity curves from breast dynamic contrast enhanced MRI. J Exp Clin Cancer Res 34:24
Kuhl CK, Mielcareck P, Klaschik S et al (1999) Dynamic breast MR imaging: are signal intensity time course data useful for differential diagnosis of enhancing lesions? Radiology 211:101–110
Ikeda DM, Hylton NM, Kinkel K et al (1999) Development, standardization, and testing of a lexicon for reporting contrast-enhanced breast magnetic resonance imaging studies. J Magn Reson Imaging 13:889–895
Heller SL, Moy L, Lavianlivi S et al (2013) Differentiation of malignant and benign breast lesions using magnetization transfer imaging and dynamic contrast-enhanced MRI. J Magn Reson Imaging 37:138–145
Bisdas S, Seitz O, Middendorp M et al (2010) An exploratory pilot study into the association between microcirculatory parameters derived by MRI-based pharmacokinetic analysis and glucose utilization estimated by PET-CT imaging in head and neck cancer. Eur Radiol 20:2358–2366
Thomas AA, Arevalo-Perez J, Kaley T et al (2015) Dynamic contrast enhanced T1 MRI perfusion differentiates pseudoprogression from recurrent glioblastoma. J Neuro-Oncol 125:183–190
Lee FK, King AD, Ma BB, Yeung DK et al (2012) Dynamic contrast enhancement magnetic resonance imaging (DCE-MRI) for differential diagnosis in head and neck cancers. Eur J Radiol 81:784–788
Kamrava M, Sepahdari AR, Leu K et al (2015) Quantitative multiparametric MRI in uveal melanoma: increased tumor permeability may predict monosomy 3. Neuroradiology 57:833–840
Buadu LD, Murakami J, Murayama S et al (1996) Breast lesions: correlation of contrast medium enhancement patterns on MR images with histopathologic findings and tumor angiogenesis. Radiology 200:639–649
Flickinger FW, Allison JD, Sherry RM, Wright JC (1993) Differentiation of benign from malignant breast masses by time-intensity evaluation of contrast enhanced MRI. Magn Reson Imaging 11:617–620
Jansen SA, Fan X, Karczmar GS, Abe H, Schmidt RA, Newstead GM (2008) Differentiation between benign and malignant breast lesions detected by bilateral dynamic contrast-enhanced MRI: a sensitivity and specificity study. Magn Reson Med 59:747–754
Barnes SL, Whisenant JG, Xia L, Yankeelov TE (2014) Techniques and applications of dynamic contrast enhanced magnetic resonance imaging in cancer. Conf Proc IEEE Eng Med Biol Soc 2014:4264–4267
Li L, Wang K, Sun X et al (2015) Parameters of dynamic contrast-enhanced MRI as imaging markers for angiogenesis and proliferation in human breast cancer. Med Sci Monit 21:376–382
El Khouli RH, Macura KJ, Kamel IR, Jacobs MA, Bluemke DA (2011) 3-T dynamic contrast-enhanced MRI of the breast: pharmacokinetic parameters versus conventional kinetic curve analysis. AJR Am J Roentgenol 197:1498–1505
Fusco R, Sansone M, Filice S et al (2015) Integration of DCE-MRI and DW-MRI Quantitative Parameters for Breast Lesion Classification. Biomed Res Int. https://doi.org/10.1155/2015/237863
Fram EK, Herfkens RJ, Johnson GA et al (1987) Rapid calculation of T1 using variable flip angle gradient refocused imaging. Magn Reson Imaging 5:201–208
Tofts PS, Brix G, Buckley DL et al (1999) Estimating kinetic parameters from dynamic contrast-enhanced T(1)-weighted MRI of a diffusable tracer: standardized quantities and symbols. J Magn Reson Imaging 10:223–232
Tofts PS (1997) Modeling tracer kinetics in dynamic Gd-DTPA MR imaging. J Magn Reson Imaging 7:91–101
Tofts PS, Berkowitz B, Schnall MD (1995) Quantitative analysis of dynamic Gd-DTPA enhancement in breast tumors using a permeability model. Magn Reson Med 33:564–568
Chang YC, Huang YH, Huang CS, Chang PK, Chen JH, Chang RF (2012) Classification of breast mass lesions using model-based analysis of the characteristic kinetic curve derived from fuzzy c-means clustering. Magn Reson Imaging 30:312–322
Kim JH, Ko ES, Lim Y et al (2017) Breast Cancer Heterogeneity: MR Imaging Texture Analysis and Survival Outcomes. Radiology 282:665–675
Noworolski SM, Fischbein NJ, Kaplan MJ et al (2003) Challenges in dynamic contrast-enhanced MRI imaging of cervical lymph nodes to detect metastatic disease. J Magn Reson Imaging 17:455–462
Khalifa F, Soliman A, El-Baz A et al (2014) Models and methods for analyzing DCE-MRI: a review. Med Phys 41:124301
Di Giovanni P, Azlan CA, Ahearn TS, Semple SI, Gilbert FJ, Redpath TW (2010) The accuracy of pharmacokinetic parameter measurement in DCE-MRI of the breast at 3 T. Phys Med Biol 55:121–132
Oshida K, Nagashima T, Ueda T et al (2005) Pharmacokinetic analysis of ductal carcinoma in situ of the breast using dynamic MR mammography. Eur Radiol 15:1353–1360
Kim JY, Kim SH, Kim YJ et al (2015) Enhancement parameters on dynamic contrast enhanced breast MRI: do they correlate with prognostic factors and subtypes of breast cancers? Magn Reson Imaging 33:72–80
Van Dijke CF, Brasch RC, Roberts TP et al (1996) Mammary carcinoma model: correlation of macromolecular contrast-enhanced MR imaging characterizations of tumor microvasculature and histologic capillary density. Radiology 198:813–818
Turetschek K, Roberts TP, Floyd E et al (2001) Tumor microvascular characterization using ultrasmall superparamagnetic iron oxide particles (USPIO) in an experimental breast cancer model. J Magn Reson Imaging 13:882–888
Barnes SL, Quarles CC, Yankeelov TE (2014) Modeling the effect of intra-voxel diffusion of contrast agent on the quantitative analysis of dynamic contrast enhanced magnetic resonance imaging. PLoS One 9:e108726
Mills SJ, Soh C, Rose CJ et al (2010) Candidate biomarkers of extravascular extracellular space: a direct comparison of apparent diffusion coefficient and dynamic contrast-enhanced MR imaging--derived measurement of the volume of the extravascular extracellular space in glioblastoma multiforme. AJNR Am J Neuroradiol 31:549–553
Yuan J, Chow SK, Yeung DK, Ahuja AT, King AD (2010) Quantitative evaluation of dual-flip-angle T1 mapping on DCE-MRI kinetic parameter estimation in head and neck. Quant Imaging Med Surg 2:245–253
Schabel MC, Fluckiger JU, DiBella EV (2010) A model-constrained Monte Carlo method for blind arterial input function estimation in dynamic contrast-enhanced MRI: I. Simulations. Phys Med Biol 55:4783–4806
Henderson E, Rutt BK, Lee TY (1998) Temporal sampling requirements for the tracer kinetics modeling of breast disease. Magn Reson Imaging 16:1057–1073
An YS, Kang DK, Jung YS, Han S, Kim TH (1998) Tumor metabolism and perfusion ratio assessed by 18F-FDG PET/CT and DCE-MRI in breast cancer patients: Correlation with tumor subtype and histologic prognostic factors. Eur J Radiol 84:1365–1370
Koo HR, Cho N, Song IC et al (2012) Correlation of perfusion parameters on dynamic contrast-enhanced MRI with prognostic factors and subtypes of breast cancers. J Magn Reson Imaging 36:145–151
Yi B, Kang DK, Yoon D et al (2014) Is there any correlation between model-based perfusion parameters and model-free parameters of time-signal intensity curve on dynamic contrast enhanced MRI in breast cancer patients? Eur Radiol 24:1089–1096
Funding
This study has received funding from the Project Supported by Guangdong Province Universities and Colleges Pearl River Scholar Funded Scheme (2017), the Scientific Research Foundation for the Returned Overseas Chinese Scholars, State Education Ministry (Zhuo Wu), the National Natural Science Foundation of China (Grant No.81671653), the Medical Scientific Research Foundation of Guangdong Province, China (Grant No. A2013204), and the PhD Start-up Fund of the Natural Science Foundation of Guangdong Province, China (Grant No. S2013040015660).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Jun Shen.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional Review Board approval was obtained from the institutional review board of Sun Yat-Sen Memorial Hospital of Sun Yat-Sen University (Guangzhou, China).
Methodology
• Prospective
• Diagnostic study
• Performed at one institution
Rights and permissions
About this article
Cite this article
Cheng, Z., Wu, Z., Shi, G. et al. Discrimination between benign and malignant breast lesions using volumetric quantitative dynamic contrast-enhanced MR imaging. Eur Radiol 28, 982–991 (2018). https://doi.org/10.1007/s00330-017-5050-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-017-5050-2