Abstract
Objectives
Collateral blood flow is accepted as a predictive factor of tissue fate in ischemic stroke. Thus, we aimed to evaluate a new method derived from MR perfusion source images to assess collateral flow in patients with ICA/MCA occlusions.
Methods
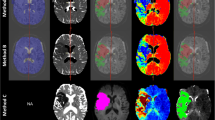
A total of 132 patients of the prospective 1000+ study were examined. MR perfusion source images were assessed according to Δimg_n = img_n + 1 − img_n − 1 using the five-grade Higashida collateral flow rating system. Higashida scores were correlated to mismatch (MM) volume, mismatch ratio, day 6 FLAIR lesion volumes and day 90 mRS.
Results
Patients with Higashida scores 3 and 4 had significantly lower admission NIHSS, smaller FLAIR day 6 lesion volumes (p < 0.001) and higher rates of better long-term outcome (mRS 0–2, p = 0.002). There was a linear trend for the association of Higashida grade 1 (p = 0.002) and 2 (p = 0.001) with unfavourable outcome (day 90 mRS 3–6), but no significant association was found for MM volume, MM ratio and day 90 mRS. Inter-rater agreement was 0.58 (95 % CI 0.43–0.73) on day 1, 0.70 (95 % CI 0.58–0.81) on day 2.
Conclusion
sMRP-SI Higashida score offers a non-invasive collateral vessel and tissue perfusion assessment of ischemic tissue. The predictive value of Higashida rating proved superior to MM with regard to day 90 mRS.
Key points
• Assessment of collateral flow using subtracted dynamic MR perfusion source imaging (sMRP-SI).
• sMRP-SI offers additional information about morphological characteristics of ischemic brain tissue.
• sMRP-SI collateral flow assessment proves superior to mismatch volume.
• Better collateral flow was significantly associated with better outcome (day 90 mRS).

Similar content being viewed by others
Abbreviations
- ASITN/SIR:
-
American Society of Interventional and Therapeutic Neuroradiology/Society of Radiology collateral flow grading system
- DWI:
-
diffusion weighted imaging
- FLAIR:
-
fluid attenuated inversion recovery
- HIR:
-
hypoperfusion intensity ratio
- ICA:
-
internal carotid artery
- iv:
-
intravenous
- MCA:
-
middle cerebral artery
- MM:
-
mismatch
- ml:
-
millilitre
- MRA:
-
magnetic resonance angiography
- mRS:
-
modified Rankin scale
- NIHSS:
-
National Institutes of Health stroke scale score
- PI:
-
perfusion imaging
- s:
-
seconds
- sMRP-SI:
-
subtracted dynamic MR perfusion source imaging
- TIMI:
-
thrombolysis in myocardial infarction
- TR:
-
repetition time
References
Hacke W, Kaste M, Bluhmki E, Investigators ECASS et al (2008) Thrombolysis with alteplase 3 to 4 · 5 hours after acute ischemic stroke. N Engl J Med 359:1317–1329
Albers GW (2013) Impact of recanalization, reperfusion, and collateral flow on clinical efficacy. Stroke 44:511–512
Wardlaw JM, Murray V, Berge E et al (2012) Recombinant tissue plasminogen activator for acute ischaemic stroke: an updated systematic review and meta-analysis. Lancet 379:2364–2372
Lee KY, Latour LL, Luby M, Hsia AW, Merino JG, Warach S (2009) Distal hyperintense vessels on FLAIR: an MRI marker for collateral circulation in acute stroke? Neurology 72:1134–1139
Bang OY, Saver JL, Alger JR, Starkman S, Ovbiagele B, Liebeskind DS et al (2008) Determinants of the distribution and severity of hypoperfusion in patients with ischemic stroke. Neurology 71:1804–1811
Christoforidis GA, Mohammad Y, Kehagias D, Avutu B, Slivka AP (2005) Angiographic assessment of pial collaterals as a prognostic indicator following intra-arterial thrombolysis for acute ischemic stroke. Am J Neuroradiol 26:1789–1797
Ciccone A, Valvassori L, Nichelatti M, for the SYNTHESIS Expansion Investigators et al (2013) Endovascular treatment for acute ischemic stroke. N Engl J Med 368:904–913
Campbell BCV, Christensen S, Tress BM, for the EPITHET Investigators et al (2013) Failure of collateral blood flow is associated with infarct growth in ischemic stroke. J Cereb Blood Flow Metab 44:3039–3043
Hotter B, Pittl S, Ebinger M et al (2009) Prospective study on the mismatch concept in acute stroke patients within the first 24 h after symptom onset – 1000Plus study. BMC Neurol. doi:10.1186/1471-2377-9-60
Higashida RT, Furlan AJ (2003) Trial design and reporting standards for intra-arterial cerebral thrombolysis for acute ischemic stroke. Stroke 34:109–137
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Ringelstein EB, Biniek R, Weiller C, Ammeling B, Nolte PN, Thron A (1992) Type and extent of hemispheric brain infarctions and clinical outcome in early and delayed middle cerebral artery recanalization. Neurology 42:289–298
Lee JH, Kim YJ, Choi JW et al (2013) Multimodal CT: favorable outcome factors in acute middle cerebral artery stroke with large artery occlusion. Eur Neurol 69:266–274
Lima FO, Furie KL, Silva GS et al (2010) The pattern of leptomeningeal collaterals on CT angiography is a strong predictor of long-term functional outcome in stroke patients with large vessel intracranial occlusion. Stroke 41:2316–2322
Liebeskind DS, Tomsick TA, Foster LD et al (2014) Collaterals at angiography and outcomes in the Interventional Management of Stroke (IMS) III Trial. Stroke 45:759–764
Miteff F, Levi CR, Bateman GA, Spratt N, McElduff P, Parsons MW (2009) The independent predictive utility of computed tomography angiographic collateral status in acute ischaemic stroke. Brain 132:2231–2238
Menon BK, Smith EE, Modi J et al (2011) Regional leptomeningeal score on CT angiography predicts clinical and imaging outcomes in patients with acute anterior circulation occlusions. Am J Neuroradiol 32:1640–1645
Tan IYL, Demchuk AM, Hopyan J et al (2009) CT angiography clot burden score and collateral score: correlation with clinical and radiologic outcomes in acute middle cerebral artery infarct. Am J Neuroradiol 30:525–531
Beyer SE, von Baumgarten L, Thierfelder KM et al (2014) Predictive value of the velocity of collateral filling in patients with acute ischemic stroke. J Cereb Blood Flow Metab 35:206–212
Smit EJ, Vonken E-J, van Seeters T et al (2013) Timing-invariant imaging of collateral vessels in acute ischemic stroke. Stroke 44:2194–2199
Calleja AI, Cortijo E, García-Bermejo P et al (2013) Collateral circulation on perfusion-computed tomography-source images predicts the response to stroke intravenous thrombolysis. Euro J Neurol 20:795–802
Menon BK, d’Esterre CD, Qazi EM et al (2015) Multiphase CT angiography: a new tool for the imaging triage of patients with acute ischemic stroke. Radiology 275:510–520
Kim SJ, Son JP, Ryoo S et al (2014) Approach to collateral flow imaging in ischemic stroke. Ann Neurol 76:356–369
Berkhemer OA, Beumer FD, van den Berg LA, for the MR CLEAN investigators et al (2015) A randomized trail of intraarterial treatment for acute ischemic stroke. N Engl J Med 372:11–20
Goyal M, Demchuk AM, Menon BK, for the ESCAPE Trial Investigators et al (2015) Randomized assessment of rapid endovascular treatment of ischemic stroke. N Engl J Med 12:1019–1030
Menon BK, Almekhlafi MA, Pereira VM et al; STAR Study Investigators (2014) Optimal workflow and process-based performance measures for endovascular therapy in acute ischemic stroke: analysis of the Solitaire FR thrombectomy for acute revasculatization study. Stroke 45:2024–2029
Khatri P, Yeatts SD, Mazighi M, Trialists IMSIII et al (2014) Time to angiographic reperfusion and clinical outcome after acute ischaemic stroke: an analysis of data from the Interventional Management of Stroke (IMS III) phase 3 trial. Lancet Neurol 13:567–574
Campbell BCV, Mitchell PJ, Kleinig TJ, for the EXTEND-IA Investigators et al (2015) Endovascular therapy for ischemic stroke with perfusion-imaging selection. N Engl J Med 372:1009–1018
Bang OY, Saver JL, Buck BH et al [on behalf of the UCLA Collateral Investigators] (2009) Impact of collateral flow on tissue fate in acute ischaemic stroke. J Neurol Neurosurg Psychiatry 79:625–629
Bang OY, Saver JL, Kim SJ et al (2011) Collateral flow predicts response to endovascular therapy for acute ischemic stroke. Stroke 42:693–699
Acknowledgments
We thank Anna Kufner for critical language revision of the manuscript. The scientific guarantor of this publication is PD Dr. Jochen Fiebach. The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article. Jochen B. Fiebach reports receiving consulting, lecture and advisory board fees from BMS, Siemens, Perceptive, Synarc, BioImaging Technologies, Novartis, Wyeth, Pfizer, Boehringer Ingelheim, Lundbeck and Sygnis
This study received funding from the Federal Ministry of Education and Research via the grant Center for Stroke Research Berlin (01EO0801 and 01EO01301). Dr. Ulrike Grittner kindly provided statistical advice for this manuscript. Institutional review board approval was obtained (EA4/026/08). Written informed consent was obtained from all subjects (patients) in this study. Some study subjects or cohorts have been previously presented at the International Stroke Conference, San Diego, 2014 as an oral presentation. Methodology: prospective, retrospective, observational, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Villringer, K., Serrano-Sandoval, R., Grittner, U. et al. Subtracted Dynamic MR Perfusion Source Images (sMRP-SI) provide Collateral Blood Flow Assessment in MCA Occlusions and Predict Tissue Fate. Eur Radiol 26, 1396–1403 (2016). https://doi.org/10.1007/s00330-015-3927-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-015-3927-5