Abstract
Objective
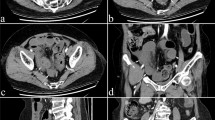
To assess the diagnostic accuracy of computed tomography (CT) angiography in the evaluation of patients with an episode of acute gastrointestinal haemorrhage.
Methods
Systematic review and meta-analysis to estimate pooled accuracy indices. A bivariate random effects model was adjusted to obtain a summary receiver-operating characteristic (sROC) curve and the corresponding area under the curve (AUC).
Results
Twenty-two studies were included and provided data on 672 patients (range of age 5–74) with a mean age of 65 years. The overall sensitivity of CT angiography for detecting active acute GI haemorrhage was 85.2 % (95 % CI 75.5 % to 91.5 %). The overall specificity of CT angiography was 92.1 % (95 % CI 76.7 % to 97.7 %). The likelihood ratios for positive and negative test results were 10.8 (95 % CI 3.4 to 34.4) and 0.16 (95 % CI 0.1 to 0.27) respectively, with an AUC of 0.935 (95 % CI 0.693 to 0.989). The sources of heterogeneity explored had no significant impact on diagnostic performance.
Conclusions
CT shows high diagnostic accuracy and is an excellent diagnostic tool for detection and localising of intestinal bleeding sites. It is highly available, provides fast detection and localisation of the bleeding site, and is minimally invasive.
Key Points
• CT angiography is increasingly used for investigating severe gastrointestinal bleeding.
• This systematic review and meta-analysis updates previous ones.
• In patients with massive gastrointestinal bleeding, CT angiography/MDCT detects bleeding accurately.
• CT angiography is useful in locating the bleeding site and determining appropriate treatment.





Similar content being viewed by others
Abbreviations
- CT:
-
Computed tomography
- MDCT:
-
Multi-detector computed tomography
- GI:
-
Gastrointestinal
- SROC:
-
Summary receiver-operating characteristic
- AUC:
-
Area under the curve
- Sen:
-
Sensitivity
- Spe:
-
Specificity
- LR:
-
Likelihood ratio
- DOR:
-
Diagnostic odds ratio
- ESS:
-
Effective sample size
- CI:
-
Confidence interval
References
Yoon W, Jeong YY, Shin SS, Lim HS, Song SG, Jang NG, Kim JK, Kang HK (2006) Acute massive gastrointestinal bleeding: detection and localization with arterial phase multi-detector row helical CT. Radiology 239:160–167
Marti M, Artigas JM, Garzon G, Alvarez-Sala R, Soto JA (2012) Acute lower intestinal bleeding: feasibility and diagnostic performance of CT angiography. Radiology 262:109–116
Al-Saeed O, Kombar O, Morsy M, Sheikh M (2011) Sixty-four multi-detector computerised tomography in the detection of lower gastrointestinal bleeding: a prospective study. J Med Imaging Radiat Oncol 55:252–258
Zink SI, Ohki SK, Stein B, Zambuto DA, Rosenberg RJ, Choi JJ, Tubbs DS (2008) Noninvasive evaluation of active lower gastrointestinal bleeding: comparison between contrast-enhanced MDCT and 99mTc-labeled RBC scintigraphy. Am J Roentgenol 191:1107–1114
Frattaroli FM, Casciani E, Spoletini D, Polettini E, Nunziale A, Bertini L, Vestri A, Gualdi G, Pappalardo G (2009) Prospective study comparing multi-detector row CT and endoscopy in acute gastrointestinal bleeding. World J Surg 33:2209–2217
Laing CJ, Tobias T, Rosenblum DI, Banker WL, Tseng L, Tamarkin SW (2007) Acute gastrointestinal bleeding: emerging role of multidetector CT angiography and review of current imaging techniques. Radiographics 27:1055–1070
Chua AE, Ridley LJ (2008) Diagnostic accuracy of CT angiography in acute gastrointestinal bleeding. J Med Imaging Radiat Oncol 52:333–338
Geffroy Y, Rodallec MH, Boulay-Coletta I, Julles MC, Ridereau-Zins C, Zins M (2011) Multidetector CT angiography in acute gastrointestinal bleeding: why, when, and how. Radiographics 31:E35–E46
Jaeckle T, Stuber G, Hoffmann MH, Freund W, Schmitz BL, Aschoff AJ (2008) Acute gastrointestinal bleeding: value of MDCT. Abdom Imaging 33:285–293
Schuetz A, Jauch KW (2001) Lower gastrointestinal bleeding: therapeutic strategies, surgical techniques and results. Langenbecks Arch Surg 386:17–25
Wu LM, Xu JR, Yin Y, Qu XH (2010) Usefulness of CT angiography in diagnosing acute gastrointestinal bleeding: a meta-analysis. World J Gastroenterol 16:3957–3963
Leeflang MM, Scholten RJ, Rutjes AW, Reitsma JB, Bossuyt PM (2006) Use of methodological search filters to identify diagnostic accuracy studies can lead to the omission of relevant studies. J Clin Epidemiol 59:234–240
Whiting P, Rutjes AW, Reitsma JB, Bossuyt PM, Kleijnen J (2003) The development of QUADAS: a tool for the quality assessment of studies of diagnostic accuracy included in systematic reviews. BMC Med Res Methodol 3:25
Reitsma JB, Glas AS, Rutjes AW, Scholten RJ, Bossuyt PM, Zwinderman AH (2005) Bivariate analysis of sensitivity and specificity produces informative summary measures in diagnostic reviews. J Clin Epidemiol 58:982–990
Deeks JJ, Macaskill P, Irwig L (2005) The performance of tests of publication bias and other sample size effects in systematic reviews of diagnostic test accuracy was assessed. J Clin Epidemiol 58:882–893
Zamora J, Abraira V, Muriel A, Khan K, Coomarasamy A (2006) Meta-DiSc: a software for meta-analysis of test accuracy data. BMC Med Res Methodol 6:31
Harbord RM (2008) Metandi:Stata module for meta-analysis of diagnostic accuracy. Statistical Software Components, Boston College Department of Economics. Revised 15 Apr 2008
Kim JW, Shin SS, Yoon W, Chang NK, Heo SH, Jeong YY, Kang HK (2011) Diagnosis of acute gastrointestinal bleeding: comparison of the arterial, the portal, and the combined set using 64-section computed tomography. J Comput Assist Tomogr 35:206–211
Palma J, Mihaila M, Pilleul F (2010) Multidetector computed tomography in acute lower gastrointestinal bleeding. Rep Med Imaging 3:107–113
Kennedy DW, Laing CJ, Tseng LH, Rosenblum DI, Tamarkin SW (2010) Detection of active gastrointestinal hemorrhage with CT angiography: a 4(1/2)-year retrospective review. J Vasc Interv Radiol 21:848–855
Foley PT, Ganeshan A, Anthony S, Uberoi R (2010) Multi-detector CT angiography for lower gastrointestinal bleeding: can it select patients for endovascular intervention? J Med Imaging Radiat Oncol 54:9–16
Hara AK, Walker FB, Silva AC, Leighton JA (2009) Preliminary estimate of triphasic CT enterography performance in hemodynamically stable patients with suspected gastrointestinal bleeding. Am J Roentgenol 193:1252–1260
Heiss P, Zorger N, Hamer OW, Seitz J, Muller-Wille R, Koller M, Herold T, Scholmerich J, Feuerbach S, Wrede CE (2009) Optimized multidetector computed tomographic protocol for the diagnosis of active obscure gastrointestinal bleeding: a feasibility study. J Comput Assist Tomogr 33:698–704
Lee S, Welman CJ, Ramsay D (2009) Investigation of acute lower gastrointestinal bleeding with 16- and 64-slice multidetector CT. J Med Imaging Radiat Oncol 53:56–63
Lee SM, Kim TO, Park HY, Kim KY, Kim GH, Kang DH, Song GA, Kim S (2008) Role of multi-detector row computed tomography for localization of acute lower gastrointestinal bleeding. Korean J Gastroenterol 51:298–304
Jaeckle T, Stuber G, Hoffmann MH, Jeltsch M, Schmitz BL, Aschoff AJ (2008) Detection and localization of acute upper and lower gastrointestinal (GI) bleeding with arterial phase multi-detector row helical CT. Eur Radiol 18:1406–1413
Scheffel H, Pfammatter T, Wildi S, Bauerfeind P, Marincek B, Alkadhi H (2007) Acute gastrointestinal bleeding: detection of source and etiology with multi-detector-row CT. Eur Radiol 17:1555–1565
Sabharwal R, Vladica P, Chou R, Law WP (2006) Helical CT in the diagnosis of acute lower gastrointestinal haemorrhage. Eur J Radiol 58:273–279
Ko HS, Tesdal K, Dominguez E, Kaehler G, Sadick M, Duber C, Diehl S (2005) Localization of bleeding using 4-row detector-CT in patients with clinical signs of acute gastrointestinal hemorrhage. RÖFO 177:1649–1654
Lijmer JG, Mol BW, Heisterkamp S, Bonsel GJ, Prins MH, van der Meulen JH, Bossuyt PM (1999) Empirical evidence of design-related bias in studies of diagnostic tests. JAMA 282:1061–1066
Tew K, Davies RP, Jadun CK, Kew J (2004) MDCT of acute lower gastrointestinal bleeding. Am J Roentgenol 182:427–430
Yamaguchi T, Yoshikawa K (2003) Enhanced CT for initial localization of active lower gastrointestinal bleeding. Abdom Imaging 28:634–636
Ernst O, Bulois P, Saint-Drenant S, Leroy C, Paris JC, Sergent G (2003) Helical CT in acute lower gastrointestinal bleeding. Eur Radiol 13:114–117
Ettorre GC, Francioso G, Garribba AP, Fracella MR, Greco A, Farchi G (1997) Helical CT angiography in gastrointestinal bleeding of obscure origin. Am J Roentgenol 168:727–731
Miller FH, Hwang CM (2004) An initial experience: using helical CT imaging to detect obscure gastrointestinal bleeding. Clin Imaging 28:245–251
Bossuyt PM, Reitsma JB, Bruns DE, Gatsonis CA, Glasziou PP, Irwig LM, Lijmer JG, Moher D, Rennie D, de Vet HC (2003) Towards complete and accurate reporting of studies of diagnostic accuracy: the STARD Initiative. Ann Intern Med 138:40–44
Acknowledgements
The EBM-CONNECT (Evidence-Based Medicine Collaboration: Network for systematic reviews and guideline development research and dissemination) Collaboration:
L. Mignini, Centro Rosarino de Estudios Perinatales, Argentina; P. von Dadelszen, L. Magee and D. Sawchuck, University of British Columbia, Canada; E. Gao, Shanghai Institute of Planned Parenthood Research, China; B.W. Mol and K. Oude Rengerink, Academic Medical Centre, The Netherlands; J. Zamora, Ramon y Cajal Hospital, Spain; C. Fox and J. Daniels, University of Birmingham, UK; K.S. Khan, S. Thangaratinam and C. Meads, Barts and the London School of Medicine, Queen Mary University of London, UK.
Funding
The authors received funding from the European Union made available to the EBM-CONNECT Collaboration through its Seventh Framework Programme, Marie Curie Actions, International Staff Exchange Scheme (proposal no.: 101377; grant agreement no.: 247613); EBM-CONNECT Canadian Collaborators received funding from the Canadian Institutes of Health Research.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Please see end of the article for a complete list of collaborators.
Rights and permissions
About this article
Cite this article
García-Blázquez, V., Vicente-Bártulos, A., Olavarria-Delgado, A. et al. Accuracy of CT angiography in the diagnosis of acute gastrointestinal bleeding: systematic review and meta-analysis. Eur Radiol 23, 1181–1190 (2013). https://doi.org/10.1007/s00330-012-2721-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-012-2721-x