Abstract
Objective
The goal of this study was to compare the semi-quantitative Goutallier classification for fat infiltration with quantitative fat-fraction derived from a magnetic resonance imaging (MRI) chemical shift-based water/fat separation technique.
Methods
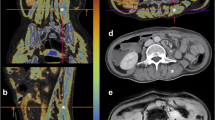
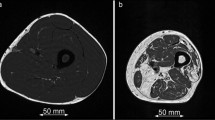
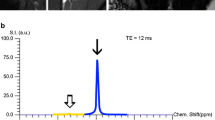
Sixty-two women (age 61 ± 6 years), 27 of whom had diabetes, underwent MRI of the calf using a T1-weighted fast spin-echo sequence and a six-echo spoiled gradient-echo sequence at 3 T. Water/fat images and fat fraction maps were reconstructed using the IDEAL algorithm with T2* correction and a multi-peak model for the fat spectrum. Two radiologists scored fat infiltration on the T1-weighted images using the Goutallier classification in six muscle compartments. Spearman correlations between the Goutallier grades and the fat fraction were calculated; in addition, intra-observer and inter-observer agreement were calculated.
Results
A significant correlation between the clinical grading and the fat fraction values was found for all muscle compartments (P < 0.0001, R values ranging from 0.79 to 0.88). Goutallier grades 0–4 had a fat fraction ranging from 3.5 to 19%. Intra-observer and inter-observer agreement values of 0.83 and 0.81 were calculated for the semi-quantitative grading.
Conclusion
Semi-quantitative grading of intramuscular fat and quantitative fat fraction were significantly correlated and both techniques had excellent reproducibility. However, the clinical grading was found to overestimate muscle fat.
Key Points
• Fat infiltration of muscle commonly occurs in many metabolic and neuromuscular diseases.
• Image-based semi-quantitative classifications for assessing fat infiltration are not well validated.
• Quantitative MRI techniques provide an accurate assessment of muscle fat.




Similar content being viewed by others
References
Wren TA, Bluml S, Tseng-Ong L, Gilsanz V (2008) Three-point technique of fat quantification of muscle tissue as a marker of disease progression in Duchenne muscular dystrophy: preliminary study. AJR Am J Roentgenol 190:W8–W12
Cheung S, Dillon E, Tham SC et al (2011) The presence of fatty infiltration in the infraspinatus: its relation with the condition of the supraspinatus tendon. Arthroscopy 27:463–470
Hilton TN, Tuttle LJ, Bohnert KL, Mueller MJ, Sinacore DR (2008) Excessive adipose tissue infiltration in skeletal muscle in individuals with obesity, diabetes mellitus, and peripheral neuropathy: association with performance and function. Phys Ther 88:1336–1344
Andersen H, Gadeberg PC, Brock B, Jakobsen J (1997) Muscular atrophy in diabetic neuropathy: a stereological magnetic resonance imaging study. Diabetologia 40:1062–1069
Andersen H, Nielsen S, Mogensen CE, Jakobsen J (2004) Muscle strength in type 2 diabetes. Diabetes 53:1543–1548
Andersen H, Poulsen PL, Mogensen CE, Jakobsen J (1996) Isokinetic muscle strength in long-term IDDM patients in relation to diabetic complications. Diabetes 45:440–445
Gallagher D, Kuznia P, Heshka S et al (2005) Adipose tissue in muscle: a novel depot similar in size to visceral adipose tissue. Am J Clin Nutr 81:903–910
Goodpaster BH, Thaete FL, Kelley DE (2000) Thigh adipose tissue distribution is associated with insulin resistance in obesity and in type 2 diabetes mellitus. Am J Clin Nutr 71:885–892
Frimel TN, Sinacore D, Wright NR, Villareal DT, Klein S (2007) Sarcopenia in frail elderly obese participants: role of excess skeletal muscle lipid accumulation. J Geriatr Phys Ther 30:138
Gaeta M, Scribano E, Mileto A et al (2011) Muscle fat fraction in neuromuscular disorders: dual-echo dual-flip-angle spoiled gradient-recalled MR imaging technique for quantification—a feasibility study. Radiology. doi:10.1148/radiol.10101108
Karampinos DC, Baum T, Nardo L et al (2011) Characterization of regional distribution of skeletal muscle adipose tissue in type 2 diabetes using chemical shift-based water/fat separation. J Magn Reson Imaging. doi:10.1002/jmri.23512
Pfirrmann CWA, Schmid MR, Zanetti M, Jost B, Gerber C, Hodler J (2004) assessment of fat content in supraspinatus muscle with proton MR spectroscopy in asymptomatic volunteers and patients with supraspinatus tendon lesions1. Radiology 232:709–715
Goutallier D, Postel J-M, Bernageau J, Lavau L, Voisin M-C (1994) Fatty muscle degeneration in cuff ruptures: pre- and postoperative evaluation by CT scan. Clin Orthop Relat Res 304:78–83
Mercuri E, Talim B, Moghadaszadeh B et al (2002) Clinical and imaging findings in six cases of congenital muscular dystrophy with rigid spine syndrome linked to chromosome 1p (RSMD1). Neuromuscul Disord 12:631–638
Kornblum C, Lutterbey G, Bogdanow M et al (2006) Distinct neuromuscular phenotypes in myotonic dystrophy types 1 and 2: a whole body highfield MRI study. J Neurol 253:753–761
Fischer D, Kley RA, Strach K et al (2008) Distinct muscle imaging patterns in myofibrillar myopathies. Neurology 71:758–765
Fuchs B, Weishaupt D, Zanetti M, Hodler J, Gerber C (1999) Fatty degeneration of the muscles of the rotator cuff: assessment by computed tomography versus magnetic resonance imaging. J Shoulder Elbow Surg 8:599–605
Dixon WT (1984) Simple proton spectroscopic imaging. Radiology 153:189–194
Glover GH, Schneider E (1991) Three-point Dixon technique for true water/fat decomposition with B0 inhomogeneity correction. Magn Reson Med 18:371–383
Reeder SB, Pineda AR, Wen Z et al (2005) Iterative decomposition of water and fat with echo asymmetry and least-squares estimation (IDEAL): application with fast spin-echo imaging. Magn Reson Med 54:636–644
Yu H, Reeder SB, Shimakawa A, Brittain JH, Pelc NJ (2005) Field map estimation with a region growing scheme for iterative 3-point water-fat decomposition. Magn Reson Med 54:1032–1039
Yu H, McKenzie CA, Shimakawa A et al (2007) Multiecho reconstruction for simultaneous water-fat decomposition and T2* estimation. J Magn Reson Imaging 26:1153–1161
Middleton MS, Hamilton G, Bydder M, Sirlin CB (2009) How much fat is under the water peak in liver fat MR spectroscopy? In: Proceedings of the 17th Annual Meeting of ISMRM, Honolulu, p 4331
Yu H, Shimakawa A, McKenzie CA, Brodsky E, Brittain JH, Reeder SB (2008) Multiecho water-fat separation and simultaneous R2* estimation with multifrequency fat spectrum modeling. Magn Reson Med 60:1122–1134
Karampinos DC, Yu H, Shimakawa A, Link TM, Majumdar S (2011) T(1)-corrected fat quantification using chemical shift-based water/fat separation: application to skeletal muscle. Magn Reson Med 66:1312–1326
Bydder M, Yokoo T, Hamilton G et al (2008) Relaxation effects in the quantification of fat using gradient echo imaging. Magn Reson Imaging 26:347–359
Liu CY, McKenzie CA, Yu H, Brittain JH, Reeder SB (2007) Fat quantification with IDEAL gradient echo imaging: correction of bias from T1 and noise. Magn Reson Med 58:354–364
Yu H, Shimakawa A, Hines CD et al (2011) Combination of complex-based and magnitude-based multiecho water-fat separation for accurate quantification of fat-fraction. Magn Reson Med 66:199–206
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Goutallier D, Postel JM, Lavau L, Bernageau J (1999) Impact of fatty degeneration of the suparspinatus and infraspinatus msucles on the prognosis of surgical repair of the rotator cuff. Rev Chir Orthop Reparatrice Appar Mot 85:668–676
Gloor M, Fasler S, Fischmann A et al (2011) Quantification of fat infiltration in oculopharyngeal muscular dystrophy: comparison of three MR imaging methods. J Magn Reson Imaging 33:203–210
Machann J, Bachmann OP, Brechtel K et al (2003) Lipid content in the musculature of the lower leg assessed by fat selective MRI: intra- and interindividual differences and correlation with anthropometric and metabolic data. J Magn Reson Imaging 17:350–357
Wattjes M, Kley R, Fischer D (2010) Neuromuscular imaging in inherited muscle diseases. Eur Radiol 20:2447–2460
Ford ES, Giles WH, Dietz WH (2002) Prevalence of the metabolic syndrome among US adults: findings from the third National Health and Nutrition Examination Survey. JAMA 287:356–359
Vettor R, Milan G, Franzin C et al (2009) The origin of intermuscular adipose tissue and its pathophysiological implications. Am J Physiol Endocrinol Metab 297:E987–E998
Gallagher D, Kelley DE, Yim JE et al (2009) Adipose tissue distribution is different in type 2 diabetes. Am J Clin Nutr 89:807–814
Durheim MT, Slentz CA, Bateman LA, Mabe SK, Kraus WE (2008) Relationships between exercise-induced reductions in thigh intermuscular adipose tissue, changes in lipoprotein particle size, and visceral adiposity. Am J Physiol Endocrinol Metab 295:E407–E412
Acknowledgements
This study was supported by the National Institutes of Health grants R01-AG17762 and RC1-AR058405.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Alizai, H., Nardo, L., Karampinos, D.C. et al. Comparison of clinical semi-quantitative assessment of muscle fat infiltration with quantitative assessment using chemical shift-based water/fat separation in MR studies of the calf of post-menopausal women. Eur Radiol 22, 1592–1600 (2012). https://doi.org/10.1007/s00330-012-2404-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-012-2404-7