Abstract
Objectives
The study aims were to identify CT features that predict outcome of fibrotic idiopathic interstitial pneumonia (IIP) when information from lung biopsy data is unavailable.
Methods
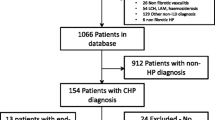
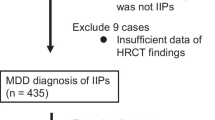
HRCTs of 146 consecutive patients presenting with fibrotic IIP were studied. Visual estimates were made of the extent of abnormal lung and proportional contribution of fine and coarse reticulation, microcystic (cysts ≤4 mm) and macrocystic honeycombing. A score for severity of traction bronchiectasis was also assigned. Using death as our primary outcome measure, variables were analysed using the Cox proportional hazards model.
Results
CT features predictive of a worse outcome were coarse reticulation, microcystic and macrocystic honeycombing, as well as overall extent of lung abnormality (p < 0.001). Importantly, increased severity of traction bronchiectasis, corrected for extent of parenchymal abnormality, was predictive of poor prognosis regardless of the background pattern of abnormal lung (HR = 1.04, CI = 1.03–1.06, p < 0.001). On bivariate Cox analysis microcystic honeycombing was a more powerful determinant of a poor prognosis than macrocystic honeycombing.
Conclusions
In fibrotic IIPs we have shown that increasingly severe traction bronchiectasis is indicative of higher mortality irrespective of the HRCT pattern and extent of disease. Extent of microcystic honeycombing is a more powerful determinant of outcome than macrocystic honeycombing.

Similar content being viewed by others
References
Demedts M, Costabel U (2002) ATS/ERS international multidisciplinary consensus classification of the idiopathic interstitial pneumonias. Eur Respir J 19:794–796
du Bois R, King TE Jr (2007) Challenges in pulmonary fibrosis x 5: the NSIP/UIP debate. Thorax 62:1008–1012
Travis WD, Hunninghake G, King TE Jr, Lynch DA, Colby TV, Galvin JR, Brown KK, Chung MP, Cordier JF, du Bois RM, Flaherty KR, Franks TJ, Hansell DM, Hartman TE, Kazerooni EA, Kim DS, Kitaichi M, Koyama T, Martinez FJ, Nagai S, Midthun DE, Müller NL, Nicholson AG, Raghu G, Selman M, Wells A (2008) Idiopathic nonspecific interstitial pneumonia: report of an American Thoracic Society project. Am J Respir Crit Care Med 177:1338–1347
Raghu G, Mageto YN, Lockhart D, Schmidt RA, Wood DE, Godwin JD (1999) The accuracy of the clinical diagnosis of new-onset idiopathic pulmonary fibrosis and other interstitial lung disease: a prospective study. Chest 116:1168–1174
Aziz ZA, Wells AU, Hansell DM, Bain GA, Copley SJ, Desai SR, Ellis SM, Gleeson FV, Grubnic S, Nicholson AG, Padley SP, Pointon KS, Reynolds JH, Robertson RJ, Rubens MB (2004) HRCT diagnosis of diffuse parenchymal lung disease: inter-observer variation. Thorax 59:506–511
Bradley B, Branley HM, Egan JJ, Greaves MS, Hansell DM, Harrison NK, Hirani N, Hubbard R, Lake F, Millar AB, Wallace WA, Wells AU, Whyte MK, Wilsher ML (2008) Interstitial lung disease guideline: the British Thoracic Society in collaboration with the Thoracic Society of Australia and New Zealand and the Irish Thoracic Society. Thorax 63(Suppl 5):1–58
MacDonald SL, Rubens MB, Hansell DM, Copley SJ, Desai SR, du Bois RM, Nicholson AG, Colby TV, Wells AU (2001) Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparative appearances at and diagnostic accuracy of thin-section CT. Radiology 221:600–605
Silva CI, Müller NL, Hansell DM, Lee KS, Nicholson AG, Wells AU (2008) Nonspecific interstitial pneumonia and idiopathic pulmonary fibrosis: changes in pattern and distribution of disease over time. Radiology 247:251–259
Johnston ID, Prescott RJ, Chalmers JC, Rudd RM (1997) British Thoracic Society study of cryptogenic fibrosing alveolitis: current presentation and initial management. Fibrosing Alveolitis Subcommittee of the Research Committee of the British Thoracic Society. Thorax 52:38–44
Nicholson AG, Addis BJ, Bharucha H, Clelland CA, Corrin B, Gibbs AR, Hasleton PS, Kerr KM, Ibrahim NB, Stewart S, Wallace WA, Wells AU (2004) Inter-observer variation between pathologists in diffuse parenchymal lung disease. Thorax 59:500–505
Wells AU (2008) An approach to diagnosis of diffuse lung disease. In: Albert RK, Spiro SG, Jett JR (eds) Clinical respiratory medicine, 3rd edn. Mosby, Lonso, pp 655–656
Walsh SL, Hansell DM (2010) Diffuse interstitial lung disease: overlaps and uncertainties. Eur Radiol 20:1859–1867
Sumikawa H, Johkoh T, Colby TV, Ichikado K, Suga M, Taniguchi H, Kondoh Y, Ogura T, Arakawa H, Fujimoto K, Inoue A, Mihara N, Honda O, Tomiyama N, Nakamura H, Müller NL (2008) Computed tomography findings in pathological usual interstitial pneumonia: relationship to survival. Am J Respir Crit Care Med 177:433–439
Shin KM, Lee KS, Chung MP, Han J, Bae YA, Kim TS, Chung MJ (2008) Prognostic determinants among clinical, thin-section CT, and histopathologic findings for fibrotic idiopathic interstitial pneumonias: tertiary hospital study. Radiology 249:328–337
Marten K, Milne D, Antoniou KM, Nicholson AG, Tennant RC, Hansel TT, Wells AU, Hansell DM (2009) Non-specific interstitial pneumonia in cigarette smokers: a CT study. Eur Radiol 19:1679–1685
Hansell DM, Bankier AA, MacMahon H, McLoud TC, Müller NL, Remy J (2008) Fleischner Society: glossary of terms for thoracic imaging. Radiology 246:697–722
Wells AU, Desai SR, Rubens MB, Goh NS, Cramer D, Nicholson AG, Colby TV, du Bois RM, Hansell DM (2003) Idiopathic pulmonary fibrosis: a composite physiologic index derived from disease extent observed by computed tomography. Am J Respir Crit Care Med 167:962–969
Brennan P, Silman A (1992) Statistical methods for assessing observer variability in clinical measures. BMJ 304:1491–1494
Antoniou KM, Hansell DM, Rubens MB, Marten K, Desai SR, Siafakas NM et al (2008) Idiopathic pulmonary fibrosis: outcome in relation to smoking status. Am J Respir Crit Care Med 177:190–194
Sumikawa H, Johkoh T, Ichikado K, Taniguchi H, Kondoh Y, Fujimoto K, Tateishi U, Hiramatsu T, Inoue A, Natsag J, Ikemoto M, Mihara N, Honda O, Tomiyama N, Hamada S, Nakamura H, Müller NL (2006) Usual interstitial pneumonia and chronic idiopathic interstitial pneumonia: analysis of CT appearance in 92 patients. Radiology 241:258–266
Akira M, Inoue Y, Kitaichi M, Yamamoto S, Arai T, Toyokawa K (2009) Usual interstitial pneumonia and nonspecific interstitial pneumonia with and without concurrent emphysema: thin-section CT findings. Radiology 251:271–279
Desai SR, Veeraraghavan S, Hansell DM, Nikolakopolou A, Goh NS, Nicholson AG, Colby TV, Denton CP, Black CM, du Bois RM, Wells AU (2004) CT features of lung disease in patients with systemic sclerosis: comparison with idiopathic pulmonary fibrosis and nonspecific interstitial pneumonia. Radiology 232:560–567
Mueller-Mang C, Grosse C, Schmid K, Stiebellehner L, Bankier AA (2007) What every radiologist should know about idiopathic interstitial pneumonias. Radiographics 27:595–615
Lynch DA, Godwin J, Safrin S, Starko KM, Hormel P, Brown KK, Raghu G, King TE Jr, Bradford WZ, Schwartz DA, Richard WW (2005) High-resolution computed tomography in idiopathic pulmonary fibrosis: diagnosis and prognosis. Am J Respir Crit Care Med 172:488–493
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Edey, A.J., Devaraj, A.A., Barker, R.P. et al. Fibrotic idiopathic interstitial pneumonias: HRCT findings that predict mortality. Eur Radiol 21, 1586–1593 (2011). https://doi.org/10.1007/s00330-011-2098-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-011-2098-2