Abstract
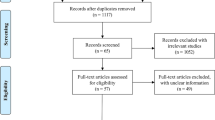
The incidence of Pneumocystis jirovecii pneumonia (PJP) has increased over recent years in patients with systemic autoimmune rheumatic diseases (SARD). PJP prognosis is poor in those receiving immunosuppressive therapy and glucocorticoids in particular. Despite the effectiveness of cotrimoxazole against PJP, the risk of adverse effects remains significant, and no consensus has emerged regarding the need for PJP prophylaxis in SARD patients undergoing immunosuppressor therapies.Objective: To evaluate the efficacy and safety of cotrimoxazole prophylaxis against PJP in SARD adult patients receiving immunosuppressive therapies. Methods: We performed a systematic review, consulting MEDLINE, EMBASE, and Cochrane Library databases up to April 2020. Outcomes covered prevention of PJP, other infections, morbidity, mortality, and safety. The information obtained was summarized with a narrative review and results were tabulated. Of the 318 identified references, 8 were included. Two were randomized controlled trials and six observational studies. The quality of studies was moderate or low. Despite disparities in the cotrimoxazole prophylaxis regimens described, results were consistent in terms of efficacy, particularly with glucocorticoid doses > 20 mg/day. However, cotrimoxazole 400 mg/80 mg/day, prescribed three times/ week, or 200 mg/40 mg/day or in dose escalation, exhibited similar positive performances. Conversely, cotrimoxazole 400 mg/80 mg/day showed higher incidences of withdrawals and adverse effects. Cotrimoxazole prophylaxis against PJP exhibited efficacy in SARD, mainly in patients taking glucocorticoids ≥ 20 mg/day. All cotrimoxazole regimens exposed seemed equally efficacious, although, higher quality trials are needed. Adverse effects were observed 2 months after initiation, particularly with the 400 mg/80 mg/day regimen. Conversely, escalation dosing or 200 mg/40 mg/day regimens appeared better tolerated.


Similar content being viewed by others
References
Thomas C, Limper A (2004) Pneumocystis pneumonia. N Engl J Med 350:2487–2498
Park JW, Curtis JR, Moon J, Song YW, Kim S, Lee EB (2018) Prophylactic effect of trimethoprim-sulfamethoxazole for pneumocystis pneumonia in patients with rheumatic diseases exposed to prolonged high-dose glucocorticoids. Ann Rheum Dis 77(5):644–649
Senanayake R, Mukhtar M (2013) Cotrimoxazole-induced hypoglycaemia in a patient with churg-strauss syndrome. Endocrinology. 2013:415810. https://doi.org/10.1155/2013/415810
Cettomai D, Gelber A, Christopher-Stine L (2010) A survey of rheumatologists’ practice for prescribing pneumocystis prophylaxis. J Rheumatol 37:792–799
Moher D, Liberati A, Tetzlaff J, Altman D (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 8(336):341
López de Argumedo M, Reviriego E, Gutiérrez A, JC B (2017) Actualización del Sistema de Trabajo Compartido para Revisiones Sistemáticas de la Evidencia Científica y Lectura Crítica (Plataforma FLC 3.0). Ministerio de Sanidad, Servicios Sociales e Igualdad Servicio de Evaluación de Tecnologías Sanitarias del País Vasco
Scottish Intercollegiate Guidelines Network (2011) SIGN 50, a guideline developer’s handbook. Edinburgh: SIGN; 2015 (SIGN publication no. 50). [November 2015]. Available from URL: http://www.sign.ac.uk
Utsunomiya M, Dobashi H, Odani T et al (2017) Optimal regimens of sulfamethoxazole-trimethoprim for chemoprophylaxis of Pneumocystis pneumonia in patients with systemic rheumatic diseases: results from a non-blinded, randomized controlled trial. Arthritis Res Ther 19(1):7
Yamamoto T, Hasunuma T, Takagi K et al (2014) A feasibility study assessing tolerability of daily versus twice weekly trimethoprim-sulfamethoxazole regimen for prophylaxis against pneumocystis pneumonia in patients with systemic autoimmune diseases on glucocorticoid therapy. Jpn J Clin Pharmacol Ther 45(3):89–92
Maezawa R, Kurasawa K, Arai S, Okada H, Owada T, Fukuda T (2013) Positivity for anti-RNP antibody is a risk factor for adverse effects caused by trimethoprim-sulfamethoxazole, a prophylactic agent for P. jiroveci pneumonia, in patients with connective tissue diseases. Mod Rheumatol 23(1):62–70
Ogawa J, Harigai M, Nagasaka K, Nakamura T, Miyasaka N (2005) Prediction of and prophylaxis against Pneumocystis pneumonia in patients with connective tissue diseases undergoing medium- or high-dose corticosteroid therapy. Mod Rheumatol 15(2):91–96
Schmajuk G, Jafri K, Evans M, et al (2018) Pneumocystis jirovecii pneumonia (PJP) prophylaxis patterns among patients with rheumatic diseases receiving high-risk immunosuppressant drugs. Semin Arthritis Rheum 48(6):1087–1092. https://doi.org/10.1016/j.semarthrit.2018.10.018
Takenaka K, Komiya Y, Ota M, Yamazaki H, Nagasaka K (2013) A dose-escalation regimen of trimethoprim-sulfamethoxazole is tolerable for prophylaxis against Pneumocystis jiroveci pneumonia in rheumatic diseases. Mod Rheumatol 23(4):752–758
Vananuvat P, Suwannalai P, Sungkanuparph S, Limsuwan T, Ngamjanyaporn P, Janwityanujit S (2011) Primary prophylaxis for Pneumocystis jirovecii pneumonia in patients with connective tissue diseases. Semin Arthritis Rheum 41(3):497–502
Meuli K, Chapman P, O’Donnell J, Frampton C, Stamp L (2007) Audit of pneumocystis pneumonia in patients seen by the Christchurch Hospital rheumatology service over a 5-year period. Intern Med J 37(10):687–692
Braga BP, Prieto-Gonzalez S, Hernandez-Rodriguez J (2019) Pneumocystis jirovecii pneumonia prophylaxis in immunocompromised patients with systemic autoimmune diseases. Med Clin (Barc) 152(12):502–507. https://doi.org/10.1016/j.medcli.2019.01.010
Godeau B, Coutant-Perronne V, Le Thi HD et al (1994) Pneumocystis carinii pneumonia in the course of connective tissue disease: report of 34 cases. J Rheumatol 21(2):246–251
Grewal P, Brassard A (2009) Fact or fiction: does the non-HIV/AIDS immunosuppressed patient need Pneumocystis jiroveci pneumonia prophylaxis? An updated literature review. J Cutan Med Surg 13(6):308–312
Cooley L, Dendle D, Wolf J, Teh BW, Chen SC, Boultis C (2014) Consensus guidelines for diagnosis, prophylaxis and management of Pneumocystis jirovecii pneumonia in patients with haematological and solid malignancies. Int Med J 44(1350):1363
Baulier G, Issa N, Gabriel F, Accoceberry I, Camou F, Duffau P (2018) Guidelines for prophylaxis of Pneumocystis pneumonia cannot rely solely on CD4-cell count in autoimmune and inflammatory diseases. Clin Exp Rheumatol 36(3):490–493
Abe Y, Fujibayashi K, Nishizaki Y et al (2019) Conventional-dose versus half-dose sulfamethoxazole-trimethoprim for the prophylaxis of pneumocystis pneumonia in patients with systemic rheumatic disease: a non-blind. Randomized Controlled Trial Acta Med Okayama 73(1):85–89
Matraiah EH, Olisaka N, Philipos M et al (2018) Late-onset Pneumocystis jirovecii pneumonia (PJP) in patients with ANCA-associated vasculitis. Clin Rheumatol 37(7):1991–1996
Ward M, Donald F (1999) Pneumocystis carinii pneumonia in patients with connective tissue diseases: the role of hospital experience in diagnosis and mortality. Arthritis Rheum 42:780–789
Ognibene FP, Shelhamer JH, Hoffman GS et al (1995) Pneumocystis carinii pneumonia: a major complication of immunosuppressive therapy in patients with Wegener’s granulomatosis. Am J Respir Crit Care Med 151(3 Pt 1):795–799
Teichtahl AJ, Morrisroe K, Ciciriello S, Jennens I, Tadros S, Wicks I (2015) Pneumocystis jirovecci pneumonia in connective tissue diseases: comparison with other immunocompromised patients. Semin Arthritis Rheum 45(1):86–90
Vallabhaneni S, Chiller TM (2016) Fungal infections and new biologic therapies. Curr Rheumatol Rep 18(5):29
Kronbichler A, Jayne DR, Mayer G (2015) Frequency, risk factors and prophylaxis of infection in ANCA-associated vasculitis. Eur J Clin Invest 45(3):346–368
Tasaka S (2020) Recent advances in the diagnosis and management of Pneumocystis pneumonia. Tuberc Respir Dis. 83(132):140
Caselli D, Petris MG, Rondelli R et al (2014) Single-day trimethoprim/sulfamethoxazole prophylaxis for Pneumocystis pneumonia in children with cancer. J Pediatr 164(2):389-392.e381
Ramesh Prasad GV, Beckley J, Mathur M, Gunasekaran M, Nash MM, Rapi L (2019) Safety and efficacy of prophylaxis for Pneumocystis jirovecii pneumonia involving trimethoprim-sulfamethoxazole dose reduction in kidney transplantation. BMC Infect Dis 19:311
Martin SL, Fishman JA (2013) Practice. aTAidCo. Pneumocystis pneumonia in solid organ transplantation. Am J Transplant 13:272–279
Wolfe RM, Peacock JE Jr (2017) Pneumocystis pneumonia and the rheumatologist: which patients are at risk and how can PCP be prevented? Curr Rheumatol Rep 19(6):35
Chung JB, Armstrong K, Schwartz JS, Albert D (2000) Cost-effectiveness of prophylaxis against Pneumocystis carinii pneumonia in patients with Wegner’s granulomatosis undergoing immunosuppressive therapy. Arthritis Rheum 43(8):1841–1848
Soejima M, Sugiura T, Kawaguchi Y et al (2007) Association of the diplotype configuration at the N-acetyltransferase 2 gene with adverse events with co-trimoxazole in Japanese patients with systemic lupus erythematosus. Arthritis Res Ther 9(2):R23
Smith CL, Brown I (1997) BM Torraca (1997) Acetylator status and tolerance of high-dose trimethoprim–sulfamethoxazole therapy among patients infected with human immunodeficiency virus. Clin Infect Dis. 25:1477–1478
Belchi-Hernandez J, Espinosa-Parrra FJ (1996) Management of adverse reactions to prophylactic trimethoprim-sulfamethoxazole in patients with human immunodeficiency virus infection. Ann Allergy Asthma Immunol 76(355):358
Petri M, Allbritton J (1992) Antibiotic allergy in systemic lupus erythematosus: a case–control study. J Rheumatol 19(265):269
Acknowledgements
The authors are grateful to Mercedes Guerra for her assistance in designing the reference search strategy and for performing primary reference selection, and to SER for revising the manuscript.
Funding
The present study was sponsored by the Spanish Society of Rheumatology (SER).
Author information
Authors and Affiliations
Contributions
CAP: visualization, writing—original draft lead, writing—review and editing. MBN-A: formal analysis, writing—original draft, writing—review and editing, lead. NB-G methodology, project administration, supervision. PDCF: conceptualization, investigation, supervision. IR-F writing—review and editing.
Corresponding author
Ethics declarations
Conflict of interest
Authors declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Pereda, C.A., Nishishinya-Aquino, M.B., Brito-García, N. et al. Is cotrimoxazole prophylaxis against Pneumocystis jirovecii pneumonia needed in patients with systemic autoimmune rheumatic diseases requiring immunosuppressive therapies?. Rheumatol Int 41, 1419–1427 (2021). https://doi.org/10.1007/s00296-021-04808-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-021-04808-4