Abstract
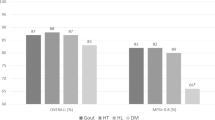
Allopurinol is effective for the control of gout and its long-term complications when taken consistently. There is evidence that adherence to allopurinol therapy varies across population groups. This may exacerbate differences in the burden of gout on population groups and needs to be accurately assessed. The aim of this study was to describe the prevalence of allopurinol use in a region of New Zealand using community pharmacy dispensing data and to examine the levels of suboptimal adherence in various population groups. Data from all community pharmacy dispensing databases in a New Zealand region were collected for a year covering 2005/2006 giving a near complete picture of dispensings to area residents. Prevalence of allopurinol use in the region by age, sex, ethnicity and socioeconomic position was calculated. Adherence was assessed using the medication possession ratio (MPR), with a MPR of 0.80 indicative of suboptimal adherence. Multiple logistic regression was used to explore variations in suboptimal adherence across population groups. A total of 953 people received allopurinol in the study year (prevalence 3 %). Prevalence was higher in males (6 %) than in females (1 %) and Māori (5 %) than non-Māori (3 %). The overall MPR during the study was 0.88, with 161 (22 %) of patients using allopurinol having suboptimal adherence. Non-Māori were 54 % less likely to have suboptimal allopurinol adherence compared to Māori (95 % CI 0.30–0.72, p = 0.001). These findings are consistent with those from other studies nationally and internationally and point to the important role for health professionals in improving patient adherence to an effective gout treatment.
Similar content being viewed by others
Notes
There were no medicines in ATC category M04AA51 (allopurinol, combinations) dispensed. No other urate-lowering medicine was available in New Zealand during the study period.
References
Brook RA, Forsythe A, Smeeding JE, Lawrence Edwards N (2010) Chronic gout: epidemiology, disease progression, treatment and disease burden. Curr Med Res Opin 26:2813–2821. doi:10.1185/03007995.2010.533647
Smith EUR, Díaz-Torné C, Perez-Ruiz F, March LM (2010) Epidemiology of gout: an update. Best Pract Res Clin Rheumatol 24:811–827. doi:10.1016/j.berh.2010.10.004
Lindsay K, Gow P, Vanderpyl J et al (2011) The experience and impact of living with gout: a study of men with chronic gout using a qualitative grounded theory approach. J Clin Rheumatol 17:1–6. doi:10.1097/RHU.0b013e318204a8f9
Winnard D, Kake T, Gow P et al (2008) Debunking the myths to provide 21st Century management of gout. N Z Med J 121:79–85
Martini N, Bryant L, Te Karu L et al (2012) Living with gout in New Zealand: an exploratory study into people’s knowledge about the disease and its treatment. J Clin Rheumatol 18:125–129. doi:10.1097/RHU.0b013e31824e1f6f
Kleinman NL, Brook RA, Patel PA et al (2007) The impact of gout on work absence and productivity. Value Heal 10:231–237. doi:10.1111/j.1524-4733.2007.00173.x
Winnard D, Wright C, Taylor WJ et al (2012) National prevalence of gout derived from administrative health data in Aotearoa New Zealand. Rheumatology 51:901–909. doi:10.1093/rheumatology/ker361
Jackson G, Wright C, Thornley S et al (2012) Potential unmet need for gout diagnosis and treatment: capture-recapture analysis of a national administrative dataset. Rheumatology 51:1820–1824. doi:10.1093/rheumatology/kes147
Trifirò G, Morabito P, Cavagna L et al (2012) Epidemiology of gout and hyperuricaemia in Italy during the years 2005–2009: a nationwide population-based study. Ann Rheum Dis. doi:10.1136/annrheumdis-2011-201254
Mikuls TR, Saag KG (2006) New insights into gout epidemiology. Curr Opin Rheumatol 18:199–203. doi:10.1097/01.bor.0000209435.89720.7c
Robinson PC, Taylor WJ, Merriman TR (2012) A systematic review of the prevalence of gout and hyperuricemia in Australia. Intern Med J 42:997–1007. doi:10.1111/j.1445-5994.2012.02794.x
Rothenbacher D, Primatesta P, Ferreira A et al (2011) Frequency and risk factors of gout flares in a large population-based cohort of incident gout. Rheumatology 50:973–981. doi:10.1093/rheumatology/keq363
Dalbeth N, So A (2010) Hyperuricaemia and gout: state of the art and future perspectives. Ann Rheum Dis 69:1738–1743. doi:10.1136/ard.2010.136218
Schlesinger N, Dalbeth N, Perez-Ruiz F (2009) Gout–what are the treatment options? Expert Opin Pharmacother 10:1319–1328. doi:10.1517/14656560902950742
Reach G (2011) Treatment adherence in patients with gout. Joint, Bone, Spine 78:456–459. doi:10.1016/j.jbspin.2011.05.010
Briesacher BA, Andrade SE, Fouayzi H, Chan KA (2008) Comparison of drug adherence rates among patients with seven different medical conditions. Pharmacotherapy 28:437–443. doi:10.1592/phco.28.4.437
Solomon DH, Avorn J, Levin R, Brookhart MA (2008) Uric acid lowering therapy: prescribing patterns in a large cohort of older adults. Ann Rheum Dis 67:609–613. doi:10.1136/ard.2007.076182
Harrold LR, Andrade SE, Briesacher BA et al (2009) Adherence with urate-lowering therapies for the treatment of gout. Arthritis Res Ther 11:R46. doi:10.1186/ar2659
Dunbar J, Dunning EJ, Dwyer K (1989) Compliance measurement with arthritis regimen. Arthritis Care Res (Hoboken) 2:A8–A16. doi:10.1002/anr.1790020309
Horsburgh S, Malik M, Norris P et al (2009) Prescribing and dispensing data sources in New Zealand: their usage and future directions. School of Pharmacy, Dunedin
Horsburgh S, Norris P, Becket G et al (2010) The equity in prescription medicines use study: using community pharmacy databases to study medicines utilisation. J Biomed Inform 43:982–987. doi:10.1016/j.jbi.2010.08.004
Statistics New Zealand (2009) QuickStats about Gisborne District. Statistics New Zealand, Wellington
Salmond C, Crampton P, Atkinson J (2007) NZDep2006 index of deprivation. Department of Public Health, University of Otago, Wellington
Statistics New Zealand (2013) Urban/rural profile (experimental) classification categories. http://www.stats.govt.nz/methods/classifications-and-standards/urban-rural-profile-experimental-class-categories.aspx. Accessed 13 Feb 2013
WHO Collaborating Centre for Drug Statistics Methodology (2007) Guidelines for ATC classification and DDD assignment. WHO Collaborating Centre for Drug Statistics Methodology, Oslo
Apotex NZ Ltd (2011) New Zealand data sheet: Apo-Allopurinol. Apotex NZ Ltd, Auckland
Andrade SE, Kahler KH, Frech F, Chan KA (2006) Methods for evaluation of medication adherence and persistence using automated databases. Pharmacoepidemiol Drug Saf 15:565–574; discussion 575–577. doi: 10.1002/pds.1230
Rothman KJ, Greenland S, Lash TL (2008) Modern epidemiology, 3rd edn. Lippincott Williams & Wilkins, Philadelphia
R Core Team (2012) R: a language and environment for statistical computing. R Foundation for Statistical Computing, Vienna
Dalbeth N, House ME, Horne A et al (2012) The experience and impact of gout in Māori and Pacific people: a prospective observational study. Clin Rheumatol. doi:10.1007/s10067-012-2110-5
Harrold LR, Mazor KM, Velten S et al (2010) Patients and providers view gout differently: a qualitative study. Chronic Illn 6:263–271. doi:10.1177/1742395310378761
Spencer K, Carr A, Doherty M (2012) Patient and provider barriers to effective management of gout in general practice: a qualitative study. Ann Rheum Dis 71:1490–1495. doi:10.1136/annrheumdis-2011-200801
Ministry of Social Development (2010) The social report. Ministry of Social Development, Wellington
Jatrana S, Crampton P, Norris P (2011) Ethnic differences in access to prescription medication because of cost in New Zealand. J Epidemiol Community Health 65:454–460. doi:10.1136/jech.2009.099101
Jatrana S, Crampton P (2009) Primary health care in New Zealand: who has access? Health Policy (New York) 93:1–10. doi:10.1016/j.healthpol.2009.05.006
Dalbeth N, Petrie KJ, House M et al (2011) Illness perceptions in patients with gout and the relationship with progression of musculoskeletal disability. Arthritis Care Res (Hoboken) 63:1605–1612. doi:10.1002/acr.20570
Davis A (2012) Geographical access to medicines in Te Tairawhiti. University of Otago
Acknowledgments
This work is based on a study funded by the Health Research Council of New Zealand (Grant Number 07/139). The authors would like to thank the pharmacists and people of Gisborne for their advice and the use of their data, as well as the support of Ngati Porou Hauora and Turanga Health. The authors would also like to acknowledge the Local Advisory Committee to the project for their extremely useful insights and comments.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Horsburgh, S., Norris, P., Becket, G. et al. Allopurinol use in a New Zealand population: prevalence and adherence. Rheumatol Int 34, 963–970 (2014). https://doi.org/10.1007/s00296-013-2935-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-013-2935-5