Abstract
Autoimmune disorders are characterized by the destruction of self-tissues by the immune system. Multiple checkpoints are in place to prevent autoreactivity under normal circumstances. Coexpression of activating and inhibitory Fc receptors (FcR) represents such a checkpoint by establishing a threshold for immune cell activation. In many human autoimmune diseases, however, balanced FcR expression is disturbed. Analysis of murine model systems provides strong evidence that aberrant FcR expression can result in uncontrolled immune responses and the initiation of autoimmune disease. This review will summarize this data and explain how this information might be used to better understand human autoimmune diseases and to develop novel therapeutic strategies.
Similar content being viewed by others
Introduction
Arthritis, multiple sclerosis (MS), autoimmune diabetes, and systemic lupus erythematosus (SLE) are autoimmune diseases that affect millions of people worldwide and require continuous medical attention. Linkage and association studies have established that several genetic and non-genetic factors contribute to the development of disease [1]. The importance of the adaptive and innate arms of the immune system in these processes is highlighted by the fact that immunosuppression is an effective treatment for these diseases [2]. Systemic immune suppression, however, renders the patient more susceptible to infections, and treatment has to be stopped during an acute infection, leading to the reoccurrence of autoimmune symptoms. Thus, more specific approaches to eliminate self-reactive cells might have fewer side effects. Indeed, depletion of B cells has shown promising results for autoimmune diseases such as SLE [2, 3]. Research in mouse models that recapitulate the human disease phenotypes has lead to important insights into the mechanisms that cause an uncontrolled immune response and destruction of self-tissues. A normal immune response is characterized by a delicate balance of activating and inhibitory signals, which will determine the strength of the following response [4]. It must be strong and long lasting enough to eliminate foreign pathogens or malignant cells but controlled and specific enough to avoid damage to non-infected or healthy tissues. Several control mechanisms prevent autoreactive or overwhelming immune responses, and potentially harmful cells can be deleted or inactivated at central or peripheral checkpoints. During early B cell development in the bone marrow, for example, cells expressing self-reactive receptors are eliminated by mechanisms such as receptor editing, deletion, or anergy [5–7]. It is widely accepted, however, that this process is incomplete, and self reactive cells can escape into the periphery; in addition, autoreactive B cells can be generated de novo in the periphery during the germinal center reaction [8, 9]. Therefore, other checkpoints must be in place continuously to prevent the accumulation and activation of autoreactive cells. In particular, B cells that secrete class-switched self-reactive antibodies, which can trigger inflammatory effector functions, have to be tightly regulated [10, 11].
Gene deletion studies in mice have identified the important role of negative regulatory proteins, such as CD5, CD22, CD72, PD-1, CTLA-4, and the inhibitory FcγRIIB (CD32B), which control signals triggered by activating receptors, thus, setting a threshold for immune cell activation. Lack of these proteins results in autoimmune phenotypes and uncontrolled immune responses [12–17]. The hallmark of this protein family is the presence of an immunoreceptor tyrosine-based inhibitory motif (ITIM) [18]. The Fc receptor (FcR) system has become a paradigm for such simultaneous triggering of activating and inhibitory signals, and several proteins of this family have been suggested to be associated with the incidence or severity of human autoimmune disorders, which will be the focus of this review. Besides the FcR family, other players of the innate and adaptive immune system have been associated with autoimmune disorders in mice and humans, which is reviewed elsewhere [19, 20].
Research over the recent years has established that FcRs are central players in several processes that, if not regulated, can lead to the appearance of autoreactive antibodies or autoimmune phenotypes [21, 22]. These range from a failure to delete or prevent the expansion of self-reactive B cells to maintaining dendritic cells (DCs) in an immature and tolerizing state; in addition, the rapid clearance of potential autoantigens such as apoptotic cells by macrophages is important to prevent the initiation of autoimmune processes [23].
A question of balance—coexpression of activating and inhibitory Fc receptors
The family of FcRs is well conserved among different species [11], although the human family is most numerous due to gene duplication and diversification processes [24]. To date, FcRs for all antibody isotypes have been identified. As IgA and IgE FcRs will be discussed elsewhere in this issue, this chapter concentrates on the FcRs for IgG, the FcγRs. Generally, FcRs can be divided into two classes: the activating and the inhibitory FcRs. Most activating receptors cannot signal autonomously and have to associate with additional adaptor molecules to be functional. A notable exception to this rule is the human FcγRIIA, which can transmit activating signals by itself. Therefore, a functional FcR consists of a ligand binding α-domain associated with signaling adaptor molecules containing immunoreceptor tyrosine-based activation motifs (ITAM). Depending on the cell type, the associated signaling adaptor molecules vary. Whereas in the majority of cells, such as monocytes, macrophages, neutrophils, and DCs, FcRs are associated with the common gamma chain (γ-chain); in human natural killer (NK) cells, FcRs are found in combination with the zeta chain (ζ-chain). In addition to the signaling function, these molecules are important for cell-surface expression of the respective α-chains. Animals deficient in the γ-chain lack cell surface expression of all activating FcγRs and several other non-FcR-related proteins such as PIR-A and NK cell cytotoxicity receptors [22, 25]. As expected, these animals demonstrated significant defects in antibody-dependent effector cell responses [26–30]. The inhibitory receptor is a single chain molecule that contains an ITIM in its cytosolic tail [18].
Humans have eight genes that encode Fcγ-receptors (FcγRIA/IB/IC, FcγRIIA/B/C and FcγRIIIA/B) located on chromosome 1. The majority of other species, including the mouse, have four different classes of IgG FcRs that correspond to their human counterparts: FcγRI (CD64), FcγRII (CD32), FcγRIII (CD16), and FcγRIV. FcγRIV is a recently identified receptor with intermediate affinity (107 M−1) and restricted subclass specificity. Based on its sequence similarity, it could be considered the mouse homologue to human FcγRIIIA [31–33]. Whereas FcγRI displays high affinity for the antibody constant region (108–109 M−1), FcγRIIB and FcγRIII have a much lower affinity (∼106 M−1) [34, 35]. The low-affinity Fc-receptor genes are clustered in close proximity to each other in syntenic regions on chromosome 1 in humans, chimpanzees, and mice. In contrast, the high-affinity FcγRI is located on chromosome 3 in mice and chromosome 1 in humans and chimpanzees [11]. This Fcγ-receptor complexity is mirrored by the existence of several IgG isotypes that show differential binding to FcγRs. In the mouse, the high-affinity FcγRI exclusively binds IgG2a, the medium-affinity FcγRIV binds IgG2a and IgG2b, and the low-affinity receptors FcγRIIB and III bind IgG1, IgG2a, and IgG2b [11]. In humans, IgG1 and IgG3 bind better to FcRs than IgG2 or IgG4. However, due to the presence of multiple FcR alleles that influence the antibody–FcR interaction, the situation is more complex [10]. As will be discussed later, some of these alleles show a significant association with autoimmune diseases, which allows to draw some conclusions about the role of antibody–FcR interactions in these disorders.
Establishing the threshold for cell activation: activating and inhibitory Fc-receptor signaling
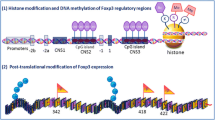
As indicated, activating and inhibitory FcRs are coexpressed on the same cell. Thus, immune complex (IC) binding will result in simultaneous triggering of activating and inhibitory signaling pathways (Fig. 1). Factors that determine whether this coengagement results in cell activation or inhibition are the relative affinities of the antibody isotype to specific FcRs, the expression level of activating and inhibitory Fc-receptors, and the cytokine environment, which can influence their relative expression levels [11]. Moreover, differential antibody glycosylation during an inflammatory response can influence the antibody–FcR interaction and thus regulate antibody activity in mice and humans [36]. Effector responses controlled by these opposing signals most prominently include degranulation of mast cells and neutrophils, release of cytotoxic mediators and inflammatory cytokines by macrophages, antibody dependent cellular cytotoxicity (ADCC), DC activation, phagocytosis, and antigen presentation [22].
Signaling pathways of activating and inhibitory FcRs. a Immune complex triggered crosslinking of activating FcRs induces phosphorylation of the ITAM motif by members of the SRC-kinase family, resulting in activation of downstream signaling events and cell activation. b Simultaneous triggering of the inhibitory FcR interferes with cell activation by recruitment of the phosphatase SHIP and inhibition of activating signaling pathways. The strength of activating versus inhibitory signals triggered by immune complexes is determined by the affinity of individual antibody isotypes to activating and inhibitory FcRs and other factors such as the cytokine environment (see text for details)
Signaling pathways of activating FcRs
The affinity of the majority of activating FcRs for monomeric antibodies is not sufficient for stable binding and induction of signaling. High-affinity receptors, like FcγRI and FcɛRI, can associate with monomeric IgG or IgE antibodies, but activating signals are only triggered upon replacement of bound IgG by ICs (in the case of FcγRI) or upon allergen binding and concomitant crosslinking of cell-surface-bound IgE [37, 38]. Ligands that bind with low affinity cannot trigger sustained receptor aggregation and might even behave as antagonists [39]. FcR aggregation by ICs induces a relocation into cell membrane subdomains called lipid rafts that are enriched in signaling molecules such as SRC-protein kinases (Fig. 1a) [40]. Tyrosine residues in the ITAM motif of the γ-chain then become phosphorylated by SRC kinases, creating SH2 docking sites for the subsequent recruitment of SYK kinases. Depending on cell type and the receptor in question, different members of the SRC-kinase family, such as LYN, HCK, or LCK, are involved in phosphorylation of the γ-chain (Fig. 1a). This enables members of the SYK-kinase family to bind and to recruit and phosphorylate a number of downstream targets including the linker for activation of T cells, multi-molecular adaptor complexes, and members of the BTK and TEC-kinase family [41–43]. Important downstream events triggered by SYK-mediated activation of phosphatidylinositol 3-kinase and phospholipase-Cγ (PLCγ) are sustained calcium release and protein kinase C activation. Moreover, the Ras–Raf–MAPK pathway becomes activated through Sos present in the multimolecular adaptor complex [22, 44].
Inhibitory signaling pathways
Depending on the cell type, alternatively spliced forms of the inhibitory FcR, FcγRIIB, have been described, which have a differential capacity to endocytose bound ICs (termed FcγRIIB-1 and FcγRIIB-2). FcγRIIB-1 is expressed on B cells, whereas the endocytic FcγRIIB-2 shows a myeloid expression pattern [44]. All of these splice forms, however, contain the ITIM motif and trigger inhibitory signaling pathways. On B cells, FcγRIIB regulates activating signals transmitted by the B cell receptor (BCR), whereas on mast cells, neutrophils, or macrophages, it balances activating signals triggered by Fcɛ- or Fcγ-receptors [22, 44]. Upon co-aggregation with its activating counterpart, LYN phosphorylates the ITIM motif, which leads to the recruitment of SHIP (SH2-domain containing inositol 5′ phosphatase). SHIP activation leads to enhanced hydrolysis of phosphatidyl inositol intermediates and thereby interferes with the membrane recruitment of BTK and PLCγ, resulting in inhibition of ITAM-signaling mediated calcium release and downstream effector functions (Fig. 1b) [45, 46]. Moreover, tyrosine-phosphorylated SHIP can bind to Shc and Dok, thereby inhibiting activation of the Ras pathway and ultimately cell proliferation. A third ITIM- and SHIP-independent signaling pathway has been described for crosslinking of FcγRIIB on B cells without concomitant activating signals by the BCR. This leads to B cell apoptosis via Abl-family kinase-dependent pathways [47, 48]. Although the in vivo relevance of this pathway remains to be established, this situation may arise during the germinal center reaction when somatic hypermutation generates BCRs that lose specificity for their cognate antigen retained in the form of ICs on follicular DCs. Thus, FcγRIIB has been suggested to be important for keeping tolerance.
Disturbing the threshold—horror autotoxicus
There are several ways how balanced signaling through activating and inhibitory FcR pairs might be perturbed, ranging from aberrant expression of FcRs to allelic variants of activating receptors that have a differential affinity for certain antibody isotypes [10, 11, 49]. Most of our current knowledge stems from gene deletion studies and autoimmune models in mice and indirect data from human autoimmune patients. Loss or inactivation of FcRs in humans has only been described for the high-affinity FcγRI and FcγRIIIB. Whereas FcγRI deficiency had no apparent impact on health, a significant amount of individuals that lost FcγRIIIB expression had autoimmune disorders [50–53]. As activating and inhibitory FcR pairs are expressed on a variety of cell types, the resulting phenotypes are a complex mixture of impaired responses at several stages throughout the adaptive and innate immune response. The following paragraphs will summarize these phenotypes with respect to the affected cell types and the molecular changes resulting in impaired FcR-dependent responses.
Changing the expression level of the inhibitory receptor on B cells
FcγRIIB, together with other negative regulatory proteins such as CD22 or CD72, regulates activating signals triggered by the BCR, thus setting a threshold for B cell activation [45, 54, 55]. Loss of FcγRIIB was therefore predicted to result in uncontrolled B cell activation. This was confirmed by the generation of FcγRIIB-deficient mice that spontaneously develop a lupus like disease characterized by the production of autoantibodies and premature death due to severe glomerulonephritis [12, 16]. This autoimmune phenotype is strain dependent; mice on the C57BL/6, but not the Balb/c, background develop autoimmune disease, suggesting that other epistatic modifiers are involved in disease susceptibility and severity [56]. Supporting this notion, Balb/c mice, double deficient in programmed death 1 (PD-1) and FcγRIIB, developed autoimmune hydronephrosis, whereas mice that were only deficient in one of these inhibitory proteins did not [57]. Moreover, Balb/c FcγRIIB-knockout mice showed enhanced disease phenotypes in a model of pristane-induced lupus [58]. In addition, Balb/c mice have been suggested to be more efficient in silencing autoreactive heavy chains by receptor editing than C57Bl/6 mice, making the latter strain more permissive for the development of autoimmunity [59, 60].
Although genetic deletion of FcγRIIB results in loss of inhibitory signaling on a variety of cell types, there is evidence that the appearance of autoantibodies is a B cell autonomous phenomenon. Autoimmune-prone mouse strains such as NZB, NOD, BXSB, and MRL express reduced levels of FcγRIIB on activated and germinal-center B cells due to a polymorphism in the FcγRIIB promoter [61–64]. Moreover, FcγRIIB bone marrow chimeras expressing normal levels of the inhibitory receptor on radiation-resistant cells but lacking FcγRIIB on B cells develop autoantibodies and disease [12]. Another important issue is to understand at which stage(s) of B cell development FcγRIIB regulates tolerance. As indicated, autoreactive B cells can be generated throughout B cell development [6]. There is accumulating evidence that FcγRIIB mediates its function during late stages of B cell maturation in mice and humans, thus representing a distal checkpoint [59, 65, 66]. By using a mouse strain in which the endogenous Ig locus has been replaced with an autoreactive heavy chain, it was shown that the absence of FcγRIIB resulted in the accumulation of IgG-positive, autoreactive plasma cells [59]. FcγRIIB deficiency did neither impact early events in the bone marrow such as receptor editing nor did it prevent the development of IgM-positive, autoreactive B cells. After class switching to IgG, however, FcγRIIB was essential in preventing the expansion of autoreactive B cells and their maturation into plasma cells. Taking the considerably higher pathogenic potential of IgG compared to the IgM antibody isotypes into account, this relatively late stage of FcγRIIB-mediated negative regulation might be sufficient to prevent the initiation of severe autoreactive processes. Thus, FcγRIIB might serve as the final barrier to control class-switched, autoreactive B cells that would otherwise induce tissue pathology by secretion of large amounts of pathogenic antibodies.
The most important question is whether these data obtained in murine model systems help to explain the development of human autoimmune disease. Analysis of human autoimmune patient cohorts indicates that this is the case, and that some of the underlying mechanisms of aberrant FcγRIIB expression are quite similar in humans and mice. For instance, polymorphisms in the human FcγRIIB promoter have been linked to the development of SLE [65, 67, 68]. The strongest association was found with a polymorphism that leads to a decreased binding of the transcription factor AP-1, resulting in a reduced surface expression of FcγRIIB on activated B cells of human lupus patients [65]. Another study showed that memory B cells of SLE patients failed to upregulate FcγRIIB expression on memory B cells, and this lower expression level was correlated with a reduced threshold for B cell activation [66] consistent with a previous study describing that B cells from lupus patients showed enhanced triggering of activating signaling pathways after BCR stimulation [69]. Such quantitative assessments of FcγRIIB expression have been complicated until the recent development of a novel antibody specific for the human inhibitory FcγRIIB [70]. It will be of interest to determine what the mechanism of this aberrant expression is and if any of the known FcγRIIB polymorphisms are involved in this phenotype. The results of these studies fit to the data obtained in murine model systems identifying FcγRIIB as a checkpoint during late stages of B cell development. Moreover, an allelic variant of FcγRIIB has been associated with human SLE and arthritis in several Asian populations (Table 1) [71–74]. In this allele, the exchange of a non-polar isoleucine residue in the transmembrane domain (amino acid 232) for a threonine results in an impaired recruitment to lipid rafts and thus exclusion from productive signaling [75–77]. This represents a novel mechanism of impaired FcγRIIB function and is unique to humans. There are, however, great disparities between different human populations and ethnicities highlighting the importance of the genetic background and other susceptibility factors for the development of autoimmune disease (Table 1). Thus, although several studies found clear associations between SLE and the FcγRIIB-I232T allele in Asian patients, Caucasians did not show this association [74]. In the latter group, aberrant transcription due to promoter polymorphisms was found more consistently [65, 74]. Similarly, the decreased expression of FcγRIIB on memory cells of SLE patients was overrepresented in the African–American population [66].
FcγRIIB as a regulator of DC activity
DCs have long been recognized as central mediators that, depending on their activation state, determine whether an adaptive immune response or tolerance is induced [78]. Several groups have shown that crosslinking of FcRs on DCs by ICs results in cell activation and cross-presentation of endocytosed antigen on MHC class I molecules to CD8+ cytotoxic T cells [79–82]. As low levels of ICs are constantly present in the serum, FcγRIIB might be crucial in preventing spontaneous activation of DCs. Indeed, blocking FcγRIIB on human DCs was sufficient to induce DC maturation by serum ICs. Besides up-regulation of costimulatory molecules, these DCs were more potent in generating and activating antigen specific T cells [70, 83], as described before for mouse DCs deficient in FcγRIIB expression [84]. Although beneficial for immunotherapeutic or vaccination approaches, this suggests that a slight deregulation of FcγRIIB expression might result in the initiation of autoreactive processes. It will be of great interest to determine if FcR-mediated uptake of ICs containing autoantigens by DCs plays a role in autoimmune diseases that depend on the priming of autoreactive T cells. In addition, expression of the inhibitory receptor on DCs present in epithelia has been implicated in establishing tolerance to air-borne and food allergens [85].
Whereas the essential role of DCs in regulating T cell responses is well accepted, it has only recently become clear that DCs are also important for the B cell response [86–88]. Unlike in macrophages, which rapidly degrade phagocytosed material, antigen taken up by DCs is degraded more slowly and therefore present in an intact form for prolonged times [89]. This might allow antigen transport from the periphery to lymphoid organs where it can be presented to B cells. DC–B cell interactions have been observed in vivo, and it has been suggested that this interaction is important for the generation of an IgG response in vitro and in vivo [88]. The role of FcγRIIB in this process is that ICs taken up via FcγRIIB are inefficiently degraded and recycled for cell surface presentation to B cells. In contrast, uptake via FcγRIII results in a faster degradation of the antigen [86]. The importance of this novel function of FcγRIIB for human or murine autoimmune diseases remains to be established.
The role of FcγRIIB in the efferent response: controlling innate immune effector cell activation
Besides its regulatory role on B cells and DCs in the afferent response, FcγRIIB is an important modulator of inflammatory effector cells, such as mast cells, neutrophils, and macrophages, during the efferent phase of an immune response [22]. On these cell types, FcγRIIB is coexpressed with activating FcRs of varying affinities and isotype specificities and negatively regulates signals delivered by these receptors. Lack of FcγRIIB leads to elevated IC-mediated inflammation and phagocytosis, as demonstrated by an enhanced Arthus reaction, systemic anaphylaxis, anti-GBM glomerulonephritis, immunothrombocytopenia (ITP), hemolytic anemia, collagen-induced arthritis, and IgG-mediated clearance of pathogens and tumor cells [11, 21]. On allergic effector cells such as mast cells and basophils, FcγRIIB regulates activating signals triggered by crosslinking FcɛRI, resulting in an enhanced IgE-mediated anaphylaxis and heightened sensitivity to allergic rhinitis [90]. Moreover, FcγRIIB deficiency renders otherwise resistant mouse strains susceptible to development of certain forms of collagen induced arthritis [91]. As described for human autoimmune disease in some of these models both increased autoantibody production due to FcγRIIB deficiency on B cells and heightened effector cell responses are likely to contribute to the observed phenotype.
Another long known observation is that IgG2a and IgG2b antibodies trigger stronger effector responses than IgG1 or IgG3 in passive antibody transfer models [92–100]. Similarly, in highly pathogenic autoimmune models such as the accelerated nephrotoxic nephritis (NTN) model, the pathogenic autoantibodies are of the IgG2b isotype [101]. In human SLE patients, IgG1, IgG3, and to a lesser extent IgG2 anti-DNA antibodies dominate in the serum, whereas all subclasses can be found in kidney biopsies [102–105].
The molecular mechanism of differential antibody isotype activity was addressed recently [97]. It was shown that the differences in affinity of different IgG isotypes for activating and inhibitory FcRs might explain this phenomenon [33, 97]. By measuring the affinities of all antibody isotypes for the various FcRs and dividing the affinities of antibody isotypes for activating FcRs by the affinity for the inhibitory receptor a so-called A/I ratio was established which predicted antibody activity in vivo [11, 97]. Thus, IgG1 (which only binds to the FcγRIII/FcγRIIB pair) has a lower affinity for the activating than for the inhibitory FcR (A/I-ratio ≪1) resulting in lower activity. In contrast, IgG2a and IgG2b have 20- to 40-fold higher affinity for the activating FcγRIV than for FcγRIII/FcγRIIB, which results in preferential triggering of FcγRIV and a lower degree of negative regulation by the inhibitory FcR. As will be discussed below, other factors such as cytokines or differential antibody glycosylation can affect this ratio. In humans, the presence of different activating FcR alleles that have differential affinities for certain human antibody isotypes might result in a similar situation, thus changing the A/I ratio and antibody activity.
The activating FcRs in the efferent response
In contrast to the inhibitory FcγRIIB, expression of activating FcRs is limited to DCs and innate immune effector cells such as mast cells, basophils, monocytes, macrophages, neutrophils, and NK cells. There is considerable heterogeneity in the expression of specific activating FcRs. In the mouse, macrophages express all activating FcRs (I, III, and IV), DCs mainly express FcγRI and III, neutrophils express FcγRIII and IV, and NK cells express FcγRIII. Genetic inactivation of all activating FcRs by deletion of the common γ-chain in mice results in abrogated or heavily impaired IC or allergen-mediated responses, such as ADCC, release of inflammatory mediators, cytokine release, and phagocytosis of ICs [11, 29]. As several activating FcRs are coexpressed on the same cell, subsequent deletion of the individual ligand-binding α-chains was crucial in elucidating the role of the individual FcRs for the activity of different antibody isotypes. Identifying the receptor and cell type responsible for tissue pathology in autoimmune diseases might allow the development of more specific therapeutic interventions. Consistent with its in vitro isotype binding profile, activating FcγRIII was essential for IgG1-mediated effector functions in a variety of models, like arthritis, glomerulonephritis, IgG-dependent anaphylaxis, IgG-mediated hemolytic anemia, and ITP [33, 93, 97, 106–110].
In contrast, IgG2b activity was not impaired in FcγRIII or FcγRI knockout mice but was almost completely abrogated in mice injected with an FcγRIV blocking antibody in passive and active models of antibody-mediated inflammation, including models of ITP and NTN [93, 94, 97, 101]. In the NTN model, mice were injected with a sheep hyperimmune serum specific for murine glomerular basement membranes (GBM). To enhance disease development, mice were pre-immunized with sheep serum, which resulted in an IgG2b-dominated antibody response [101]. After injection of the sheep anti-GBM serum, many animals died within 8–10 days due to severe inflammation and kidney failure. In the presence of an FcγRIV-blocking antibody, however, animals did not develop fatal glomerulonephritis. Despite C3 deposition in the kidneys, the observed pathology was fully dependent on activating FcRs as observed before [26, 28, 111–113]. This suggests that identification and blocking of the responsible activating FcRs in human autoimmune disease might be a promising therapeutic intervention.
Similar to IgG2b, IgG2a antibody activity was greatly impaired in mice with blocked FcγRIV activity in models of antibody-mediated clearance of platelets, B cells, or tumor cells, and neither deficiency in members of the complement cascade nor in FcγRI or III had a significant effect on antibody activity [94, 97, 100]. Depending on the model system, the amount of ICs and effector cell type, FcγRI and FcγRIII variably contributed to IgG2a activity [93, 114–116]. For example, in a model of autoimmune hemolytic anemia (AIHA) that—in contrast to the ITP model—requires higher antibody doses and several days for developing a maximal response, FcγRIII was significantly involved in mediating IgG2a activity [93]; in addition, the complement component C3 enhanced IgG2b and IgG3 activity [117]. Regarding the role of FcγRIII in this model, it was recently demonstrated that C5a, a strong inflammatory mediator, induces upregulation of FcγRIII, which is important for the development of AIHA [118, 119]. Further, generation of C5a occurred independently of the classical and alternative complement pathways and was triggered in an FcR-dependent fashion [118]. Moreover, it was suggested that Kupffer cells in the liver are the main effector cell type that mediates red blood cell phagocytosis, and it is not known if FcγRIV is expressed on these cells. Taken together, this demonstrates the influence of the effector cell type and the cytokine milieu on the cellular FcR expression pattern, which will be discussed in greater detail later.
In humans, low-affinity FcγRs bind better to IgG1 and IgG3 than to IgG2 or IgG4. However, certain FcγRIIA and IIIA alleles show increased binding to human antibody isotypes [10]. For instance, the FcγRIIA131H allele binds IgG2 approximately tenfold better than FcγRIIA with arginine at that position (FcγRIIA131R). Similarly, human FcγRIIIA158V has a higher affinity for IgG1 and IgG3 than its 158F counterpart [10]. This selectively higher affinity of the activating FcR increases the A/I ratio and predicts that cytotoxic antibodies show a higher activity in such individuals. Indeed, cancer patients with the FcγRIIIA158V allele responded better to antibody therapy [120–122]. In autoimmune patients, the FcγRIIIA158V allele was linked to more severe arthritis in Caucasians [123, 124]. In the majority of studies, however, the low-affinity alleles have been identified as risk factors for the development or severity of autoimmune disease. Several studies have found an association of the low-affinity FcγRIIIA158F and the FcγRIIA131R alleles with the incidence and severity of lupus nephritis and arthritis [71, 125–137]. In addition, the low-affinity allele of human FcγRIIIB (FcγRIIIB-NA2) has been associated with SLE [71, 138, 139]. Alternatively, a low-copy-number polymorphism of this gene was associated with glomerulonephritis in humans and rats [140]. The results of these various studies suggested a model in which FcRs on macrophages or neutrophils might be involved in clearance of ICs containing potential autoantigens under non-inflammatory conditions, thereby preventing the initiation of autoimmune responses. Data from other model systems indicate that inefficient or delayed clearance of apoptotic cells can lead to the loss of tolerance and is associated with autoimmune diseases such as SLE [23, 141–143].
As described for FcγRIIB, a strong heterogeneity exists between different ethnicities and populations. For example, studies in African–American, Brazilian, German, and Thai populations have found significant associations between the FcγRIIA131R allele and SLE disease susceptibility or severity of nephritis [71, 126, 128, 129, 131, 133, 136, 137, 144]. Moreover, several studies in Caucasian, Dutch, and Korean populations have found associations between the FcγRIIIA158F allele and disease susceptibility and severity [127, 130, 134, 145]. In addition, some studies have found a connection between the FcγRIIIB-NA2 allele and SLE in Thai, Spanish, and Japanese populations [71, 138, 139]. In contrast, the FcγRIIA131R allele was not increased in SLE or nephritis in African–Caribean, British, Dutch, Greek, Hispanic, Korean, and Spanish populations [127, 130, 134, 139, 145–149]. Similarly, studies in Chinese, German, and African–American populations have found no associations between the FcγRIIIA158F and the FcγRIIIB-NA2 allele [71, 127, 131, 138, 144, 150, 151].
Exogenous factors modulating the balance—cytokines and sugar
Several studies have addressed the impact of cytokines on Fc-receptor expression. Frequently, cytokines regulate expression of the associated signaling adaptors (β- and γ-chains), which leads to a concomitant change in α-chain expression, as shown for transforming growth factor β (TGF-β), IL-4, and IL-10 [152, 153]. Moreover, inflammatory cytokines/mediators such as TNF-α, C5a, or LPS tend to upregulate activating receptors such as Fcα-, Fcɛ-, and Fcγ-receptors, whereas TH-2 cytokines such as TGF-β, IL-4, and IL-10 seem to decrease expression [33, 153, 154]. These effects can be cell-type specific as IL-4 upregulates the inhibitory FcγRIIB on myeloid cells but has the opposite effect on activated B cells [155].
The outcome of cytokine-mediated changes in activating and inhibitory expression might vary depending on the differential regulation of IgG isotypes by the inhibitory FcR. Thus, IgG2a and, to a lesser degree, IgG2b antibodies might be insensitive to elevated FcγRIIB expression relative to the severe impairment of IgG1 activity. During antibody-mediated inflammation, however, the steady state ratios change in favor of the activating FcRs, as the release of inflammatory mediators, such as IFN-γ and C5a, can upregulate activating Fcγ-receptors and at the same time reduces FcγRIIB expression levels [156, 157]. Under these circumstances, autoreactive IgG1 antibodies are capable of triggering severe damage. In fact, the regulation of FcR expression by cytokines is coupled to the regulation of isotypes by these same cytokines: TH-1 cytokines such as IFN-γ induce class switching to IgG2a, TH-2-type cytokines (IL-4) induce class switching to IgG1, and TGF-β induces switching to IgG2b [158, 159]. As these cytokines also influence Fc-receptor expression, the pathogenicity of an autoimmune response will be determined by both cytokine-mediated regulation of class switching and the changes in expression levels of the responsible activating versus inhibitory FcRs. This dual regulation might allow the development of new therapeutic strategies to treat autoimmune disease.
Another factor that can influence the interaction of antibodies with cellular FcRs is the sugar moiety attached to the asparagine residue at position 297 in the antibody Fc-fragment. Deletion of this sugar side-chain results in loss of FcR binding [160]. In addition, this core sugar structure contains variable amounts of branching and terminal sugar residues such as N-acetylglucosamine, fucose, galactose, and sialic acid. Presence or absence of these terminal or branching sugar residues can significantly influence antibody–FcR interactions. Thus, antibodies without fucose bind approximately tenfold stronger to mouse-activating FcγRIV and human FcγRIIIA [161–163]. In contrast, high levels of terminal sialic acid residues impair antibody binding to FcRs [36], and there is evidence that antibody sialylation levels differ during an immune response. Antibodies from human arthritis patients and autoimmune mouse strains such as MRL/lpr have reduced amounts of terminal sialic acid and galactose and were found to be more pathogenic [164–167]. Similarly, murine serum IgG antibodies have reduced amounts of sialic acid after induction of nephrotoxic nephritis [36]. Taken together, these studies indicate that antibody sialylation represents another mechanism-regulating antibody activity, and manipulating antibody sialylation levels in vivo might be a promising strategy to decrease autoantibody-associated pathogenicity.
Regaining the balance—therapeutic interventions that modulate FcR expression
The most important question is how this information might be used to develop strategies that restore a balanced immune response and stop autoimmune processes. Regarding the lower expression level or functional impairment of the inhibitory receptor on B cells in SLE, one approach would be to restore FcγRIIB expression by gene transfer. This approach was recently tested in autoimmune prone mouse strains like NZM, BXSB, and FcγRIIB-knockout mice [168]. These animals had strongly reduced levels of autoantibodies and did not develop glomerulonephritis. Highlighting the threshold nature of autoimmunity, restoration of FcγRIIB expression on approximately 40% of peripheral B cells was sufficient to prevent the development of autoantibodies and autoimmune disease [22, 168].
Instead of gene transfer, one could manipulate the expression level of activating and inhibitory receptors with anti-inflammatory drugs. The successful use of high-dose intravenous gamma globulin (IVIG) for the treatment of several autoimmune diseases provides an excellent example of the validity of this approach.
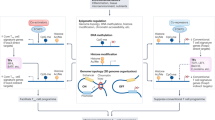
Currently, IVIG is used to alleviate autoimmune symptoms in SLE, Kawaski disease, and MS [169]. IVIG consists of the pooled serum IgG fraction of thousands of human donors and has to be given at high doses to obtain its beneficial anti-inflammatory activity. Immunotherapeutic studies in mice and humans have shown that the Fc portion of IVIG antibodies is responsible for its activity [101, 106, 170, 171]. Although several mechanisms of IVIG action have been proposed [169], mounting evidence suggests that the inhibitory FcγRIIB is essential for the anti-inflammatory activity of IVIG. In mouse models of ITP, rheumatoid arthritis, and nephrotoxic nephritis, IVIG administration blocked autoantibody-mediated inflammation; this protective effect was abolished in mice deficient in the inhibitory FcγRIIB [101, 106, 171]. More importantly, IVIG upregulated FcγRIIB expression on effector macrophages, resulting in a heightened threshold for cell activation. In addition, IVIG induced a significant reduction of the triggering activating FcγRIV in the NTN model, thus strongly modulating the balance of activating and inhibitory receptors [101]. As FcγRIIB upregulation was absent in mice lacking CSF-1-dependent macrophages, a two-cell model was suggested in which IVIG binds to CSF-1-dependent macrophages, resulting in upregulation of FcγRIIB on effector macrophages (Fig. 2) [106].
Factors that influence FcR-dependent effector cell activation. Factors that shift the balance towards cell activation or inhibition are shown in green or red, respectively. Inflammatory cytokines/mediators such as IFN-γ, LPS or C5a upregulate activating FcRs (shown in green) resulting in a lower threshold for cell activation. In addition, allelic variants of activating and inhibitory receptors that influence antibody binding or FcR function might have similar effects. A higher threshold for cell activation is induced by anti-inflammatory cytokines or therapeutics such as IVIG that upregulate the inhibitory FcγRIIB (shown in red). In addition, activating FcR alleles with low affinity for antibody isotypes will trigger activating signaling pathways less efficiently. Moreover, the composition of ICs with respect to antibody isotype and antibody glycosylation pattern determines if activating or inhibitory signals will dominate
A longstanding question was why such high doses of IVIG were required to achieve its therapeutic effects. One possibility was that the actual active component is only a minor fraction of the total IVIG preparation. Indeed, each of the four IgG isotypes in the IVIG preparation contains differentially glycosylated sugar moieties attached to the Fc region resulting in considerable heterogeneity. Recently, it was shown that the sialic-acid-rich IgG fraction in the IVIG preparation might be the active component. By using the sialic-acid-rich IVIG Fc portion, the therapeutic dose of IVIG could be reduced by a factor of 10 [36]. Other proteins like fetuin or transferrin that contain similar sialic-acid-rich sugar side chains did not recapitulate the anti-inflammatory activity, indicating that the amino acid backbone of the antibody Fc portion was required, too. Together with the previous observations, this suggests a model in which sialic-acid-rich IVIG binds to a receptor on CSF-1-dependent macrophages that indirectly induces the modulation of activating and inhibitory FcRs on effector macrophages (Fig. 2). As sialic-acid-rich antibodies bind FcRs with reduced affinity, the cell surface receptor responsible for this anti-inflammatory effect is most likely not a conventional FcR [36]. Thus, the identification and selective triggering of this putative IVIG receptor might enhance the anti-inflammatory activity of IVIG.
In addition, TH-2 cytokines such as IL-4 that induce FcγRIIB upregulation and downregulate activating FcRs might have therapeutic value. Along these lines, adoptive transfer of DCs engineered to produce high levels of IL-4 blocked active arthritis in mice [172, 173]. Besides modifying FcR expression levels, this would also skew the antibody response to IgG1 rather than IgG2a and IgG2b, resulting in a more strict regulation by the inhibitory receptor. Moreover, IL-4 inhibits the TH-1 cytokines, IL-2 and IFN-γ, suppressing inflammatory macrophage activation.
Whereas these previous approaches predominantly interfere with the effector phase of an autoimmune response, an alternative strategy would target DCs and thus block the initiation phase. Elegant work by the groups of Steinman and Nussenzweig [78] suggests that targeting antigens to immature DCs in vivo results in the induction of tolerance. Antigen targeting is achieved by genetic fusion to a DEC-205 specific antibody that selectively recognizes DCs. To prevent activation of DCs by crosslinking activating FcRs, this antibody contains a mutation that abrogates FcR binding. With the current development of antibodies with preferential binding to activating or inhibitory FcRs, one could generate a DEC-205 antibody that specifically engages FcγRIIB to deliver a strong tolerogenic signal and block the priming of autoreactive cells.
Conclusions
Research over the recent years has provided important insights into the regulation of cell activation by cellular FcRs. Disturbing the threshold set by coexpression of activating and inhibitory FcRs results in an uncontrolled immune response ultimately leading to the loss of tolerance and the initiation of autoimmune pathology. The inhibitory FcγRIIB represents a distal checkpoint during B cell development and regulates the expansion of autoreactive memory or plasma cells in mice and humans. In addition, it controls the activation of innate immune effector cells including neutrophils, mast cells, and macrophages. Restoring FcγRIIB expression might be a promising strategy to interfere with self-destructive processes both in the initiation and effector phase of an autoimmune response. Despite disparate results between different human populations, the analysis of autoimmune patients has demonstrated that low-affinity allelic variants of activating FcRs are frequently associated with the severity or incidence of autoimmune diseases, suggesting that impaired removal of ICs by FcRs contributes to disease development. Finally, the antibody–FcR interaction is significantly influenced by the antibody glycosylation pattern. Autoimmune patients and mice with active autoimmune disease have antibodies with a lower level of terminal galactose and sialic acid, which enhances the interaction with cellular FcRs. Thus, influencing antibody glycosylation might be another strategy to interfere with autoimmune pathology.
References
Tsao BP (2003) The genetics of human systemic lupus erythematosus. Trends Immunol 24:595–602
Bussel J (2006) Treatment of immune thrombocytopenic purpura in adults. Semin Hematol 43:S3–S10 (discussion S18–S19)
Martin F, Chan AC (2006) B cell immunobiology in disease: evolving concepts from the clinic. Annu Rev Immunol 24:467–496
Lanier LL (2001) Face off—the interplay between activating and inhibitory immune receptors. Curr Opin Immunol 13:326–331
Goodnow CC, Sprent J, de St Groth BF, Vinuesa CG (2005) Cellular and genetic mechanisms of self tolerance and autoimmunity. Nature 435:590–597
Grimaldi CM, Hicks R, Diamond B (2005) B cell selection and susceptibility to autoimmunity. J Immunol 174:1775–1781
Meffre E, Casellas R, Nussenzweig MC (2000) Antibody regulation of B cell development. Nat Immunol 1:379–385
Bona CA, Stevenson FK (2004) B cells producing pathogenic autoantibodies. In: Honjo T, Alt FW, Neuberger MS (eds) Molecular biology of B cells. Elsevier, Boston, pp 381–402
Ray SK, Putterman C, Diamond B (1996) Pathogenic autoantibodies are routinely generated during the response to foreign antigen: a paradigm for autoimmune disease. Proc Natl Acad Sci USA 93:2019–2024
Dijstelbloem HM, van de Winkel JG, Kallenberg CG (2001) Inflammation in autoimmunity: receptors for IgG revisited. Trends Immunol 22:510–516
Nimmerjahn F, Ravetch JV (2006) Fcgamma receptors: old friends and new family members. Immunity 24:19–28
Bolland S, Ravetch JV (2000) Spontaneous autoimmune disease in Fc(gamma)RIIB-deficient mice results from strain-specific epistasis. Immunity 13:277–285
Nishimura H, Nose M, Hiai H, Minato N, Honjo T (1999) Development of lupus-like autoimmune diseases by disruption of the PD-1 gene encoding an ITIM motif-carrying immunoreceptor. Immunity 11:141–151
O’Keefe TL, Williams GT, Batista FD, Neuberger MS (1999) Deficiency in CD22, a B cell-specific inhibitory receptor, is sufficient to predispose to development of high affinity autoantibodies. J Exp Med 189:1307–1313
Penninger JM, Timms E, Shahinian A, Jezo-Bremond A, Nishina H, Ionescu J, Hedrick SM, Mak TW (1995) Alloreactive gamma delta thymocytes utilize distinct costimulatory signals from peripheral T cells. J Immunol 155:3847–3855
Takai T, Ono M, Hikida M, Ohmori H, Ravetch JV (1996) Augmented humoral and anaphylactic responses in Fc gamma RII-deficient mice. Nature 379:346–349
Tivol EA, Borriello F, Schweitzer AN, Lynch WP, Bluestone JA, Sharpe AH, Penninger JM, Timms E, Shahinian A, Jezo-Bremond A, Nishina H, Ionescu J, Hedrick SM, Mak TW (1995) Loss of CTLA-4 leads to massive lymphoproliferation and fatal multiorgan tissue destruction, revealing a critical negative regulatory role of CTLA-4. Immunity 3:541–547
Ravetch JV, Lanier LL (2000) Immune inhibitory receptors. Science 290:84–89
Carroll MC (2004) The complement system in regulation of adaptive immunity. Nat Immunol 5:981–986
Nguyen C, Limaye N, Wakeland EK (2002) Susceptibility genes in the pathogenesis of murine lupus. Arthritis Res 4:S255–S263 (Epub 2002 May 9)
Takai T (2002) Roles of Fc receptors in autoimmunity. Nat Rev Immunol 2:580–592
Ravetch JV (2003) Fc receptors. In: Paul WE (ed) Fundamental immunology. Lippincott-Raven, Philadelphia, pp 685–700
Hanayama R, Tanaka M, Miyasaka K, Aozasa K, Koike M, Uchiyama Y, Nagata S (2004) Autoimmune disease and impaired uptake of apoptotic cells in MFG-E8-deficient mice. Science 304:1147–1150
Qiu WQ, de Bruin D, Brownstein BH, Pearse R, Ravetch JV (1990) Organization of the human and mouse low-affinity Fc gamma R genes: duplication and recombination. Science 248:732–735
Moretta A, Bottino C, Vitale M, Pende D, Cantoni C, Mingari MC, Biassoni R, Moretta L (2001) Activating receptors and coreceptors involved in human natural killer cell-mediated cytolysis. Annu Rev Immunol 19:197–223
Clynes R, Ravetch JV (1995) Cytotoxic antibodies trigger inflammation through Fc receptors. Immunity 3:21–26
Park SY, Ueda S, Ohno H, Hamano Y, Tanaka M, Shiratori T, Yamazaki T, Arase H, Arase N, Karasawa A, Sato S, Ledermann B, Kondo Y, Okumura K, Ra C, Saito T (1998) Resistance of Fc receptor- deficient mice to fatal glomerulonephritis. J Clin Invest 102:1229–1238
Sylvestre DL, Ravetch JV (1994) Fc receptors initiate the Arthus reaction: redefining the inflammatory cascade. Science 265:1095–1098
Takai T, Li M, Sylvestre D, Clynes R, Ravetch JV (1994) FcR gamma chain deletion results in pleiotrophic effector cell defects. Cell 76:519–529
Zhang M, Zhang Z, Garmestani K, Goldman CK, Ravetch JV, Brechbiel MW, Carrasquillo JA, Waldmann TA (2004) Activating Fc receptors are required for antitumor efficacy of the antibodies directed toward CD25 in a murine model of adult t-cell leukemia. Cancer Res 64:5825–5829
Davis RS, Dennis G Jr, Odom MR, Gibson AW, Kimberly RP, Burrows PD, Cooper MD (2002) Fc receptor homologs: newest members of a remarkably diverse Fc receptor gene family. Immunol Rev 190:123–136
Mechetina LV, Najakshin AM, Alabyev BY, Chikaev NA, Taranin AV (2002) Identification of CD16-2, a novel mouse receptor homologous to CD16/Fc gamma RIII. Immunogenetics 54:463–468 (Epub 2002 Aug 02)
Nimmerjahn F, Bruhns P, Horiuchi K, Ravetch JV (2005) FcgammaRIV: a novel FcR with distinct IgG subclass specificity. Immunity 23:41–51
Hulett MD, Hogarth PM (1994) Molecular basis of Fc receptor function. Adv Immunol 57:1–127
Ravetch JV, Kinet JP (1991) Fc receptors. Annu Rev Immunol 9:457–492
Kaneko Y, Nimmerjahn F, Ravetch JV (2006) Anti-inflammatory activity of immunoglobulin G resulting from Fc sialylation. Science 313:670–673
Galli SJ, Kalesnikoff J, Grimbaldeston MA, Piliponsky AM, Williams CM, Tsai M (2005) Mast cells as “tunable” effector and immunoregulatory cells: recent advances. Annu Rev Immunol 23:749–786
Gould HJ, Sutton BJ, Beavil AJ, Beavil RL, McCloskey N, Coker HA, Fear D, Smurthwaite L (2003) The biology of IGE and the basis of allergic disease. Annu Rev Immunol 21:579–628
Torigoe C, Inman JK, Metzger H (1998) An unusual mechanism for ligand antagonism. Science 281:568–572
Lang ML, Shen L, Wade WF (1999) Gamma-chain dependent recruitment of tyrosine kinases to membrane rafts by the human IgA receptor Fc alpha R. J Immunol 163:5391–5398
Gulle H, Samstag A, Eibl MM, Wolf HM (1998) Physical and functional association of Fc alpha R with protein tyrosine kinase Lyn. Blood 91:383–391
Launay P, Grossetete B, Arcos-Fajardo M, Gaudin E, Torres SP, Beaudoin L, Patey-Mariaud de Serre N, Lehuen A, Monteiro RC (2000) Fcalpha receptor (CD89) mediates the development of immunoglobulin A (IgA) nephropathy (Berger’s disease). Evidence for pathogenic soluble receptor-Iga complexes in patients and CD89 transgenic mice. J Exp Med 191:1999–2009
Park RK, Izadi KD, Deo YM, Durden DL (1999) Role of Src in the modulation of multiple adaptor proteins in FcalphaRI oxidant signaling. Blood 94:2112–2120
Daeron M (1997) Fc receptor biology. Annu Rev Immunol 15:203–234
Bolland S, Ravetch JV (1999) Inhibitory pathways triggered by ITIM-containing receptors. Adv Immunol 72:149–177
Daeron M, Lesourne R (2006) Negative signaling in Fc receptor complexes. Adv Immunol 89:39–86
Pearse RN, Kawabe T, Bolland S, Guinamard R, Kurosaki T, Ravetch JV (1999) SHIP recruitment attenuates Fc gamma RIIB-induced B cell apoptosis. Immunity 10:753–760
Tzeng SJ, Bolland S, Inabe K, Kurosaki T, Pierce SK (2005) The B cell inhibitory Fc receptor triggers apoptosis by a novel c-Abl-family kinase dependent pathway. J Biol Chem 22:22
Wijngaarden S, van de Winkel JG, Jacobs KM, Bijlsma JW, Lafeber FP, van Roon JA (2004) A shift in the balance of inhibitory and activating Fcgamma receptors on monocytes toward the inhibitory Fcgamma receptor IIb is associated with prevention of monocyte activation in rheumatoid arthritis. Arthritis Rheum 50:3878–3887
de Haas M, Kleijer M, van Zwieten R, Roos D, von dem Borne AE (1995) Neutrophil Fc gamma RIIIb deficiency, nature, and clinical consequences: a study of 21 individuals from 14 families. Blood 86:2403–2413
Clark MR, Liu L, Clarkson SB, Ory PA, Goldstein IM (1990) An abnormality of the gene that encodes neutrophil Fc receptor III in a patient with systemic lupus erythematosus. J Clin Invest 86:341–346
Huizinga TW, Kuijpers RW, Kleijer M, Schulpen TW, Cuypers HT, Roos D, von dem Borne AE (1990) Maternal genomic neutrophil FcRIII deficiency leading to neonatal isoimmune neutropenia. Blood 76:1927–1932
van de Winkel JG, de Wit TP, Ernst LK, Capel PJ, Ceuppens JL (1995) Molecular basis for a familial defect in phagocyte expression of IgG receptor I (CD64). J Immunol 154:2896–2903
Nitschke L, Tsubata T (2004) Molecular interactions regulate BCR signal inhibition by CD22 and CD72. Trends Immunol 25:543–550
Ravetch JV, Bolland S (2001) IgG Fc receptors. Annu Rev Immunol 19:275–290
Bolland S, Yim YS, Tus K, Wakeland EK, Ravetch JV (2002) Genetic modifiers of systemic lupus erythematosus in FcgammaRIIB(−/−) mice. J Exp Med 195:1167–1174
Okazaki T, Otaka Y, Wang J, Hiai H, Takai T, Ravetch JV, Honjo T (2005) Hydronephrosis associated with antiurothelial and antinuclear autoantibodies in BALB/c−Fcgr2b−/−Pdcd1−/− mice. J Exp Med 202:1643–1648 (Epub 2005 Dec 13)
Clynes R, Calvani N, Croker BP, Richards HB (2005) Modulation of the immune response in pristane-induced lupus by expression of activation and inhibitory Fc receptors. Clin Exp Immunol 141:230–237
Fukuyama H, Nimmerjahn F, Ravetch JV (2005) The inhibitory Fcgamma receptor modulates autoimmunity by limiting the accumulation of immunoglobulin G+ anti-DNA plasma cells. Nat Immunol 6:99–106 (Epub 2004 Dec 12)
Witsch EJ, Cao H, Fukuyama H, Weigert M (2006) Light chain editing generates polyreactive antibodies in chronic graft-versus-host reaction. J Exp Med 203:1761–1772
Jiang Y, Hirose S, Abe M, Sanokawa-Akakura R, Ohtsuji M, Mi X, Li N, Xiu Y, Zhang D, Shirai J, Hamano Y, Fujii H, Shirai T (2000) Polymorphisms in IgG Fc receptor IIB regulatory regions associated with autoimmune susceptibility. Immunogenetics 51:429–435
Jiang Y, Hirose S, Sanokawa-Akakura R, Abe M, Mi X, Li N, Miura Y, Shirai J, Zhang D, Hamano Y, Shirai T (1999) Genetically determined aberrant down-regulation of FcgammaRIIB1 in germinal center B cells associated with hyper-IgG and IgG autoantibodies in murine systemic lupus erythematosus. Int Immunol 11:1685–1691
Pritchard NR, Cutler AJ, Uribe S, Chadban SJ, Morley BJ, Smith KG (2000) Autoimmune-prone mice share a promoter haplotype associated with reduced expression and function of the Fc receptor FcgammaRII. Curr Biol 10:227–230
Xiu Y, Nakamura K, Abe M, Li N, Wen XS, Jiang Y, Zhang D, Tsurui H, Matsuoka S, Hamano Y, Fujii H, Ono M, Takai T, Shimokawa T, Ra C, Shirai T, Hirose S (2002) Transcriptional regulation of Fcgr2b gene by polymorphic promoter region and its contribution to humoral immune responses. J Immunol 169:4340–4346
Blank MC, Stefanescu RN, Masuda E, Marti F, King PD, Redecha PB, Wurzburger RJ, Peterson MG, Tanaka S, Pricop L (2005) Decreased transcription of the human FCGR2B gene mediated by the −343 G/C promoter polymorphism and association with systemic lupus erythematosus. Hum Genet 117:220–227 (Epub 2005 May 14)
Mackay M, Stanevsky A, Wang T, Aranow C, Li M, Koenig S, Ravetch JV, Diamond B (2006) Selective dysregulation of the Fc{gamma}IIB receptor on memory B cells in SLE. J Exp Med 203:2157–2164
Su K, Li X, Edberg JC, Wu J, Ferguson P, Kimberly RP (2004) A promoter haplotype of the immunoreceptor tyrosine-based inhibitory motif-bearing FcgammaRIIb alters receptor expression and associates with autoimmunity. II. Differential binding of GATA4 and Yin-Yang1 transcription factors and correlated receptor expression and function. J Immunol 172:7192–7199
Su K, Wu J, Edberg JC, Li X, Ferguson P, Cooper GS, Langefeld CD, Kimberly RP (2004) A promoter haplotype of the immunoreceptor tyrosine-based inhibitory motif-bearing FcgammaRIIb alters receptor expression and associates with autoimmunity. I. Regulatory FCGR2B polymorphisms and their association with systemic lupus erythematosus. J Immunol 172:7186–7191
Enyedy EJ, Mitchell JP, Nambiar MP, Tsokos GC (2001) Defective FcgammaRIIb1 signaling contributes to enhanced calcium response in B cells from patients with systemic lupus erythematosus. Clin Immunol 101:130–135
Boruchov AM, Heller G, Veri MC, Bonvini E, Ravetch JV, Young JW (2005) Activating and inhibitory IgG Fc receptors on human DCs mediate opposing functions. J Clin Invest 15:15
Siriboonrit U, Tsuchiya N, Sirikong M, Kyogoku C, Bejrachandra S, Suthipinittharm P, Luangtrakool K, Srinak D, Thongpradit R, Fujiwara K, Chandanayingyong D, Tokunaga K (2003) Association of Fcgamma receptor IIb and IIIb polymorphisms with susceptibility to systemic lupus erythematosus in Thais. Tissue Antigens 61:374–383
Chu ZT, Tsuchiya N, Kyogoku C, Ohashi J, Qian YP, Xu SB, Mao CZ, Chu JY, Tokunaga K (2004) Association of Fcgamma receptor IIb polymorphism with susceptibility to systemic lupus erythematosus in Chinese: a common susceptibility gene in the Asian populations. Tissue Antigens 63:21–27
Kyogoku C, Dijstelbloem HM, Tsuchiya N, Hatta Y, Kato H, Yamaguchi A, Fukazawa T, Jansen MD, Hashimoto H, van de Winkel JG, Kallenberg CG, Tokunaga K (2002) Fcgamma receptor gene polymorphisms in Japanese patients with systemic lupus erythematosus: contribution of FCGR2B to genetic susceptibility. Arthritis Rheum 46:1242–1254
Tsuchiya N, Kyogoku C (2005) Role of Fc gamma receptor IIb polymorphism in the genetic background of systemic lupus erythematosus: insights from Asia. Autoimmunity 38:347–352
Li X, Wu J, Carter RH, Edberg JC, Su K, Cooper GS, Kimberly RP (2003) A novel polymorphism in the Fcgamma receptor IIB (CD32B) transmembrane region alters receptor signaling. Arthritis Rheum 48:3242–3252
Floto RA, Clatworthy MR, Heilbronn KR, Rosner DR, MacAry PA, Rankin A, Lehner PJ, Ouwehand WH, Allen JM, Watkins NA, Smith KG (2005) Loss of function of a lupus-associated FcgammaRIIb polymorphism through exclusion from lipid rafts. Nat Med 11:1056–1058 (Epub 2005 Sep 18)
Kono H, Kyogoku C, Suzuki T, Tsuchiya N, Honda H, Yamamoto K, Tokunaga K, Honda Z (2005) FcgammaRIIB Ile232Thr transmembrane polymorphism associated with human systemic lupus erythematosus decreases affinity to lipid rafts and attenuates inhibitory effects on B cell receptor signaling. Hum Mol Genet 14:2881–2892 (Epub 2005 Aug 22)
Steinman RM, Hawiger D, Liu K, Bonifaz L, Bonnyay D, Mahnke K, Iyoda T, Ravetch J, Dhodapkar M, Inaba K, Nussenzweig M (2003) Dendritic cell function in vivo during the steady state: a role in peripheral tolerance. Ann NY Acad Sci 987:15–25
Dhodapkar KM, Krasovsky J, Williamson B, Dhodapkar MV (2002) Antitumor monoclonal antibodies enhance cross-presentation of cellular antigens and the generation of myeloma-specific killer T cells by dendritic cells. J Exp Med 195:125–133
Groh V, Li YQ, Cioca D, Hunder NN, Wang W, Riddell SR, Yee C, Spies T (2005) Efficient cross-priming of tumor antigen-specific T cells by dendritic cells sensitized with diverse anti-MICA opsonized tumor cells. Proc Natl Acad Sci USA 102:6461–6466 (Epub 2005 Apr 11)
Rafiq K, Bergtold A, Clynes R (2002) Immune complex-mediated antigen presentation induces tumor immunity. J Clin Invest 110:71–79
Regnault A, Lankar D, Lacabanne V, Rodriguez A, Thery C, Rescigno M, Saito T, Verbeek S, Bonnerot C, Ricciardi-Castagnoli P, Amigorena S (1999) Fcgamma receptor-mediated induction of dendritic cell maturation and major histocompatibility complex class I-restricted antigen presentation after immune complex internalization. J Exp Med 189:371–380
Dhodapkar KM, Kaufman JL, Ehlers M, Banerjee DK, Bonvini E, Koenig S, Steinman RM, Ravetch JV, Dhodapkar MV (2005) Selective blockade of inhibitory Fcgamma receptor enables human dendritic cell maturation with IL-12p70 production and immunity to antibody-coated tumor cells. Proc Natl Acad Sci USA 102:2910–2915 (Epub 2005 Feb 9)
Kalergis AM, Ravetch JV (2002) Inducing tumor immunity through the selective engagement of activating Fcgamma receptors on dendritic cells. J Exp Med 195:1653–1659
Samsom JN, van Berkel LA, van Helvoort JM, Unger WW, Jansen W, Thepen T, Mebius RE, Verbeek SS, Kraal G (2005) Fc gamma RIIB regulates nasal and oral tolerance: a role for dendritic cells. J Immunol 174:5279–5287
Bergtold A, Desai DD, Gavhane A, Clynes R (2005) Cell surface recycling of internalized antigen permits dendritic cell priming of B cells. Immunity 23:503–514
Kushnir N, Liu L, MacPherson GG (1998) Dendritic cells and resting B cells form clusters in vitro and in vivo: T cell independence, partial LFA-1 dependence, and regulation by cross-linking surface molecules. J Immunol 160:1774–1781
Wykes M, Pombo A, Jenkins C, MacPherson GG (1998) Dendritic cells interact directly with naive B lymphocytes to transfer antigen and initiate class switching in a primary T-dependent response. J Immunol 161:1313–1319
Delamarre L, Pack M, Chang H, Mellman I, Trombetta ES (2005) Differential lysosomal proteolysis in antigen-presenting cells determines antigen fate. Science 307:1630–1634
Kraft S, Novak N (2006) Fc receptors as determinants of allergic reactions. Trends Immunol 27:88–95
Yuasa T, Kubo S, Yoshino T, Ujike A, Matsumura K, Ono M, Ravetch JV, Takai T (1999) Deletion of fcgamma receptor IIB renders H-2(b) mice susceptible to collagen-induced arthritis. J Exp Med 189:187–194
Coutelier JP, van der Logt JT, Heessen FW, Warnier G, Van Snick J (1987) IgG2a restriction of murine antibodies elicited by viral infections. J Exp Med 165:64–69
Fossati-Jimack L, Ioan-Facsinay A, Reininger L, Chicheportiche Y, Watanabe N, Saito T, Hofhuis FM, Gessner JE, Schiller C, Schmidt RE, Honjo T, Verbeek JS, Izui S (2000) Markedly different pathogenicity of four immunoglobulin G isotype-switch variants of an antierythrocyte autoantibody is based on their capacity to interact in vivo with the low-affinity Fcgamma receptor III. J Exp Med 191:1293–1302
Hamaguchi Y, Xiu Y, Komura K, Nimmerjahn F, Tedder TF (2006) Antibody isotype-specific engagement of Fcgamma receptors regulates B lymphocyte depletion during CD20 immunotherapy. J Exp Med 203:743–753 (Epub 2006 Mar 6)
Kipps TJ, Parham P, Punt J, Herzenberg LA (1985) Importance of immunoglobulin isotype in human antibody-dependent, cell-mediated cytotoxicity directed by murine monoclonal antibodies. J Exp Med 161:1–17
Markine-Goriaynoff D, Coutelier JP (2002) Increased efficacy of the immunoglobulin G2a subclass in antibody-mediated protection against lactate dehydrogenase-elevating virus–induced polioencephalomyelitis revealed with switch mutants. J Virol 76:432–435
Nimmerjahn F, Ravetch JV (2005) Divergent immunoglobulin g subclass activity through selective Fc receptor binding. Science 310:1510–1512
Schlageter AM, Kozel TR (1990) Opsonization of cryptococcus neoformans by a family of isotype–switch variant antibodies specific for the capsular polysaccharide. Infect Immun 58:1914–1918
Taborda CP, Rivera J, Zaragoza O, Casadevall A (2003) More is not necessarily better: prozone-like effects in passive immunization with IgG. J Immunol 170:3621–3630
Uchida J, Hamaguchi Y, Oliver JA, Ravetch JV, Poe JC, Haas KM, Tedder TF (2004) The innate mononuclear phagocyte network depletes B lymphocytes through Fc receptor-dependent mechanisms during anti-CD20 antibody immunotherapy. J Exp Med 199:1659–1669
Kaneko Y, Nimmerjahn F, Madaio MP, Ravetch JV (2006) Pathology and protection in nephrotoxic nephritis is determined by selective engagement of specific Fc receptors. J Exp Med 203:789–797 (Epub 2006 Mar 6)
Bijl M, Dijstelbloem HM, Oost WW, Bootsma H, Derksen RH, Aten J, Limburg PC, Kallenberg CG (2002) IgG subclass distribution of autoantibodies differs between renal and extra-renal relapses in patients with systemic lupus erythematosus. Rheumatology 41:62–67
Imai H, Hamai K, Komatsuda A, Ohtani H, Miura AB (1997) IgG subclasses in patients with membranoproliferative glomerulonephritis, membranous nephropathy, and lupus nephritis. Kidney Int 51:270–276
Winkler TH, Henschel TA, Kalies I, Baenkler HW, Skvaril F, Kalden JR (1988) Constant isotype pattern of anti-dsDNA antibodies in patients with systemic lupus erythematosus. Clin Exp Immunol 72:434–439
Loizou S, Cofiner C, Weetman AP, Walport MJ (1992) Immunoglobulin class and IgG subclass distribution of anticardiolipin antibodies in patients with systemic lupus erythematosus and associated disorders. Clin Exp Immunol 90:434–439
Bruhns P, Samuelsson A, Pollard JW, Ravetch JV (2003) Colony-stimulating factor-1-dependent macrophages are responsible for IVIG protection in antibody-induced autoimmune disease. Immunity 18:573–581
Hazenbos WL, Gessner JE, Hofhuis FM, Kuipers H, Meyer D, Heijnen IA, Schmidt RE, Sandor M, Capel PJ, Daeron M, van de Winkel JG, Verbeek JS (1996) Impaired IgG-dependent anaphylaxis and Arthus reaction in Fc gamma RIII (CD16) deficient mice. Immunity 5:181–188
Hazenbos WL, Heijnen IA, Meyer D, Hofhuis FM, Renardel de Lavalette CR, Schmidt RE, Capel PJ, van de Winkel JG, Gessner JE, van den Berg TK, Verbeek JS (1998) Murine IgG1 complexes trigger immune effector functions predominantly via Fc gamma RIII (CD16). J Immunol 161:3026–3032
Ji H, Ohmura K, Mahmood U, Lee DM, Hofhuis FM, Boackle SA, Takahashi K, Holers VM, Walport M, Gerard C, Ezekowitz A, Carroll MC, Brenner M, Weissleder R, Verbeek JS, Duchatelle V, Degott C, Benoist C, Mathis D (2002) Arthritis critically dependent on innate immune system players. Immunity 16:157–168
Meyer D, Schiller C, Westermann J, Izui S, Hazenbos WL, Verbeek JS, Schmidt RE, Gessner JE (1998) FcgammaRIII (CD16)-deficient mice show IgG isotype-dependent protection to experimental autoimmune hemolytic anemia. Blood 92:3997–4002
Clynes R, Dumitru C, Ravetch JV (1998) Uncoupling of immune complex formation and kidney damage in autoimmune glomerulonephritis. Science 279:1052–1054
Clynes R, Maizes JS, Guinamard R, Ono M, Takai T, Ravetch JV (1999) Modulation of immune complex-induced inflammation in vivo by the coordinate expression of activation and inhibitory Fc receptors. J Exp Med 189:179–185
Sylvestre D, Clynes R, Ma M, Warren H, Carroll MC, Ravetch JV (1996) Immunoglobulin G-mediated inflammatory responses develop normally in complement-deficient mice. J Exp Med 184:2385–2392
Barnes N, Gavin AL, Tan PS, Mottram P, Koentgen F, Hogarth PM (2002) FcgammaRI-deficient mice show multiple alterations to inflammatory and immune responses. Immunity 16:379–389
Bevaart L, Jansen MJ, van Vugt MJ, Verbeek JS, van de Winkel JG, Leusen JH (2006) The high-affinity IgG receptor, FcgammaRI, plays a central role in antibody therapy of experimental melanoma. Cancer Res 66:1261–1264
Ioan-Facsinay A, de Kimpe SJ, Hellwig SM, van Lent PL, Hofhuis FM, van Ojik HH, Sedlik C, da Silveira SA, Gerber J, de Jong YF, Roozendaal R, Aarden LA, van den Berg WB, Saito T, Mosser D, Amigorena S, Izui S, van Ommen GJ, van Vugt M, van de Winkel JG, Verbeek JS (2002) FcgammaRI (CD64) contributes substantially to severity of arthritis, hypersensitivity responses, and protection from bacterial infection. Immunity 16:391–402
Azeredo da Silveira S, Kikuchi S, Fossati-Jimack L, Moll T, Saito T, Verbeek JS, Botto M, Walport MJ, Carroll M, Izui S (2002) Complement activation selectively potentiates the pathogenicity of the IgG2b and IgG3 isotypes of a high affinity anti-erythrocyte autoantibody. J Exp Med 195:665–672
Kumar V, Ali SR, Konrad S, Zwirner J, Verbeek JS, Schmidt RE, Gessner JE (2006) Cell-derived anaphylatoxins as key mediators of antibody-dependent type II autoimmunity in mice. J Clin Invest 116:512–520
Schmidt RE, Gessner JE (2005) Fc receptors and their interaction with complement in autoimmunity. Immunol Lett 100:56–67
Cartron G, Dacheux L, Salles G, Solal-Celigny P, Bardos P, Colombat P, Watier H (2002) Therapeutic activity of humanized anti-CD20 monoclonal antibody and polymorphism in IgG Fc receptor FcgammaRIIIa gene. Blood 99:754–758
Weng WK, Czerwinski D, Timmerman J, Hsu FJ, Levy R (2004) Clinical outcome of lymphoma patients after idiotype vaccination is correlated with humoral immune response and immunoglobulin G Fc receptor genotype. J Clin Oncol 22:4717–4724 (Epub 2004 Oct 13)
Weng WK, Levy R (2003) Two immunoglobulin G fragment C receptor polymorphisms independently predict response to rituximab in patients with follicular lymphoma. J Clin Oncol 21:3940–3947 (Epub 2003 Sep 15)
Morgan AW, Griffiths B, Ponchel F, Montague BM, Ali M, Gardner PP, Gooi HC, Situnayake RD, Markham AF, Emery P, Isaacs JD (2000) Fcgamma receptor type IIIA is associated with rheumatoid arthritis in two distinct ethnic groups. Arthritis Rheum 43:2328–2334
Morgan AW, Keyte VH, Babbage SJ, Robinson JI, Ponchel F, Barrett JH, Bhakta BB, Bingham SJ, Buch MH, Conaghan PG, Gough A, Green M, Lawson CA, Pease CT, Markham AF, Ollier WE, Emery P, Worthington J, Isaacs JD (2003) FcgammaRIIIA-158V and rheumatoid arthritis: a confirmation study. Rheumatology 42:528–533
Magnusson V, Johanneson B, Lima G, Odeberg J, Alarcon-Segovia D, Alarcon-Riquelme ME (2004) Both risk alleles for FcgammaRIIA and FcgammaRIIIA are susceptibility factors for SLE: a unifying hypothesis. Genes Immun 5:130–137
Bazilio AP, Viana VS, Toledo R, Woronik V, Bonfa E, Monteiro RC (2004) Fc gamma RIIa polymorphism: a susceptibility factor for immune complex-mediated lupus nephritis in Brazilian patients. Nephrol Dial Transplant 19:1427–1431 (Epub 2004 Mar 5)
Dijstelbloem HM, Bijl M, Fijnheer R, Scheepers RH, Oost WW, Jansen MD, Sluiter WJ, Limburg PC, Derksen RH, van de Winkel JG, Kallenberg CG (2000) Fcgamma receptor polymorphisms in systemic lupus erythematosus: association with disease and in vivo clearance of immune complexes. Arthritis Rheum 43:2793–2800
Dijstelbloem HM, Hepkema BG, Kallenberg CG, van der Linden MW, Keijsers V, Huizinga TW, Jansen MD, van de Winkel JG (2002) The R–H polymorphism of FCgamma receptor IIa as a risk factor for systemic lupus erythematosus is independent of single-nucleotide polymorphisms in the interleukin-10 gene promoter. Arthritis Rheum 46:1125–1126
Gelmetti AP, Freitas AC, Woronik V, Barros RT, Bonfa E, Monteiro RC (2006) Polymorphism of the FcgammaRIIalpha IgG receptor in patients with lupus nephritis and glomerulopathy. J Rheumatol 33:523–530
Koene HR, Kleijer M, Swaak AJ, Sullivan KE, Bijl M, Petri MA, Kallenberg CG, Roos D, von dem Borne AE, de Haas M (1998) The Fc gammaRIIIA-158F allele is a risk factor for systemic lupus erythematosus. Arthritis Rheum 41:1813–1818
Manger K, Repp R, Jansen M, Geisselbrecht M, Wassmuth R, Westerdaal NA, Pfahlberg A, Manger B, Kalden JR, van de Winkel JG (2002) Fcgamma receptor IIa, IIIa, and IIIb polymorphisms in German patients with systemic lupus erythematosus: association with clinical symptoms. Ann Rheum Dis 61:786–792
Nieto A, Caliz R, Pascual M, Mataran L, Garcia S, Martin J (2000) Involvement of Fcgamma receptor IIIA genotypes in susceptibility to rheumatoid arthritis. Arthritis Rheum 43:735–739
Salmon JE, Millard S, Schachter LA, Arnett FC, Ginzler EM, Gourley MF, Ramsey-Goldman R, Peterson MG, Kimberly RP (1996) Fc gamma RIIA alleles are heritable risk factors for lupus nephritis in African Americans. J Clin Invest 97:1348–1354
Seligman VA, Suarez C, Lum R, Inda SE, Lin D, Li H, Olson JL, Seldin MF, Criswell LA (2001) The Fcgamma receptor IIIA-158F allele is a major risk factor for the development of lupus nephritis among Caucasians but not non-Caucasians. Arthritis Rheum 44:618–625
Tanaka Y, Suzuki Y, Tsuge T, Kanamaru Y, Horikoshi S, Monteiro RC, Tomino Y (2005) FcgammaRIIa-131R allele and FcgammaRIIIa-176V/V genotype are risk factors for progression of IgA nephropathy. Nephrol Dial Transplant 20:2439–2445
Yun HR, Koh HK, Kim SS, Chung WT, Kim DW, Hong KP, Song GG, Chang HK, Choe JY, Bae SC, Salmon JE, Yoo DH, Kim TY, Kim SY (2001) FcgammaRIIa/IIIa polymorphism and its association with clinical manifestations in Korean lupus patients. Lupus 10:466–472
Zuniga R, Ng S, Peterson MG, Reveille JD, Baethge BA, Alarcon GS, Salmon JE (2001) Low-binding alleles of Fcgamma receptor types IIA and IIIA are inherited independently and are associated with systemic lupus erythematosus in Hispanic patients. Arthritis Rheum 44:361–367
Gonzalez-Escribano MF, Aguilar F, Sanchez-Roman J, Nunez-Roldan A (2002) FcgammaRIIA, FcgammaRIIIA and FcgammaRIIIB polymorphisms in Spanish patients with systemic lupus erythematosus. Eur J Immunogenet 29:301–306
Hatta Y, Tsuchiya N, Ohashi J, Matsushita M, Fujiwara K, Hagiwara K, Juji T, Tokunaga K (1999) Association of Fc gamma receptor IIIB, but not of Fc gamma receptor IIA and IIIA polymorphisms with systemic lupus erythematosus in Japanese. Genes Immun 1:53–60
Aitman TJ, Dong R, Vyse TJ, Norsworthy PJ, Johnson MD, Smith J, Mangion J, Roberton-Lowe C, Marshall AJ, Petretto E, Hodges MD, Bhangal G, Patel SG, Sheehan-Rooney K, Duda M, Cook PR, Evans DJ, Domin J, Flint J, Boyle JJ, Pusey CD, Cook HT (2006) Copy number polymorphism in Fcgr3 predisposes to glomerulonephritis in rats and humans. Nature 439:851–855
Davies KA, Peters AM, Beynon HL, Walport MJ (1992) Immune complex processing in patients with systemic lupus erythematosus. In vivo imaging and clearance studies. J Clin Invest 90:2075–2083
Herrmann M, Voll RE, Zoller OM, Hagenhofer M, Ponner BB, Kalden JR (1998) Impaired phagocytosis of apoptotic cell material by monocyte-derived macrophages from patients with systemic lupus erythematosus. Arthritis Rheum 41:1241–1250
Potter PK, Cortes-Hernandez J, Quartier P, Botto M, Walport MJ (2003) Lupus-prone mice have an abnormal response to thioglycolate and an impaired clearance of apoptotic cells. J Immunol 170:3223–3232
Lee HS, Chung YH, Kim TG, Kim TH, Jun JB, Jung S, Bae SC, Yoo DH (2003) Independent association of HLA-DR and FCgamma receptor polymorphisms in Korean patients with systemic lupus erythematosus. Rheumatology 42:1501–1507
Salmon JE, Ng S, Yoo DH, Kim TH, Kim SY, Song GG (1999) Altered distribution of Fcgamma receptor IIIA alleles in a cohort of Korean patients with lupus nephritis. Arthritis Rheum 42:818–819
Villarreal J, Crosdale D, Ollier W, Hajeer A, Thomson W, Ordi J, Balada E, Villardell M, Teh LS, Poulton K (2001) Mannose binding lectin and FcgammaRIIa (CD32) polymorphism in Spanish systemic lupus erythematosus patients. Rheumatology 40:1009–1012
Botto M, Theodoridis E, Thompson EM, Beynon HL, Briggs D, Isenberg DA, Walport MJ, Davies KA (1996) Fc gamma RIIa polymorphism in systemic lupus erythematosus (SLE): no association with disease. Clin Exp Immunol 104:264–268
Smyth LJ, Snowden N, Carthy D, Papasteriades C, Hajeer A, Ollier WE (1997) Fc gamma RIIa polymorphism in systemic lupus erythematosus. Ann Rheum Dis 56:744–746
Yap SN, Phipps ME, Manivasagar M, Tan SY, Bosco JJ (1999) Human Fc gamma receptor IIA (FcgammaRIIA) genotyping and association with systemic lupus erythematosus (SLE) in Chinese and Malays in Malaysia. Lupus 8:305–310
Oh M, Petri MA, Kim NA, Sullivan KE (1999) Frequency of the Fc gamma RIIIA-158F allele in African American patients with systemic lupus erythematosus. J Rheumatol 26:1486–1489
Yap SN, Phipps ME, Manivasagar M, Bosco JJ (1999) Fc gamma receptor IIIB-NA gene frequencies in patients with systemic lupus erythematosus and healthy individuals of Malay and Chinese ethnicity. Immunol Lett 68:295–300
Gillespie SR, DeMartino RR, Zhu J, Chong HJ, Ramirez C, Shelburne CP, Bouton LA, Bailey DP, Gharse A, Mirmonsef P, Odom S, Gomez G, Rivera J, Fischer-Stenger K, Ryan JJ (2004) IL-10 inhibits Fc epsilon RI expression in mouse mast cells. J Immunol 172:3181–3188
Tridandapani S, Wardrop R, Baran CP, Wang Y, Opalek JM, Caligiuri MA, Marsh CB (2003) TGF-beta 1 suppresses [correction of supresses] myeloid Fc gamma receptor function by regulating the expression and function of the common gamma-subunit. J Immunol 170:4572–4577
Otten MA, van Egmond M (2004) The Fc receptor for IgA (FcalphaRI, CD89). Immunol Lett 92:23–31
Rudge EU, Cutler AJ, Pritchard NR, Smith KG (2002) Interleukin 4 reduces expression of inhibitory receptors on B cells and abolishes CD22 and Fc gamma RII-mediated B cell suppression. J Exp Med 195:1079–1085
Guyre PM, Morganelli PM, Miller R (1983) Recombinant immune interferon increases immunoglobulin G Fc receptors on cultured human mononuclear phagocytes. J Clin Invest 72:393–397
Shushakova N, Skokowa J, Schulman J, Baumann U, Zwirner J, Schmidt RE, Gessner JE (2002) C5a anaphylatoxin is a major regulator of activating versus inhibitory FcgammaRs in immune complex-induced lung disease. J Clin Invest 110:1823–1830
Coffman RL, Savelkoul HF, Lebman DA (1989) Cytokine regulation of immunoglobulin isotype switching and expression. Semin Immunol 1:55–63
Finkelman FD, Holmes J, Katona IM, Urban JF Jr, Beckmann MP, Park LS, Schooley KA, Coffman RL, Mosmann TR, Paul WE (1990) Lymphokine control of in vivo immunoglobulin isotype selection. Annu Rev Immunol 8:303–333
Shields RL, Namenuk AK, Hong K, Meng YG, Rae J, Briggs J, Xie D, Lai J, Stadlen A, Li B, Fox JA, Presta LG (2001) High resolution mapping of the binding site on human IgG1 for Fc gamma RI, Fc gamma RII, Fc gamma RIII, and FcRn and design of IgG1 variants with improved binding to the Fc gamma R. J Biol Chem 276:6591–6604
Okazaki A, Shoji-Hosaka E, Nakamura K, Wakitani M, Uchida K, Kakita S, Tsumoto K, Kumagai I, Shitara K (2004) Fucose depletion from human IgG1 oligosaccharide enhances binding enthalpy and association rate between IgG1 and FcgammaRIIIa. J Mol Biol 336:1239–1249
Shields RL, Lai J, Keck R, O’Connell LY, Hong K, Meng YG, Weikert SH, Presta LG, Namenuk AK, Rae J, Briggs J, Xie D, Stadlen A, Li B, Fox JA (2002) Lack of fucose on human IgG1 N-linked oligosaccharide improves binding to human Fcgamma RIII and antibody-dependent cellular toxicity. J Biol Chem 277:26733–26740
Shinkawa T, Nakamura K, Yamane N, Shoji-Hosaka E, Kanda Y, Sakurada M, Uchida K, Anazawa H, Satoh M, Yamasaki M, Hanai N, Shitara K (2003) The absence of fucose but not the presence of galactose or bisecting N-acetylglucosamine of human IgG1 complex-type oligosaccharides shows the critical role of enhancing antibody-dependent cellular cytotoxicity. J Biol Chem 278:3466–3473 (Epub 2002 Nov 8)
Bond A, Cooke A, Hay FC (1990) Glycosylation of IgG, immune complexes and IgG subclasses in the MRL-lpr/lpr mouse model of rheumatoid arthritis. Eur J Immunol 20:2229–2233
Matsumoto A, Shikata K, Takeuchi F, Kojima N, Mizuochi T (2000) Autoantibody activity of IgG rheumatoid factor increases with decreasing levels of galactosylation and sialylation. J Biochem (Tokyo) 128:621–628
Mizuochi T, Hamako J, Nose M, Titani K (1990) Structural changes in the oligosaccharide chains of IgG in autoimmune MRL/Mp-lpr/lpr mice. J Immunol 145:1794–1798
RadeMacher TW, Williams P, Dwek RA (1994) Agalactosyl glycoforms of IgG autoantibodies are pathogenic. Proc Natl Acad Sci USA 91:6123–6127
McGaha TL, Sorrentino B, Ravetch JV (2005) Restoration of tolerance in lupus by targeted inhibitory receptor expression. Science 307:590–593
Sherer Y, Shoenfeld Y (2006) Intravenous immunoglobulin for immunomodulation of systemic lupus erythematosus. Autoimmun Rev 5:153–155
Debre M, Bonnet MC, Fridman WH, Carosella E, Philippe N, Reinert P, Vilmer E, Kaplan C, Teillaud JL, Griscelli C (1993) Infusion of Fc gamma fragments for treatment of children with acute immune thrombocytopenic purpura. Lancet 342:945–949
Samuelsson A, Towers TL, Ravetch JV (2001) Anti-inflammatory activity of IVIG mediated through the inhibitory Fc receptor. Science 291:484–486
Kim SH, Kim S, Evans CH, Ghivizzani SC, Oligino T, Robbins PD (2001) Effective treatment of established murine collagen-induced arthritis by systemic administration of dendritic cells genetically modified to express IL-4. J Immunol 166:3499–3505
Morita Y, Yang J, Gupta R, Shimizu K, Shelden EA, Endres J, Mule JJ, McDonagh KT, Fox DA (2001) Dendritic cells genetically engineered to express IL-4 inhibit murine collagen-induced arthritis. J Clin Invest 107:1275–1284
Acknowledgements
This work was supported by the Cancer Research Institute. I apologize to all colleagues whose important work was not directly cited due to limitations of space. These references can be found in the numerous review articles referred to in this article. I would like to thank Jeffrey Ravetch for his support and Josie Clowney, Robert Anthony, and Diana Dudziak for critically reading the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nimmerjahn, F. Activating and inhibitory FcγRs in autoimmune disorders. Springer Semin Immun 28, 305–319 (2006). https://doi.org/10.1007/s00281-006-0052-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00281-006-0052-1