Abstract
Purpose
The time of a paclitaxel (PTX) concentration remains above 0.05 μM (Tc > 0.05) has been associated with PTX-induced adverse effects in Caucasians, while limited studies were reported in Asians. This study was aimed to explore the characteristics of Tc > 0.05 and the relationship between PTX exposure and toxicity in East-Asian patients.
Methods
This study was based on two prospective phase II clinical trials and patients with advanced nasopharyngeal cancer (NPC) and non-small cell lung cancer (NSCLC) who were naïve to PTX were included independently. Eligible patients receive PTX (175 mg/m2) and carboplatin (AUC = 5) treatment every 3 weeks. PTX pharmacokinetic analysis was accessed. The relationship between PTX exposure and toxicities after first cycle as well as clinical efficacy was evaluated.
Results
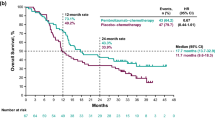
A total of 93 NPC and 40 NSCLC patients were enrolled. PTX exposure was consistent in two trials with average Tc > 0.05 duration of 38.8 h and 38.4 h, respectively. Average Tc > 0.05 in patients with grade 3/4 neutropenia was significantly higher than those without severe neutropenia in NPC patients (P = 0.003) and NSCLC patients (P = 0.007). Cut-off value of Tc > 0.05 were identified from the NPC cohort and then verified in the NSCLC cohort, dividing patients into high exposure Tc > 0.05 group (> 39 h) and low exposure group (≤ 39 h). Incidence of grade 3/4 neutropenia were significantly higher in the high exposure group in NPC cohort (43.3% vs 10.0%, P < 0.001) and NSCLC cohort (42.1% vs 9.5%, P = 0.028). No significant relationship between Tc > 0.05 and efficacy were observed.
Conclusion
Patients with PTX Tc > 0.05 duration above 39 h experience more severe neutropenia than those under 39 h. Prospective studies are needed to verify this threshold.



Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article and its supplementary information files.
References
Kumar N (1981) Taxol-induced polymerization of purified tubulin. Mechanism of action. J Biol Chem 256(20):10435–10441
Weaver BA (2014) How Taxol/paclitaxel kills cancer cells. Mol Biol Cell 25(18):2677–2681. https://doi.org/10.1091/mbc.E14-04-0916
Miller K, Wang M, Gralow J, Dickler M, Cobleigh M, Perez EA, Shenkier T, Cella D, Davidson NE (2007) Paclitaxel plus bevacizumab versus paclitaxel alone for metastatic breast cancer. N Engl J Med 357(26):2666–2676. https://doi.org/10.1056/NEJMoa072113
Belani CP, Choy H, Bonomi P, Scott C, Travis P, Haluschak J, Curran WJ Jr (2005) Combined chemoradiotherapy regimens of paclitaxel and carboplatin for locally advanced non-small-cell lung cancer: a randomized phase II locally advanced multi-modality protocol. J Clin Oncol 23(25):5883–5891. https://doi.org/10.1200/jco.2005.55.405
Fountzilas G, Papakostas P, Dafni U, Makatsoris T, Karina M, Kalogera-Fountzila A, Maniadakis N, Aravantinos G, Syrigos K, Bamias A, Christodoulou C, Economopoulos T, Kalofonos H, Nikolaou A, Angouridakis N, Stathopoulos G, Bafaloukos D, Pavlidis N, Daniilidis J (2006) Paclitaxel and gemcitabine vs. paclitaxel and pegylated liposomal doxorubicin in advanced non-nasopharyngeal head and neck cancer. An efficacy and cost analysis randomized study conducted by the Hellenic Cooperative Oncology Group. Ann Oncol 17(10):1560–1567. https://doi.org/10.1093/annonc/mdl151
Ozols RF, Bundy BN, Greer BE, Fowler JM, Clarke-Pearson D, Burger RA, Mannel RS, DeGeest K, Hartenbach EM, Baergen R (2003) Phase III trial of carboplatin and paclitaxel compared with cisplatin and paclitaxel in patients with optimally resected stage III ovarian cancer: a Gynecologic Oncology Group study. J Clin Oncol 21(17):3194–3200. https://doi.org/10.1200/jco.2003.02.153
Marupudi NI, Han JE, Li KW, Renard VM, Tyler BM, Brem H (2007) Paclitaxel: a review of adverse toxicities and novel delivery strategies. Expert Opin Drug Saf 6(5):609–621. https://doi.org/10.1517/14740338.6.5.609
Henningsson A, Karlsson MO, Viganò L, Gianni L, Verweij J, Sparreboom A (2001) Mechanism-based pharmacokinetic model for paclitaxel. J Clin Oncol 19(20):4065–4073. https://doi.org/10.1200/jco.2001.19.20.4065
Sandler A, Gray R, Perry MC, Brahmer J, Schiller JH, Dowlati A, Lilenbaum R, Johnson DH (2006) Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer. N Engl J Med 355(24):2542–2550. https://doi.org/10.1056/NEJMoa061884
Ramalingam SS, Dahlberg SE, Langer CJ, Gray R, Belani CP, Brahmer JR, Sandler AB, Schiller JH, Johnson DH (2008) Outcomes for elderly, advanced-stage non small-cell lung cancer patients treated with bevacizumab in combination with carboplatin and paclitaxel: analysis of Eastern Cooperative Oncology Group Trial 4599. J Clin Oncol 26(1):60–65. https://doi.org/10.1200/jco.2007.13.1144
Aagaard T, Reekie J, Jørgensen M, Roen A, Daugaard G, Specht L, Sengeløv H, Mocroft A, Lundgren J, Helleberg M (2020) Mortality and admission to intensive care units after febrile neutropenia in patients with cancer. Cancer Med 9(9):3033–3042. https://doi.org/10.1002/cam4.2955
Kuderer NM, Dale DC, Crawford J, Cosler LE, Lyman GH (2006) Mortality, morbidity, and cost associated with febrile neutropenia in adult cancer patients. Cancer 106(10):2258–2266. https://doi.org/10.1002/cncr.21847
Ma Y, Lin Y, Zou B, Liu W, Zhang Y, Zhao L, Huang Y, Yang Y, Fang W, Zhao Y, Sheng J, Qin T, Hu Z, Salamone SJ, Li Y, Zhang L, Zhao H (2016) Pharmacokinetic and pharmacodynamic analyses of 5-fluorouracil in east-asian patients with nasopharyngeal carcinoma. Clin Pharmacokinet 55(10):1205–1216. https://doi.org/10.1007/s40262-016-0395-2
Tong Z, Cheng M, Yu Y, Yu J, Yin Y, Liu J, Zhang S, Jiang S, Dong M (2022) Correlation between pharmacokinetic parameters of 5-fluorouracil and related metabolites and adverse reactions in East-Asian patients with advanced colorectal cancer. Cancer Chemother Pharmacol. https://doi.org/10.1007/s00280-021-04387-y
Huizing MT, Giaccone G, van Warmerdam LJ, Rosing H, Bakker PJ, Vermorken JB, Postmus PE, van Zandwijk N, Koolen MG, ten Bokkel Huinink WW, van der Vijgh WJ, Bierhorst FJ, Lai A, Dalesio O, Pinedo HM, Veenhof CH, Beijnen JH (1997) Pharmacokinetics of paclitaxel and carboplatin in a dose-escalating and dose-sequencing study in patients with non-small-cell lung cancer. The European Cancer Centre. J Clin Oncol 15(1):317–329. https://doi.org/10.1200/jco.1997.15.1.317
Gianni L, Kearns CM, Giani A, Capri G, Viganó L, Lacatelli A, Bonadonna G, Egorin MJ (1995) Nonlinear pharmacokinetics and metabolism of paclitaxel and its pharmacokinetic/pharmacodynamic relationships in humans. J Clin Oncol 13(1):180–190. https://doi.org/10.1200/jco.1995.13.1.180
Hasegawa Y, Kawaguchi T, Kubo A, Ando M, Shiraishi J, Isa S, Tsuji T, Tsujino K, Ou SH, Nakagawa K, Takada M (2011) Ethnic difference in hematological toxicity in patients with non-small cell lung cancer treated with chemotherapy: a pooled analysis on Asian versus non-Asian in phase II and III clinical trials. J Thorac Oncol 6(11):1881–1888. https://doi.org/10.1097/JTO.0b013e31822722b6
Joerger M, Kraff S, Huitema AD, Feiss G, Moritz B, Schellens JH, Beijnen JH, Jaehde U (2012) Evaluation of a pharmacology-driven dosing algorithm of 3-weekly paclitaxel using therapeutic drug monitoring: a pharmacokinetic-pharmacodynamic simulation study. Clin Pharmacokinet 51(9):607–617. https://doi.org/10.1007/bf03261934
Miller AA, Rosner GL, Egorin MJ, Hollis D, Lichtman SM, Ratain MJ (2004) Prospective evaluation of body surface area as a determinant of paclitaxel pharmacokinetics and pharmacodynamics in women with solid tumors: Cancer and Leukemia Group B Study 9763. Clin Cancer Res 10(24):8325–8331. https://doi.org/10.1158/1078-0432.Ccr-04-1078
Ohtsu T, Sasaki Y, Tamura T, Miyata Y, Nakanomyo H, Nishiwaki Y, Saijo N (1995) Clinical pharmacokinetics and pharmacodynamics of paclitaxel: a 3-hour infusion versus a 24-hour infusion. Clin Cancer Res 1(6):599–606
Joerger M, Huitema AD, Richel DJ, Dittrich C, Pavlidis N, Briasoulis E, Vermorken JB, Strocchi E, Martoni A, Sorio R, Sleeboom HP, Izquierdo MA, Jodrell DI, Calvert H, Boddy AV, Hollema H, Féty R, Van der Vijgh WJ, Hempel G, Chatelut E, Karlsson M, Wilkins J, Tranchand B, Schrijvers AH, Twelves C, Beijnen JH, Schellens JH (2007) Population pharmacokinetics and pharmacodynamics of paclitaxel and carboplatin in ovarian cancer patients: a study by the European organization for research and treatment of cancer-pharmacology and molecular mechanisms group and new drug development group. Clin Cancer Res 13(21):6410–6418. https://doi.org/10.1158/1078-0432.Ccr-07-0064
Joerger M, von Pawel J, Kraff S, Fischer JR, Eberhardt W, Gauler TC, Mueller L, Reinmuth N, Reck M, Kimmich M, Mayer F, Kopp HG, Behringer DM, Ko YD, Hilger RA, Roessler M, Kloft C, Henrich A, Moritz B, Miller MC, Salamone SJ, Jaehde U (2016) Open-label, randomized study of individualized, pharmacokinetically (PK)-guided dosing of paclitaxel combined with carboplatin or cisplatin in patients with advanced non-small-cell lung cancer (NSCLC). Ann Oncol 27(10):1895–1902. https://doi.org/10.1093/annonc/mdw290
Cline DJ, Zhang H, Lundell GD, Harney RL, Riaz HK, Jarrah J, Li Y, Miyazaki M, Courtney JB, Baburina I, Salamone SJ (2013) Development and evaluation of a nanoparticle-based immunoassay for determining paclitaxel concentrations on routine clinical analyzers. Ther Drug Monit 35(6):809–815. https://doi.org/10.1097/FTD.0b013e318296be01
Joerger M, Kraff S, Jaehde U, Hilger RA, Courtney JB, Cline DJ, Jog S, Baburina I, Miller MC, Salamone SJ (2017) Validation of a commercial assay and decision support tool for routine paclitaxel therapeutic drug monitoring (TDM). Ther Drug Monit 39(6):617–624. https://doi.org/10.1097/ftd.0000000000000446
Carter JV, Pan J, Rai SN, Galandiuk S (2016) ROC-ing along: evaluation and interpretation of receiver operating characteristic curves. Surgery 159(6):1638–1645. https://doi.org/10.1016/j.surg.2015.12.029
Gandara DR, Kawaguchi T, Crowley J, Moon J, Furuse K, Kawahara M, Teramukai S, Ohe Y, Kubota K, Williamson SK, Gautschi O, Lenz HJ, McLeod HL, Lara PN Jr, Coltman CA Jr, Fukuoka M, Saijo N, Fukushima M, Mack PC (2009) Japanese-US common-arm analysis of paclitaxel plus carboplatin in advanced non-small-cell lung cancer: a model for assessing population-related pharmacogenomics. J Clin Oncol 27(21):3540–3546. https://doi.org/10.1200/jco.2008.20.8793
Zhao C, Wang F, Huang J, Lv Y, Yin F, Liu H, Zheng Q, Li L (2021) The impacts of race and regimens on the efficacy and safety of paclitaxel and platinum combination treatment for patients with advanced non-small cell lung cancer. Eur J Clin Pharmacol 77(5):685–695. https://doi.org/10.1007/s00228-021-03129-6
Sonnichsen DS, Relling MV (1994) Clinical pharmacokinetics of paclitaxel. Clin Pharmacokinet 27(4):256–269. https://doi.org/10.2165/00003088-199427040-00002
Tamura T, Sasaki Y, Eguchi K, Shinkai T, Ohe Y, Nishio M, Kunikane H, Arioka H, Karato A, Omatsu H et al (1994) Phase I and pharmacokinetic study of paclitaxel by 24-hour intravenous infusion. Jpn J Cancer Res Gann 85(10):1057–1062. https://doi.org/10.1111/j.1349-7006.1994.tb02906.x
Belani CP, Kearns CM, Zuhowski EG, Erkmen K, Hiponia D, Zacharski D, Engstrom C, Ramanathan RK, Capozzoli MJ, Aisner J, Egorin MJ (1999) Phase I trial, including pharmacokinetic and pharmacodynamic correlations, of combination paclitaxel and carboplatin in patients with metastatic non-small-cell lung cancer. J Clin Oncol 17(2):676–684. https://doi.org/10.1200/jco.1999.17.2.676
Rowinsky EK, Jiroutek M, Bonomi P, Johnson D, Baker SD (1999) Paclitaxel steady-state plasma concentration as a determinant of disease outcome and toxicity in lung cancer patients treated with paclitaxel and cisplatin. Clin Cancer Res 5(4):767–774
Kasai T, Oka M, Soda H, Tsurutani J, Fukuda M, Nakamura Y, Kawabata S, Nakatomi K, Nagashima S, Takatani H, Fukuda M, Kinoshita A, Kohno S (2002) Phase I and pharmacokinetic study of paclitaxel and irinotecan for patients with advanced non-small cell lung cancer. Eur J Cancer (Oxford, England: 1990) 38(14):1871–1878. https://doi.org/10.1016/s0959-8049(02)00231-9
Joerger M, Huitema AD, Huizing MT, Willemse PH, de Graeff A, Rosing H, Schellens JH, Beijnen JH, Vermorken JB (2007) Safety and pharmacology of paclitaxel in patients with impaired liver function: a population pharmacokinetic-pharmacodynamic study. Br J Clin Pharmacol 64(5):622–633. https://doi.org/10.1111/j.1365-2125.2007.02956.x
Naoki K, Kunikane H, Fujii T, Tsujimura S, Hida N, Okamoto H, Watanabe K (2009) Dose-escalating and pharmacokinetic study of a weekly combination of paclitaxel and carboplatin for inoperable non-small cell lung cancer: JCOG 9910-DI. Jpn J Clin Oncol 39(9):569–575. https://doi.org/10.1093/jjco/hyp059
Tsubata Y, Okimoto T, Miura K, Karino F, Iwamoto S, Tada M, Honda T, Hamaguchi S, Ohe M, Sutani A, Kuraki T, Hamada A, Isobe T (2013) Phase I clinical and pharmacokinetic study of bi-weekly carboplatin/paclitaxel chemotherapy in elderly patients with advanced non-small cell lung cancer. Anticancer Res 33(1):261–266
Posocco B, Buzzo M, Follegot A, Giodini L, Sorio R, Marangon E, Toffoli G (2018) A new high-performance liquid chromatography-tandem mass spectrometry method for the determination of paclitaxel and 6α-hydroxy-paclitaxel in human plasma: Development, validation and application in a clinical pharmacokinetic study. PLoS ONE 13(2):e0193500. https://doi.org/10.1371/journal.pone.0193500
Kraff S, Nieuweboer AJ, Mathijssen RH, Baty F, de Graan AJ, van Schaik RH, Jaehde U, Joerger M (2015) Pharmacokinetically based dosing of weekly paclitaxel to reduce drug-related neurotoxicity based on a single sample strategy. Cancer Chemother Pharmacol 75(5):975–983. https://doi.org/10.1007/s00280-015-2724-9
Hertz DL, Kidwell KM, Vangipuram K, Li F, Pai MP, Burness M, Griggs JJ, Schott AF, Van Poznak C, Hayes DF, Lavoie Smith EM, Henry NL (2018) Paclitaxel plasma concentration after the first infusion predicts treatment-limiting peripheral neuropathy. Clin Cancer Res 24(15):3602–3610. https://doi.org/10.1158/1078-0432.Ccr-18-0656
Chen Y, Pandya KJ, Feins R, Johnstone DW, Watson T, Smudzin T, Keng PC (2008) Toxicity profile and pharmacokinetic study of a phase I low-dose schedule-dependent radiosensitizing paclitaxel chemoradiation regimen for inoperable non-small-cell lung cancer. Int J Radiat Oncol Biol Phys 71(2):407–413. https://doi.org/10.1016/j.ijrobp.2007.10.011
Xin DS, Zhou L, Li CZ, Zhang SQ, Huang HQ, Qiu GD, Lin LF, She YQ, Zheng JT, Chen C, Fang L, Chen ZS, Zhang SY (2018) TC > 0.05 as a Pharmacokinetic Parameter of Paclitaxel for Therapeutic Efficacy and Toxicity in Cancer Patients. Recent Patents Anti-Cancer Drug Discov 13(3):341–347. https://doi.org/10.2174/1574892813666180305170439
Zhang J, Zhou F, Qi H, Ni H, Hu Q, Zhou C, Li Y, Baburina I, Courtney J, Salamone SJ (2019) Randomized study of individualized pharmacokinetically-guided dosing of paclitaxel compared with body-surface area dosing in Chinese patients with advanced non-small cell lung cancer. Br J Clin Pharmacol 85(10):2292–2301. https://doi.org/10.1111/bcp.13982
Fountzilas G, Skarlos D, Athanassiades A, Kalogera-Fountzila A, Samantas E, Bacoyiannis C, Nicolaou A, Dombros N, Briasoulis E, Dinopoulou M, Stathopoulos G, Pavlidis N, Kosmidis P, Daniilidis J (1997) Paclitaxel by three-hour infusion and carboplatin in advanced carcinoma of nasopharynx and other sites of the head and neck. A phase II study conducted by the Hellenic Cooperative Oncology Group. Ann Oncol 8(5):451–455. https://doi.org/10.1023/a:1008279503428
Tan EH, Khoo KS, Wee J, Fong KW, Lee KS, Lee KM, Chua ET, Tan T, Khoo-Tan HS, Yang TL, Au E, Tao M, Ong YK, Chua EJ (1999) Phase II trial of a paclitaxel and carboplatin combination in Asian patients with metastatic nasopharyngeal carcinoma. Ann Oncol 10(2):235–237. https://doi.org/10.1023/a:1008390929826
Ma Y, Lin Q, Yang Y, Liang W, Salamone SJ, Li Y, Lin Y, Zhao H, Zhao Y, Fang W, Huang Y, Zhang L (2020) Clinical pharmacokinetics and drug exposure-toxicity correlation study of docetaxel based chemotherapy in Chinese head and neck cancer patients. Ann Transl Med 8(5):236. https://doi.org/10.21037/atm.2020.01.76
Ojara FW, Henrich A, Frances N, Huisinga W, Hartung N, Joerger M, Kloft C (2020) Time-to-event analysis of paclitaxel-associated peripheral neuropathy in advanced non-small-cell lung cancer highlighting key influential treatment/patient factors. J Pharmacol Exp Ther 375(3):430–438. https://doi.org/10.1124/jpet.120.000053
Acknowledgements
The authors gratefully thank the patients and their families, study investigators, and personnel who participated in this trial.
Funding
This work was supported by National Nature Science Foundation of China (Grant Number: 81872499 for L Zhang, Grant Number: 82002409 for Y Ma, Grant Number: 82073396 for H Zhao), Guangdong Basic and Applied Basic Research Foundation (2020A1515010020 for Y Ma), and Bristol-Myers Squibb.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
Li Zhang reports receiving research support from Bristol-Myers Squibb. Other authors declare no conflict of interest in connection with the work submitted.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xue, J., He, H., Lin, Z. et al. Paclitaxel exposure-toxicity analysis reveals a pharmacokinetic determinant for dose-limiting neutropenia in East-Asian solid tumor patients: results from two prospective, phase II studies. Cancer Chemother Pharmacol 90, 229–237 (2022). https://doi.org/10.1007/s00280-022-04456-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-022-04456-w