Abstract
Objectives
Chemotherapy-related acute exacerbation (AE) of interstitial lung disease (ILD) is observed in certain patients with non-small cell lung cancer (NSCLC) who have ILD. Although the prognosis of AE-ILD is extremely poor, there are no established risk factors for its occurrence. Therefore, we retrospectively investigated whether high-resolution computed tomography (HRCT) findings could identify risk factors for AE-ILD.
Materials and methods
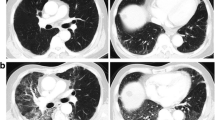
Between January 2005 and December 2016, 35 patients with NSCLC who received chemotherapy at Hiroshima University Hospital and were diagnosed with ILD on HRCT were enrolled. The extent of ground-glass attenuation (GGA), reticulation, honeycomb appearance, and emphysema, as well as the presence of micronodules, traction bronchiectasis, and consolidation were evaluated in five levels of the lung bilaterally. The HRCT scores of GGA, reticulation, honeycomb appearance, and emphysema were determined by the following formula: 100 × sum of the extent of the HRCT findings/lung area.
Results
Thirty-five patients underwent various first- to fifth-line chemotherapy regimens. Nine patients (25.7%) developed AE-ILD. The median HRCT scores of GGA and reticulation were significantly higher in patients with AE-ILD than in those without. On univariate analysis, a GGA area score ≥ 24.8, reticulation area score ≥ 19.5, and KL-6 level ≥ 946 U/mL were significant risk factors. Multivariate logistic analysis revealed that only a GGA area score ≥ 24.8 was an independent risk factor of AE-ILD.
Conclusions
The GGA area on HRCT is a risk factor for chemotherapy-related AE-ILD. Therefore, this parameter can be used to predict the risk of AE-ILD before administering chemotherapy.
Similar content being viewed by others
References
Raghu G, Nyberg F, Morgan G (2004) The epidemiology of interstitial lung disease and its association with lung cancer. Br J Cancer 91(Suppl 2):S3–S10
American Thoracic Society (2000) Idiopathic pulmonary fibrosis: diagnosis and treatment. International consensus statement. American Thoracic Society (ATS), and the European Respiratory Society (ERS). Am J Respir Crit Care Med 161:646–664
American Thoracic Society/European Respiratory Society International Multidisciplinary Consensus Classification of the Idiopathic Interstitial Pneumonias (2002) This joint statement of the American Thoracic Society (ATS), and the European Respiratory Society (ERS) was adopted by the ATS board of directors, June 2001 and by the ERS Executive Committee, June 2001. Am J Respir Crit Care Med 165:277–304
Raghu G, Collard HR, Egan JJ, Martinez FJ, Behr J, Brown KK, Colby TV, Cordier JF, Flaherty KR, Lasky JA, Lynch DA, Ryu JH, Swigris JJ, Wells AU, Ancochea J, Bouros D, Carvalho C, Costabel U, Ebina M, Hansell DM, Johkoh T, Kim DS, King TE Jr, Kondoh Y, Myers J, Muller NL, Nicholson AG, Richeldi L, Selman M, Dudden RF, Griss BS, Protzko SL, Schunemann HJ (2011) An official ATS/ERS/JRS/ALAT statement: idiopathic pulmonary fibrosis: evidence-based guidelines for diagnosis and management. Am J Respir Crit Care Med 183:788–824
Collard HR, Moore BB, Flaherty KR, Brown KK, Kaner RJ, King TE Jr, Lasky JA, Loyd JE, Noth I, Olman MA, Raghu G, Roman J, Ryu JH, Zisman DA, Hunninghake GW, Colby TV, Egan JJ, Hansell DM, Johkoh T, Kaminski N, Kim DS, Kondoh Y, Lynch DA, Muller-Quernheim J, Myers JL, Nicholson AG, Selman M, Toews GB, Wells AU, Martinez FJ (2007) Acute exacerbations of idiopathic pulmonary fibrosis. Am J Respir Crit Care Med 176:636–643
Kim DS, Park JH, Park BK, Lee JS, Nicholson AG, Colby T (2006) Acute exacerbation of idiopathic pulmonary fibrosis: frequency and clinical features. Eur Respir J 27:143–150
Martinez FJ, Safrin S, Weycker D, Starko KM, Bradford WZ, King TE Jr, Flaherty KR, Schwartz DA, Noble PW, Raghu G, Brown KK (2005) The clinical course of patients with idiopathic pulmonary fibrosis. Ann Intern Med 142:963–967
Minegishi Y, Takenaka K, Mizutani H, Sudoh J, Noro R, Okano T, Azuma A, Yoshimura A, Ando M, Tsuboi E, Kudoh S, Gemma A (2009) Exacerbation of idiopathic interstitial pneumonias associated with lung cancer therapy. Intern Med 48:665–672
Isobe K, Hata Y, Sakamoto S, Takai Y, Shibuya K, Homma S (2010) Clinical characteristics of acute respiratory deterioration in pulmonary fibrosis associated with lung cancer following anti-cancer therapy. Respirology 15:88–92
Shukuya T, Ishiwata T, Hara M, Muraki K, Shibayama R, Koyama R, Takahashi K (2010) Carboplatin plus weekly paclitaxel treatment in non-small cell lung cancer patients with interstitial lung disease. Anticancer Res 30:4357–4361
Minegishi Y, Sudoh J, Kuribayasi H, Mizutani H, Seike M, Azuma A, Yoshimura A, Kudoh S, Gemma A (2011) The safety and efficacy of weekly paclitaxel in combination with carboplatin for advanced non-small cell lung cancer with idiopathic interstitial pneumonias. Lung Cancer 71:70–74
Kinoshita T, Azuma K, Sasada T, Okamoto M, Hattori S, Imamura Y, Yamada K, Tajiri M, Yoshida T, Zaizen Y, Kawahara A, Fujimoto K, Hoshino T (2012) Chemotherapy for non-small cell lung cancer complicated by idiopathic interstitial pneumonia. Oncol Lett 4:477–482
Choi MK, Hong JY, Chang W, Kim M, Kim S, Jung HA, Lee SJ, Park S, Chung MP, Sun JM, Park K, Ahn MJ, Ahn JS (2014) Safety and efficacy of gemcitabine or pemetrexed in combination with a platinum in patients with non-small-cell lung cancer and prior interstitial lung disease. Cancer Chemother Pharmacol 73:1217–1225
Kato M, Shukuya T, Takahashi F, Mori K, Suina K, Asao T, Kanemaru R, Honma Y, Muraki K, Sugano K, Shibayama R, Koyama R, Shimada N, Takahashi K (2014) Pemetrexed for advanced non-small cell lung cancer patients with interstitial lung disease. BMC Cancer 14:508
Kenmotsu H, Naito T, Mori K, Ko R, Ono A, Wakuda K, Imai H, Taira T, Murakami H, Endo M, Takahashi T (2015) Effect of platinum-based chemotherapy for non-small cell lung cancer patients with interstitial lung disease. Cancer Chemother Pharmacol 75:521–526
Sekine A, Satoh H, Baba T, Ikeda S, Okuda R, Shinohara T, Komatsu S, Hagiwara E, Iwasawa T, Ogura T, Kato T (2016) Safety and efficacy of S-1 in combination with carboplatin in non-small cell lung cancer patients with interstitial lung disease: a pilot study. Cancer Chemother Pharmacol 77:1245–1252
Non-Small Cell Lung Cancer Collaborative Group (2010) Chemotherapy and supportive care versus supportive care alone for advanced non-small cell lung cancer. Cochrane Database Syst Rev. https://doi.org/10.1002/14651858.CD007309.pub2
Kenmotsu H, Naito T, Kimura M, Ono A, Shukuya T, Nakamura Y, Tsuya A, Kaira K, Murakami H, Takahashi T, Endo M, Yamamoto N (2011) The risk of cytotoxic chemotherapy-related exacerbation of interstitial lung disease with lung cancer. J Thorac Oncol 6:1242–1246
Enomoto Y, Inui N, Imokawa S, Karayama M, Hasegawa H, Ozawa Y, Matsui T, Yokomura K, Suda T (2015) Safety of topotecan monotherapy for relapsed small cell lung cancer patients with pre-existing interstitial lung disease. Cancer Chemother Pharmacol 76:499–505
Watanabe N, Niho S, Kirita K, Umemura S, Matsumoto S, Yoh K, Ohmatsu H, Goto K (2015) Second-line docetaxel for patients with platinum-refractory advanced non-small cell lung cancer and interstitial pneumonia. Cancer Chemother Pharmacol 76:69–74
Asai N, Katsuda E, Hamanaka R, Kosaka K, Matsubara A, Nishimura M, Tanaka H, Yokoe N, Takahashi A, Yamaguchi E, Kubo A (2017) The ATS/ERS/JRS/ALAT statement “IPF by HRCT” could predict acute exacerbation of interstitial lung disease in non-small cell lung cancer. Tumori 103:60–65
Ozawa Y, Akahori D, Koda K, Abe T, Hasegawa H, Matsui T, Tanahashi M, Niwa H, Yamada K, Yokomura K, Suda T (2016) Distinctive impact of pre-existing interstitial lung disease on the risk of chemotherapy-related lung injury in patients with lung cancer. Cancer Chemother Pharmacol 77:1031–1038
Sumikawa H, Johkoh T, Colby TV, Ichikado K, Suga M, Taniguchi H, Kondoh Y, Ogura T, Arakawa H, Fujimoto K, Inoue A, Mihara N, Honda O, Tomiyama N, Nakamura H, Muller NL (2008) Computed tomography findings in pathological usual interstitial pneumonia: relationship to survival. Am J Respir Crit Care Med 177:433–439
Mura M, Porretta MA, Bargagli E, Sergiacomi G, Zompatori M, Sverzellati N, Taglieri A, Mezzasalma F, Rottoli P, Saltini C, Rogliani P (2012) Predicting survival in newly diagnosed idiopathic pulmonary fibrosis: a 3-year prospective study. Eur Respir J 40:101–109
Collard HR, Ryerson CJ, Corte TJ, Jenkins G, Kondoh Y, Lederer DJ, Lee JS, Maher TM, Wells AU, Antoniou KM, Behr J, Brown KK, Cottin V, Flaherty KR, Fukuoka J, Hansell DM, Johkoh T, Kaminski N, Kim DS, Kolb M, Lynch DA, Myers JL, Raghu G, Richeldi L, Taniguchi H, Martinez FJ (2016) Acute exacerbation of idiopathic pulmonary fibrosis. An international working group report. Am J Respir Crit Care Med 194:265–275
Zerhouni E (1989) Computed tomography of the pulmonary parenchyma. An overview. Chest 95:901–907
Kadoch MA, Cham MD, Beasley MB, Ward TJ, Jacobi AH, Eber CD, Padilla ML (2015) Idiopathic interstitial pneumonias: a radiology-pathology correlation based on the revised 2013 American Thoracic Society-European Respiratory Society classification system. Curr Probl Diagn Radiol 44:15–25
Sheppard MN, Harrison NK (1992) New perspectives on basic mechanisms in lung disease. 1. Lung injury, inflammatory mediators, and fibroblast activation in fibrosing alveolitis. Thorax 47:1064–1074
Suzuki H, Sekine Y, Yoshida S, Suzuki M, Shibuya K, Yonemori Y, Hiroshima K, Nakatani Y, Mizuno S, Takiguchi Y, Yoshino I (2011) Risk of acute exacerbation of interstitial pneumonia after pulmonary resection for lung cancer in patients with idiopathic pulmonary fibrosis based on preoperative high-resolution computed tomography. Surg Today 41:914–921
Reichmann WM, Yu YF, Macaulay D, Wu EQ, Nathan SD (2015) Change in forced vital capacity and associated subsequent outcomes in patients with newly diagnosed idiopathic pulmonary fibrosis. BMC Pulm Med 15:167
Ishikawa N, Hattori N, Yokoyama A, Kohno N (2012) Utility of KL-6/MUC1 in the clinical management of interstitial lung diseases. Respir Investig 50:3–13
Ohshimo S, Ishikawa N, Horimasu Y, Hattori N, Hirohashi N, Tanigawa K, Kohno N, Bonella F, Guzman J, Costabel U (2014) Baseline KL-6 predicts increased risk for acute exacerbation of idiopathic pulmonary fibrosis. Respir Med 108:1031–1039
Inata J, Hattori N, Yokoyama A, Ohshimo S, Doi M, Ishikawa N, Hamada H, Kohno N (2007) Circulating KL-6/MUC1 mucin carrying sialyl Lewisa oligosaccharide is an independent prognostic factor in patients with lung adenocarcinoma. Int J Cancer 120:2643–2649
Ishikawa N, Hattori N, Yokoyama A, Tanaka S, Nishino R, Yoshioka K, Ohshimo S, Fujitaka K, Ohnishi H, Hamada H, Arihiro K, Kohno N (2008) Usefulness of monitoring the circulating Krebs von den Lungen-6 levels to predict the clinical outcome of patients with advanced nonsmall cell lung cancer treated with epidermal growth factor receptor tyrosine kinase inhibitors. Int J Cancer 122:2612–2620
Enomoto Y, Inui N, Kato T, Baba T, Karayama M, Nakamura Y, Ogura T, Suda T (2016) Low forced vital capacity predicts cytotoxic chemotherapy-associated acute exacerbation of interstitial lung disease in patients with lung cancer. Lung Cancer 96:63–67
Song JW, Hong SB, Lim CM, Koh Y, Kim DS (2011) Acute exacerbation of idiopathic pulmonary fibrosis: incidence, risk factors and outcome. Eur Respir J 37:356–363
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Ethical approval
This retrospective analysis was approved by the Hiroshima University Institutional Review Board (No. E404). All procedures performed in studies involving human participants were in accordance with ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Informed consent
To obtain consent of the patients, opt-out method was applied in this retrospective study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Masuda, T., Hirano, C., Horimasu, Y. et al. The extent of ground-glass attenuation is a risk factor of chemotherapy-related exacerbation of interstitial lung disease in patients with non-small cell lung cancer. Cancer Chemother Pharmacol 81, 131–139 (2018). https://doi.org/10.1007/s00280-017-3476-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-017-3476-5