Abstract
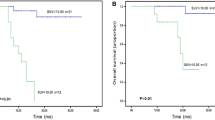
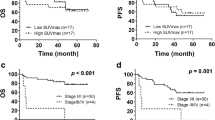
Interim 18F-FDG PET/CT (I-PET) has a role in response evaluation and treatment guidance in patients with nasal-type extranodal natural killer/T cell lymphoma (ENKTL). However, there was no agreement on the timing of I-PET performed, after chemotherapy or after chemoradiotherapy. We aimed to find the appropriate timing for I-PET by assessing the prognostic value of I-PET in response evaluation in ENKTL patients. Two hundred and twenty-seven ENKTL patients who had undergone I-PET were retrospectively included. All patients were grouped based on their therapeutic strategy received, chemotherapy or chemoradiotherapy. The Deauville 5-point score (DS) was used to interpret the I-PET images. The hazard ratio (HR) and C-index were used to measure the discriminatory and prognostic capacities of I-PET performed at different times. One hundred and six patients underwent the I-PET after chemotherapy (chemotherapy group), while I-PET was performed after chemoradiotherapy in 121 patients (chemoradiotherapy group). Eighty-seven patients were classified as metabolic remission (DS score of 1–3), while the other 140 were classified as non-metabolic remission (DS score of 4–5) according to the Deauville criteria. There were no significant survival differences between patients in metabolic remission and in non-metabolic remission in either progression-free survival (PFS, p = 0.406) or overall survival (OS, p = 0.350). In the chemotherapy group, patients in metabolic remission had significantly superior PFS than patients in non-metabolic remission (p = 0.012). For OS, a discriminative trend was also found on the survival curve between patients in metabolic remission and in non-metabolic remission (p = 0.082). In the chemoradiotherapy group, there was no significant difference in PFS (P = 0.185) or OS (P = 0.627) between patients in metabolic remission and in non-metabolic remission. I-PET after chemotherapy yields higher discriminative power and has the ability for prognostic prediction in nasal-type ENKTL patients. I-PET after radiochemotherapy has no prognostic value. Thus, the appropriate timing for I-PET is after chemotherapy but before radiotherapy for response evaluation in nasal-type ENKTL patients.






Similar content being viewed by others
Data availability
All authors agree to publicize this manuscript. Neither the manuscript nor a similar part of the content has been published or is being considered for publication elsewhere.
References
Wang H, Fu BB, Gale RP, Liang YA-O (2021) NK-/T-cell lymphomas. Leukemia 35(9):2460–2468
Alaggio R, Amador C, Anagnostopoulos I et al (2022) The 5th edition of the world health organization classification of haematolymphoid tumours: lymphoid neoplasms. Leukemia 36(7):1720–1748. https://doi.org/10.1038/s41375-022-01620-2
Tse E, Zhao WL, Xiong J, Kwong YL (2022) How we treat NK/T-cell lymphomas. J Hematol Oncol 15(1):74. https://doi.org/10.1186/s13045-022-01293-5
Tse E, Kwong YL (2017) The diagnosis and management of NK/T-cell lymphomas. J Hematol Oncol 10(1):85. https://doi.org/10.1186/s13045-017-0452-9
Harabuchi Y, Takahara M, Kishibe K, Nagato T, Kumai T (2019) Extranodal natural killer/T-cell lymphoma, nasal type: Basic Science and Clinical Progress. Front Pediatr 7(2296–2360):141. https://doi.org/10.3389/fped.2019.00141
Horwitz SM, Ansell S, Ai WZ et al (2022) T-cell lymphomas, version 2.2022, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw 20(3):285–308. https://doi.org/10.6004/jnccn.2022.0015
Tse E, Kwong YL (2019) NK/T-cell lymphomas. Best Pract Res Clin Haematol 32(3):253–261
Chim CS, Ma SY, Au WY, Choy C, Lie AK, Liang R, Yau CC, Kwong YL (2004) Primary nasal natural killer cell lymphoma: long-term treatment outcome and relationship with the international prognostic index. Blood 103(1):216–221. https://doi.org/10.1182/blood-2003-05-1401
Lee J, Suh C, Park YH et al (2006) Extranodal natural killer T-cell lymphoma, nasal-type: a prognostic model from a retrospective multicenter study. J Clin Oncol 24(4):612–618. https://doi.org/10.1200/JCO.2005.04.1384
Kim SJ, Yoon DH, Jaccard A et al (2016) A prognostic index for natural killer cell lymphoma after non-anthracycline-based treatment: a multicentre, retrospective analysis. Lancet Oncol 17(3):389–400. https://doi.org/10.1016/S1470-2045(15)00533-1
Hoppe RT, Advani RH, Ai WZ et al (2020) Hodgkin lymphoma, version 2.2020, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw 18(6):755–781. https://doi.org/10.6004/jnccn.2020.0026
Cheson BD, Meignan M (2021) Current role of functional imaging in the management of lymphoma. Curr Oncol Rep 23(12):144
Khong PL, Pang CB, Liang R, Kwong YL, Au WY (2008) Fluorine-18 fluorodeoxyglucose positron emission tomography in mature T-cell and natural killer cell malignancies. Ann Hematol 87(8):613–621. https://doi.org/10.1007/s00277-008-0494-8
Chan WK, Au WY, Wong CY, Liang R, Leung AY, Kwong YL, Khong PL (2010) Metabolic activity measured by F-18 FDG PET in natural killer-cell lymphoma compared to aggressive B- and T-cell lymphomas. Clin Nucl Med 35(8):571–575. https://doi.org/10.1097/RLU.0b013e3181e4dcbf
Moon SH, Cho SK, Kim WS, Kim SJ, Chan Ahn Y, Choe YS, Lee KH, Kim BT, Choi JY (2013) The role of 18F-FDG PET/CT for initial staging of nasal type natural killer/T-cell lymphoma: a comparison with conventional staging methods. J Nucl Med 54(7):1039–1044. https://doi.org/10.2967/jnumed.112.113399
Wang H, Shen G, Jiang C, Li L, Cui F, Tian R (2018) Prognostic value of baseline, interim and end-of-treatment 18F-FDG PET/CT parameters in extranodal natural killer/T-cell lymphoma: a meta-analysis. PLoS One 13(3):e0194435. https://doi.org/10.1371/journal.pone.0194435
Qin C, Yang S, Sun X, Xia X, Li C, Lan X (2019) 18F-FDG PET/CT for prognostic stratification of patients with extranodal natural killer/T-cell lymphoma. Clin Nucl Med 44(3):201–208. https://doi.org/10.1097/RLU.0000000000002440
Jiang C, Su M, Kosik RO, Zou L, Jiang M, Tian R (2015) The Deauville 5-point scale improves the prognostic value of interim FDG PET/CT in extranodal natural killer/T-cell lymphoma. Clin Nucl Med 40(10):767–773. https://doi.org/10.1097/RLU.0000000000000892
Xu P, Guo R, You J, Cheng S, Li J, Zhong H, Sun C, Xu H, Huang H, Li B, Zhao W (2021) Dynamic evaluation of the prognostic value of (18)F-FDG PET/CT in extranodal NK/T-cell lymphoma, nasal type. Ann Hematol 100(4):1039–1047. https://doi.org/10.1007/s00277-021-04466-3
Ding JJ, Chen YL, Zhou SH, Zhao K (2018) Positron emission tomography/computed tomography in the diagnosis, staging, and prognostic evaluation of natural killer/T-cell lymphoma. J Int Med Res 46(12):4920–4929. https://doi.org/10.1177/0300060518804375
Chen X, Zhao S, Wang H, Fu C, Tian R, Zou L (2021) Assessment of the prognostic value of interim fluorodeoxyglucose positron emission tomography/computed tomography in nasal-type extranodal natural killer/T-cell lymphoma. Quant Imaging Med Surg 11(4):1220–1233. https://doi.org/10.21037/qims-20-620
Cheson BD (2015) Staging and response assessment in lymphomas: the new Lugano classification. Chin Clin Oncol 4(1):5. https://doi.org/10.3978/j.issn.2304-3865.2014.11.03
Rahman WT, Wale DJ, Viglianti BL, Townsend DM, Manganaro MS, Gross MD, Wong KK, Rubello D (2019) The impact of infection and inflammation in oncologic (18)F-FDG PET/CT imaging. Biomed Pharmacother 117(1950-6007 (Electronic)):109168. https://doi.org/10.1016/j.biopha.2019.109168
Khong PL, Huang B, Lee EY, Chan WK, Kwong YL (2014) Midtreatment 18F-FDG PET/CT scan for early response assessment of SMILE therapy in natural killer/T-cell lymphoma: a prospective study from a single center. J Nucl Med 55(6):911–916
Kim H, Ko YH (2022) The pathologic and genetic characteristics of extranodal NK/T-cell lymphoma. Life-Basel 12(1):73. https://doi.org/10.3390/life12010073
Tse E, Kwong YL (2019) NK/T-cell lymphomas. Best Pract Res Cl Ha 32(3):253–261. https://doi.org/10.1016/j.beha.2019.06.005
Kaim AH, Weber B, Kurrer MO, Gottschalk J, von Schulthess GK, Buck A (2002) Autoradiographic quantification of 18F-FDG uptake in experimental soft-tissue abscesses in rats. Radiology 223(2):446–451
Yamada S, Kubota K, Kubota R, Ido T, Tamahashi N (1995) High accumulation of fluorine-18-fluorodeoxyglucose in turpentine-induced inflammatory tissue. J Nucl Med 36(7):1301–1306
Jingjing Zhang HC, Yanru Ma Yu, Xiao NN, Lin W, Wang X, Liang Z, Zhang F, Li F, Zhang W, Zhu Z (2014) Characterizing IgG4-related disease with 18F-FDG PET/CT: a prospective cohort study. Eur J Nucl Med Mol Imaging 41(8):1624–1634
Lee N, Yoo Ie R, Park SY, Yoon H, Lee Y, Oh JK (2015) Significance of incidental nasopharyngeal uptake on (18)F-FDG PET/CT: patterns of benign/physiologic uptake and differentiation from malignancy. Nucl Med Mol Imaging 49(1):11–18
Masieri S, Trabattoni D, Incorvaia C, De Luca MC, Dell’Albani I, Leo G, Frati F (2014) A role for Waldeyer’s ring in immunological response to allergens. Curr Med Res Opin 30(2):203–205. https://doi.org/10.1185/03007995.2013.855185
Nakamoto Y, Tatsumi M, Hammoud D, Cohade C, Osman MM, Wahl RL (2005) Normal FDG distribution patterns in the head and neck: PET/CT evaluation. Radiology 234(3):879–885. https://doi.org/10.1148/radiol.2343030301
Purohit BSAA, Dulguerov N, Becker CD, Ratib O, Becker M (2014) FDG-PET/CT pitfalls in oncological head and neck imaging. Insights Imaging 5(5):585–602
Funding
This work was supported by the Post-Doctor Research Project, West China Hospital, Sichuan University (grant 2023HXBH075).
Author information
Authors and Affiliations
Contributions
Conceived and designed the experiments: RW and MGS. Performed the experiments: RW, YZ, and QPF. Analyzed the data: RW, YZ, and MGS. Contributed reagents/materials/analysis tools: RW, YZ, and MGS. Provided critical input into the design and drafting of the manuscript: MJ and LQZ. Wrote and revised the paper: RW and MGS.
Corresponding author
Ethics declarations
Ethics approval
Sichuan University West China Hospital Review Board approved the study.
Consent to participate and consent for publication
All patients signed informed consent before undergoing PET/CT scans.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, R., Zhang, Y., Fan, Q. et al. Appropriate timing to perform an interim 18F-FDG PET/CT in patients with nasal-type extranodal natural killer/T cell lymphoma. Ann Hematol 103, 885–892 (2024). https://doi.org/10.1007/s00277-023-05562-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-023-05562-2