Abstract
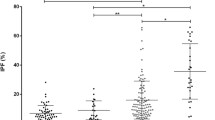
The platelet antibodies that cause pseudothrombocytopenia (PTCP) act only in vitro and do not produce clinical bleeding. Most studies on PTCP have focused on improving differential diagnosis with true thrombocytopenia but studies on the characteristics of patients with PTCP are limited. In this study, we aimed to evaluate the clinical and biological characteristics of 192 patients with PTCP. In addition to general variables, we evaluated automated and microscopic platelet counts, platelet clumps, platelet diameters, immature platelet fraction (IPF), and platelet antibodies. Adult women accounted for the largest subgroup of patients (n=82; 42.7%) and 67 patients (34.9%) were grouped into families. Forty-four patients (22.9%) had one or more associated autoimmune disorders (ADs); 39 relatives of these patients (19.8%) had ADs and 45 relatives (23.4%) had immune thrombocytopenia (ITP) or unspecified thrombocytopenia. Platelet cryptantibodies and/or autoantibodies were positive in 56 patients (30.1%). Most patients (n=169; 80%) had automated platelet counts >80×109/L. In all patients, microscopic platelet counts were ≥150×109/L. The platelet clump index (% increase in microscopic platelet count compared to automatic count) ranged from 30 to >7000%. Platelet diameters and IPF parameters were significantly greater in the PTCP versus healthy controls (p<0.001). A total of 17 patients (8.8%) had had previous ITP or the PTCP evolved into ITP. Our data suggest that PTCP should be considered a situation of autoimmunity; the assessment of platelet clumps has a high diagnostic value; the close association between ITP and PTCP suggests that these conditions could be different phases of the same process.



Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Gowland E, Kay E, Spillman JC, Williamson JR (1969) Agglutination of platelets by a serum factor in the presence of EDTA. J Clin Pathol 22:460–464. https://doi.org/10.1136/jcp.22.4.460
Pegels JG, Bruynes ECE, Engelfriet CP, von dem Borne AEGK (1982) Pseudothrombocytopenia: an immunologic study on platelet antibodies dependent on ethylene diamine tetra-acetate. Blood 59:157–161
von dem Borne AEGK, van der Lelie H, Vos JJE, van der Plas-van Dalen CM, Risseeuw-Bogaert NJ, Ticheler MDA, Pegels HG (1986) III. Antibodies against cryptantigens of platelets. Characterization and significance for the serologist. Curr Stud Hematol Blood Transfus 52:33–46
Casonato A, Bertomoro A, Pontara E, Dannhauser D, Lazzaro AR, Girolami A (1994) EDTA dependent pseudothrombocytopenia caused by antibodies against the cytoadhesive receptor of platelet gpIIB-IIIA. J Clin Pathol 47:625–630. https://doi.org/10.1136/jcp.47.7.625
Garcia Suarez J, Calero MA, Ricard MP, Krsnik I, Rus F, Perera F, Merino JL (1992) EDTA-dependent pseudothrombocytopenia in ambulatory patients: clinical characteristics and role of new automated cell-counting in its detection. Am J Hematol 39:146–147. https://doi.org/10.1002/ajh.2830390215
Bizzaro N (1995) EDTA-dependent pseudothrombocytopenia: a clinical and epidemiological study of 112 cases, with 10-year follow-up. Am J Hematol 50:103–109. https://doi.org/10.1002/ajh.2830500206
Nagler M, Keller P, Siegrist D, Alberio L (2014) A case of EDTA-dependent pseudothrombocytopenia: simple recognition of an underdiagnosed and misleading phenomenon. BMC Clin Pathol 14:19. https://doi.org/10.1186/1472-6890-14-19
Lardinois B, Favresse J, Chatelain B, Lippi G, Mullier F (2021) Pseudothrombocytopenia - a review on causes, occurrence and clinical implications. J Clin Med 10:594. https://doi.org/10.3390/jcm10040594
Xiao Y, Yu S, Xu Y (2015) The prevalence and biochemical profiles of EDTA-dependent pseudothrombocytopenia in a generally healthy population. Acta Haematol 134:177–180. https://doi.org/10.1159/000373915
Zhang L, Xu J, Gao L, Pan S (2018) Spurious thrombocytopenia in automated platelet count. Lab Med 49:130–133. https://doi.org/10.1093/labmed/lmx081
Maslanka K, Marciniak-Bielak D, Szczepinski A (2008) Pseudothrombocytopenia in blood donors. Vox Sang 95:349. https://doi.org/10.1111/j.1423-0410.2008.01103.x
Berkman N, Michaeli Y, Or R, Eldor A (1991) EDTA-dependent pseudothrombocytopenia: a clinical study of 18 patients and review of the literature. Am J Hematol 36:195–201
Muñiz-Diaz E, Madoz P, Pujol-Moix N, Pastoret C, Arilla M, Ibañez M, Guanyabens C, Domingo-Albós A (1995) Characterization of antibodies directed against platelet cryptantigens detected during the immunological study of 356 consecutive patients with presumed autoimmune thrombocytopenia (AITP). Transfus Med 5:185–191. https://doi.org/10.1111/j.1365-3148.1995.tb00226.x
Froom P, Barak M (2011) Prevalence and course of pseudothrombocytopenia in outpatients. Clin Chem Lab Med 49:111–114. https://doi.org/10.1515/CCLM.2011.013
Baccini V, Franck G, Jacqmin H, Chatelain B, Girard S, Wuilleme S, Vedrenne A, Guiheneu E, Toussaint-Hacquard M, Everaere F, Soulard M, Lesesve JF, Bardet V (2020) Platelet counting: ugly traps and good advice. Proposals from the French-Speaking Cellular Hematology Group (GFHC). J Clin Med 9:808. https://doi.org/10.3390/jcm9030808
Schuff-Werner P, Mansour J, Gropp A (2020) Pseudo-thrombocytopenia (PTCP). A challenge in the daily laboratory routine? J Lab Med 44:295–304. https://doi.org/10.1515/labmed-2020-0099
Pujol-Moix N, Jimenez B, Muñiz-Diaz E, Roca M, Souto JC (2018) Familial immune thrombocytopenia. Report of 16 cases and literature review. J Rare Dis Res Treat 4:52–60
George JN, Woolf SH, Raskob GE, Wasser JS, Aledort LM, Ballem PJ, Blanchette VS, Bussel JB, Cines DB, Kelton JG, Lichtin AE, McMillan R, Okerbloom JA, Regan DH, Warrier I (1996) Idiopathic thrombocytopenic purpura: a practice guideline developed by explicit methods for the American Society of Hematology. Blood 88:3–40. https://doi.org/10.3109/07853899808999383
Aledort LM, Hayward CP, Chen MG, Nichol JL, Bussel J, ITP Study Group (2004) Prospective screening of 205 patients with ITP, including diagnosis, serological markers, and the relationship between platelet counts, endogenous thrombopoietin, and circulating antithrombopoietin antibodies. Am J Hematol 76:205–213. https://doi.org/10.1002/ajh.20104
Noris P, Biino G, Pecci A, Civaschi E, Savoia A, Seri M, Melazzini F, Loffredo G, Russo G, Bozzi V, Notarangelo LD, Gresele P, Heller PG, Pujol-Moix N, Kunishima S, Cattaneo M, Bussel J, De Candia E, Cagioni C et al (2014) Platelet diameters in inherited thrombocytopenias: analysis of 376 patients with all known disorders. Blood 124:e4–e10. https://doi.org/10.1182/blood-2014-03-564328
Pujol-Moix N, Muñiz-Diaz E, Soler JA, Hernandez A, Boqué C, Callís M, López-Andrés N, Madoz P (1996) Familial immune pseudothrombocytopenia (9 cases). Transfus Med 6:197
Isik A, Balcik OS, Akdeniz D, Cipil H, Uysal S, Kosar A (2012) Relationship between some clinical situations, autoantibodies, and pseudothrombocytopenia. Clin Appl Thromb Hemost 18:645–649. https://doi.org/10.1177/1076029611434525
Díaz-Polo LE, Pujol-Moix N, Jiménez B, Canals C, Barranco-Charris E, Muñiz-Díaz E, Souto JC (2016) Shared autoimmunity: a case series of 56 patients with immune thrombocytopenia (ITP) associated with other autoimmune disorders. OALibJ 3:e2807
Rojas-Villarraga A, Amaya-Amaya J, Rodriguez-Rodriguez A, Mantilla RD, Anaya JM (2012) Introducing polyautoimmunity: secondary autoimmune diseases no longer exist. Autoimmune Dis 2012:254319. https://doi.org/10.1155/2012/254319
Mackay IR (2009) Clustering and commonalities among autoimmune diseases. J Autoimmun 33:170–177. https://doi.org/10.1016/j.jaut.2009.09.006
Anaya JM, Tobon GJ, Vega P, Castiblanco J (2006) Autoimmune disease aggregation in families with primary Sjögren's syndrome. J Rheumatol 33:2227–2234
Spitzer-Kravitz M, Marai I, Shoenfeld Y (2005) Coexistence of thyroid autoimmunity with other autoimmune diseases: Friend or foe? Additional aspects on the mosaic of autoimmunity. Autoimmunity 38:247–255. https://doi.org/10.1080/08916930500050194
Bai M, Feng J, Liang G (2018) Transient EDTA-dependent pseudothrombocytopenia phenomenon in a patient with antiphospholipid syndrome. Clin Lab 64:1581–1583. https://doi.org/10.7754/Clin.Lab.2018.180337
Lee AC (2021) Pseudothrombocytopenia: what every clinician should know. Pediatr Neonatol 62:218–219. https://doi.org/10.1016/j.pedneo.2020.12.002
Zandecki M, Genevieve F, Gerard J, Godon A (2007) Spurious counts and spurious results on haematology analysers: a review. Part I: platelets. Int J Lab Hematol 29:4–20. https://doi.org/10.1111/j.1365-2257.2006.00870.x
Cornbleet PJ, Myrick D, Levy R (1993) Evaluation of the Coulter STKS. five-part differential. Am J Clin Pathol 99:72–81. https://doi.org/10.1093/ajcp/99.1.72
Gulati GL, Kocher W, Schwarting R, Issa A, Dhanjal M (1999) Suspect flags and regional flags on the Coulter-STKS. An assessment Lab Med 30:675–680
Sandhaus LM, Osei ES, Agrawal NN, Dillman CA, Meyerson HJ (2002) Platelet counting by the Coulter LH 750, Sysmex XE 2100, and Advia 120. A comparative analysis using the RBC/platelet ratio reference method. Am J Clin Pathol 118:235–241. https://doi.org/10.1309/MK3G-MC3V-P06R-PNV2
Briggs CJ, Linssen J, Longair I, Machin SJ (2011) Improved flagging rates on the Sysmex XE-5000 compared with the XE-2100 reduce the number of manual film reviews and increase laboratory productivity. Am J Clin Pathol 136:309–316. https://doi.org/10.1309/AJCPDLR4KGKAFW4W
Ali I, Graham C, Dempsey-Hibbert NC (2019) Immature platelet fraction as a useful marker in the etiological determination of thrombocytopenia. Exp Hematol 78:56–61. https://doi.org/10.1016/j.exphem.2019.09.001
Miyazaki K, Koike Y, Kunishima S, Ishii R, Danbara M, Horie R, Yatomi Y, Higashihara M (2015) Immature platelet fraction measurement is influenced by platelet size and is a useful parameter for discrimination of macrothrombocytopenia. Hematology 20:587–592. https://doi.org/10.1179/1607845415Y.0000000021
Chiurazzi F, Villa MR, Rotoli B (1999) Transplacental transmission of EDTA-dependent pseudothrombocytopenia. Haematologica 84:664
Ohno N, Kobayashi M, Hayakawa S, Utsunomiya A, Karakawa S (2012) Transient pseudothrombocytopenia in a neonate: transmission of a maternal EDTA-dependent anticoagulant. Platelets 23:399–400. https://doi.org/10.3109/09537104.2011.624210
Korterink JJ, Boersma B, Schoorl M, Porcelijn L, Bartels PCM (2013) Pseudothrombocytopenia in a neonate due to mother? Eur J Pediatr 172:987–989. https://doi.org/10.1007/s00431-012-1892-4
Forscher CA, Sussman II, Friedman EW, Solomon V, Spaet TH (1985) Pseudothrombocytopenia masking true thrombocytopenia. Am J Hmatol 18:313–317. https://doi.org/10.1002/ajh.2830180314
Fozza C, Pardini S, Marras T, Longu F, Isoni A, Contini S, Longinotti M (2014) Pseudothrombocytopenia in a patient receiving romiplostim for immune thrombocytopenic purpura. Ann Hematol 93:899–900. https://doi.org/10.1007/s00277-013-1907-x
Salama A (2015) Autoimmune thrombocytopenia complicated by EDTA and/or citrate-dependent pseudothrombocytopenia. Transfus Med Hemother 42:345–348. https://doi.org/10.1159/000437220
Acknowledgments
The authors wish to thank Bradley Londres for professional language editing.
Author information
Authors and Affiliations
Contributions
N. Pujol-Moix and E. Muñiz-Diaz designed and coordinated de study. N. Pujol-Moix wrote the article. N. Pujol-Moix, J. C. Souto, I. Español, and A. Soler collected the clinical and laboratory data (automated platelet counts and indices, microscopic platelet counts and analyses on blood smears). E. Muñiz-Diaz performed the analyses of platelet antibodies. S. Mojal performed the statistical analyses. All authors critically reviewed and approved the final version of the manuscript.
Corresponding author
Ethics declarations
-The authors have no relevant financial or non-financial interests to disclose.
-The study was conducted in accordance with the ethical standards of the Declaration of Helsinki and was approved by the Institutional Review Board of the Hospital de la Santa Creu i Sant Pau.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pujol-Moix, N., Muñiz-Díaz, E., Español, I. et al. Pseudothrombocytopenia, beyond a laboratory phenomenon: study of 192 cases. Ann Hematol 102, 1363–1374 (2023). https://doi.org/10.1007/s00277-023-05192-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-023-05192-8