Abstract
Acute myeloid leukemia (AML) is the most common hematopoietic malignancy with abnormal lipid metabolism. However, currently available information on the involvement of the alterations in lipid metabolism in AML development is limited. In this study, we demonstrate that FABP5 expression facilitates AML cell viability, protects AML cells from apoptosis, and maintains triglyceride production. Our bioinformatics analysis revealed that FABP5 expression was upregulated and correlated with unfavorable overall survival of AML patients. FABP5 expression may be used to distinguish normal and AML with high accuracy. FABP5-based risk score was an independent risk factor for AML patients. AML patients with highly expressed FABP5 predicted resistance to drugs. In vitro study showed that FABP5 expression was remarkably elevated in primary AML blasts and an AML cell line. Silencing FABP5 expression attenuated AML cell viability, reduced triglyceride production and lipid droplet accumulation, and induced apoptosis. We utilized AutoDock online tool to identify lycorine as an FABP5 inhibitor by binding FABP5 at amino acid residues Ile54, Thr56, Thr63, and Arg109. Lycorine treatment downregulated the expression levels of FABP5 and its target PPARγ, impaired AML cell viability, triggered apoptosis, and reduced triglyceride production in AML cells. These results demonstrate that FABP5 is critical for AML cell survival and highlight a novel metabolic vulnerability for AML.
Graphical Abstract







Similar content being viewed by others
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Marando L, Huntly BJP (2020) Molecular landscape of acute myeloid leukemia: prognostic and therapeutic implications. Curr Oncol Rep 22(6):61. https://doi.org/10.1007/s11912-020-00918-7
Molica M, Breccia M, Foa R, Jabbour E, Kadia TM (2019) Maintenance therapy in AML: the past, the present and the future. Am J Hematol 94(11):1254–1265. https://doi.org/10.1002/ajh.25620
Pepe S, Scalzulli E, Colafigli G, Di Prima A, Diverio D, Mancini M, Latagliata R, Martelli M, Foà R, Breccia M (2020) Predictive factors for response and survival in elderly acute myeloid leukemia patients treated with hypomethylating agents: a real-life experience. Ann Hematol 99(10):2405–2416. https://doi.org/10.1007/s00277-020-04217-w
Samudio I, Harmancey R, Fiegl M, Kantarjian H, Konopleva M, Korchin B, Kaluarachchi K, Bornmann W, Duvvuri S, Taegtmeyer H, Andreeff M (2010) Pharmacologic inhibition of fatty acid oxidation sensitizes human leukemia cells to apoptosis induction. J Clin Investig 120(1):142–156. https://doi.org/10.1172/jci38942
Senga S, Kobayashi N, Kawaguchi K, Ando A (1863) Fujii H (2018) Fatty acid-binding protein 5 (FABP5) promotes lipolysis of lipid droplets, de novo fatty acid (FA) synthesis and activation of nuclear factor-kappa B (NF-κB) signaling in cancer cells. Biochim Biophys Acta 9:1057–1067. https://doi.org/10.1016/j.bbalip.2018.06.010
Pabst T, Kortz L, Fiedler GM, Ceglarek U, Idle JR, Beyoğlu D (2017) The plasma lipidome in acute myeloid leukemia at diagnosis in relation to clinical disease features. BBA clinical 7:105–114. https://doi.org/10.1016/j.bbacli.2017.03.002
Wang D, Dubois RN (2010) Eicosanoids and cancer. Nature reviews. Cancer 10(3):181–193. https://doi.org/10.1038/nrc2809
Stevens BM, Jones CL, Pollyea DA, Culp-Hill R, D’Alessandro A, Winters A, Krug A, Abbott D, Goosman M, Pei S, Ye H, Gillen AE, Becker MW, Savona MR, Smith C, Jordan CT (2020) Fatty acid metabolism underlies venetoclax resistance in acute myeloid leukemia stem cells. Nature cancer 1(12):1176–1187. https://doi.org/10.1038/s43018-020-00126-z
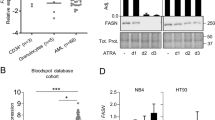
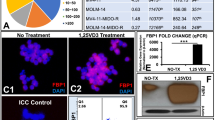
Humbert M, Seiler K, Mosimann S, Rentsch V, Sharma K, Pandey AV, McKenna SL, Tschan MP (2021) Reducing FASN expression sensitizes acute myeloid leukemia cells to differentiation therapy. Cell Death Differ 28(8):2465–2481. https://doi.org/10.1038/s41418-021-00768-1
Chen YQ, Edwards IJ, Kridel SJ, Thornburg T, Berquin IM (2007) Dietary fat-gene interactions in cancer. Cancer Metastasis Rev 26(3–4):535–551. https://doi.org/10.1007/s10555-007-9075-x
Hajri T, Abumrad NA (2002) Fatty acid transport across membranes: relevance to nutrition and metabolic pathology. Annu Rev Nutr 22:383–415. https://doi.org/10.1146/annurev.nutr.22.020402.130846
Lee GS, Pan Y, Scanlon MJ, Porter CJH, Nicolazzo JA (2018) Fatty acid-binding protein 5 mediates the uptake of fatty acids, but not drugs, into human brain endothelial cells. J Pharm Sci 107(4):1185–1193. https://doi.org/10.1016/j.xphs.2017.11.024
Armstrong EH, Goswami D, Griffin PR, Noy N, Ortlund EA (2014) Structural basis for ligand regulation of the fatty acid-binding protein 5, peroxisome proliferator-activated receptor β/δ (FABP5-PPARβ/δ) signaling pathway. J Biol Chem 289(21):14941–14954. https://doi.org/10.1074/jbc.M113.514646
Adamson J, Morgan EA, Beesley C, Mei Y, Foster CS, Fujii H, Rudland PS, Smith PH, Ke Y (2003) High-level expression of cutaneous fatty acid-binding protein in prostatic carcinomas and its effect on tumorigenicity. Oncogene 22(18):2739–2749. https://doi.org/10.1038/sj.onc.1206341
Liu XS, Jiang J, Jiao XY, Wu YE, Lin JH, Cai YM (2009) Lycorine induces apoptosis and down-regulation of Mcl-1 in human leukemia cells. Cancer Lett 274(1):16–24. https://doi.org/10.1016/j.canlet.2008.08.029
Zhang C, Liao Y, Liu P, Du Q, Liang Y, Ooi S, Qin S, He S, Yao S, Wang W (2020) FABP5 promotes lymph node metastasis in cervical cancer by reprogramming fatty acid metabolism. Theranostics 10(15):6561–6580. https://doi.org/10.7150/thno.44868
Seo J, Jeong DW, Park JW, Lee KW, Fukuda J, Chun YS (2020) Fatty-acid-induced FABP5/HIF-1 reprograms lipid metabolism and enhances the proliferation of liver cancer cells. Commun Biol 3(1):638. https://doi.org/10.1038/s42003-020-01367-5
Geeleher P, Cox NJ, Huang RS (2014) Clinical drug response can be predicted using baseline gene expression levels and in vitro drug sensitivity in cell lines. Genome Biol 15(3):R47. https://doi.org/10.1186/gb-2014-15-3-r47
Trott O, Olson AJ (2010) AutoDock Vina: improving the speed and accuracy of docking with a new scoring function, efficient optimization, and multithreading. J Comput Chem 31(2):455–461. https://doi.org/10.1002/jcc.21334
Carbonetti G, Converso C, Clement T, Wang C, Trotman LC, Ojima I, Kaczocha M (2020) Docetaxel/cabazitaxel and fatty acid binding protein 5 inhibitors produce synergistic inhibition of prostate cancer growth. Prostate 80(1):88–98. https://doi.org/10.1002/pros.23921
Pan Y, Tian T, Park CO, Lofftus SY, Mei S, Liu X, Luo C, O’Malley JT, Gehad A, Teague JE, Divito SJ, Fuhlbrigge R, Puigserver P, Krueger JG, Hotamisligil GS, Clark RA, Kupper TS (2017) Survival of tissue-resident memory T cells requires exogenous lipid uptake and metabolism. Nature 543(7644):252–256. https://doi.org/10.1038/nature21379
Pan Y, Scanlon MJ, Owada Y, Yamamoto Y, Porter CJ, Nicolazzo JA (2015) Fatty acid-binding protein 5 facilitates the blood-brain barrier transport of docosahexaenoic acid. Mol Pharm 12(12):4375–4385. https://doi.org/10.1021/acs.molpharmaceut.5b00580
Bao Z, Malki MI, Forootan SS, Adamson J, Forootan FS, Chen D, Foster CS, Rudland PS, Ke Y (2013) A novel cutaneous fatty acid-binding protein-related signaling pathway leading to malignant progression in prostate cancer cells. Genes Cancer 4(7–8):297–314. https://doi.org/10.1177/1947601913499155
Evans RM, Barish GD, Wang YX (2004) PPARs and the complex journey to obesity. Nat Med 10(4):355–361. https://doi.org/10.1038/nm1025
Khan D, Ara T, Ravi V, Rajagopal R, Tandon H, Parvathy J, Gonzalez EA, Asirvatham-Jeyaraj N, Krishna S, Mishra S, Raghu S, Bhati AS, Tamta AK, Dasgupta S, Kolthur-Seetharam U, Etchegaray JP, Mostoslavsky R, Rao PSM, Srinivasan N, Sundaresan NR (2021) SIRT6 transcriptionally regulates fatty acid transport by suppressing PPARγ. Cell reports 35(9):109190. https://doi.org/10.1016/j.celrep.2021.109190
Yan S, Elmes MW, Tong S, Hu K, Awwa M, Teng GYH, Jing Y, Freitag M, Gan Q, Clement T, Wei L, Sweeney JM, Joseph OM, Che J, Carbonetti GS, Wang L, Bogdan DM, Falcone J, Smietalo N, Zhou Y, Ralph B, Hsu HC, Li H, Rizzo RC, Deutsch DG, Kaczocha M, Ojima I (2018) SAR studies on truxillic acid mono esters as a new class of antinociceptive agents targeting fatty acid binding proteins. Eur J Med Chem 154:233–252. https://doi.org/10.1016/j.ejmech.2018.04.050
Seeliger D, de Groot BL (2010) Ligand docking and binding site analysis with PyMOL and Autodock/Vina. J Comput Aided Mol Des 24(5):417–422. https://doi.org/10.1007/s10822-010-9352-6
Carbonetti G, Wilpshaar T, Kroonen J, Studholme K, Converso C, d’Oelsnitz S, Kaczocha M (2019) FABP5 coordinates lipid signaling that promotes prostate cancer metastasis. Sci Rep 9(1):18944. https://doi.org/10.1038/s41598-019-55418-x
Gupta S, Pramanik D, Mukherjee R, Campbell NR, Elumalai S, de Wilde RF, Hong SM, Goggins MG, De Jesus-Acosta A, Laheru D, Maitra A (2012) Molecular determinants of retinoic acid sensitivity in pancreatic cancer. Clin Cancer Res 18(1):280–289. https://doi.org/10.1158/1078-0432.Ccr-11-2165
Thulasiraman P, McAndrews DJ, Mohiudddin IQ (2014) Curcumin restores sensitivity to retinoic acid in triple negative breast cancer cells. BMC Cancer 14:724. https://doi.org/10.1186/1471-2407-14-724
Mazzarella L, Botteri E, Matthews A, Gatti E, Di Salvatore D, Bagnardi V, Breccia M, Montesinos P, Bernal T, Gil C, Ley TJ, Sanz M, Bhaskaran K, Coco FL, Pelicci PG (2020) Obesity is a risk factor for acute promyelocytic leukemia: evidence from population and cross-sectional studies and correlation with FLT3 mutations and polyunsaturated fatty acid metabolism. Haematologica 105(6):1559–1566. https://doi.org/10.3324/haematol.2019.223925
Shibue K, Yamane S, Harada N, Hamasaki A, Suzuki K, Joo E, Iwasaki K, Nasteska D, Harada T, Hayashi Y, Adachi Y, Owada Y, Takayanagi R, Inagaki N (2015) Fatty acid-binding protein 5 regulates diet-induced obesity via GIP secretion from enteroendocrine K cells in response to fat ingestion. Am J Physiol Endocrinol Metab 308(7):E583-591. https://doi.org/10.1152/ajpendo.00543.2014
Dong SR, Ju XL, Yang WZ (2019) STAT5A reprograms fatty acid metabolism and promotes tumorigenesis of gastric cancer cells. Eur Rev Med Pharmacol Sci 23(19):8360–8370. https://doi.org/10.26355/eurrev_201910_19147
Wu T, Tian J, Cutler RG, Telljohann RS, Bernlohr DA, Mattson MP, Handa JT (2010) Knockdown of FABP5 mRNA decreases cellular cholesterol levels and results in decreased apoB100 secretion and triglyceride accumulation in ARPE-19 cells. Lab Investig 90(6):906–914
Lv Q, Wang G, Zhang Y, Han X, Li H, Le W, Zhang M, Ma C, Wang P, Ding Q (2019) FABP5 regulates the proliferation of clear cell renal cell carcinoma cells via the PI3K/AKT signaling pathway. Int J Oncol 54(4):1221–1232. https://doi.org/10.3892/ijo.2019.4721
Field CS, Baixauli F, Kyle RL, Puleston DJ, Cameron AM, Sanin DE, Hippen KL, Loschi M, Thangavelu G, Corrado M, Edwards-Hicks J, Grzes KM, Pearce EJ, Blazar BR, Pearce EL (2020) Mitochondrial integrity regulated by lipid metabolism is a cell-intrinsic checkpoint for treg suppressive function. Cell Metab 31(2):422-437.e425. https://doi.org/10.1016/j.cmet.2019.11.021
Wang W, Liu Z, Chen X, Lu Y, Wang B, Li F, Lu S, Zhou X (2021) Downregulation of FABP5 suppresses the proliferation and induces the apoptosis of gastric cancer cells through the hippo signaling pathway. DNA Cell Biol 40(8):1076–1086. https://doi.org/10.1089/dna.2021.0370
Yan F, Liu X, Zhang S, Su J, Zhang Q, Chen J (2018) Molecular dynamics exploration of selectivity of dual inhibitors 5M7, 65X, and 65Z toward fatty acid binding proteins 4 and 5. International journal of molecular sciences 19 (9) https://doi.org/10.3390/ijms19092496
Hsu HC, Tong S, Zhou Y, Elmes MW, Yan S, Kaczocha M, Deutsch DG, Rizzo RC, Ojima I, Li H (2017) The antinociceptive agent SBFI-26 binds to anandamide transporters FABP5 and FABP7 at two different sites. Biochemistry 56(27):3454–3462. https://doi.org/10.1021/acs.biochem.7b00194
Funding
This work was supported by the National Natural Science Foundation of China (31960137, 32260171) and the Guizhou Provincial Natural Science Foundation (Qiankehejichu [2016]1416).
Author information
Authors and Affiliations
Contributions
Q.F.Z. and H.B. conceived and designed the study. B.X.G diagnosed AML patients and provided samples. X.M.L., W.L.F., Y.H.P, J.J.D., T.Z, D.G.F., and W.H. obtained and assembled data. X.L.Q., C.X.W., Y.H., and W.F.Y. analyzed and interpreted the data. Y.H. and C.J.W. did the statistical analysis. The paper was written by Q.F.Z. All authors read and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Consent to participate
Informed consent was obtained from all patients for being included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liang, X., Fu, W., Peng, Y. et al. Lycorine induces apoptosis of acute myeloid leukemia cells and inhibits triglyceride production via binding and targeting FABP5. Ann Hematol 102, 1073–1086 (2023). https://doi.org/10.1007/s00277-023-05169-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-023-05169-7