Abstract
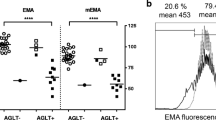
This prospective study was carried out to assess the usefulness of five laboratory tests in the diagnosis of hereditary spherocytosis (HS), based on the correlation of erythrocyte membrane protein defects with clinical and laboratory features, and also to determine the membrane protein deficiencies detected in Argentina. Of 116 patients and their family members tested, 62 of them were diagnosed to have HS. The specificity of cryohemolysis (CH) test was 95.2%, and its cut-off value to distinguish HS from normal was 2.8%. For flow cytometry, cut-off points of 17% for mean channel fluorescence (MCF) decrease and 14% coefficient of variation (CV) increase showed 95.9% and 92.2% specificity, respectively. Both tests showed the highest percentages of positive results for diagnosis. Either CH or flow cytometry was positive in 93.5% of patients. In eight patients, flow cytometry was positive only through CV increase. Protein defects were detected in 72.3% of patients; ankyrin and spectrin were the most frequently found deficiencies. The CV of the fluorescence showed significantly higher increases in moderate and severe anemia than in mild anemia (p = 0.003). Severity of anemia showed no other correlation with tests results, type of deficient protein, inheritance pattern, or neonatal jaundice. CH and flow cytometry are easy methods with the highest diagnostic accuracy. Simultaneous reading of mean channel fluorescence (MCF) decrease and CV increase improve diagnostic usefulness of flow cytometry. This test seems to be a reliable predictor of severity. The type of detected protein deficiency has no predictive value for outcome. Predominant ankyrin and spectrin deficiencies agree with reports from other Latin American countries.




Similar content being viewed by others
References
Grace RF, Lux SE (2009) Disorders of the red cell membrane. In: Orkin SH, Nathan DG, Ginsburg D, Fisher DE, Lux SE (eds) Hematology of infancy and childhood. Saunders, Philadelphia, pp 659–838
Hassoun H, Palek J (1996) Hereditary spherocytosis: a review of the clinical and molecular aspects of the disease. Blood Rev 10:129–147
Bolton-Maggs PHB, Stevens RF, Dodd NJ, Lamont G, Tittensor P (2004) On behalf of the General Haematology Task Force of the British Committee for Standards in Haematology. Guidelines for the diagnosis and management of hereditary spherocytosis. Br J Haematol 126:455–474
Gallagher PG (2005) Red cell membrane disorders. Hematology. Am Soc Hematol Educ Program
Mariani M, Barcellini W, Vercellati C, Marcello AP, Fermo E, Pedotti P et al (2008) Clinical and hematologic features of 300 patients affected by hereditary spherocytosis grouped according to the type of the membrane protein defect. Haematologica 93:1310–1317
Iolascon A, Avvisati RA (2008) Genotype/phenotype correlation in hereditary spherocytosis. Haematologica 93:1283–1288
King MJ, Telfer P, MacKinnon H, Langabeer L, McMahon C, Darbyshire P et al (2008) Using the eosin-5-maleimide binding test in the differential diagnosis of hereditary spherocytosis and hereditary pyropoikilocytosis. Cytometry Part B Clin Cytom 74B:244–250
Dacie JV, Lewis SM, Luzzato L (1991) Investigation of the hereditary haemolytic anaemias: membrane and enzyme abnormalities. In: Dacie JV, Lewis SM (eds) Practical haematology. Churchill Livingstone, Edinburgh, pp 195–225
Korones D, Pearson HA (1989) Normal erythrocyte osmotic fragility in hereditary spherocytosis. J Pediatr 114:264–266
Perrotta S, Gallagher PG, Mohandas N (2008) Hereditary spherocytosis. Lancet 372:1411–1426
King MJ, Behrens J, Rogers C, Flynn C, Greenwood D, Chambers K (2000) Rapid flow cytometric test for the diagnosis of membrane cytoskeleton-associated haemolytic anaemia. Br J Haematol 111:924–933
Streichman S, Gesheidt Y, Tatarsky I (1990) Hypertonic cryohemolysis: a diagnostic test for hereditary spherocytosis. Am J Hematol 35:104–109
Streichman S, Gescheidt Y (1998) Cryohemolysis for the detection of hereditary spherocytosis: correlation studies with osmotic fragility and autohemolysis. Am J Hematol 58:206–212
Stoya G, Gruhn B, Vogelsang H, Baumann E, Linss W (2006) Flow cytometry as a diagnostic tool for hereditary spherocytosis. Acta Haematol 116:186–191
Tachavanich K, Tanphaichitr VS, Utto W, Viprakasit V (2009) Rapid flow cytometric test using eosin-5-maleimide for diagnosis of red blood cell membrane disorders. Southeast Asian J Trop Med Public Health 40:570–574
Parpart AK, Lorenz PB, Papart ER, Gregg JR, Chase AM (1947) The osmotic resistance (fragility) of human red cells. J Clin Invest 26:636–640
Selwyn JG, Dacie JV (1954) Autohemolysis and other changes resulting from the incubation in vitro of red cells from patients with congenital hemolytic anemia. Blood 9:414–438
Vittori D, Garbossa G, Lafourcade C, Pérez G, Nesse A (2002) Human erytroid cells are affected by aluminium. Alteration of membrane band 3 protein. Biochem Biophys Acta 1558:142–150
Lowry OH, Roseborough NJ, Farr AL, Randall RL (1951) Protein measurements with Folin reagent. J Biol Chem 193:267–275
Streichman S, Kahana E, Tatarsky I (1985) Hypertonic cryohemolysis of pathologic red blood cells. Am J Hematol 20:373–381
Romero RR, Poo JL, Robles JA, Uriostegui A, Vargas F, Majluf-Cruz A (1997) Usefulness of cryohemolysis test in the diagnosis of hereditary spherocytosis. Arch Med Res 28:247–251
Iglauer A, Reinhardt D, Schröter W, Pekrun A (1999) Cryohemolysis test as a diagnostic tool for hereditary spherocytosis. Ann Hematol 78:555–557
Girodon F, Garçon L, Bergoin E, Largier M, Delaunay J, Feneant-Thibault M et al (2008) Usefulness of the eosin-5′-maleimide cytometric method as a first-line screening test for the diagnosis of hereditary spherocytosis: comparison with ektacytometry and protein electrophoresis. Br J Haematol 140:468–470
Kar R, Rao S, Srinivas UM, Mishra P, Pati HP (2009) Clinico-hematological profile of hereditary spherocytosis: experience from a tertiary care center in North India. Hematology 14:164–167
Kedar PS, Colah RB, Kullkarni S, Ghosh K, Mohanty D (2003) Experience with eosin-5-maleimide as a diagnostic tool for red cell membrane cytoskeleton disorders. Clin Lab Haematol 25:373–376
Miraglia del Giudice F, Iolascon A, Pinto L, Nobili B, Perrotta S (1994) Erythrocyte membrana protein alterations underlying clinical heterogeneity in hereditary spherocytosis. Br J Haematol 88:52–55
Yawata Y, Kanzaki A, Yawata A, Doerfler W, Ozcan R, Eber SW (2000) Characteristic features of the genotype and phenotype of hereditary spherocytosis in the Japanese population. Int J Hematol 7:118–135
Lee YK, Cho HI, Park SS, Lee YJ, Ra E, Chang YH et al (2000) Abnormalities of erythrocyte membrane proteins in Korean patients with hereditary spherocytosis. J Korean Med Sci 15:284–288
Sánchez-López JY, Camacho AL, Magaña MT, Ibarra B, Perea FJ (2003) Red cell membrane protein deficiencias in Mexican patients with hereditary spherocytosis. Blood Cells Mol Dis 31:357–359
Costa FF, Agre P, Watkins PC, Winkelmann JC, Tang TK, John KM et al (1990) Linkage of dominant hereditary spherocytosis to the gene for the erythrocyte membrane-skeleton protein ankyrin. N Engl J Med 323:1046–1050
Saad ST, Costa FF, Vicentin DL, Salles TS, Pranke PH (1994) Red cell membrane protein abnormalities in hereditary spherocytosis in Brazil. Br J Haematol 88:295–299
Lanciotti M, Perutelli P, Valetto A, Di Martino D, Mori PG (1997) Ankyrin deficiency is the most common defect in dominant and non dominant hereditary spherocytosis. Haematologica 82:460–462
Dhermy D, Bournier O, Bougeois M, Grandchamp B (1999) The red blood cell band 3 variant (band 3 Bicetrel: R 490 C) association with dominant hereditary spherocytosis causes defective membrane targeting of the molecule and a dominant negative effect. Mol Membr Biol 16:305–312
Premetis E, Stamoulakatou A, Loukopoulos D (1999) Hereditary spherocytosis in Greece: collective data on a large number of patients. Hematology 4:361–366
Ricard MP, Gilsanz F, Millan I (2000) Erythroid membrane protein defects in hereditary spherocytosis. A study of 62 Spanish cases. Haematologica 85:994–995
Cynober T, Mohandas N, Tchernia G (1996) Red cell abnormalities in hereditary spherocytosis: relevance to diagnosis and understanding of the variable expression of clinical severity. J Lab Clin Med 12:259–269
Rocha S, Rebelo I, Costa E, Catarino C, Belo L, Castro EBM et al (2005) Protein deficiency balance as a predictor of clinical outcome in hereditary spherocytosis. Eur J Haematol 74:374–380
Shi Z, Afzal V, Coller B, Patel D, Chasis JA, Parra M et al (1999) Protein 4.1R-deficient mice are viable but have erythroid membrane skeleton abnormalities. J Clin Invest 103:331–340
Delaunay J (2007) The molecular basis of hereditary red cell membrane disorders. Blood 21:1–20
Rivera A, De Franceschi L, Peters LL, Gascard P, Mohandas N, Brugnara C (2006) Effect of complete protein 4.1R deficiency on ion transport properties of murine erythrocytes. Am J Physiol Cell Physiol 291:C880–C886
Goodman SR, Shiffer KA, Casoria LA, Eyster ME (1982) Identification of the molecular defect in the erythrocyte membrane skeleton of some kindreds with hereditary spherocytosis. Blood 60:772–784
Becker PS, Morrow JS, Lux SE (1987) Abnormal oxidant sensitivity and beta-chain structure of spectrin in hereditary spherocytosis associated with defective spectrin-protein 4.1 binding. J Clin Invest 80:557–565
Agre P, Asimos A, Casella JF, McMillan C (1986) Inheritance pattern and clinical response to splenectomy as a reflection of erythrocyte spectrin deficiency in hereditary spherocytosis. N Engl J Med 315:1579–1583
Jarolim P, Murray JL, Rubin HL, Taylor WM, Prchal JT, Ballas SK et al (1996) Characterization of 13 novel band 3 gene defects in hereditary spherocytosis with band 3 deficiency. Blood 88:4366–4374
Nakanishi H, Kanzaki A, Yawata A, Yamada O, Yawata Y (2001) Ankyrin gene mutations in Japanese patients with hereditary spherocytosis. Int J Hematol 73:54–63
Morton NE, MacKinney AA, Kosower N, Schilling RF, Gray MP (1963) Genetics of spherocytosis. Am J Hum Genet 14:170–184
Eber SW, Armbrust R, Schröter W (1990) Variable clinical severity of hereditary spherocytosis: relation to erythrocyte spectrin concentration, osmotic fragility and autohemolysis. J Pediatr 117:409–416
Gallagher PG, Forget BG (2001) Hereditary spherocytosis, elliptocytosis and related disorders. In: Beutler E, Lichtman MA, Coller BS, Kipps TJ, Seligsohn U (eds) Williams hematology. McGraw-Hill, New York, pp 503–518
Eber SW, Gonzalez JM, Dornwell M et al (1996) Ankyrin-1 mutations are a major cause of dominant and recessive hereditary spherocytosis. Nat Genet 13:214–218
Gallagher PJ, Ferreira JD, Costa FF, Saad ST, Forget BG (2000) A recurrent frameshift mutation of the ankyrin gene associated with severe hereditary spherocytosis. Br J Haematol 111:1190–1193
Miraglia del Giudice E, Nobili B, Francese M, D’Urso L, Iolascon A, Eber S et al (2001) Clinical and molecular evaluation of non-dominant hereditary spherocytosis. Br J Haematol 112:42–47
Pinto L, Iolascon A, MiragliadelGiudice E, Matarese MRS, Nobili B, Perrotta S (1995) The Italian pediatric survey on hereditary spherocytosis. Int J Pediatr Hematol Oncol 2:43–47
Aramburu Arriaga N, Fernández Cuesta MA, Martínez Gonzalez MJ, Astigarraga Aguirre I, Fernandez-Teijeiro Alvarez A, Navajas Gutierrez A et al (2000) Hereditary spherocytosis in neonates. Review of our casuistics. Ann Esp Pediatr 52:569–572
Delhommeau F, Cynober T, Schischmanoff PO, Rohrlich P, Delaunay N, Mohandas N et al (2000) Natural history of hereditary spherocytosis during the first year of life. Blood 95:393–397
Acknowledgment
The authors would like to thank Viviana Sanchez for her technical assistance in the preparation of the manuscript and Laura Marangunich for statistical advice.
Conflicts of Interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Crisp, R.L., Solari, L., Vota, D. et al. A prospective study to assess the predictive value for hereditary spherocytosis using five laboratory tests (cryohemolysis test, eosin-5′-maleimide flow cytometry, osmotic fragility test, autohemolysis test, and SDS-PAGE) on 50 hereditary spherocytosis families in Argentina. Ann Hematol 90, 625–634 (2011). https://doi.org/10.1007/s00277-010-1112-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00277-010-1112-0