Abstract.
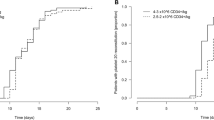
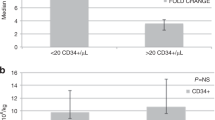
We assessed the influence of amifostine on immune reconstitution after conventional-dose paclitaxel, ifosfamide, cisplatin and high-dose carboplatin, etoposide and thiotepa followed by autologous peripheral blood progenitor cell (PBPC) rescue in patients with germ cell tumor (GCT). A total of 40 patients were treated with one cycle of paclitaxel and ifosfamide (TI) followed by granulocyte-colony stimulating factor (G-CSF) to mobilize PBPC, three cycles of paclitaxel, ifosfamide and cisplatin (TIP) and one course of high-dose carboplatin, etoposide and thiotepa (CET) plus PBPC rescue. Patients were randomized to receive an absolute dose of 500 mg amifostine (group A, n=20) on each day of chemotherapy or no amifostine (group B, n=20). Prior to each cycle of chemotherapy, after hematologic engraftment from CET, 6 weeks and 3 months after transplantation the subpopulations of lymphocytes were phenotyped. Between the two study groups no statistically significant differences were observed concerning reconstitution of lymphocyte subpopulations. Throughout treatment with TIP or CET lymphocyte counts and their subpopulations remained low without severe clinical complications. Delayed reconstitution of the CD4+ cell compartment after PBPC rescue was observed in both study groups, but did not result in any severe or atypical infections. Treatment with amifostine administered at this dose did not significantly influence the reconstitution of lymphocyte subpopulations. Low numbers of lymphocytes during chemotherapy and delayed reconstitution of CD4+ cells and other lymphocyte subpopulations after PBPC rescue had no clinical relevance for patients with GCT.
Similar content being viewed by others
Author information
Authors and Affiliations
Additional information
Electronic Publication
Rights and permissions
About this article
Cite this article
Rick, .O., Beyer, .J., Schwella, .N. et al. Influence of amifostine on reconstitution of lymphocyte subpopulations after conventional- and high-dose chemotherapy in patients with germ cell tumor. Ann Hematol 81, 717–722 (2002). https://doi.org/10.1007/s00277-002-0538-4
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s00277-002-0538-4